At 2:47 AM on a Tuesday in October, a ventilator in the cardiac ICU of a 400-bed teaching hospital threw an error code. The night nurse — one of three covering 18 patients — silenced the alarm, power-cycled the unit, and reconnected the circuit. The ventilator resumed normal operation for eleven minutes before failing completely.
The patient was manually bagged for fourteen minutes while a replacement unit was located. The replacement came from the NICU two floors down, requiring a respiratory therapist to physically transport it through a locked stairwell because the freight elevator was out of service for — ironically — a maintenance issue of its own.
The patient survived. But those fourteen minutes of manual ventilation during a period of hemodynamic instability contributed to a longer ICU stay, a ventilator-associated complication, and an additional $47,000 in care costs. The root cause was not a freak mechanical failure. It was a missed preventive maintenance inspection that had been deferred three times over five months because the biomed team was understaffed and had no system to flag escalating risk.
This is not a rare event. It is Tuesday.
The Scope of a Problem Nobody Quantifies
Here is the uncomfortable truth about hospital equipment downtime: almost nobody measures it systematically, and the organizations that do measure it are alarmed by what they find.
Hospital administrators track bed occupancy rates to the decimal point. They monitor patient throughput, readmission rates, and staff-to-patient ratios with sophisticated dashboards. But ask most hospital COOs how many hours of unplanned equipment downtime their facility experienced last quarter, and you will get a blank stare or a guess.
This blind spot exists because equipment downtime lives in the gap between clinical operations and facilities management — a no-man's-land where neither group has full visibility, full accountability, or full data.
The numbers, when someone does bother to count, are staggering:
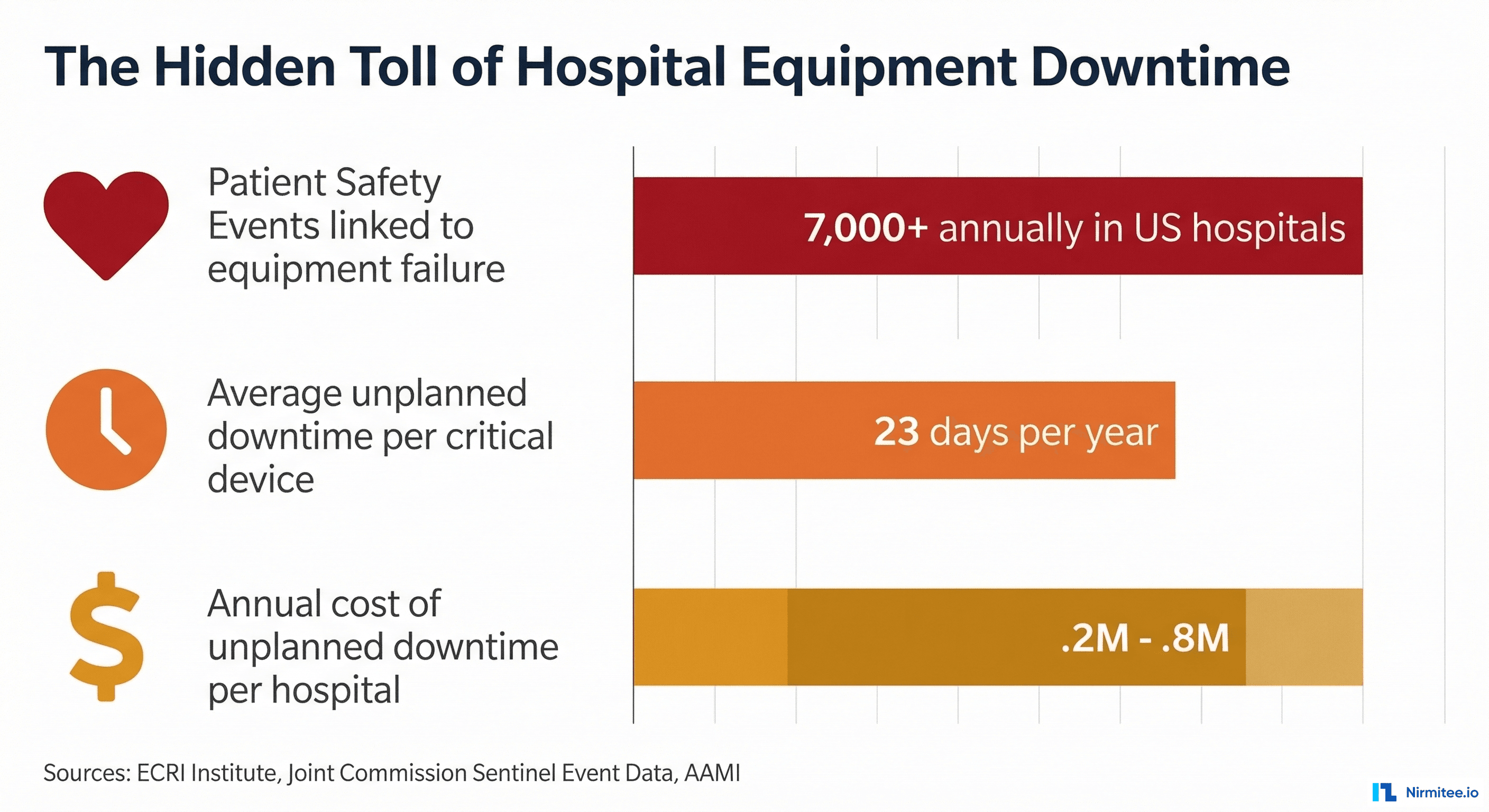
- ECRI Institute has consistently ranked equipment-related issues among the top 10 health technology hazards for over a decade. Their 2025 analysis identified infusion pump failures, ventilator malfunctions, and patient monitor disconnections as contributing factors in over 7,000 adverse events annually across US hospitals.
