Hospital asset management has evolved from clipboard-based tracking into a strategic discipline that directly impacts patient outcomes, regulatory compliance, and operational budgets. In 2026, healthcare organizations that still rely on spreadsheets and manual logs face mounting pressure from rising equipment costs, tighter regulations, and growing patient volumes.
This guide breaks down everything you need to know about hospital asset management — why it matters now more than ever, which features separate great software from mediocre solutions, and how to implement a system that delivers measurable ROI within 90 days.
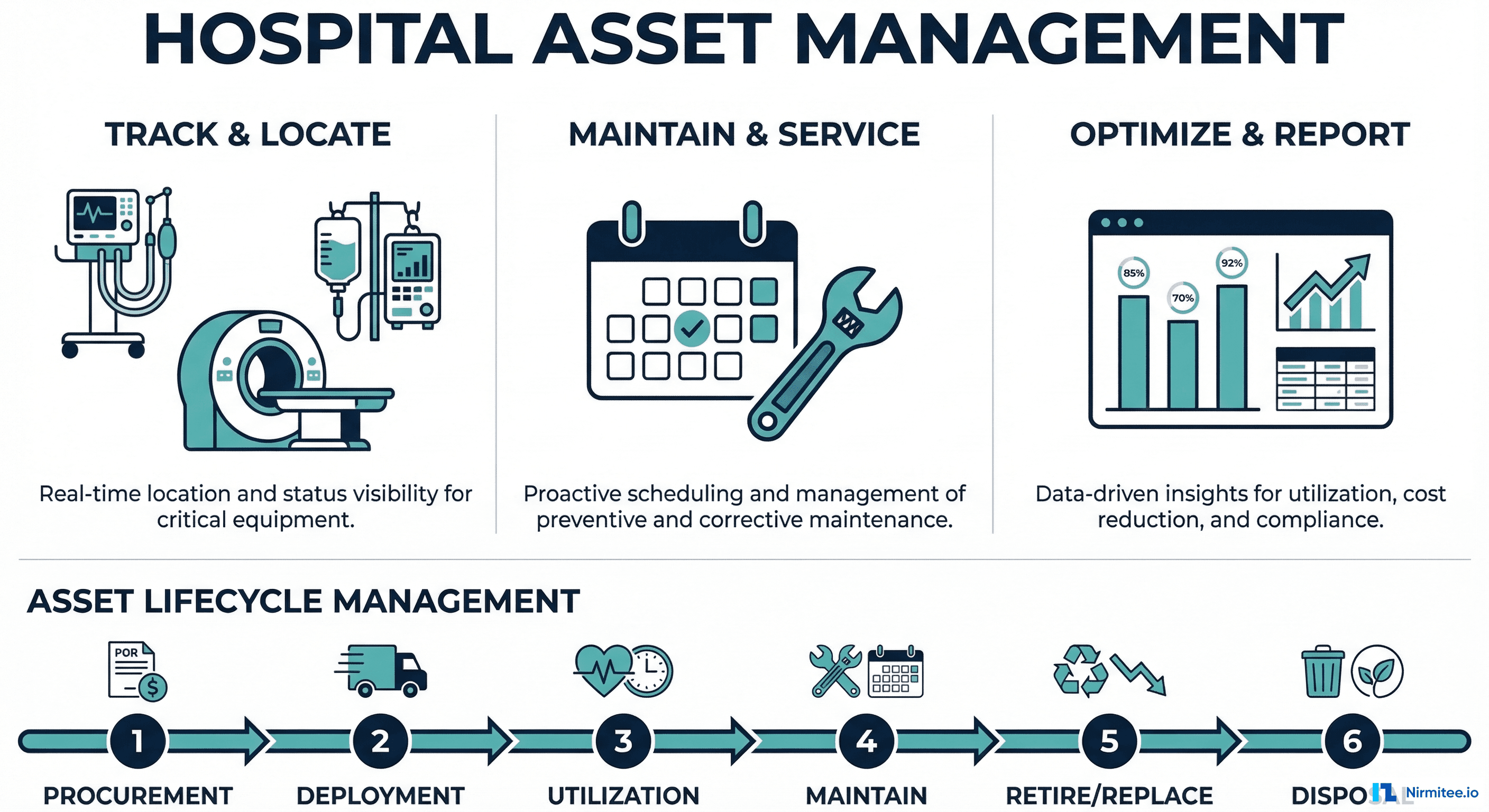
What Is Hospital Asset Management?
