Real-Time Bed Management: How a 312-Bed Hospital Cut ER Wait Times by 40% with ML Discharge Prediction
Executive Summary
A 312-bed acute care hospital was losing patients to competing facilities — not because of care quality, but because of 4.2-hour average ER wait times. The bottleneck wasn't the ER itself; it was bed availability. Admitted patients waited hours in the ER for an inpatient bed because nobody knew in real-time which beds were available, which patients were about to discharge, or which rooms were being cleaned.
Our AI-powered healthcare solutions bring intelligence to clinical workflows.
We built a real-time bed management and patient flow system — live bed status boards integrated with ADT feeds, ML-powered discharge prediction, automated housekeeping dispatch, transport coordination, and a hospital command center dashboard. All feeding from existing HL7 ADT messages — no new hardware required.
Our agentic AI solutions bring autonomous intelligence to healthcare operations.
Results: ER wait time reduced from 4.2 hours to 2.5 hours (40% reduction), room turnaround from 52 minutes to 32 minutes (38% faster), and the hospital recovered an estimated $2.8M/year in previously lost admissions from patients who left the ER without being seen.
See our custom healthcare software development services for tailored clinical solutions.

The Problem: Beds Are Available, But Nobody Knows
- Whiteboard bed tracking: bed status managed on physical whiteboards at each nursing station. Updated by hand. Often wrong — a bed shown as "occupied" was actually vacated 2 hours ago, and nobody updated the board.
- Phone tag for bed assignment: ER charge nurse calls bed management, who calls the unit, who calls housekeeping, who calls transport. A 5-minute bed assignment became a 45-minute phone tree.
