A 300-bed hospital in Mumbai recently discovered it had purchased 17 duplicate pulse oximeters over two years — not because they needed them, but because nobody knew where the existing ones were. Total wasted spend: ₹8.5 lakhs. This is not an outlier. It is the norm across Indian healthcare.
India's hospital sector manages an estimated ₹2.5 lakh crore worth of medical equipment. Industry studies suggest that 15-25% of this value is leaked annually through poor tracking, unplanned downtime, missed warranties, and ghost assets that exist on paper but cannot be physically located. For a typical 200-bed hospital, this translates to ₹1.5–3 crore in preventable losses every year.
This article breaks down exactly where the money goes, why traditional tracking methods fail at scale, and what hospitals can do to plug these leaks.
The Five Ways Hospitals Bleed Money on Equipment
Poor asset tracking does not show up as a single line item on the balance sheet. It is death by a thousand cuts — spread across departments, hidden in procurement budgets, and buried in emergency repair invoices. Here are the five biggest categories of financial leakage:
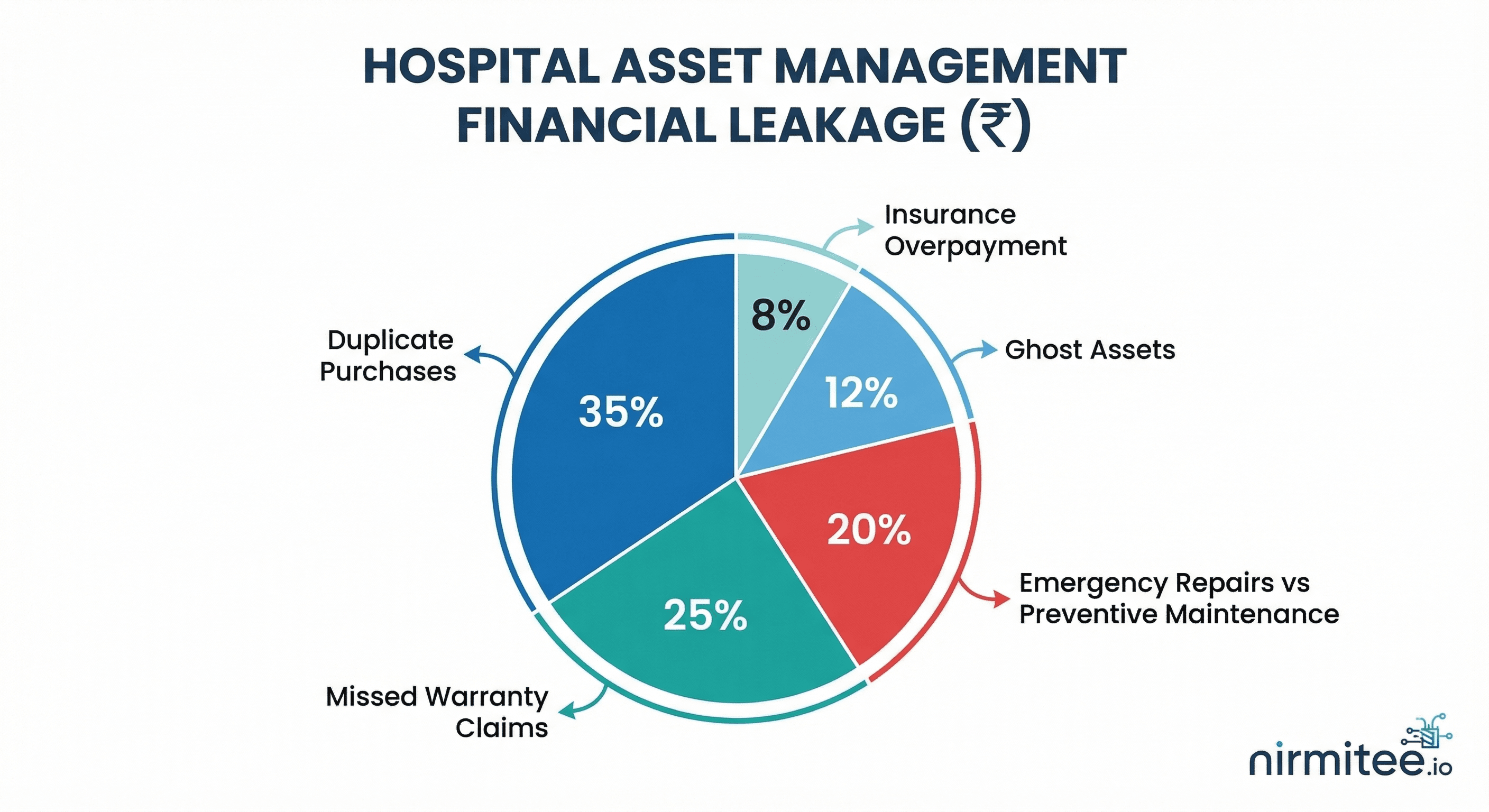
1. Duplicate and Unnecessary Purchases (30-35% of Losses)
This is the single largest source of wasted spend. When hospitals cannot accurately track what equipment they have and where it is located, departments inevitably submit purchase requests for assets that already exist elsewhere in the facility.