Hospital asset management is the systematic process of tracking, maintaining, and optimizing every physical asset within a healthcare facility — from high-value imaging equipment and surgical instruments to beds, wheelchairs, infusion pumps, and IT infrastructure.
Unlike generic asset tracking, hospital asset management must account for:
- Patient safety implications — a malfunctioning ventilator or miscalibrated infusion pump can be life-threatening
- Regulatory compliance — FDA, Joint Commission (JCAHO), HIPAA, and state health department requirements mandate documented maintenance histories
- Infection control — assets must be tracked through decontamination cycles and sterile processing
- Clinical workflow integration — equipment must be available where and when clinicians need it, without disrupting care delivery
- Depreciation and capital planning — hospitals manage asset portfolios worth tens of millions of dollars with multi-year replacement cycles
A modern hospital asset management system (AMS) replaces manual processes with digital tracking, automated maintenance scheduling, real-time location visibility, and data-driven decision-making across the entire asset lifecycle.
Why Hospital Asset Management Matters in 2026
The stakes have never been higher. Healthcare systems face a convergence of cost pressure, regulatory scrutiny, and operational complexity that makes disciplined asset management essential rather than optional.
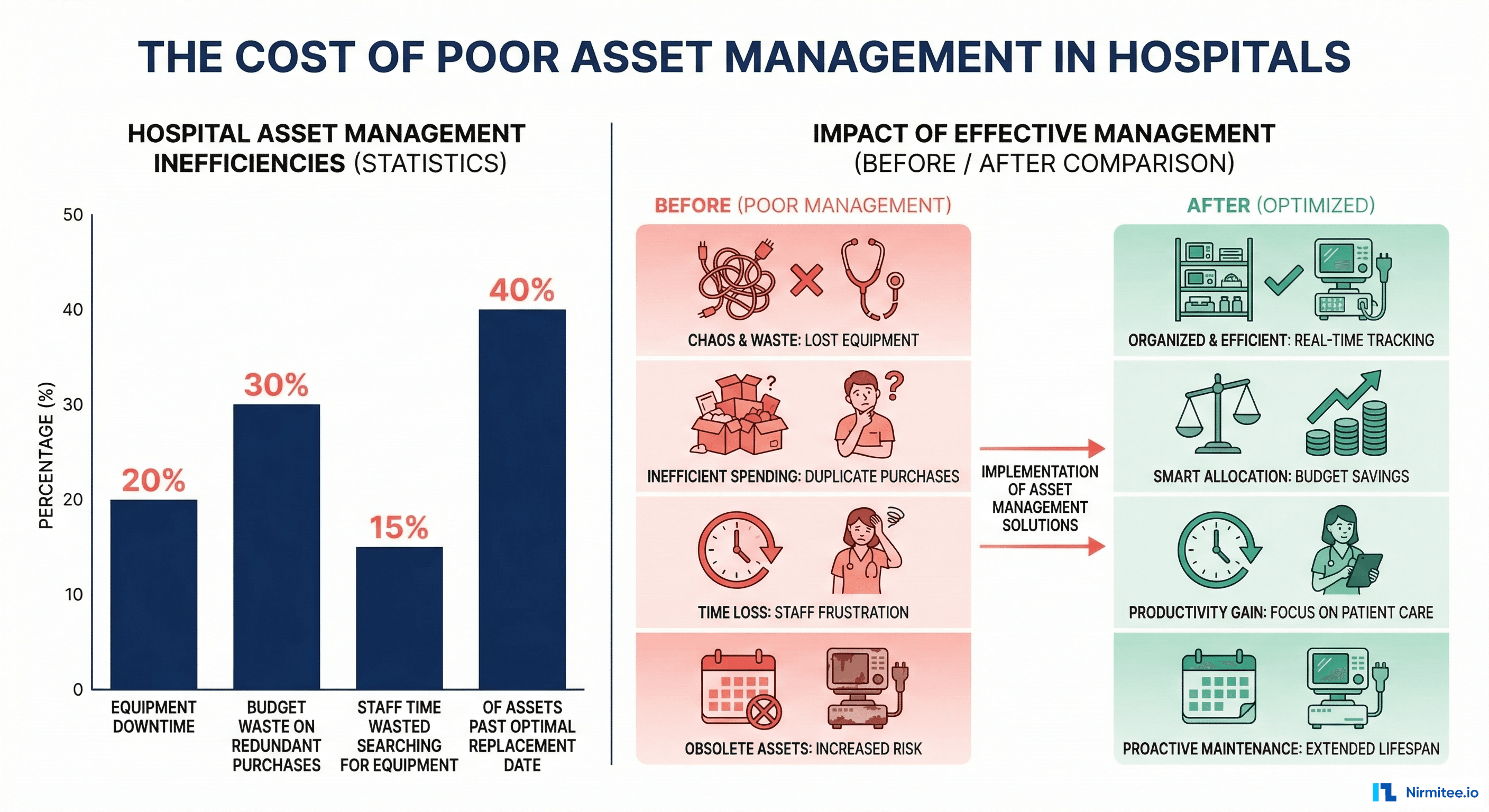
The Financial Impact
Hospitals that lack systematic asset management routinely experience:
- 10–20% equipment downtime due to reactive rather than preventive maintenance, costing an average hospital $1.2 million annually in lost productivity and emergency repairs
- Up to 30% redundant purchasing because departments cannot locate existing equipment or verify what is already available across facilities