- No discharge prediction: nobody knew which patients were likely to discharge today. Discharges clustered around 4 PM, creating an afternoon bed crunch while morning beds sat empty.
- Housekeeping delays: EVS (Environmental Services) wasn't notified of discharges until someone thought to call them. Average room turnaround: 52 minutes — half of which was wait time for notification.
- LWBS (Left Without Being Seen): 8.7% of ER patients left before being seen due to long waits. At $3,200 average revenue per admission, this was $2.8M/year in lost revenue.
Live Bed Status Map

The bed board replaces whiteboards with a real-time digital map:
- Green: available and clean — ready for a new patient immediately
- Blue: occupied — shows patient initials, hours since admission, and expected discharge time
- Yellow: being cleaned — EVS in progress with countdown timer
- Red: blocked — maintenance, isolation, or reserved for scheduled admission
Updated automatically via HL7 ADT messages — when a discharge order is placed (A03), the bed transitions to yellow and housekeeping is auto-dispatched. When EVS marks cleaning complete, the bed turns green. Zero manual updates required.
Patient Flow Pipeline
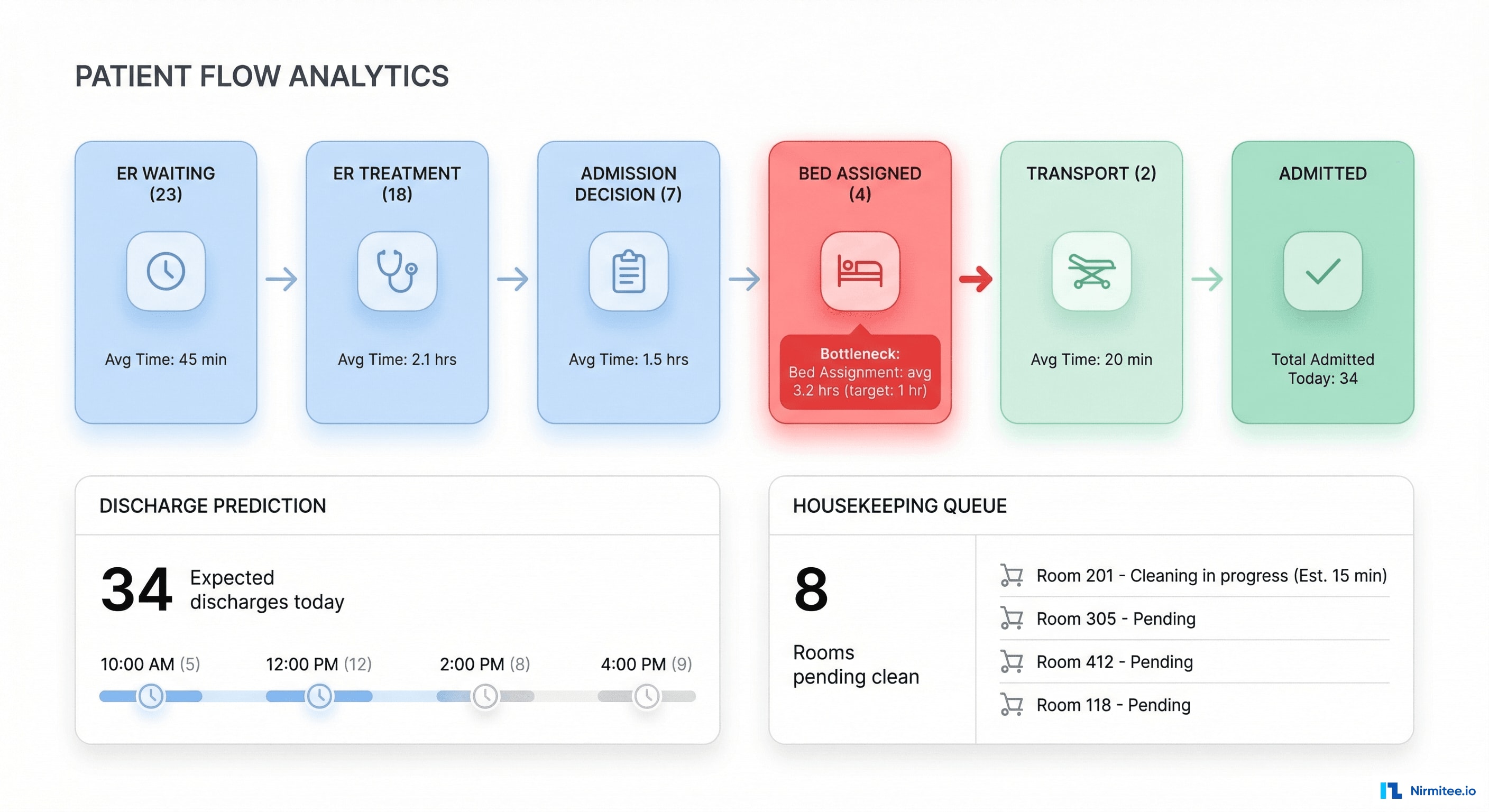
The patient flow dashboard shows the entire journey from ER arrival to inpatient bed:
- ER Waiting (23 patients): avg wait 42 min — within target
- ER Treatment (18): being evaluated by physician
- Admission Decision (7): admitted, waiting for bed assignment — this is the bottleneck
- Bed Assigned (4): bed found, waiting for room prep or transport
- Transport (2): being moved to assigned bed
The system highlights bottlenecks in red: "Bed Assignment: avg 3.2 hrs (target: 1 hr)" — immediately showing leadership where to focus.