Common scenarios:
- Equipment hoarding — Departments hold onto spare equipment "just in case" because they do not trust they can get it when needed. This creates artificial scarcity for other departments.
- Transfer blindness — An infusion pump moved from ICU to the general ward six months ago is still listed under ICU in the Excel sheet. ICU requests a new one. The general ward does not know they have a "borrowed" asset.
- Post-audit surprises — Physical audits routinely find 10-15% more equipment than what records show, and 5-8% of recorded equipment that cannot be physically located.
Real impact: A FICCI-EY study on Indian healthcare found that hospitals with manual tracking systems over-procure equipment by an average of 18-22% compared to digitally-tracked facilities.
2. Emergency Repairs vs. Preventive Maintenance (20-25% of Losses)
The math is simple but devastating: emergency breakdown repairs cost 3-5x more than scheduled preventive maintenance (PM). Yet most Indian hospitals run a reactive maintenance model because they lack the systems to track PM schedules across thousands of assets.
- Breakdown costs — Emergency technician callouts, rush-ordered spare parts, overtime labour, and the clinical cost of equipment downtime during patient care
- Shortened asset life — Equipment that is not regularly maintained degrades 30-40% faster. A ventilator with a 10-year expected life running without proper PM may need replacement in 6-7 years
- Cascading failures — One unmaintained component failure can damage connected systems. A compressor failure in a CT scanner due to missed filter cleaning can damage the entire cooling unit — turning a ₹5,000 PM task into a ₹15 lakh repair
Real impact: Indian hospitals spend an average of 8-12% of their equipment value on maintenance annually. Hospitals with proactive PM programs reduce this to 4-6% while achieving higher equipment uptime.
3. Missed Warranty and AMC Claims (12-15% of Losses)
This is the most frustrating category because it is pure, avoidable waste. Hospitals pay for warranties and Annual Maintenance Contracts (AMCs) but fail to utilise them because:
- No centralised warranty database — Warranty documents are filed in procurement folders, rarely accessible to the biomedical engineering team that actually needs them
- Expiry blindness — Nobody tracks when warranties are about to expire, so hospitals miss the window to claim repairs or negotiate renewals
- AMC under-utilisation — Many AMCs include a fixed number of PM visits and spare parts. Hospitals paying ₹2-3 lakh annually for an AMC often use less than 60% of the entitled services
- Out-of-pocket repairs — Biomedical teams call external technicians for repairs that were covered under existing AMCs — simply because they did not know the AMC existed for that equipment
Real impact: A study of 50 multi-specialty hospitals in India found that ₹12-18 lakhs per year per hospital was spent on repairs that should have been covered under existing warranties or AMCs.
4. Ghost Assets and Insurance Overpayment (8-12% of Losses)
Ghost assets are equipment that exists in your register but not in your facility. They have been condemned, scrapped, stolen, or simply lost — but nobody updated the records. The financial consequences are real:
- Insurance premiums — Hospitals pay insurance on the declared value of all assets on their register. Ghost assets inflate this value, leading to overpayment of premiums by 10-15%
- Tax implications — Depreciation claims on non-existent assets can create audit and compliance risks
- Budget distortion — Capital planning based on inaccurate asset registers leads to poor allocation decisions
Real impact: Physical verification audits at Indian hospitals typically find a 8-12% discrepancy between recorded and actual assets. For a hospital with ₹50 crore in declared equipment value, this means ₹4-6 crore of ghost assets inflating insurance and depreciation costs.