- 15% of nursing staff time spent searching for equipment instead of delivering patient care — translating to roughly 45 minutes per 8-hour shift per nurse
- Premature asset replacement driven by poor maintenance records rather than actual condition data, accelerating capital expenditure cycles by 2–3 years
Regulatory and Compliance Pressure
In 2026, regulatory bodies have intensified their focus on asset management:
- Joint Commission surveys now require documented evidence of preventive maintenance completion rates, calibration schedules, and recall response timelines
- FDA medical device reporting mandates traceable maintenance histories for all Class II and Class III devices
- CMS Conditions of Participation tie reimbursement eligibility to demonstrable equipment safety programs
- State health department audits increasingly request digital asset registers during unannounced inspections
Failing an audit does not just mean a citation — it can mean suspended accreditation, reduced reimbursement rates, and reputational damage that affects patient acquisition for years.
Operational Complexity
Modern hospitals are more complex than ever:
- Multi-facility health systems need asset visibility across campuses, satellite clinics, and ambulatory care centers
- Equipment sharing programs between departments require transparent movement tracking
- Telemedicine and remote patient monitoring have introduced thousands of connected devices that need lifecycle management
- Supply chain disruptions have made equipment availability unpredictable, making utilization optimization critical
Core Features to Look for in Hospital Asset Management Software
Not all asset management systems are built for healthcare. A solution designed for manufacturing or logistics will not meet the specialized requirements of a hospital environment. Here are the features that separate purpose-built healthcare AMS platforms from generic alternatives.