- The Joint Commission's Sentinel Event database shows that equipment-related factors contribute to approximately 4–6% of all reported sentinel events — roughly 200–350 events per year that result in death, permanent harm, or severe temporary harm.
- AAMI (Association for the Advancement of Medical Instrumentation) research indicates the average critical medical device in a US hospital experiences 23 days of unplanned downtime per year — a number that has not improved significantly in the past decade despite advances in device technology.
- The financial impact ranges from $1.2 million to $3.8 million annually per hospital, depending on size and acuity level, when you account for emergency repairs, overtime labor, rental equipment costs, extended patient stays, and the revenue lost from cancelled or delayed procedures.
But these numbers — as troubling as they are — only capture what gets reported. The vast majority of equipment downtime events never make it into a formal incident report. The nurse who spends twenty minutes searching for a working pulse oximeter does not file a report. The surgeon who delays a case by forty-five minutes because the electrosurgical unit was not properly maintained does not fill out a form. The respiratory therapist who jury-rigs a workaround for a malfunctioning CPAP does not log it anywhere.
The real scope of hospital equipment downtime is an iceberg problem. What gets reported is the visible tip. What actually happens on the floor — every shift, every day — is the massive, submerged bulk that nobody talks about because there is no system to capture it.
How One Equipment Failure Becomes a Patient Safety Event
Equipment downtime does not harm patients through a single dramatic failure. It harms them through cascading consequences — a chain of small disruptions that compound until clinical care is compromised.
Understanding this cascade is critical because it reveals why traditional approaches to equipment management (fix it when it breaks) are fundamentally inadequate for healthcare environments.
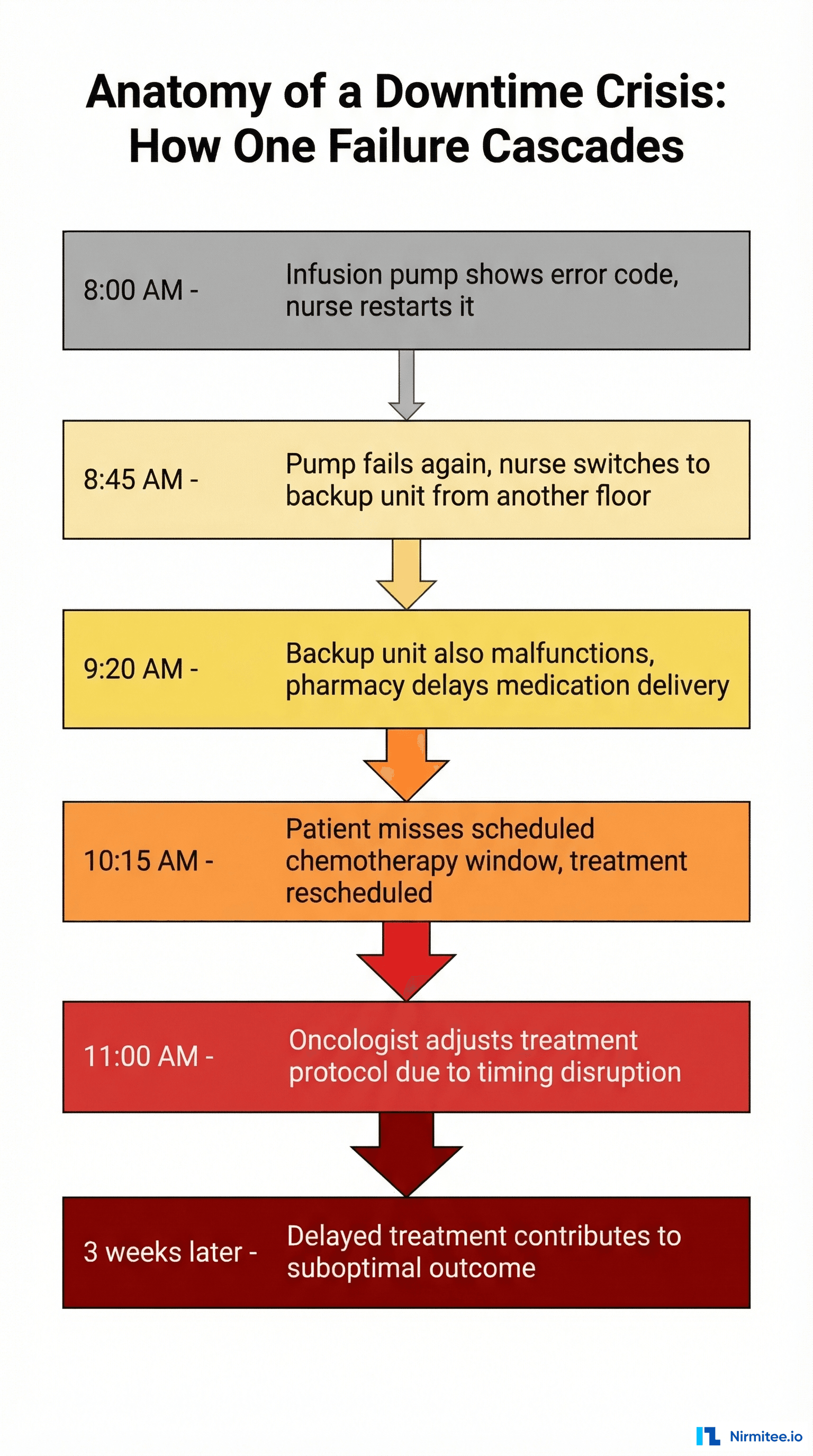
The cascade follows a predictable pattern:
Stage 1: Initial Failure. A device malfunctions. In some cases, the failure is sudden and complete — a ventilator stops delivering breaths, a defibrillator will not charge. More often, it is a degraded performance that triggers nuisance alarms, intermittent errors, or inconsistent output. Staff respond by restarting, resetting, or switching to a workaround.
