Mental Health Telemedicine Platform: Secure Video Therapy, AI-Assisted Notes, and Digital Outcome Tracking
Executive Summary
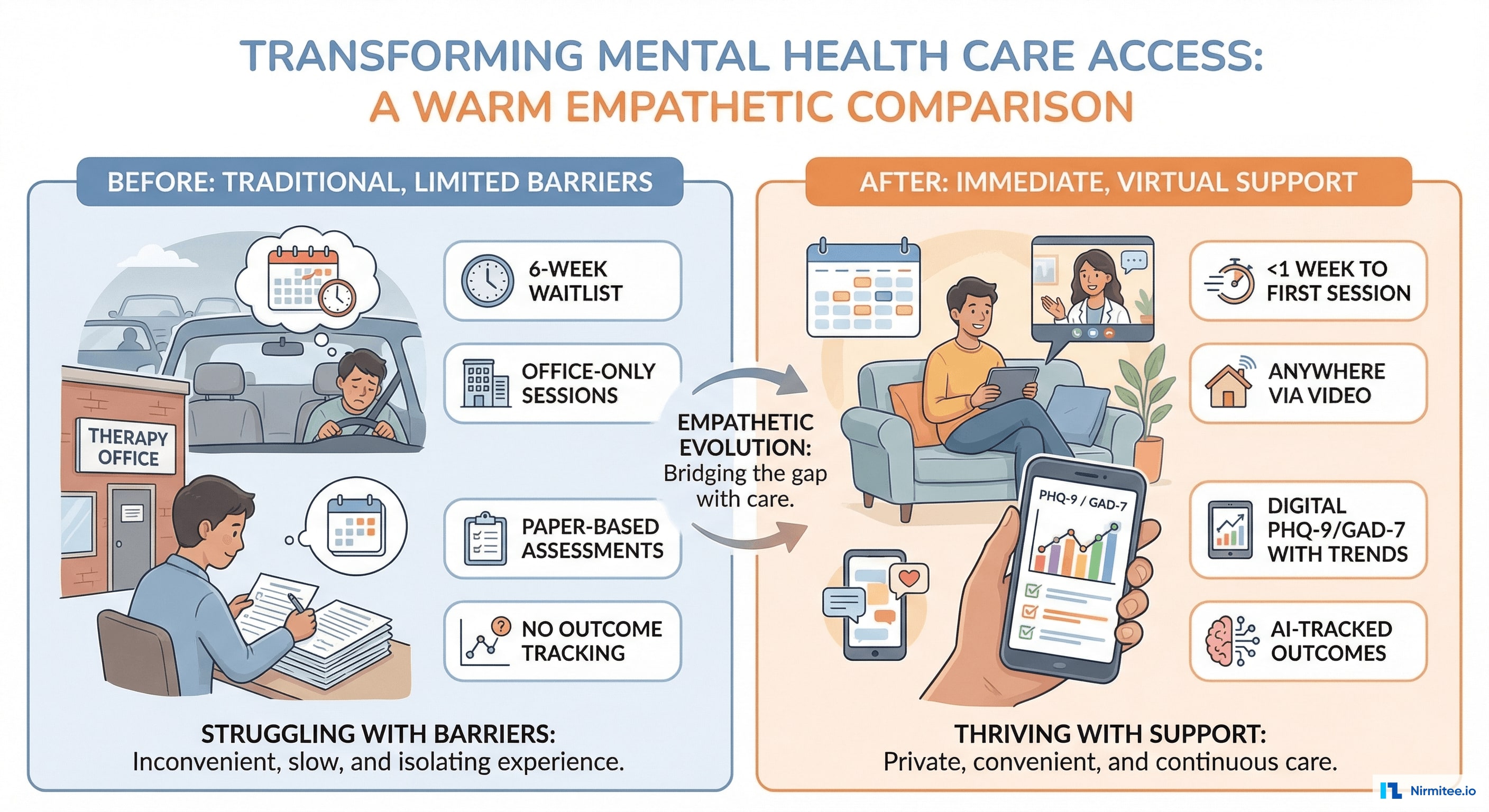
Mental health in America is in crisis: 1 in 5 adults experience mental illness, but over 50% receive no treatment. The barriers are well-known — 6-8 week waitlists, limited office hours, geographic access gaps, stigma, and cost. A US-based behavioral health startup set out to remove every barrier.
Our interoperability solutions ensure seamless data flow across healthcare systems.
