We have built over 20 healthcare applications. The pattern is unmistakable: every client who deferred agent architecture to V2 ended up spending 4-6x more to retrofit it than it would have cost to include it from day one. Some never shipped it at all because the retrofit was too painful.
This is not a pitch to over-engineer your MVP. It is the opposite. We are arguing that one well-chosen agent — built into your architecture from sprint 1 — actually simplifies your product, accelerates your roadmap, and costs surprisingly little when done at the right time.
The Retrofit Tax — Why V2 Agent Integration Costs 6x More
Adding an agent to an existing healthcare product is not like adding a new feature. It is like adding a nervous system to a body that was built without one. Here is what actually happens when teams try to bolt on agent capabilities after the fact.

The Data Model Has to Change
An agent needs structured, queryable data to reason over. Most MVPs store data in whatever shape the UI requires — denormalized, UI-coupled, and often inconsistent. Retrofitting means migrating your data model to support both the existing UI and the agent's needs. In healthcare, this means moving toward FHIR-aligned resources, which touches every endpoint, every database query, and every frontend component.
At MVP stage, you choose FHIR-aligned data models from the start. No migration needed. The cost difference is zero at design time versus weeks of migration later.
Orchestration Has to Be Added
Agents need an orchestration layer — something that manages tool calls, handles retries, maintains conversation state, and routes between autonomous execution and human review. In an existing product, this layer has to be inserted between your API and your business logic without breaking either. Every existing endpoint becomes a potential tool the agent can call, which means every endpoint needs proper error handling, idempotency, and structured responses.
At MVP stage, you build your endpoints as agent-callable tools from day one. They return structured responses, handle errors gracefully, and are idempotent by default. These are good API practices anyway — the agent just forces you to follow them.
Auth and Permissions Need Restructuring
An agent acts on behalf of users, which means your auth system needs to support delegation. The agent needs its own identity, scoped permissions, and audit trails that distinguish between "the user did this" and "the agent did this on behalf of the user." In healthcare, this is not optional — HIPAA requires knowing exactly who accessed what and why.
Retrofitting delegated auth into an existing system is one of the most dangerous changes you can make. It touches every protected endpoint and every audit log. In practice, at you design your auth with agent delegation from the start — adding maybe two days of work to your auth implementation.
Compliance Testing Starts Over
If your healthcare product has gone through any compliance review — SOC 2, HIPAA risk assessment, or payer certification — adding an agent means re-doing significant portions of that work. The agent introduces new data flows, new access patterns, and new risk vectors that your existing compliance documentation does not cover.
Notably, at your first compliance review includes the agent. No re-work, no supplemental assessments, no second round of penetration testing.
What "Agent-Ready" Architecture Actually Means
When we say "include agent architecture from day one," we do not mean building a fully autonomous AI system in your MVP. We mean making five specific architectural decisions that cost almost nothing at build time but save enormous effort later.
Decision 1: FHIR-Aligned Data Models
Store your core clinical and operational data in FHIR-aligned structures. You do not need a full FHIR server — just align your database schemas with FHIR resource types. Patient, Encounter, Observation, Claim. When your agent needs to reason about a patient's history, it can query structured resources instead of parsing UI-specific data blobs.
Cost at MVP stage: essentially zero. You are choosing one data model over another. The FHIR-aligned model is actually simpler because it follows an established standard instead of inventing your own schema.
Decision 2: Structured API Responses
Every API endpoint returns structured, self-describing responses. Not just the data, but metadata: what operation was performed, what the result was, what errors occurred. This is the difference between returning a 200 with a blob of JSON and returning a response that an agent (or a developer, or a monitoring system) can reason about.
Specifically, cost stage: about one day. You create a response wrapper and use it everywhere.
Decision 3: An Event Bus
Emit domain events for significant state changes. Patient created, appointment scheduled, claim submitted, eligibility verified. You do not need Kafka or RabbitMQ — a simple in-process event bus or a Postgres LISTEN/NOTIFY setup is enough. The agent subscribes to relevant events and can react to them.
Cost at MVP stage: one to two days. A simple event bus is maybe 100 lines of code.
Decision 4: A Compliance Logger
Log every data access and every decision with structured metadata: who, what, when, why, and at what confidence level. For your MVP without an agent, the "who" is always a human user and the confidence is always 100%. When you add the agent, you change nothing — the agent's actions go through the same logger with its own identity and confidence scores.
In practice, cost stage: one day. You are building audit logging anyway for HIPAA. This just makes it structured instead of free-text.
Decision 5: A Human-in-the-Loop Router
Build a simple task queue where automated processes can escalate decisions to humans. In your MVP, this might just be a notification system or a task list. When the agent arrives, it uses the same queue to escalate low-confidence decisions. The UI already exists. The workflow already exists. The agent just becomes another source of tasks.
Notably, cost stage: two to three days if you were not already building a task system. Zero if you were.