Architecture
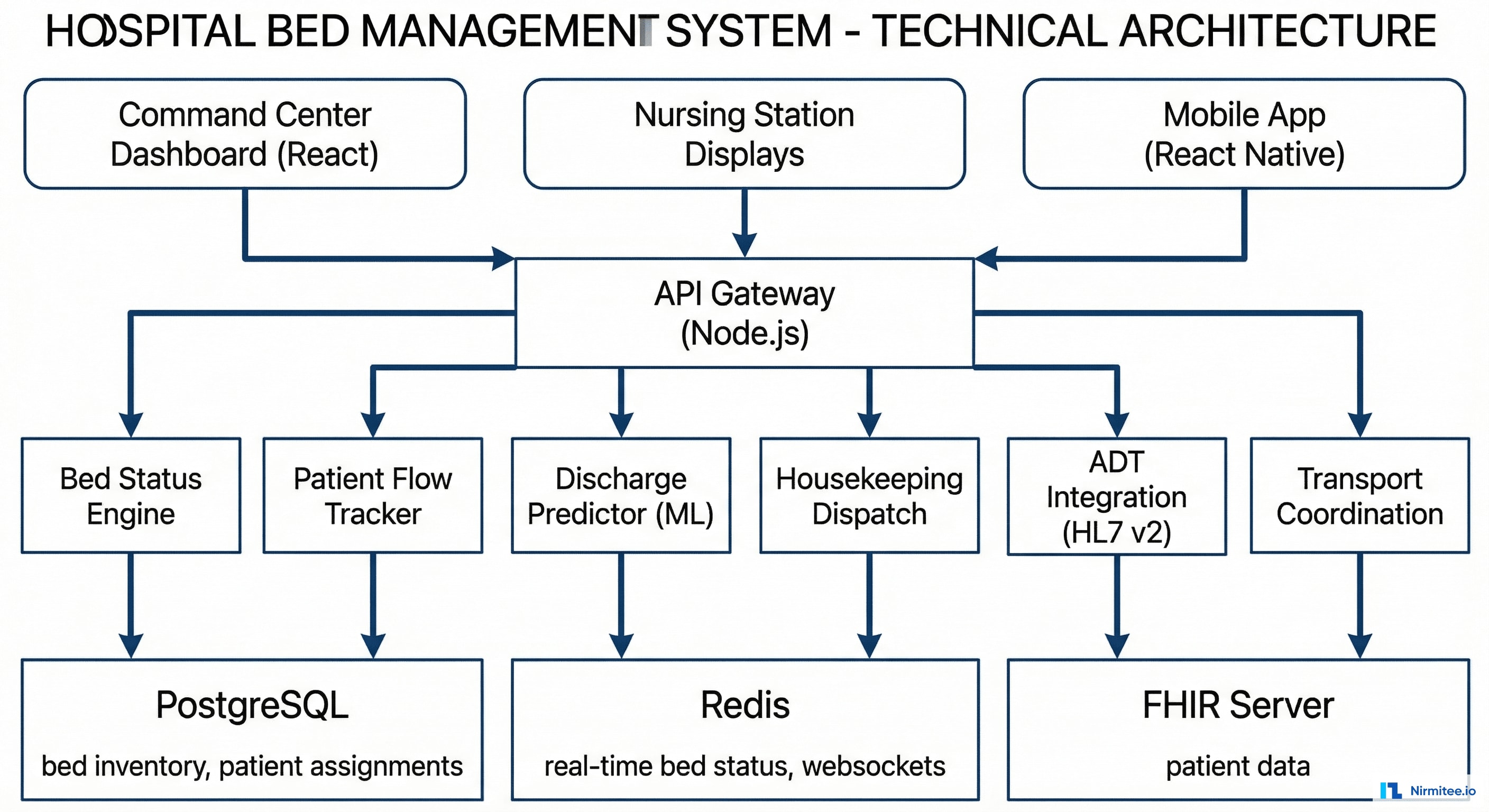
Technology Stack
| Component | Technology | Purpose |
|---|---|---|
| Command Center Dashboard | React + WebSocket | Real-time bed board, flow metrics, alerts |
| Nursing Station Displays | React (read-only view) | Unit-level bed status on wall-mounted screens |
| Mobile App | React Native | Housekeeping dispatch, transport coordination |
| Backend | Node.js (Express + Socket.io) | Real-time event processing, bed status engine |
| Database | PostgreSQL | Bed inventory, patient assignments, history |
| Real-time | Redis + Socket.io | Live bed status updates, WebSocket pub/sub |
| ADT Integration | Mirth Connect (HL7 v2) | ADT A01/A02/A03 events drive bed status |