5. Regulatory Non-Compliance Costs (5-10% of Losses)
With NABH accreditation becoming a requirement for CGHS empanelment and insurance tie-ups, non-compliance has direct revenue implications:
- NABH accreditation failure — Hospitals that fail equipment-related NABH standards must reapply, costing ₹5-15 lakhs in fees plus months of lost empanelment revenue
- AERB and PCPNDT compliance — Radiation equipment and ultrasound machines require specific tracking and documentation. Non-compliance carries penalties of ₹1-5 lakhs per violation
- State drug controller audits — Storage equipment (cold chain, pharmacy refrigerators) must maintain calibration records. Failed audits can result in license suspension
Why Excel and Paper Registers Fail
Most Indian hospitals still rely on a combination of paper-based asset registers, Excel spreadsheets maintained by individual departments, and periodic physical verification drives. Here is why this approach breaks down:
| Challenge | Paper/Excel Reality | What Hospitals Actually Need |
|---|---|---|
| Real-time visibility | Last updated 3 months ago; 40% of entries are stale | Live location and status of every asset, updated on every scan |
| Maintenance tracking | PM schedule pinned on a wall; no completion tracking | Automated work orders with SLA tracking and escalation |
| Movement tracking | "I think radiology sent it to ortho last month" | Approved transfer workflows with complete movement history |
| Audit readiness | 2-3 weeks of frantic data collection before every audit | Always-ready audit module with real-time compliance dashboard |
| Warranty management | Paper filed somewhere in procurement; nobody checks | Centralised warranty tracker with expiry alerts |
| Multi-department access | Each department has its own version of the truth | Single source of truth with role-based access control |
The core problem is not the tool — it is the gap between when something happens and when it gets recorded. A nurse moves a syringe pump from Ward A to Ward B. In an Excel system, this might get updated in the monthly stock register — or it might not. In a digital system, the nurse scans a QR code, and the transfer is recorded instantly with full traceability.
The Digital Solution: What to Look For
Hospitals that transition to digital asset management platforms see measurable results within the first quarter. But not all solutions are equal. Here are the features that actually move the needle on cost savings:
QR Code-Based Asset Identification
Every asset gets a unique QR code. Any staff member with a mobile device can scan it to view the asset's complete profile — location, maintenance history, warranty status, calibration records. No more "I don't know where that equipment is."
Automated Preventive Maintenance Scheduling
The system automatically generates maintenance work orders based on OEM schedules, regulatory requirements, and usage patterns. Work orders are assigned to technicians with priority levels, SLA tracking, and escalation protocols. PM completion rates jump from a typical 40-60% to above 90%.
Real-Time Movement Tracking
Every asset transfer — between facilities, between departments — goes through a digital approval workflow. The system maintains a complete movement history, eliminating ghost assets and department-level hoarding.
Comprehensive Audit Module
Department-wise audit sessions with asset condition checks (Pass/Fail/Pending), real-time progress dashboards, and automated discrepancy reports. What used to take 2-3 weeks of preparation now takes 2-3 days.
Role-Based Access Control