Stage 2: The Workaround. Clinical staff are resourceful by necessity. When equipment fails, they adapt — borrowing from another unit, using a manual alternative, adjusting the care plan. These workarounds keep patients safe in the short term but introduce new risks: the borrowed equipment may have different settings or interfaces, the manual alternative increases cognitive load on already-burdened staff, and the adjusted care plan may be suboptimal.
Stage 3: Resource Drain. Finding replacement equipment, coordinating with biomed, documenting the failure, and communicating the change to the care team all consume time and attention. In a high-acuity environment, this resource drain does not just affect the patient with the failed equipment — it affects every other patient whose nurse or therapist is now diverted from their care.
Stage 4: Clinical Consequence. The cascade reaches the patient in one of several ways:
- Treatment delay: A chemotherapy infusion is postponed because the pump failed. A surgical case is pushed back because the imaging equipment was not available. A medication dose is late because the pharmacy's automated dispensing system was down.
- Suboptimal care delivery: A ventilator is set to a generic mode instead of the patient-specific protocol because the replacement unit has different capabilities. A patient is monitored with spot checks instead of continuous telemetry because there are not enough working monitors.
- Diagnostic gap: A lab result is delayed because the analyzer was down. A portable X-ray is unavailable, so the patient is transported to radiology — increasing fall risk, infection exposure, and staff workload.
- Near-miss or adverse event: In the worst cases, the cascade leads to direct patient harm — a missed deterioration, a dosing error, a delayed resuscitation.
Stage 5: The Invisible Aftermath. The patient's outcome is affected, but the connection to equipment downtime is rarely documented in the medical record. The discharge summary notes "prolonged ICU course" or "treatment modification due to clinical factors" — not "our infusion pump broke and nobody had maintained it." The causal link between equipment failure and patient outcome is severed at the documentation level, making it invisible to quality improvement teams, regulatory auditors, and hospital leadership.
Four Clinical Scenarios That Happen Every Day
These are not worst-case hypotheticals. These are Tuesday. They happen in hospitals of every size, in every state, with predictable regularity. The only variable is whether anyone notices.

Scenario 1: The ICU Ventilator
A mechanically ventilated patient in the surgical ICU develops auto-PEEP because the ventilator's expiratory valve is not cycling properly. The condition builds gradually — the device does not alarm because the parameters are technically within set limits. By the time the respiratory therapist identifies the problem during routine assessment, the patient's hemodynamics have deteriorated.
The root cause: the expiratory valve was due for replacement 6 weeks ago. The work order was generated but deprioritized because the biomed department was handling 47 open work orders with a team of three technicians. There was no system to flag this particular work order as high-risk based on the device's criticality classification.
What systematic asset management changes: Criticality-based work order prioritization ensures life-support equipment maintenance is never deprioritized. Automated escalation alerts the department head when a critical PM is overdue by more than 48 hours.
Scenario 2: The Infusion Pump Fleet
A 300-bed hospital operates a fleet of 420 infusion pumps across all units. At any given time, 8–12% are out of service — some in biomed for repair, some awaiting parts, some sitting in soiled utility rooms with dead batteries because nobody tracks their location. Nursing staff on the night shift routinely spend 15–20 minutes at the start of each shift locating functional pumps.
One evening, a nurse pulls a pump from a crash cart on another floor because it was the closest available unit. That crash cart is now missing a pump. Two hours later, a code is called on that floor. The code team arrives to find an incomplete crash cart.
What systematic asset management changes: Real-time location tracking shows exactly where every pump is and its operational status. Par-level alerts notify materials management when available pump inventory on any unit drops below the safety threshold. Crash cart equipment is flagged as non-removable in the system.