We built a complete mental health telemedicine platform — secure video therapy sessions via WebRTC, AI-assisted session documentation, validated digital assessments (PHQ-9, GAD-7, PCL-5), patient outcome tracking with longitudinal trend visualization, between-session tools (mood check-ins, coping exercises, thought journals), and integrated billing for both insurance and self-pay.
Our agentic AI solutions bring autonomous intelligence to healthcare operations.
The platform serves therapists and patients: therapists get a practice management dashboard with AI-generated session notes. Patients get a mobile app with video sessions, mood tracking, coping tools, and continuous connection to their care.
Results: waitlist reduced from 6 weeks to under 1 week, average PHQ-9 scores improved by 56% over 24 sessions, and therapist documentation time dropped from 15 minutes to 3 minutes per session with AI-assisted notes.

The Problem: Mental Healthcare Is Inaccessible
The US faces a severe mental health provider shortage — an estimated shortage of 28,000 practitioners. In rural areas, the nearest therapist may be 2+ hours away. Even in cities, the best therapists have waitlists measured in months. Meanwhile:
- 6-8 week average waitlist for a first therapy appointment in most US metro areas
- 47% of Americans live in a mental health professional shortage area (HPSA)
- Office-only sessions: most therapists see patients 9 AM - 5 PM, Monday-Friday — exactly when working adults can't attend
- Paper-based assessments: PHQ-9 and GAD-7 completed on paper at each visit, hand-scored, results filed in charts with no trending or longitudinal analysis
- Documentation burden: therapists spend 15+ minutes writing session notes after each 50-minute session — eating into their capacity to see more patients
- No between-session support: patients leave the session and have no tools until the next appointment, often 1-2 weeks away
Therapist Dashboard
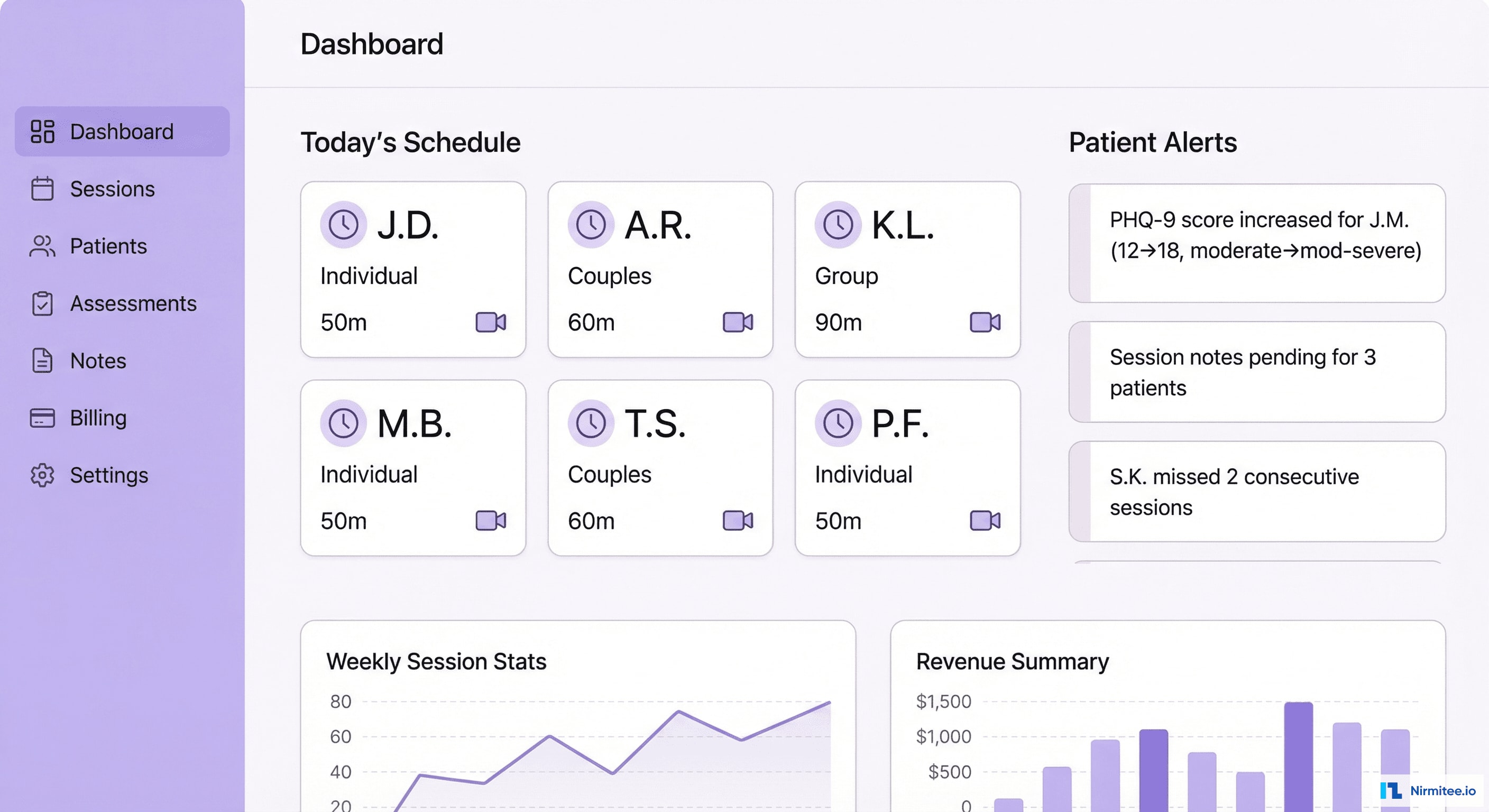
The therapist's command center provides practice-wide visibility:
- Today's schedule: upcoming video sessions with patient initials (privacy-first — no full names in overview), session type (individual, couples, group), and duration
- Patient alerts: proactive notifications — PHQ-9 score increases requiring clinical attention, patients who missed consecutive sessions, unsigned session notes
- One-click session launch: click a scheduled session → video call starts in the browser with patient context loaded automatically