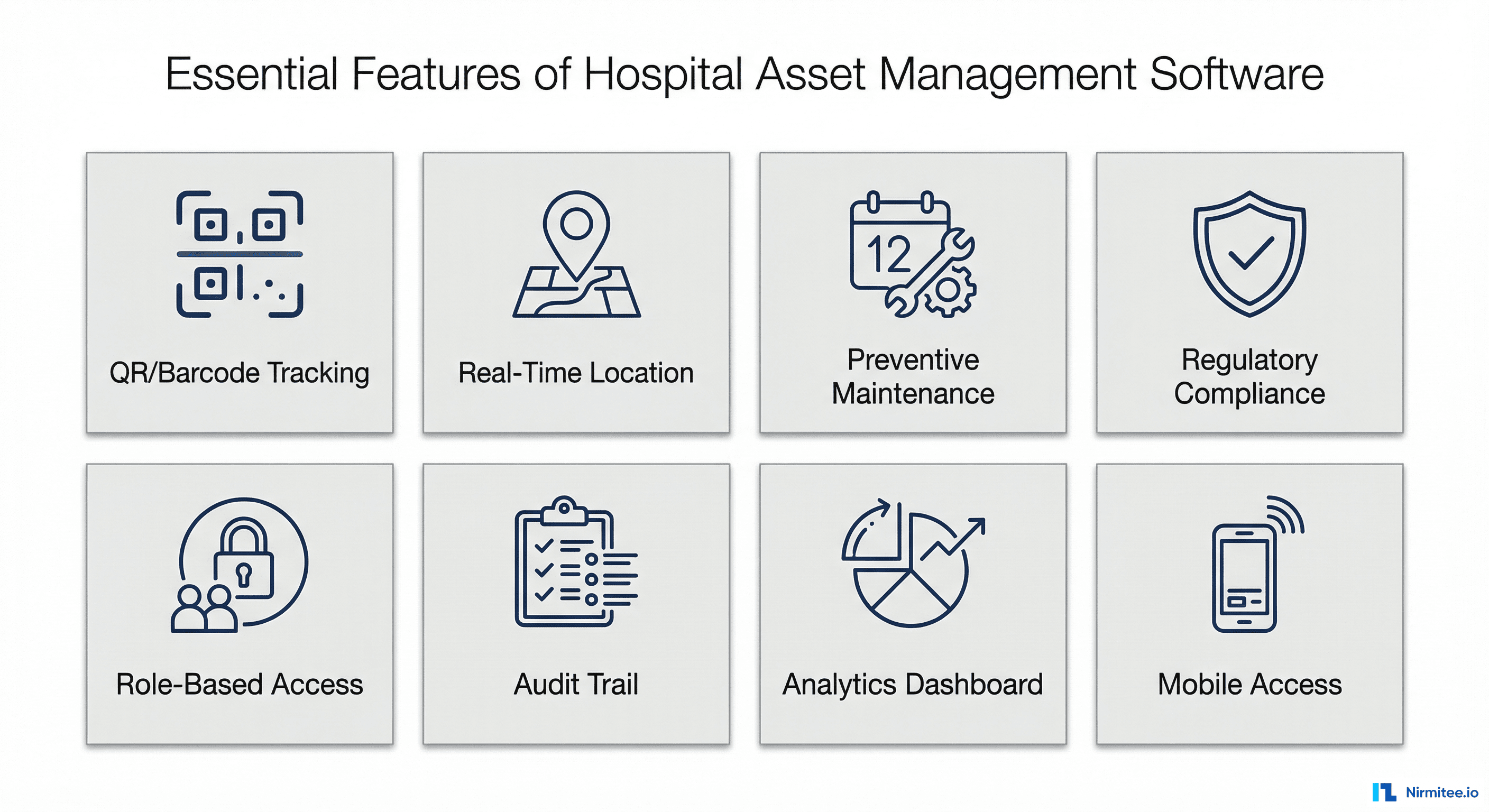
1. QR Code and Barcode Tracking
Every asset should have a unique identifier — whether a QR code, barcode, or RFID tag — that links to its complete digital record. Staff should be able to scan any piece of equipment with a mobile device and instantly see:
- Asset details (make, model, serial number, purchase date)
- Current location and assignment
- Maintenance history and next scheduled service
- Warranty status and vendor contacts
- Compliance documentation and calibration certificates
QR codes are the most cost-effective option for most hospitals, requiring only printed labels and smartphone cameras rather than specialized RFID infrastructure.
2. Preventive Maintenance Scheduling
Reactive maintenance — fixing equipment after it breaks — costs 3–5x more than preventive maintenance. A strong AMS automates maintenance scheduling based on:
- Manufacturer recommendations — OEM-specified service intervals
- Usage-based triggers — hours of operation, cycle counts, or procedure volumes
- Regulatory requirements — mandatory calibration and safety testing schedules
- Condition monitoring — predictive alerts based on performance degradation patterns
The system should automatically generate work orders, assign them to qualified technicians, and escalate overdue tasks before they become compliance violations.