Scenario 3: The Defibrillator That Was Not Ready
During a rapid response, the team discovers that the defibrillator on the unit has a depleted battery. The device was last used three weeks ago and returned to its docking station, but the docking station's charging contact was faulty — a known issue with this model that the manufacturer addressed in a service bulletin the hospital never acted on.
The team uses the defibrillator from the adjacent unit, adding 90 seconds to the response time. In cardiac arrest, survival probability decreases by approximately 10% for every minute of delay in defibrillation.
What systematic asset management changes: Manufacturer service bulletins are tracked against the asset register, generating automatic work orders. Battery health monitoring with threshold alerts ensures devices are always charge-ready. Daily automated readiness checks replace the manual log that nobody was filling out.
Scenario 4: The Silent Monitor
A telemetry patient on a step-down unit has their monitor alarm silenced by a nurse who is managing alarm fatigue across six monitored patients. The monitor subsequently loses signal due to a loose lead, but no alarm sounds because the alarm was silenced, not paused. The patient's rhythm deteriorates over a 40-minute window with no clinical notification.
The monitor is seven years old — past its recommended replacement cycle. Its alarm management software is two versions behind the current release because the hospital's biomed team did not have the capacity to perform the firmware update that the manufacturer released eighteen months ago.
What systematic asset management changes: Asset lifecycle tracking flags devices past their recommended replacement date. Firmware and software update tracking generates work orders when critical updates are released. Alarm management system performance is tracked as a maintenance metric, not just a clinical workflow issue.
Why This Keeps Happening: A Root Cause Analysis
If hospital equipment downtime is predictable, measurable, and preventable — and it is all three — then why does it persist at the scale it does? The answer is not a single failure. It is a system of interconnected root causes that reinforce each other.

The Reactive Maintenance Trap
Most hospitals operate in a reactive maintenance model — they fix equipment when it breaks. This feels efficient because you are only spending money when there is a visible problem. In reality, it is the most expensive and dangerous approach:
- Emergency repairs cost 3–5x more than planned maintenance because of overtime labor, expedited parts shipping, and rental equipment during downtime
- Reactive maintenance shortens equipment lifespan by 25–40% because small issues that would have been caught in a PM inspection become catastrophic failures
- Every reactive repair is an unplanned disruption to clinical operations — by definition, it happens at the worst possible time
The trap is self-reinforcing: because the biomed team is constantly fighting fires (reactive repairs), they have no capacity to implement preventive programs, which means more equipment breaks unexpectedly, which means more fires to fight.
The Visibility Gap
You cannot manage what you cannot see. In most hospitals, asset data lives in disconnected silos:
- Finance tracks depreciation in the ERP system
- Biomed tracks maintenance in a spreadsheet or legacy CMMS
- Nursing tracks equipment availability through word of mouth and personal knowledge
- Materials management tracks inventory by department but not by device status
- Risk management tracks incidents but cannot connect them to equipment maintenance histories
No single person or system has a complete picture of which devices are where, what condition they are in, when they were last serviced, and what risk they pose to patients if they fail. This fragmentation makes it impossible to make proactive, risk-informed decisions about equipment management.
The Budget Disconnect
Hospital capital and operating budgets are set annually, often 12–18 months in advance. Equipment replacement decisions are made based on age and depreciation schedules rather than actual condition data. Maintenance budgets are among the first to be cut during financial pressure because the consequences of deferred maintenance are delayed and invisible — until they are not.
The cruel irony: every dollar cut from preventive maintenance generates $3–5 in reactive repair costs within 12–18 months. But those costs show up in different budget lines (overtime, rental equipment, extended patient stays), so the connection is never made explicit in financial reporting.
The Staffing Crisis in Biomedical Engineering
The biomedical engineering workforce is aging and shrinking. The average hospital biomed technician is responsible for maintaining 800–1,200 devices. Industry benchmarks recommend 300–500 devices per technician for adequate coverage. This 2–3x overload means:
- Preventive maintenance completion rates hover around 60–70% instead of the 90%+ target
- Low-priority work orders accumulate for months
- Technicians spend more time on emergency repairs than planned maintenance
- There is no capacity for technology upgrades, firmware updates, or process improvement
The Compliance-Only Mindset
Many hospitals approach equipment management as a compliance exercise — do the minimum required to pass Joint Commission surveys. This creates a checkbox culture where the goal is documentation rather than actual equipment reliability. PM inspections become paperwork exercises rather than genuine condition assessments. Equipment is "maintained" on paper but deteriorating in reality.
The 5-Layer Downtime Prevention Framework
Breaking the cycle requires a structured approach that builds capability in layers. Each layer reduces risk incrementally, and the compounding effect creates a resilient system that catches problems before they reach patients.