- Practice analytics: weekly session count, revenue (insurance + self-pay), patient retention, outcome trends across caseload
Video Therapy Session
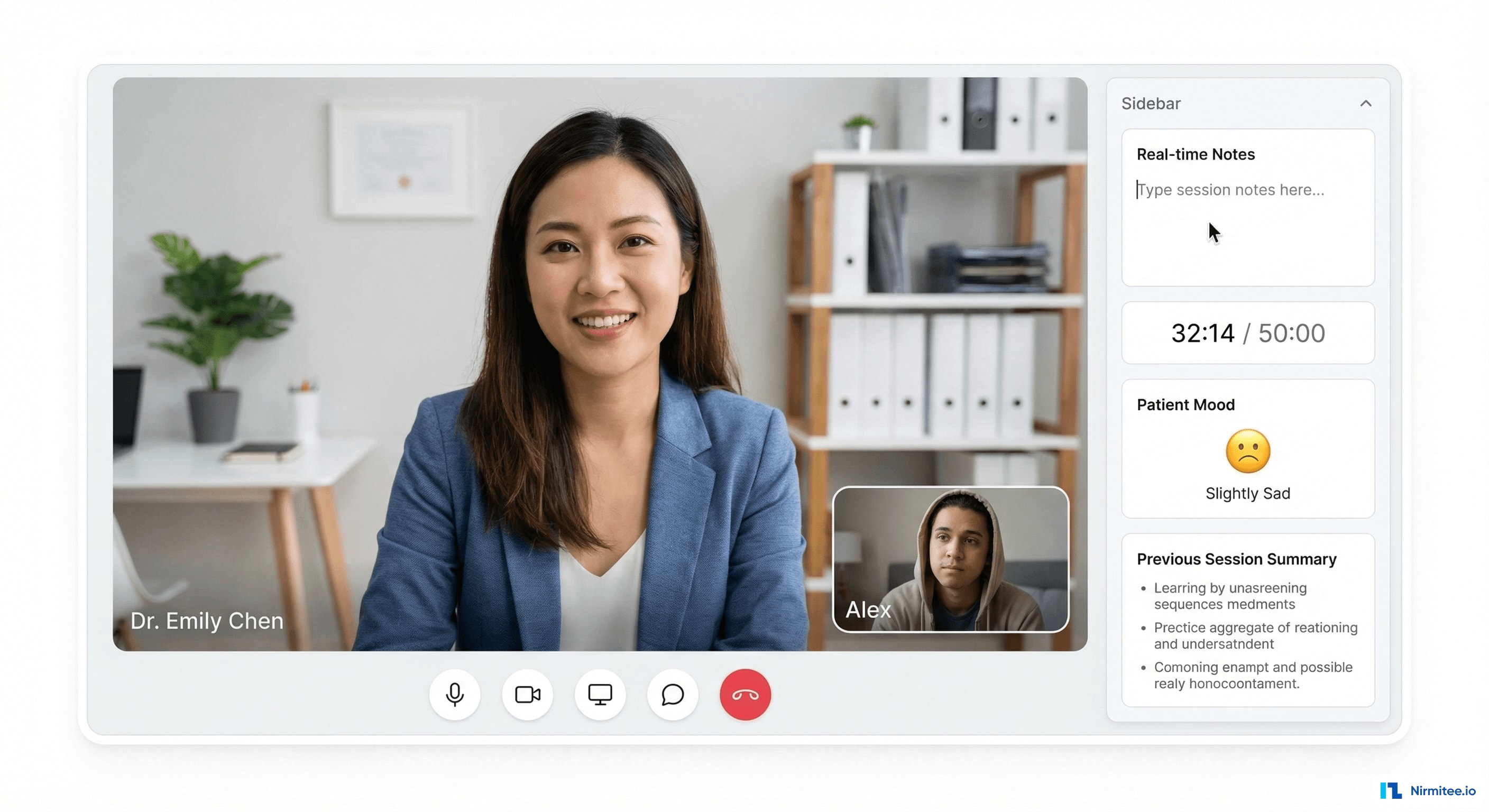
The video session interface is designed for therapeutic presence, not distraction:
- End-to-end encrypted video: WebRTC with TURN/STUN servers for NAT traversal. AES-256 encryption. No recording unless explicitly consented by both parties.
- Minimal chrome: clean video feed dominates the screen. Controls are subtle and accessible without breaking eye contact.
- Session sidebar (collapsible): real-time note-taking area, session timer, patient's pre-session mood check-in result, previous session summary for context
- Screen sharing: therapists can share worksheets, CBT thought records, or psychoeducational materials during session
- Network resilience: adaptive bitrate adjusts video quality based on connection speed. Audio prioritized over video. Auto-reconnect on brief disconnections.
Architecture
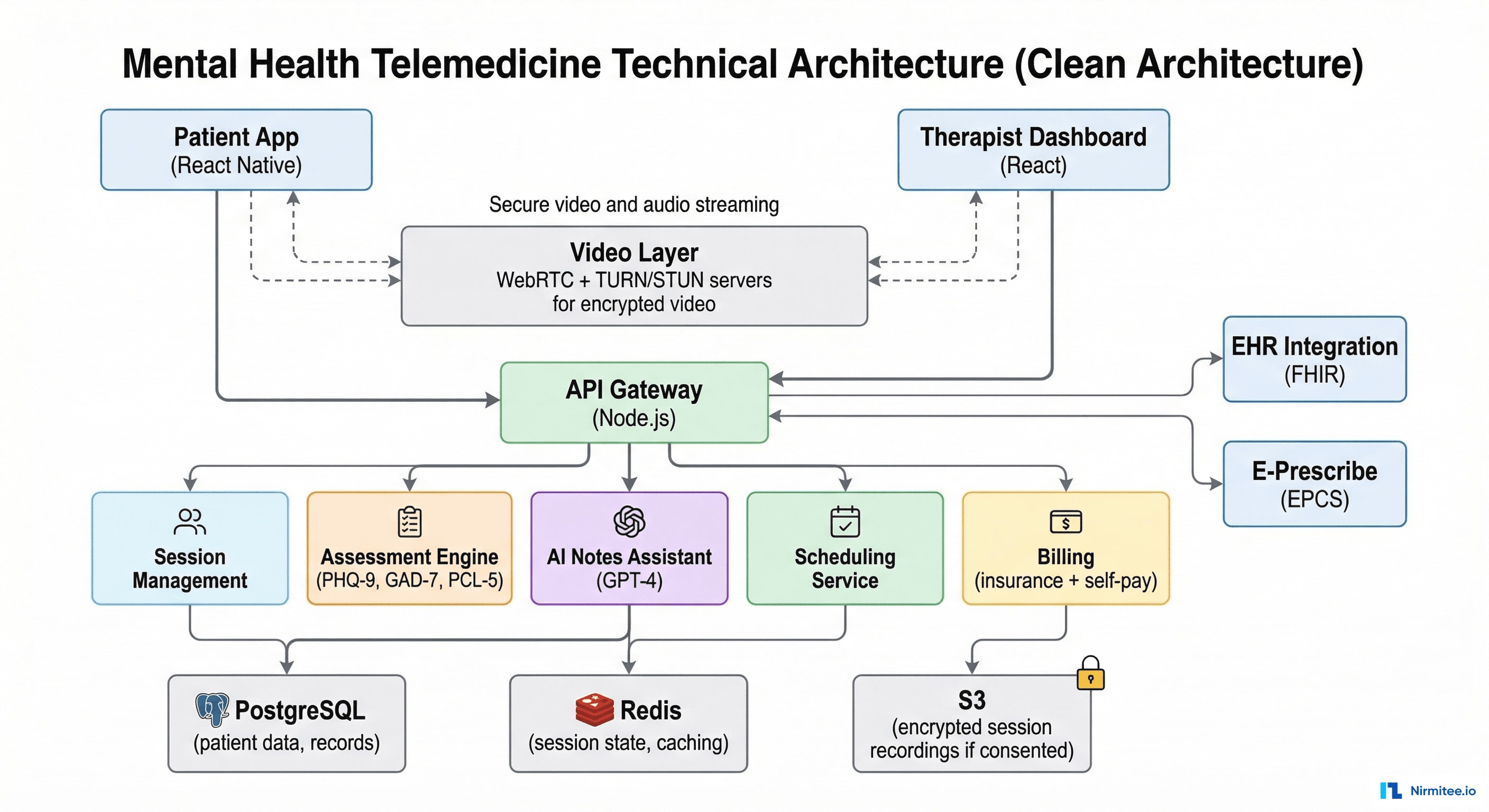
Technology Stack
| Layer | Technology | Purpose |
|---|---|---|
| Patient App | React Native | Video sessions, mood tracking, assessments, coping tools |
| Therapist Dashboard | React + TypeScript | Schedule, notes, assessments, billing, analytics |