Different roles see different things. A department head sees their department's assets. A biomedical engineer sees maintenance work orders across the hospital. A Super Admin sees everything. This ensures data integrity while keeping workflows efficient.
Activity Logging and Audit Trail
Every action — creation, modification, transfer, maintenance update — is logged with the user, timestamp, and details. This is not just for compliance; it creates accountability that naturally reduces mismanagement.
Real Numbers: The ROI of Digital Asset Management
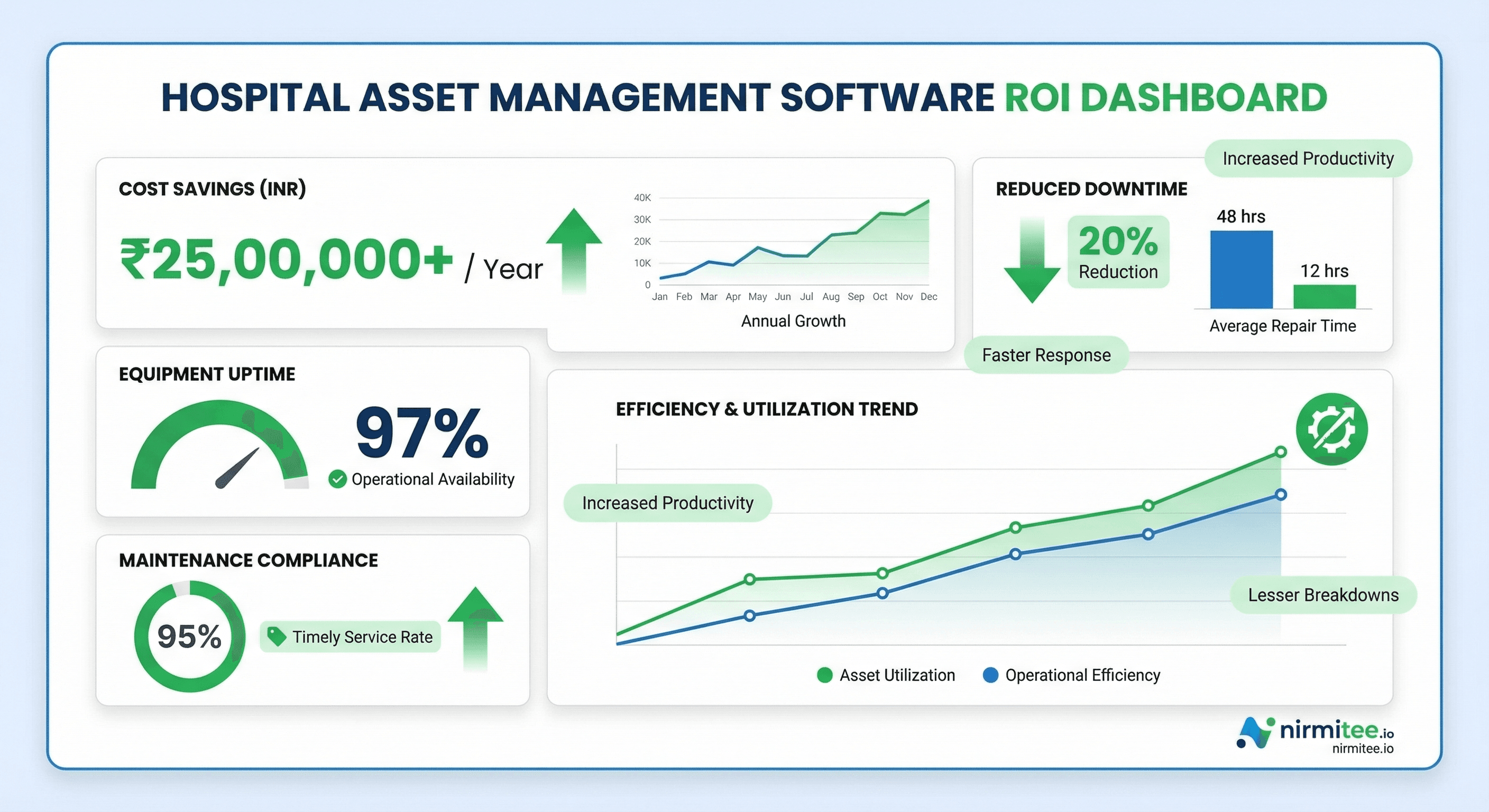
Based on data from hospitals that have implemented digital asset management platforms like Assetly by Nirmitee.io, here are the typical outcomes within the first 12 months:
| Metric | Before (Manual) | After (Digital) | Impact |
|---|---|---|---|
| Duplicate purchases | 18-22% over-procurement | 2-3% variance | ₹40-80 lakhs saved/year (200-bed hospital) |
| PM completion rate | 40-60% | 90-95% | 40% reduction in emergency repairs |
| Equipment downtime | 12-18% annual downtime | 3-5% annual downtime | ₹20-50 lakhs saved in lost revenue recovery |
| Warranty utilisation | 50-60% of entitled claims used | 90-95% utilisation | ₹12-18 lakhs saved on out-of-pocket repairs |
| Ghost assets | 8-12% of register | Less than 1% | ₹5-10 lakhs saved on insurance premiums |
| Audit preparation time | 2-3 weeks | 2-3 days | 80% reduction in staff hours for compliance |
Total typical savings for a 200-bed hospital: ₹1-2 crore per year.
The payback period for implementing a digital asset management platform is typically 3-6 months — making it one of the highest-ROI technology investments a hospital can make.
Getting Started: The 3-Step Approach
Transitioning from paper to digital does not have to be a big-bang transformation. Here is a practical approach:
Step 1: Start with High-Value Assets
Begin by digitising your top 20% of assets by value — typically radiology equipment, operation theatre instruments, ICU ventilators, and laboratory analysers. These represent 80% of your financial exposure and give you the fastest ROI.
Step 2: Establish PM Discipline
Once assets are tracked, set up automated preventive maintenance schedules. This single change typically reduces emergency repair costs by 30-40% within the first six months.
Step 3: Scale Across the Hospital
Expand to all departments, add movement tracking and audit workflows, and integrate with your existing HIS/HMIS. By this point, the system pays for itself and staff adoption is natural because they have seen the benefits.
Conclusion
The crores that Indian hospitals lose to poor equipment tracking are not inevitable. They are the predictable result of managing 21st-century medical technology with 20th-century paper registers and spreadsheets.
Digital asset management is not a luxury for large corporate hospitals — it is a necessity for any facility that wants to control costs, ensure patient safety, maintain regulatory compliance, and extend the useful life of its equipment investments.
Assetly by Nirmitee is purpose-built for the Indian hospital context — from QR code-based tracking and automated maintenance scheduling to NABH-ready audit modules and role-based access control. It is how smart hospitals stop the financial bleeding and start managing their assets like the strategic investments they are.
Stop losing crores. Start tracking smarter. Book a free demo with Nirmitee.io and see exactly where your hospital is leaking money.
Share
Related Posts
NABH Asset Management Compliance: A Complete Guide for Indian Hospitals
The Complete Guide to Hospital Asset Management in 2026