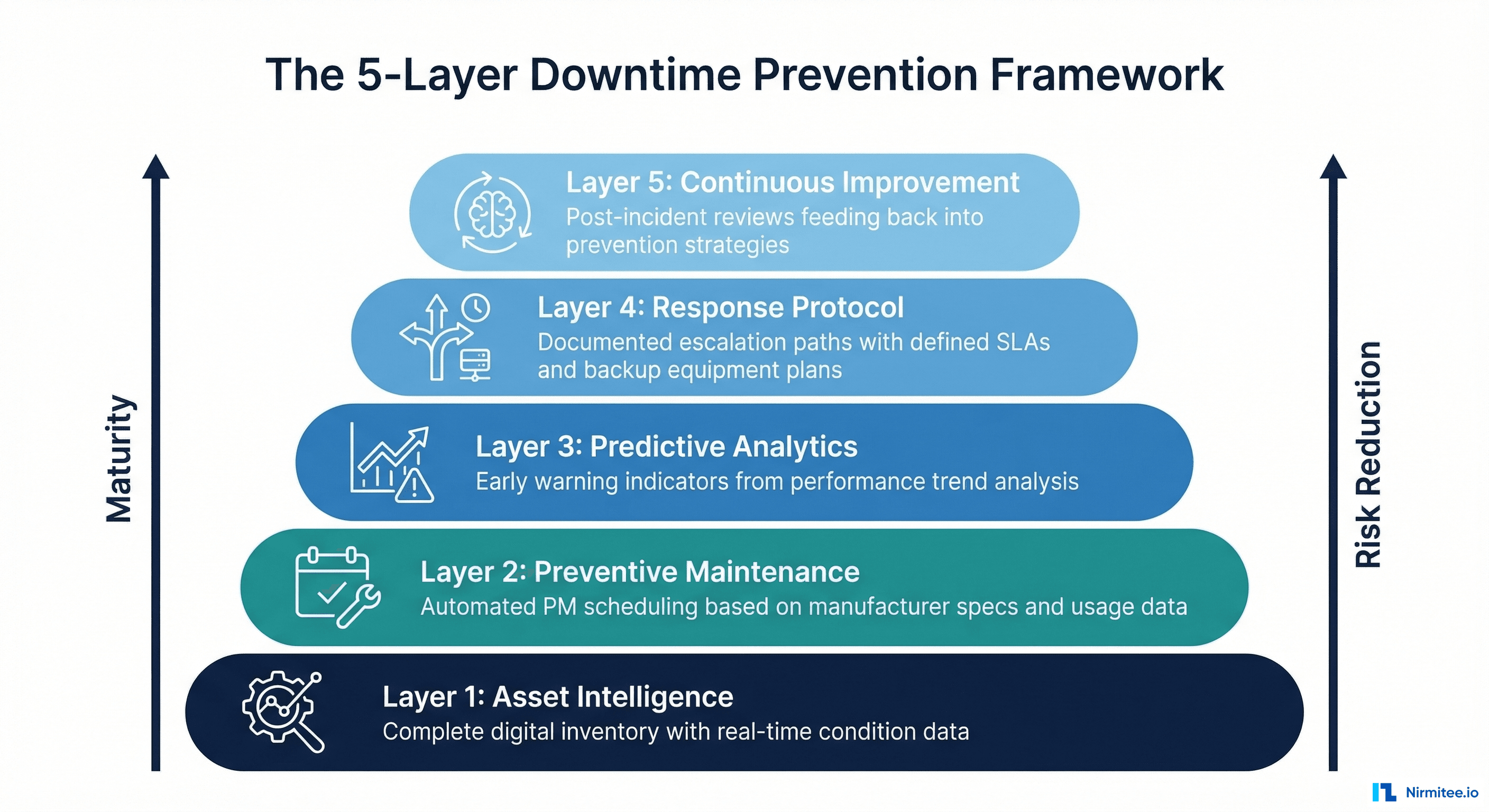
Layer 1: Asset Intelligence
You start by knowing what you have, where it is, and what condition it is in. This is the foundation — without it, every other layer is built on guesswork.
What this means in practice:
- A complete digital asset register covering every medical device, with make, model, serial number, purchase date, warranty status, and criticality classification
- QR code or barcode tagging that allows any staff member to scan a device and see its full history
- Real-time location tracking — at minimum, department-level assignment with movement history; ideally, room-level visibility for high-value and critical devices
- Condition grading: a standardized assessment of each device's current operational status, updated at every maintenance touch and clinical interaction
The outcome: When someone asks "where is the nearest working sequential compression device?" or "which ventilators are due for PM this month?" the answer is instant, accurate, and actionable.
Layer 2: Preventive Maintenance
With asset intelligence in place, you can build a preventive maintenance program that is driven by data rather than calendar pages.
What this means in practice:
- Automated PM scheduling based on manufacturer specifications, regulatory requirements, and usage data — not just "every 6 months regardless of how heavily the device is used"
- Criticality-based prioritization: life-support and high-risk devices are scheduled and tracked with tighter SLAs than low-risk equipment
- Work order management with assignment, tracking, parts documentation, and completion verification
- Escalation protocols that automatically alert supervisors when critical PMs are overdue
- Completion rate tracking as a department KPI — with a target of 90%+ for critical devices and 80%+ overall
The outcome: Equipment is maintained before it fails. The biomed team shifts from firefighting to proactive management. Compliance documentation is generated as a byproduct of actual maintenance work rather than a separate paperwork exercise.