| Video | WebRTC + TURN/STUN (Twilio) | End-to-end encrypted video therapy sessions |
| Backend | Node.js (Express) | API gateway, session management, scheduling |
| AI Notes | GPT-4 (Azure OpenAI, HIPAA BAA) | Session note drafting from therapist's quick notes |
| Assessments | Custom engine | PHQ-9, GAD-7, PCL-5 scoring with longitudinal tracking |
| Database | PostgreSQL | Patient records, session data, assessment scores |
| E-Prescribe | Surescripts (EPCS) | Psychiatric medication prescribing for MD/NP providers |
| Billing | Custom + Stripe + clearinghouse | Insurance claims + self-pay processing |
| Infrastructure | AWS (HIPAA BAA) | US data residency, encrypted storage |
Digital Assessments (PHQ-9)
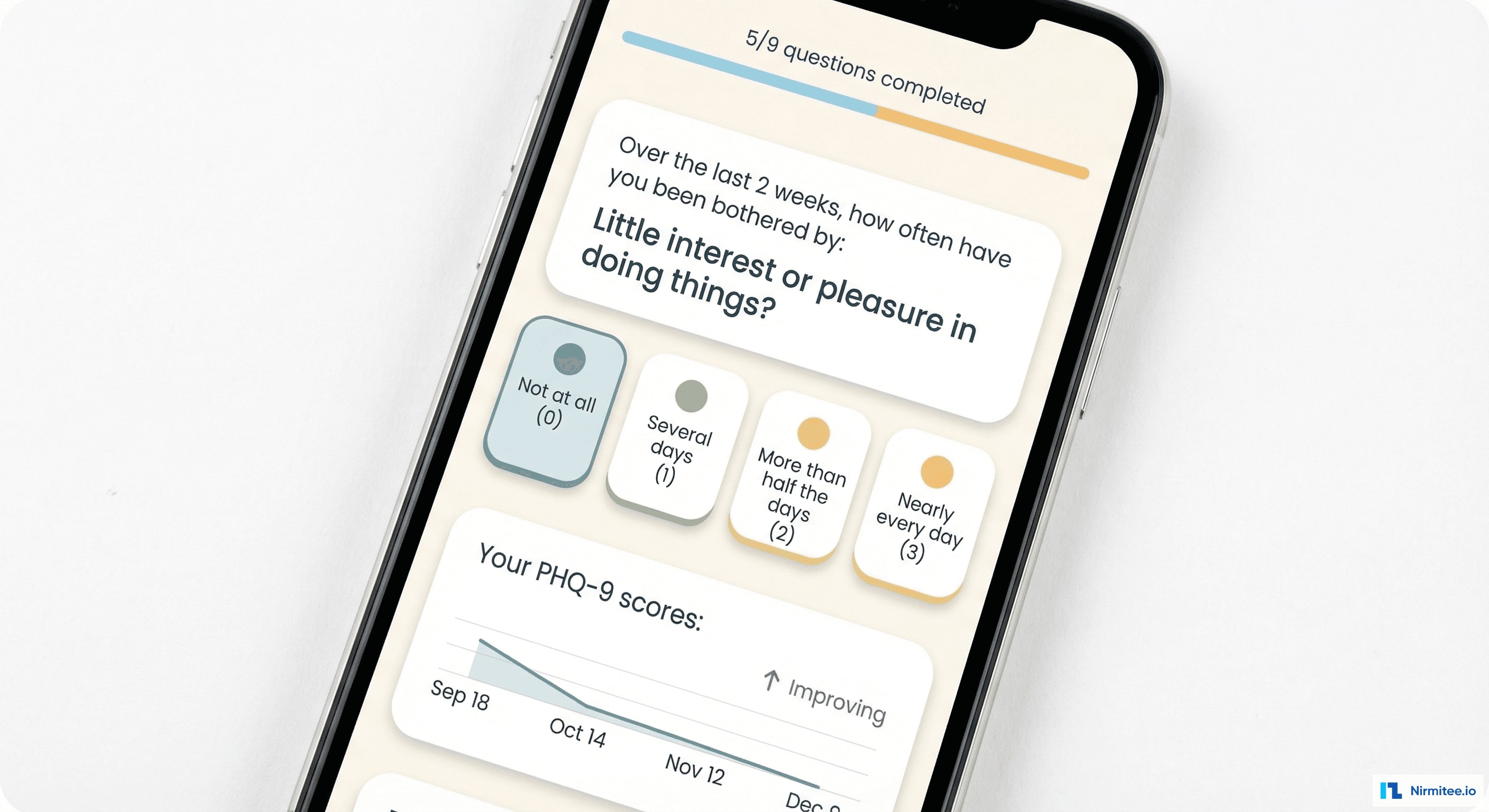
Validated clinical assessments are administered digitally with automatic scoring and trending:
- PHQ-9 (depression): 9 questions, auto-scored (0-27), severity categorized (minimal/mild/moderate/moderately severe/severe)
- GAD-7 (anxiety): 7 questions, auto-scored (0-21), severity levels mapped to treatment recommendations
- PCL-5 (PTSD): 20 questions, auto-scored, tracks trauma symptom clusters