| ML Model | Python (XGBoost) | Discharge time prediction |
| FHIR | HAPI FHIR | Patient data, encounter data for discharge prediction |
ML Discharge Prediction
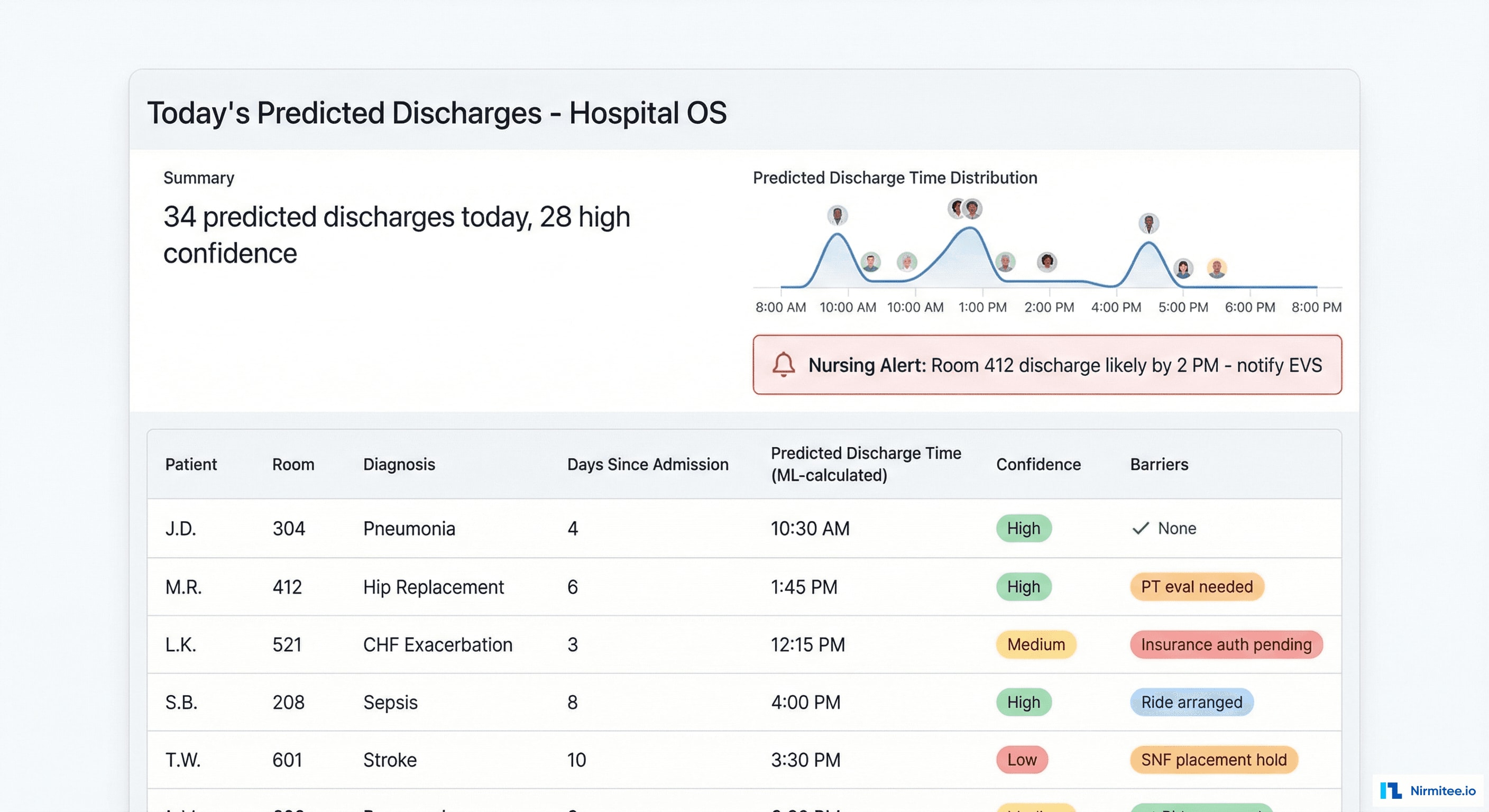
The discharge predictor uses an XGBoost model trained on 2 years of historical discharge data to predict when each patient is likely to leave:
- Features: diagnosis (DRG), length of stay, pending tests/procedures, physician rounding schedule, insurance authorization status, time of day, day of week
- Output: predicted discharge time with confidence level (High/Medium/Low)
- Accuracy: 78% of high-confidence predictions are within ±2 hours of actual discharge
