The Integration Challenge That Defines Healthcare Technology
Every healthtech product lives or dies by one capability: can it connect to the hospital's EHR? A brilliant clinical decision support tool, a revolutionary patient engagement platform, or an AI diagnostic assistant — none of them matter if they can't access and exchange data with Epic, Cerner, MEDITECH, or whichever EHR system a hospital runs.
EHR integration is simultaneously the most critical and most complex challenge in healthcare technology. Get it right, and you unlock access to 96% of US hospitals. Get it wrong, and you've built a product no one can use.
This guide covers every dimension: integration methods, vendor ecosystems, FHIR API capabilities, security architecture, project timelines, costs, and the practical lessons learned from real implementations.
The 4 Methods of EHR Integration
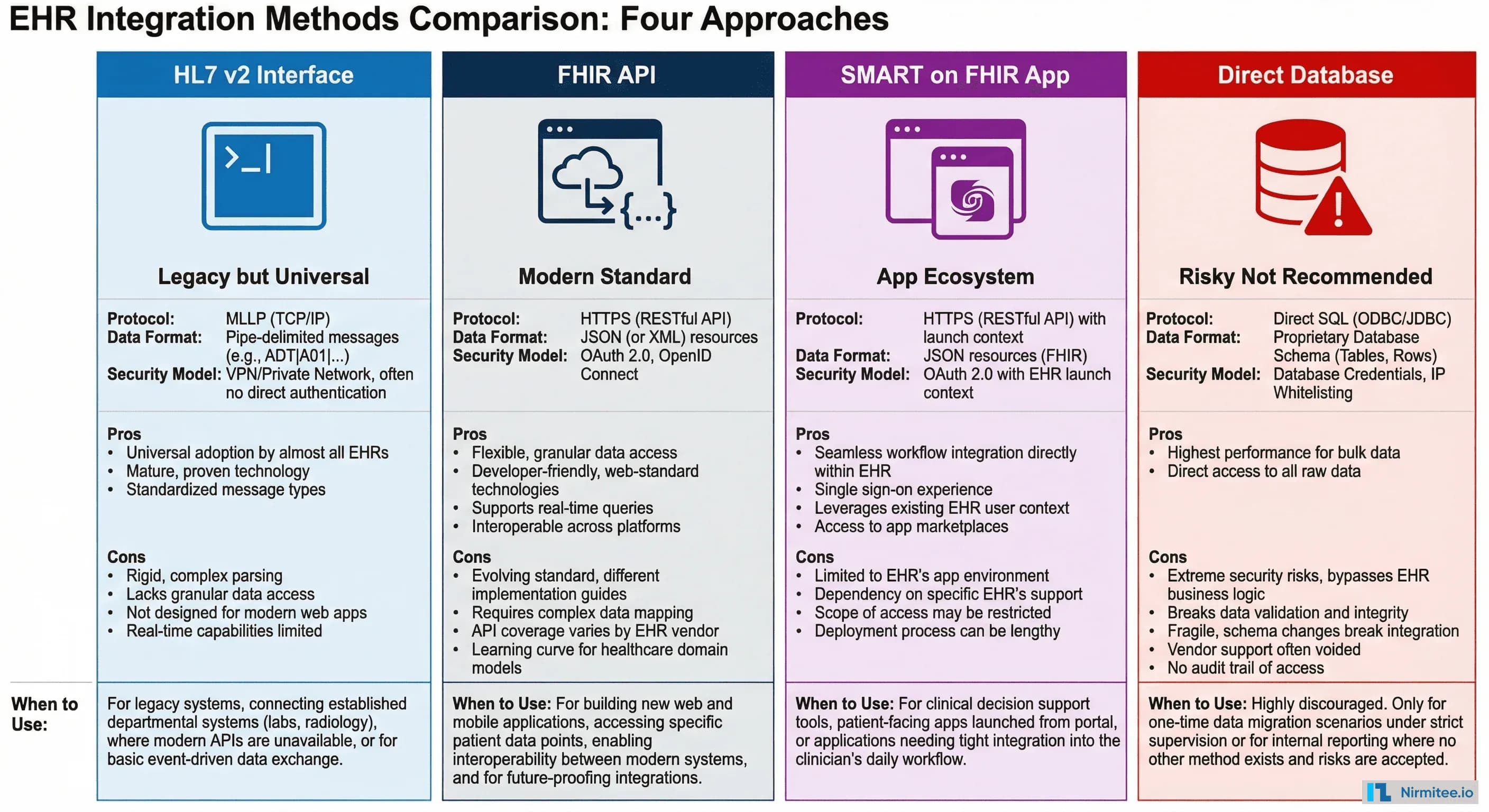
There are four ways to connect to an EHR system. Each has different trade-offs in terms of capability, complexity, and vendor requirements.