3. Role-Based Access Control (RBAC)
Hospitals have diverse stakeholders who need different levels of access:
- Biomedical engineers need full access to maintenance records and work orders
- Nursing staff need to report issues and view equipment locations
- Department heads need utilization reports and budget projections
- Administrators need system-wide dashboards and compliance reports
- Auditors need read-only access to specific compliance documentation
Granular, permission-based access ensures data security while giving each role exactly the information they need.
4. Real-Time Asset Location and Movement Tracking
Knowing where equipment is — right now — eliminates the daily scavenger hunts that waste clinical staff time. Effective tracking includes:
- Current department and facility assignment
- Movement history with timestamps and transfer reasons
- Custody chain documentation for high-value or regulated assets
- Automated alerts when assets leave designated zones
5. Comprehensive Audit Trail
Every action taken on an asset — creation, modification, movement, maintenance, condition assessment — should be logged with timestamps, user identification, and change details. This is not optional in healthcare; it is a regulatory requirement.
A well-designed audit system lets you reconstruct the complete history of any asset, answer inspector questions in seconds rather than days, and identify process breakdowns before they become systemic.
6. Analytics and Reporting Dashboard
Data without insight is noise. Your AMS should provide:
- Asset utilization rates — identifying underused equipment that could be redeployed or shared
- Maintenance cost trends — flagging assets approaching the repair-vs-replace threshold
- Depreciation tracking — supporting capital budget planning and financial reporting
- Compliance scorecards — showing maintenance completion rates, overdue work orders, and audit readiness
- Custom reports — exportable data for board presentations, regulatory submissions, and operational reviews
7. Mobile Access
Biomedical technicians, nurses, and facilities staff do not sit at desks. Mobile access — via native app or responsive web interface — enables:
- On-the-spot equipment scanning and condition reporting
- Work order creation and completion from the field
- Photo documentation of equipment issues
- Real-time notifications for urgent maintenance tasks
8. Integration Capabilities
A hospital AMS does not exist in isolation. Look for systems that integrate with:
- CMMS (Computerized Maintenance Management System) for detailed work order management