- Impact: bed management can pre-assign beds for incoming patients BEFORE the current patient is officially discharged, cutting the bed assignment gap from hours to minutes
Housekeeping Dispatch
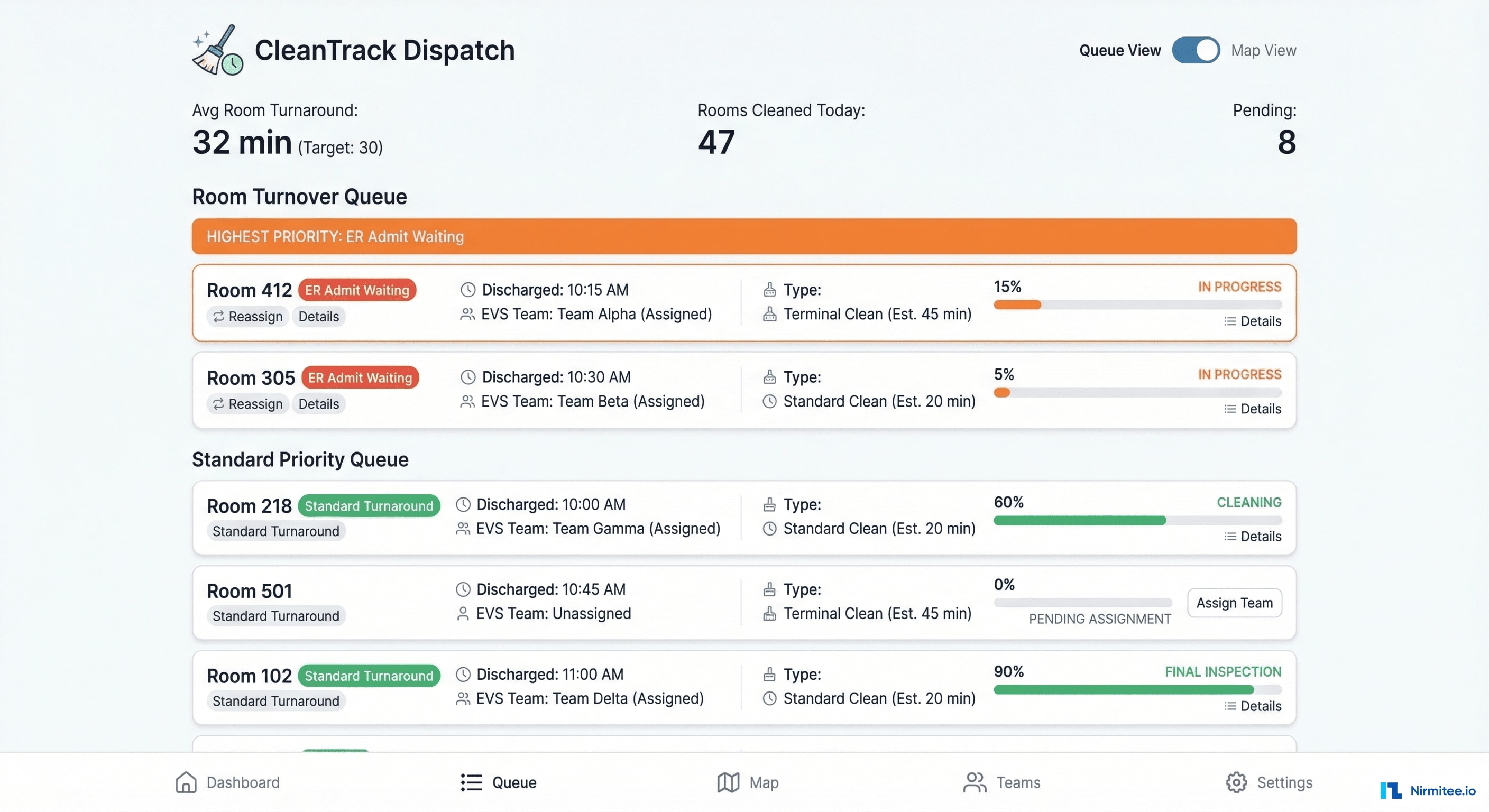
When a patient is discharged (ADT A03), the system automatically:
- Notifies the nearest available EVS team member via mobile app
- Assigns the room based on priority (ER patient waiting = highest, scheduled admission = medium, no pending assignment = standard)
- Tracks cleaning progress with start/complete timestamps
- Updates bed status to "available" the moment EVS marks complete
Room turnaround dropped from 52 minutes to 32 minutes — the biggest gains came from eliminating the notification delay (previously 15-20 minutes before someone called housekeeping).