1. HL7 v2 Interface (Legacy but Universal)
The traditional approach. HL7 v2 messages flow between systems over MLLP connections through an integration engine. Every EHR supports this. It's battle-tested and well-understood. The downsides: it requires on-premise infrastructure, VPN connectivity, and specialized HL7 expertise. Best for internal hospital integrations — lab orders, ADT feeds, billing.
2. FHIR API (Modern Standard)
REST APIs using FHIR R4. Standard HTTP requests return JSON data. Every major EHR vendor now provides FHIR APIs. This is the path for cloud-based applications, mobile apps, and any integration where you want modern web architecture. The downside: FHIR API coverage varies by vendor — some expose dozens of resources, others only the minimum required by CMS.
3. SMART on FHIR App Launch
Your application launches directly inside the EHR's user interface. Clinicians click a button in Epic or Cerner, and your app opens in context — with the current patient already selected and authorized. This is the gold standard for clinical workflow integration. Requires listing in the EHR vendor's app marketplace (Epic App Orchard, Cerner Code).
4. Direct Database Access (Not Recommended)
Some legacy integrations connect directly to the EHR's underlying database. This is risky — it bypasses the EHR's access controls, breaks with upgrades, and most vendors explicitly prohibit it in their contracts. Avoid this approach entirely for new integrations.
The US EHR Market in 2026
Your integration strategy is shaped by which EHR vendors your target customers use. Here's how the US market stands in 2026.
Epic dominates with 38% of the acute care hospital market. If you build one EHR integration, start with Epic — it covers more than a third of US hospitals and nearly all large academic medical centers. Oracle Health (formerly Cerner) is second at 22%, followed by MEDITECH at 16%.
The practical implication: Integrating with Epic and Oracle Health alone gives you access to 60% of US hospitals. Add MEDITECH and athenahealth, and you're at 83%. Most healthtech companies start with Epic, then expand.
Epic Integration Ecosystem
Epic is the most integrated-with EHR in healthcare. Understanding its integration ecosystem is essential for any healthtech company or hospital IT team.
Epic provides multiple integration pathways:
- Epic App Orchard — The marketplace for SMART on FHIR apps. Over 500 apps listed. Requires Epic's review and approval process.
- Epic FHIR R4 APIs — Comprehensive FHIR support including Patient Access, Provider Access, and Payer Access APIs. Epic has one of the most complete FHIR implementations in the industry.
- HL7 v2 Bridges — Traditional ADT, ORM, ORU, and DFT interfaces. Still the primary method for most internal hospital integrations.
- Care Everywhere — Epic's proprietary network for cross-organization data exchange. Connects Epic hospitals to each other and to non-Epic organizations through Carequality.
- CDS Hooks — Real-time clinical decision support. Your application can present recommendations, alerts, or links to clinicians at specific workflow trigger points.
EHR Vendor FHIR API Capabilities
Not all EHR FHIR implementations are equal. This comparison helps you understand what's available from each major vendor.
Key takeaways:
- Epic leads in FHIR completeness — full R4 support, SMART app launch, Bulk Data, CDS Hooks, and extensive write-back capabilities.