Layer 3: Predictive Analytics
Once you have reliable historical data from Layers 1 and 2, you can begin identifying patterns that predict failure before it occurs.
What this means in practice:
- Trend analysis of repair frequency — a device that has needed three unplanned repairs in six months is sending a clear signal
- Cost-per-device tracking that identifies assets approaching the repair-vs-replace threshold (typically when annual maintenance cost exceeds 40–50% of replacement cost)
- Fleet-level analysis that identifies systemic issues — if 30% of your infusion pump fleet from the same manufacturer is showing the same error code, that is a design issue, not random failure
- Age and condition correlation that supports evidence-based replacement planning instead of arbitrary depreciation-based timelines
The outcome: Capital replacement decisions are made proactively based on data. Equipment is replaced before it becomes a safety risk. Budget requests are supported by evidence rather than anecdote.
Layer 4: Response Protocol
Even with the best prevention, equipment will sometimes fail. Layer 4 ensures that when failure occurs, the clinical impact is minimized through documented, practiced response protocols.
What this means in practice:
- Defined response SLAs by device criticality: life-support equipment gets a 15-minute response, diagnostic equipment gets 2 hours, non-critical equipment gets next business day
- Backup equipment plans: every critical device has a documented backup — where it is, how to deploy it, and who is responsible for maintaining the backup in ready state
- Communication protocols: when a critical device fails, who gets notified, in what order, through what channel
- Temporary workaround documentation: clinician-facing guides for maintaining patient safety during equipment transitions
The outcome: Equipment failure becomes a managed event rather than a crisis. The fourteen-minute gap between ventilator failure and replacement — the gap that started this article — is eliminated because the response is planned, not improvised.
Layer 5: Continuous Improvement
The final layer closes the loop by turning every equipment event — planned or unplanned — into an opportunity to strengthen the system.
What this means in practice:
- Post-incident review for every unplanned downtime event on critical equipment: what failed, why it was not caught by Layers 1–3, and what changes to prevent recurrence
- Monthly equipment reliability dashboards shared with clinical leadership — making downtime visible at the leadership level
- Quarterly root cause analysis of the top 5 equipment-related issues
- Annual equipment management program assessment against benchmarks (AAMI, ECRI, Joint Commission standards)
- Staff feedback loops: frontline clinicians and technicians see the changes that result from their reports, reinforcing a culture of reporting
The outcome: The system gets measurably better over time. Downtime decreases quarter over quarter. The connection between equipment management and patient safety becomes explicit, visible, and valued by the organization.
The Financial Case That Changes Minds
Patient safety should be reason enough to invest in systematic equipment management. In practice, budget decisions require financial justification. Fortunately, the financial case is overwhelming.

Direct Cost Reductions
- Maintenance costs decrease 30–40% when shifting from reactive to preventive. Planned repairs use standard-rate labor, pre-ordered parts at negotiated prices, and scheduled vendor visits — versus overtime labor, expedited shipping, and emergency service calls.
- Equipment lifespan extends 30–50% with proper maintenance. A CT scanner that lasts 12 years instead of 8 years defers a $2–3 million capital expenditure by four years.
- Rental equipment costs drop 60–80%. Hospitals spend $50,000–$200,000 annually on rental equipment to cover devices that are out of service for unplanned repairs. Preventive maintenance dramatically reduces the need for rentals.
- Redundant purchasing decreases 15–25% when departments can see what equipment is actually available and where it is located. The infusion pump that "disappeared" was in the soiled utility room on 4 West — it did not need to be replaced.
Revenue Protection
- Procedure cancellations due to equipment unavailability cost hospitals $5,000–$50,000 per cancelled case in lost revenue, depending on the procedure type. A single cancelled cardiac catheterization generates more lost revenue than an entire year of a device's preventive maintenance.
- OR delays attributable to equipment issues cost $30–$60 per minute in lost utilization. A 45-minute delay while waiting for a functioning electrosurgical unit costs $1,350–$2,700 — for one case, on one day.
- Reduced length of stay: When equipment works reliably, patients receive timely diagnostics and treatment, supporting faster discharge. Even a 0.1-day reduction in average length of stay across a 300-bed hospital represents significant revenue improvement.
Risk Mitigation
- Malpractice and liability exposure related to equipment failure is a growing concern. Plaintiffs' attorneys have become increasingly sophisticated at connecting equipment maintenance records — or the lack thereof — to patient outcomes.
- Regulatory penalties: Joint Commission citations related to equipment management can trigger Conditions of Participation reviews, affecting CMS reimbursement eligibility.
- Insurance premiums: Hospitals with documented, systematic equipment management programs may qualify for reduced professional liability premiums.
Where to Start Tomorrow Morning
If you have read this far and recognized your hospital in these scenarios, here is what you can do immediately — not in six months, not after a capital budget cycle, but this week:
1. Quantify your current state. Pull three numbers: your PM completion rate for critical equipment (ask biomed), your unplanned equipment-related work orders from the last quarter (ask biomed or facilities), and your equipment-related incident reports from the last year (ask risk management). These three numbers will tell you whether you have a smoldering problem or a five-alarm fire.