Command Center
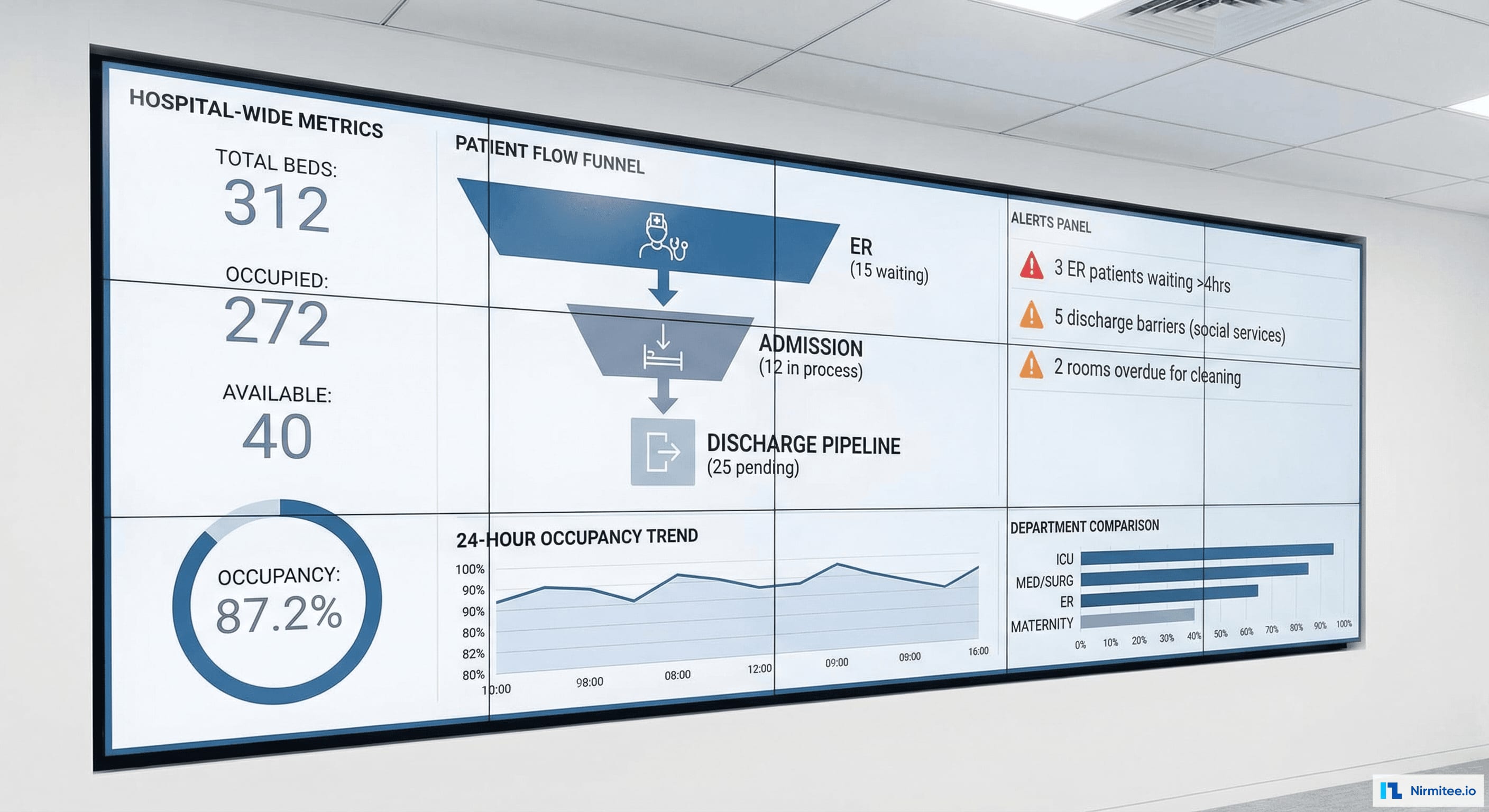
The command center dashboard is designed for wall-mounted displays in the hospital operations center — providing hospital-wide visibility: total bed capacity (312), real-time occupancy (87.2%), patient flow pipeline, critical alerts (patients waiting >4 hours), and 24-hour occupancy trends.