- Oracle Health (Cerner) has strong FHIR support with its Millennium platform. Good SMART integration and growing resource coverage.
- MEDITECH Expanse has improved significantly — solid FHIR R4 read access and Patient Access API compliance, but write-back is more limited.
- Ambulatory EHRs (athenahealth, eClinicalWorks, NextGen) vary widely. Many meet CMS minimum requirements but offer limited FHIR functionality beyond that.
Critical question to ask any EHR vendor: "Which FHIR resources do you support for read and write, and what is your SMART on FHIR app launch certification status?"
Common EHR Integration Data Flows
A typical hospital EHR connects to 8 or more external systems. Understanding these standard data flows helps you scope your integration project and identify dependencies.
The eight most common EHR integrations:
- Lab System — Bidirectional: ORM orders out, ORU results back (HL7 v2)
- Pharmacy — Bidirectional: prescriptions out, dispense confirmations back (HL7 v2)
- Radiology/PACS — Bidirectional: imaging orders out, reports back (HL7 v2 + DICOM)
- Billing/RCM — Outbound: charges, encounters, claims (HL7 v2 DFT or X12 837)
- Patient Portal — Outbound: patient data via FHIR APIs (FHIR R4)
- Public Health — Outbound: immunizations, syndromic surveillance (HL7 v2)
- HIE/TEFCA — Bidirectional: clinical documents and queries (CCDA + FHIR)
- Third-Party Apps — Inbound: SMART on FHIR app launch with read/write access (FHIR R4)
Security Architecture for EHR Integration
Every EHR integration touches Protected Health Information (PHI), making HIPAA compliance non-negotiable. Here's the security architecture that meets both regulatory requirements and EHR vendor expectations.
The architecture follows a three-zone model:
- External Zone — Third-party apps and patient apps connect over the public internet using TLS 1.3.
- DMZ — API Gateway handles rate limiting, token validation, and request routing. OAuth 2.0 Authorization Server manages authentication and consent. This is your security perimeter.
- Internal Zone — FHIR Server and EHR Database sit behind the DMZ, accessible only to authenticated and authorized requests. Every data access is logged to an Audit Service for HIPAA compliance.
EHR vendors will audit your security architecture during the app review process. Hospitals will require a BAA (Business Associate Agreement), penetration test results, and SOC 2 Type II certification before allowing production access.
EHR Integration Project Timeline
How long does an EHR integration project actually take? Here's a realistic timeline based on typical healthtech implementations.
The biggest time sink: The vendor app review process (Phase 3) is where most timelines slip. Epic's App Orchard review takes 4-8 weeks minimum, and often longer if security or compliance issues surface. Plan for this.
Total timeline: 4-6 months for a single EHR integration. Multi-EHR platforms typically take 9-12 months to reach three vendor integrations.
Cost Breakdown
EHR integration costs vary enormously based on scope, but understanding the typical cost structure helps with budgeting.
Typical cost ranges:
- Single EHR Integration (one vendor, read-only FHIR): $50K-$150K
- Multi-EHR Platform (2-3 vendors, read/write): $200K-$500K
- Enterprise Health System (full HL7 v2 + FHIR, 20+ interfaces): $500K-$2M
Development and engineering typically account for 35% of total cost. Don't underestimate vendor fees (marketplace listing, API access), testing and certification (conformance testing, security audits), and ongoing maintenance (10% of build cost annually).
Getting Started
The path to EHR integration is well-worn — thousands of healthtech companies have walked it before you. The keys to success: start with one EHR vendor (preferably Epic), use FHIR APIs where possible, invest in security from day one, and plan for the vendor review timeline.
For foundational context, see our guides on HL7, FHIR, and Healthcare Interoperability. For integration engine selection, see our Mirth Connect Guide.
Need help with EHR integration? Our team has integrated with Epic, Oracle Health, MEDITECH, and athenahealth across dozens of healthcare organizations.