- Longitudinal trending: every assessment score plotted over time — therapists and patients can see improvement trajectory across weeks and months
- Clinical alerts: if a PHQ-9 score increases significantly between sessions, the therapist is alerted before the next appointment. Item 9 (suicidal ideation) triggers immediate safety protocol notification.
AI-Assisted Session Notes
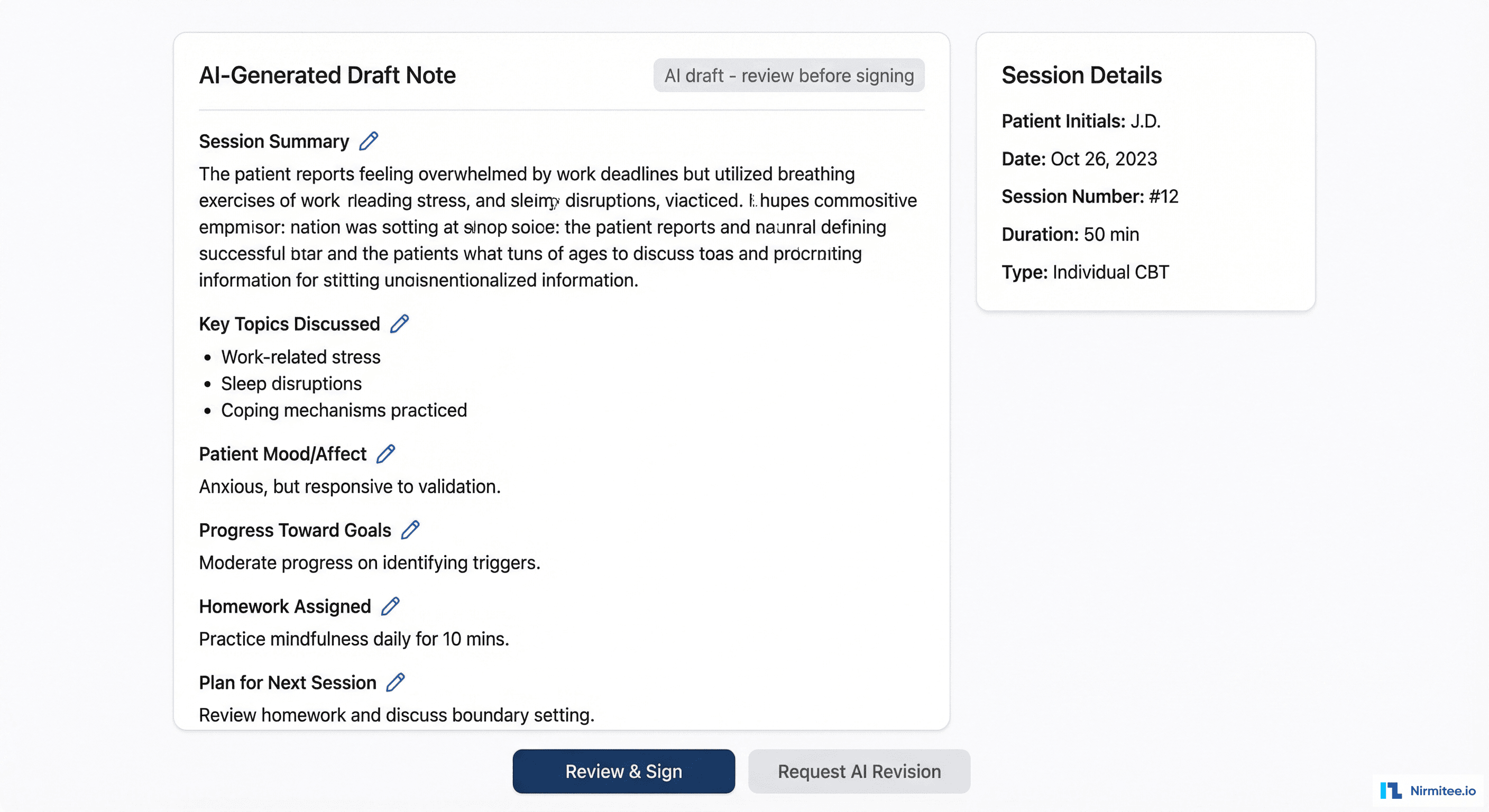
Session documentation is the biggest time sink for therapists. Our AI assistant transforms quick bullet points into comprehensive clinical notes:
- During session: therapist jots quick notes in the sidebar — bullet points, keywords, observations
- After session: clicks "Generate Note" — GPT-4 (HIPAA-compliant Azure deployment) expands the bullets into a structured clinical note with: session summary, key topics, patient mood/affect, progress toward goals, therapeutic interventions used, homework assigned, plan for next session
- Review and sign: therapist reviews the AI draft, makes any corrections, and signs. Average review time: 3 minutes (vs. 15 minutes writing from scratch)
Critical safeguard: the AI never invents clinical content. It only expands and structures what the therapist noted. If the therapist wrote "discussed panic attacks at work," the AI generates a paragraph about workplace anxiety management — it does not fabricate details the therapist didn't observe.
Our AI-powered healthcare solutions bring intelligence to clinical workflows.
Patient Outcome Tracking
Outcome tracking transforms therapy from subjective impression to data-driven care:
- PHQ-9 trend: depression score declining from 18 (moderate-severe) to 8 (mild) over 24 sessions — visual proof that treatment is working
- GAD-7 trend: anxiety scores tracked alongside depression — many patients have comorbid conditions that need parallel monitoring
- Treatment goals: custom goals with measurable progress bars — "Reduce panic attacks from 4/week to 1/week: 75% achieved"
- Session attendance: consistency tracking — missing sessions correlates with poorer outcomes. The system identifies attendance patterns.
- Step-down recommendations: when scores stabilize in the mild range for 4+ consecutive assessments, the system suggests stepping down from weekly to biweekly sessions — evidence-based frequency optimization
Patient Mobile App

The patient app provides between-session support that traditional therapy lacks:
- Daily mood check-in: 5-second emoji-based mood entry with optional journal note. Builds awareness and provides therapist with between-session data.