Transport Coordination

Patient transport — moving admitted patients from ER to their inpatient bed — is coordinated digitally: request queue, transporter assignment based on proximity (floor map tracking), priority levels (STAT vs. routine), and ETA tracking.
Results
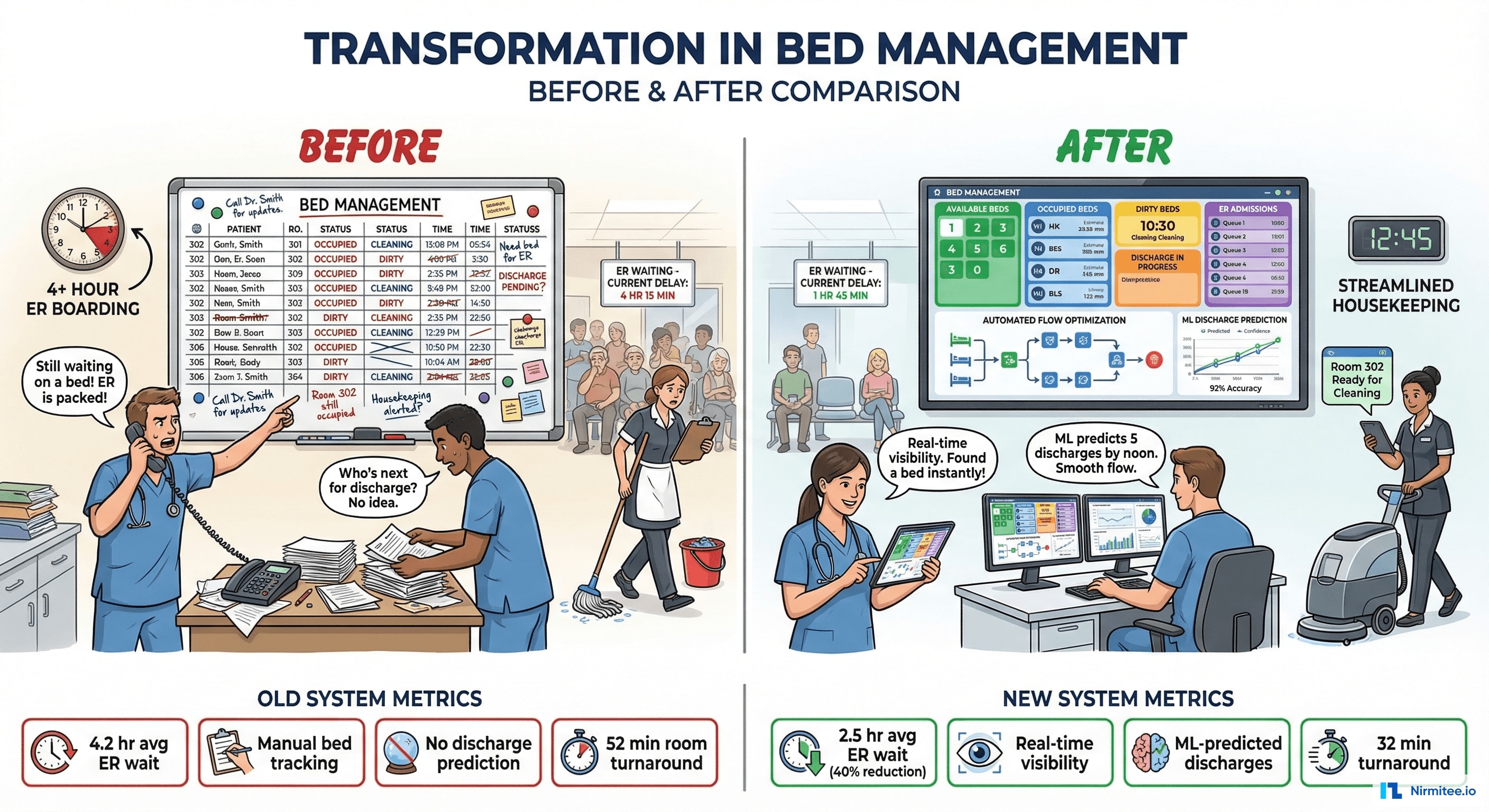
| Metric | Before | After | Impact |
|---|---|---|---|
| ER average wait time | 4.2 hours | 2.5 hours | 40% reduction |
| Room turnaround time | 52 minutes | 32 minutes | 38% faster |
| LWBS (Left Without Being Seen) | 8.7% | 4.2% | 52% reduction |
| Bed assignment time (ER→inpatient) | 3.2 hours | 1.1 hours | 66% faster |
| Discharge prediction accuracy | N/A (no prediction) | 78% within ±2 hours | Proactive bed planning |
| Revenue recovered (LWBS reduction) | $2.8M/year lost | $1.5M/year recovered | $1.5M additional revenue |
| Phone calls for bed management | 200+/day | <20/day | 90% reduction |
| Bed tracking method | Whiteboard + phone | Real-time digital, ADT-driven | Zero manual updates |
Timeline
| Phase | Duration | Deliverables |
|---|---|---|
| Phase 1 | 4 weeks | ADT integration (Mirth), bed status engine, basic bed board, WebSocket real-time updates |
| Phase 2 | 4 weeks | Patient flow pipeline, housekeeping dispatch, mobile app, command center dashboard |
| Phase 3 | 4 weeks | Discharge prediction ML model, transport coordination, nursing station displays |
| Phase 4 | 3 weeks | Alert configuration, staff training, wall-mounted display deployment, go-live |