Total Additional Cost: About 5,000 Dollars and One Week
Five architectural decisions. One week of additional development. About 5,000 dollars in a typical engagement. Compare that to the 30,000 to 50,000 dollar retrofit that takes 8-12 weeks and carries significant risk of breaking existing functionality.
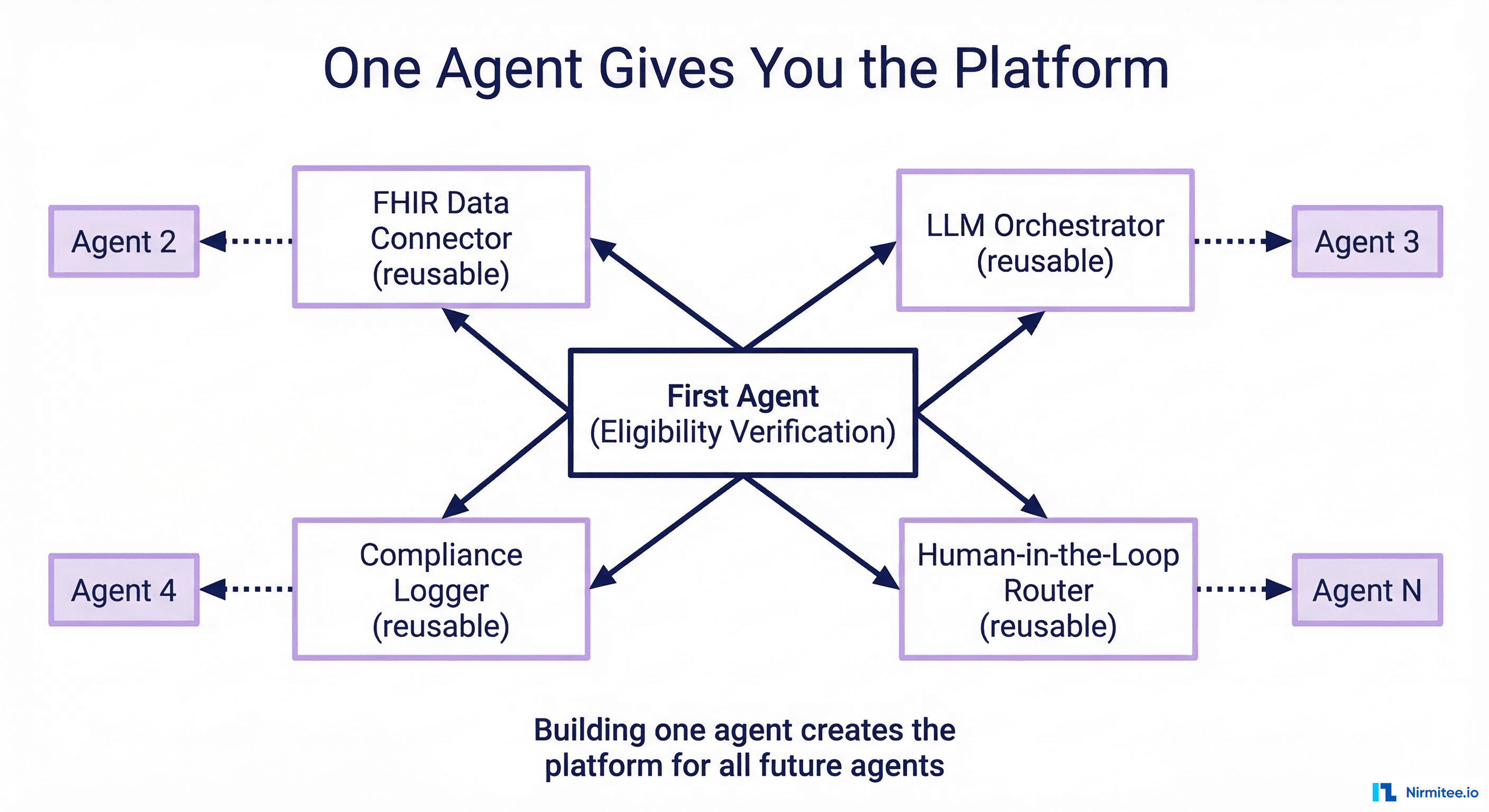
How One Agent Creates the Platform for All Future Agents
Here is the part that most teams miss: your first agent is not just a feature. It is the validation of your entire agent infrastructure. Once you have one agent running in production, adding the second and third is dramatically easier because the hard problems are already solved.
The Reusable FHIR Connector
Your first agent needs to read and write FHIR resources. You build a connector that handles authentication, pagination, error handling, and data validation. Every subsequent agent reuses the same connector. An eligibility verification agent and a prior authorization agent both need to read Patient and Coverage resources — same connector, different workflows.