2. Identify your highest-risk assets. Make a list of every device in your facility that (a) directly sustains patient life, (b) has no backup, or (c) has had more than two unplanned repairs in the last six months. This is your critical vulnerability list. It is probably shorter than you think — which makes it actionable.
3. Start tracking what you are not tracking. Implement a simple system — even if it is a shared spreadsheet initially — to log every instance of equipment downtime, including the clinical impact. Do this for 30 days. The data will make the case for investment more powerfully than any consultant's report.
4. Connect the silos. Get your biomed director, your chief nursing officer, your risk manager, and your CFO in the same room. Present the three numbers from step 1 and the critical vulnerability list from step 2. This conversation — which almost certainly has never happened in your organization — is where change begins.
5. Evaluate purpose-built solutions. A modern hospital asset management system replaces the fragmented spreadsheets, legacy CMMS, and tribal knowledge with a single source of truth. QR-based tracking, automated maintenance scheduling, role-based access, real-time dashboards, and mobile accessibility are not luxury features — they are the minimum viable infrastructure for safe equipment management in 2026.
The Question That Matters
Hospital equipment downtime is not a facilities problem. It is not a biomed problem. It is not a budget problem. It is a patient safety problem that masquerades as all three.
Every hospital in the country has equipment that is overdue for maintenance right now. Every hospital has devices that are past their recommended replacement date. Every hospital has staff who waste time every shift working around equipment that does not work properly.
The difference between hospitals that manage this risk and hospitals that absorb it comes down to a single decision: will you build a system to see the problem, or will you continue to look away?
The fourteen minutes between a ventilator failure and a replacement — the fourteen minutes that change a patient's outcome — are not an inevitability. They are a choice. They are the measurable consequence of every deferred maintenance inspection, every unfilled biomed position, every capital budget that prioritized expansion over reliability, and every leadership meeting where equipment management was not on the agenda.
Those fourteen minutes are waiting in your ICU right now. The only question is whether you will find them before they find your patients.
Share
Related Posts
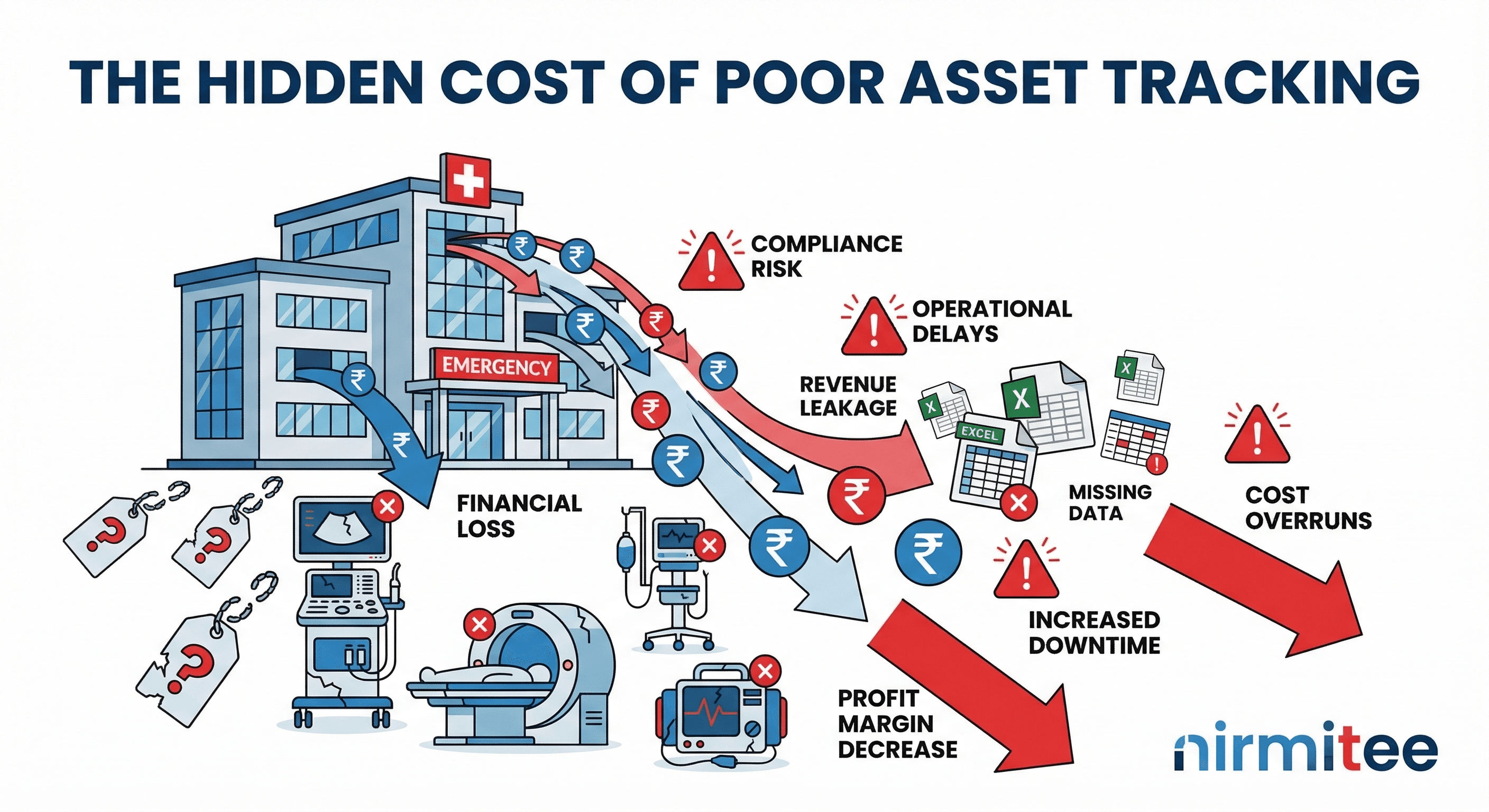
Why Indian Hospitals Lose Crores Every Year to Poor Equipment Tracking
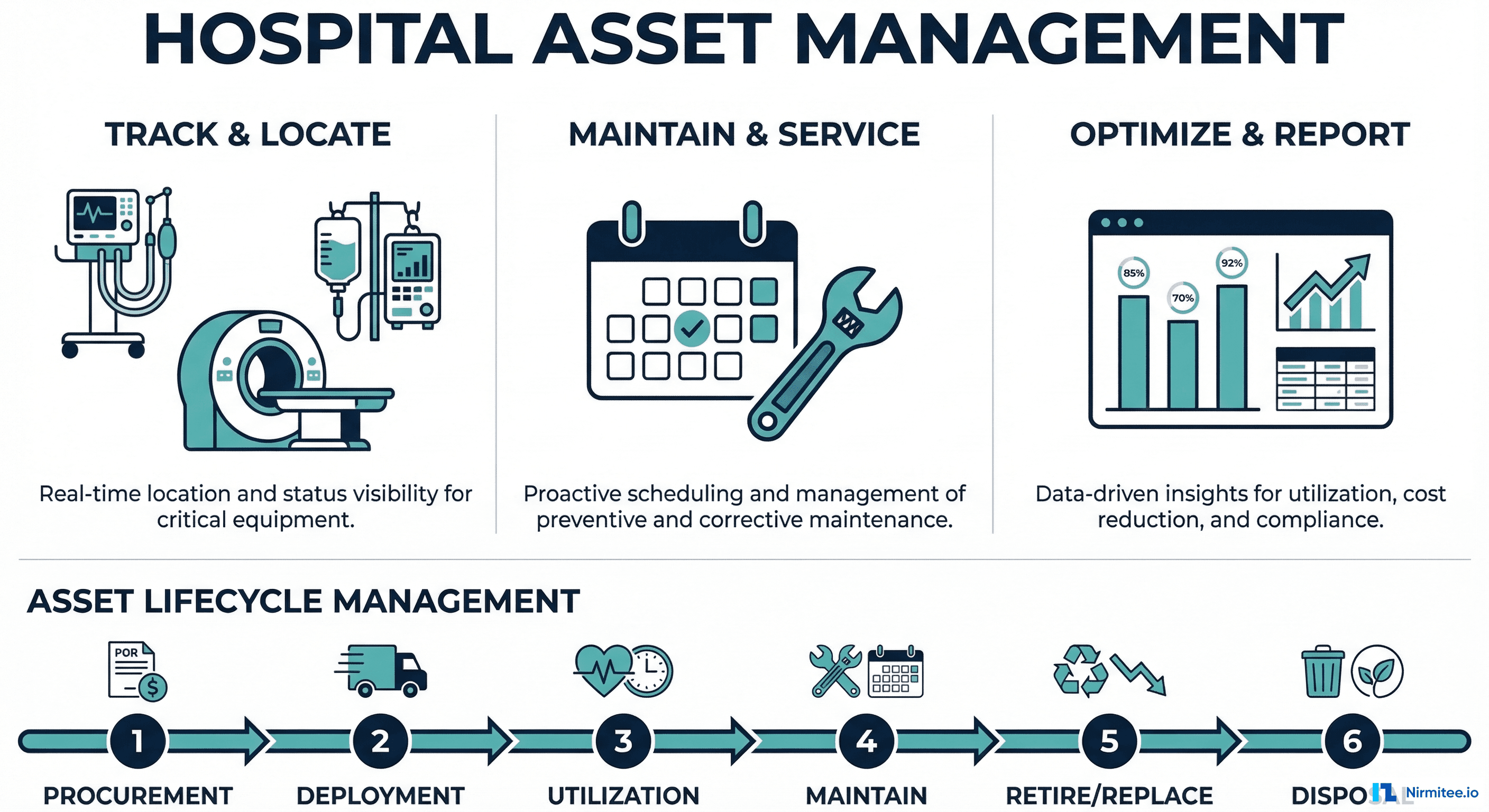
The Complete Guide to Hospital Asset Management in 2026