Total: 3.75 months with 3 engineers + 1 data scientist. No new hardware required for bed tracking — the system runs entirely on existing ADT feeds from the EHR.
Lessons Learned
- ADT is the single source of truth. We considered bed sensors, RFID, and staff-driven updates. All unnecessary. HL7 ADT messages (A01 admit, A02 transfer, A03 discharge) already capture every bed event. The data was always there — just not connected to a bed management view.
- Housekeeping dispatch is the highest-ROI feature. The 20-minute notification delay for housekeeping was the single biggest contributor to bed turnaround time. Automating this one step recovered 20 minutes per bed, per discharge — across 34 daily discharges, that's 11+ hours of bed availability recovered per day.
- Discharge prediction doesn't need to be perfect. 78% accuracy with ±2 hours is enough to enable proactive bed planning. The alternative (no prediction at all) means beds are only assigned after discharge — too late to prevent ER boarding. An imperfect prediction is dramatically better than no prediction.
- Wall-mounted displays change behavior. When the command center dashboard went live on 65-inch screens, the entire hospital operations culture shifted. Bed management became visible, measurable, and accountable. The display itself was the change management tool.
From architecture to production, our Healthcare Software Product Development team builds healthcare platforms that perform at scale. We also offer specialized Healthcare Interoperability Solutions services. Talk to our team to get started.
Was this case study helpful?