The LLM Orchestrator
Your first agent needs to call an LLM, parse structured responses, handle rate limits, manage costs, and retry on failures. You build an orchestrator that handles all of this. Every subsequent agent plugs into the same orchestrator. You have one place to manage API keys, monitor costs, switch between models, and enforce token limits.
The Compliance Logger
Your first agent generates audit logs with reasoning chains and confidence scores. The logging infrastructure, the audit dashboard, and the compliance reporting are all built for agent one. Agent two and three use the same infrastructure with zero additional compliance work.
The HITL Router
Your first agent escalates low-confidence decisions to humans. The escalation UI, the notification system, and the feedback loop (where human overrides improve future agent confidence) are all built for agent one. Notably, every uses the same escalation path. Your clinical staff learns one workflow for reviewing agent decisions, not a different workflow per agent.
The Investor Pitch Advantage
If you are raising capital for a healthcare startup, agent-ready architecture is a material differentiator. Here is why investors care.
Defensibility. "We have agent-ready architecture" means your product can evolve with AI capabilities without expensive rewrites. Competitors who built traditional architectures will spend quarters catching up — quarters where you are shipping agent features they cannot.
Marginal cost of new features. Each new agent you add costs less than the previous one because of shared infrastructure. Your cost curve for new capabilities is declining while competitors face a flat or increasing cost curve.
Enterprise readiness. Enterprise healthcare buyers are starting to ask about AI strategy in RFPs. "Our architecture supports agentic AI with built-in compliance logging and human-in-the-loop oversight" is a concrete answer to a question your competitors will fumble.
Talent efficiency. Agent-ready architecture means your engineering team spends time on domain-specific agent logic, not on infrastructure. You need fewer engineers to ship more capabilities, which directly improves your unit economics.
The Agent-Ready MVP Checklist
If you are building a healthcare product right now, here is exactly what to include in your MVP for agent readiness. Print this list and tape it to your monitor.
- Data layer: FHIR-aligned resource schemas for your core entities (Patient, Encounter, Observation, Claim, Coverage — whichever are relevant to your domain)
- API layer: Structured response envelopes with operation metadata, consistent error formats, and idempotent mutations
- Event system: Domain event emission for state changes, even if you only have one subscriber initially
- Auth system: Service account support with scoped permissions and delegated-action audit trails, separate from user auth
- Compliance: Structured audit logging with who/what/when/why fields, not just free-text logs
- Escalation: A task queue or notification system where automated processes can route decisions to humans
- One agent: Pick your highest-volume, most-repetitive workflow and build a single agent for it. Eligibility verification is a common first choice — high volume, well-defined rules, clear success metrics
- Monitoring: Agent-specific metrics — decisions per hour, confidence distribution, escalation rate, human override rate
Choosing Your First Agent
Not every workflow is a good candidate for your first agent. The ideal first agent has these characteristics:
High volume. It processes enough transactions that the efficiency gain is measurable. Eligibility verification, appointment reminders, and claims status checks are good candidates. Rare, complex clinical decisions are not.
Well-defined success criteria. You can objectively measure whether the agent got it right. "Was the patient eligible: yes or no" is measurable. "Was the clinical note comprehensive" is subjective and harder to evaluate.
Low risk of harm. If the agent gets it wrong, the consequence is inconvenience, not patient harm. Checking eligibility wrong means a phone call to fix it. Getting a drug interaction wrong means potential patient harm. Start with administrative workflows, not clinical decisions.
Human bottleneck. The workflow is currently bottlenecked by human processing time, not by system limitations. Your staff spends hours on this task daily. Automating it frees real human capacity.
In our experience across 20+ healthcare applications, the three best first agents are: eligibility verification (high volume, binary outcome, low risk), appointment scheduling optimization (high volume, measurable utilization improvement, low risk), and claims status monitoring (high volume, clear success criteria, frees staff from portal-checking drudgery).
The Cost of Waiting
Every month you operate without agent-ready architecture is a month of technical debt accumulating. Your data models are hardening around UI-specific shapes. Your APIs are growing without structured response patterns. Your auth system is solidifying without delegation support. Your compliance documentation is being written without agent considerations.
None of this is fatal. All of it is expensive to fix later.
The math is simple. Spend one additional week and 5,000 dollars during your MVP build to include agent-ready architecture. Or spend 8-12 weeks and 30,000-50,000 dollars six months from now to retrofit it — assuming you can afford the disruption to your existing customers and your team's feature roadmap.
We have seen both paths. We have helped clients take both paths. The right answer is obvious, but it requires making the decision now, when the cost is lowest and the optionality is highest.
Your V2 roadmap will thank you. Your investors will notice. And your engineering team will not have to spend a quarter rebuilding what could have been built right the first time.
Building production-grade healthcare AI agents requires careful architecture. Our Agentic AI for Healthcare team ships agents that meet clinical and compliance standards. We also offer specialized Healthcare Software Product Development services. Talk to our team to get started.