- ERP/Financial systems for procurement, depreciation, and budget tracking
- EHR/EMR systems for clinical workflow integration
- Building management systems for environmental monitoring of sensitive equipment
Understanding the Hospital Asset Lifecycle
Effective asset management covers every stage of an asset's life within your organization. Understanding this lifecycle helps you identify where your current processes have gaps and where technology can deliver the most value.
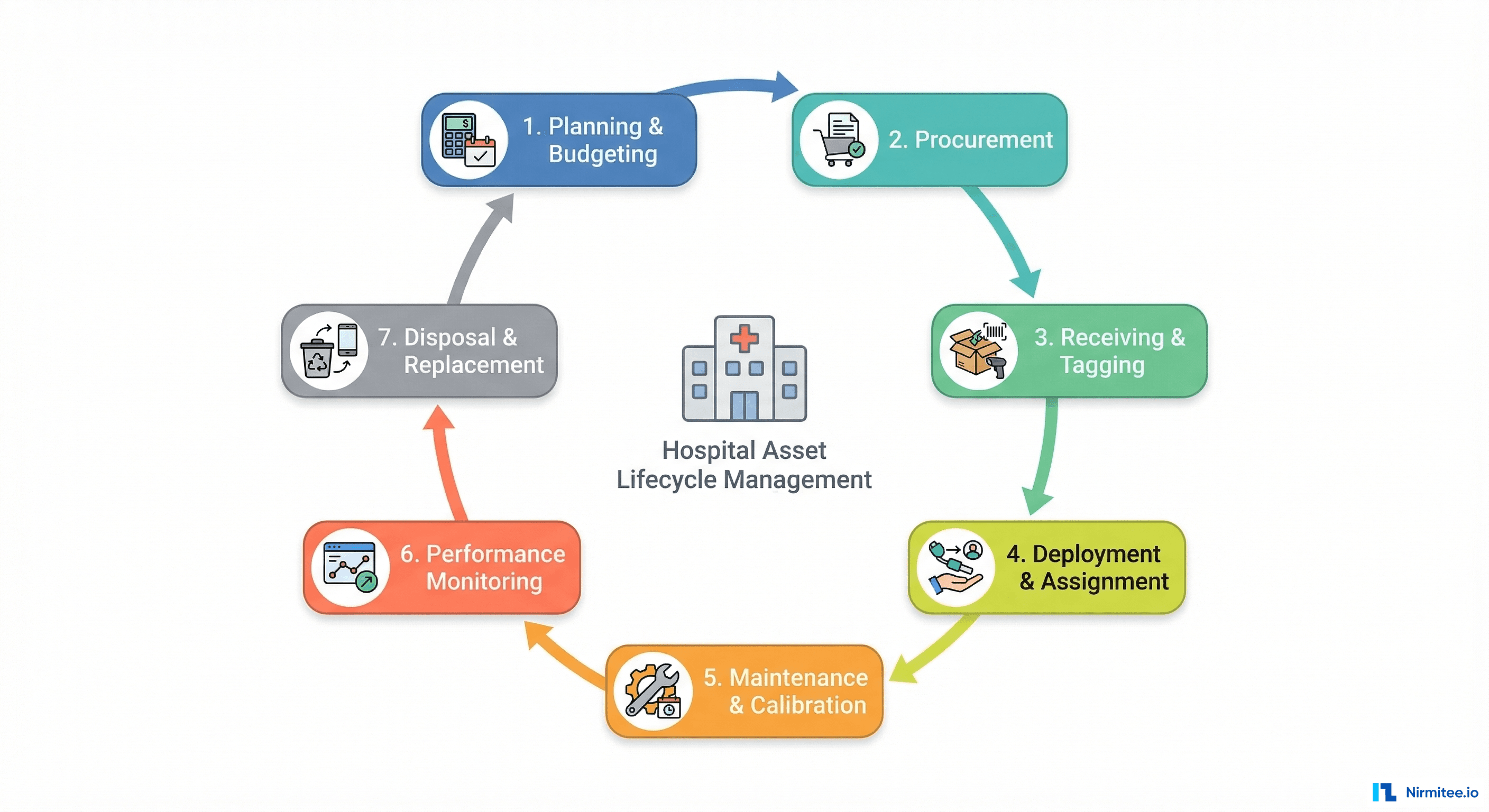
Stage 1: Planning and Budgeting
Before purchasing any asset, hospitals need data to justify the investment. A good AMS provides historical utilization data, maintenance cost trends, and condition assessments that inform capital budget requests with evidence rather than guesswork.
Stage 2: Procurement
Once approved, procurement benefits from standardized specifications, vendor comparison data, and purchase history. The AMS should capture purchase orders, warranty terms, vendor contacts, and expected delivery timelines.
Stage 3: Receiving and Tagging
When equipment arrives, it enters the system immediately — tagged with a QR code or barcode, photographed, and registered with all manufacturer details. This is the critical moment where an asset becomes trackable. Skip this step, and the asset becomes a ghost in your inventory.
Stage 4: Deployment and Assignment
Assets are assigned to specific facilities, departments, and sometimes individual users. The system tracks who has custody, where the equipment is located, and what clinical workflows it supports.
Stage 5: Maintenance and Calibration
This is where most of the ongoing value lives. Automated preventive maintenance schedules, work order management, parts tracking, and compliance documentation keep equipment safe, functional, and regulation-ready.
Stage 6: Performance Monitoring
Throughout its operational life, each asset generates data — uptime, repair frequency, cost per use, patient throughput contribution. This data drives decisions about redeployment, replacement timing, and future procurement strategy.
Stage 7: Disposal and Replacement
When an asset reaches end-of-life — whether due to obsolescence, irreparable failure, or regulatory decertification — the system manages decommissioning, data sanitization (for connected devices), environmentally compliant disposal, and replacement planning informed by historical performance data.
How to Get Started: A 90-Day Implementation Roadmap
Implementing a hospital asset management system does not need to be a multi-year IT project. With the right approach, you can have a functional system delivering value within 90 days.