- Check-in streak: gamified consistency — patients maintain streaks for daily engagement, building the habit of self-monitoring
- Coping toolkit: therapist-assigned and self-selected exercises — 4-7-8 breathing, progressive muscle relaxation, grounding techniques (5-4-3-2-1), thought challenging worksheets
- Thought journal: CBT-based thought record — capture automatic thoughts, identify cognitive distortions, develop balanced alternatives. Entries shared with therapist (with permission).
- Crisis resources: always-visible emergency contact button and 988 Suicide & Crisis Lifeline — because safety can't wait for office hours
Results
| Metric | Before | After | Impact |
|---|---|---|---|
| Time to first session | 6-8 weeks | <1 week | 85% faster access |
| PHQ-9 improvement (24 sessions) | Variable (no tracking) | 56% avg reduction | Measurable outcomes |
| Session note documentation time | 15 minutes | 3 minutes | 80% faster with AI |
| Therapist session capacity | 6 patients/day | 8 patients/day | 33% more capacity |
| Patient engagement (between sessions) | Zero tools | 72% daily mood check-in | Continuous care connection |
| Session no-show rate | 18% (office visits) | 7% (video sessions) | 61% reduction |
| Patient satisfaction | 3.8/5 | 4.7/5 | 24% improvement |
| Geographic reach | 20-mile radius of office | Entire state (licensure-based) | Statewide access |
Financial Impact for a 5-Therapist Practice
- Capacity increase: 2 additional patients/day × 5 therapists × $150/session × 250 days = $375,000/year additional revenue
- No-show reduction: 11% fewer no-shows × 30 sessions/week × $150 = $25,740/year recovered
- Documentation savings: 12 min saved × 8 sessions/day × 5 therapists = 8 hours/day freed
- Office cost reduction: smaller physical footprint needed = $40,000-60,000/year savings
Compliance
- HIPAA: full compliance — encrypted video (WebRTC + AES-256), encrypted data at rest, BAA with all vendors, comprehensive audit logging
- 42 CFR Part 2: substance use disorder records receive additional federal protections — the platform enforces stricter consent requirements for SUD data
- State telehealth laws: configurable per state — consent requirements, prescribing rules, cross-state licensure (Psychology Interjurisdictional Compact supported)
- E-Prescribe (EPCS): DEA-compliant electronic prescribing for controlled substances (psychiatric medications) via Surescripts
- Crisis protocols: PHQ-9 Item 9 (suicidal ideation) triggers automated safety workflows — therapist notified, crisis resources surfaced to patient, safety plan activated
Timeline
| Phase | Duration | Deliverables |
|---|---|---|
| Phase 1 | 6 weeks | Video calling infrastructure (WebRTC), therapist dashboard, scheduling, patient app MVP |
| Phase 2 | 6 weeks | Digital assessments (PHQ-9/GAD-7/PCL-5), AI session notes, outcome tracking, mood check-ins |
| Phase 3 | 4 weeks | Billing (insurance + self-pay), e-prescribe integration, coping toolkit, thought journal |
| Phase 4 | 4 weeks | EHR integration (FHIR), compliance audit (HIPAA + 42 CFR Part 2), pilot with 5 therapists, launch |
Total: 5 months with 4 engineers + 1 clinical advisor (licensed psychologist).
Lessons Learned
- Video quality is non-negotiable in therapy. A pixelated video or audio delay breaks therapeutic rapport. We over-invested in video infrastructure — TURN servers in 3 regions, adaptive bitrate, audio-priority fallback. Zero tolerance for call quality issues.
- AI notes must be transparent. Therapists were initially suspicious of AI writing their notes. When we showed them exactly how it works (expands THEIR bullets, never fabricates), adoption went from 30% to 92% within a month. Transparency = trust.
- Between-session tools drive outcomes. Patients who used daily mood check-ins had 40% better PHQ-9 improvement than those who didn't. The app isn't just convenient access to therapy — it extends therapy into daily life.
- Crisis safety is the #1 priority. Before any feature, we built the crisis protocol system. PHQ-9 Item 9 detection, 988 integration, safety plan activation, therapist notification. This was the first thing we tested and the last thing we'd ever compromise on.
Shipping healthcare software that scales requires deep domain expertise. See how our Healthcare Software Product Development practice can accelerate your roadmap. We also offer specialized Custom Healthcare Software Development services. Talk to our team to get started.
Was this case study helpful?