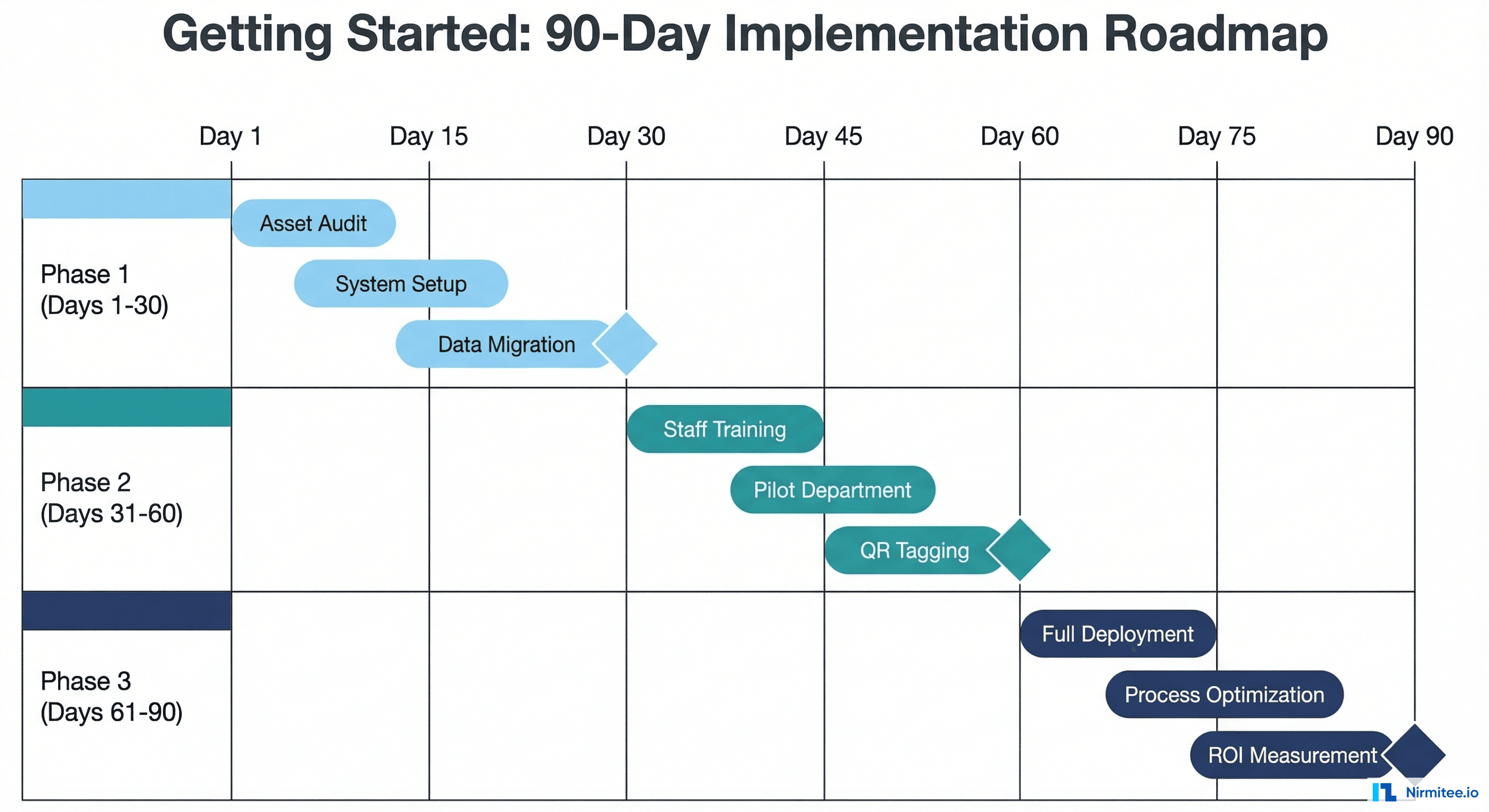
Phase 1: Foundation (Days 1–30)
Week 1–2: Asset Audit
You cannot manage what you have not counted. Start with a physical inventory of your highest-value and highest-risk assets. Focus on:
- Medical devices requiring regulatory maintenance (Class II and III)
- Equipment with active warranties or service contracts
- Assets above a defined cost threshold (e.g., items over $5,000)
- Safety-critical equipment (life support, surgical, diagnostic imaging)
Do not try to inventory everything in week one. Start with the assets that carry the most risk and cost if mismanaged.
Week 3–4: System Setup and Data Migration
- Configure your AMS with your organizational structure — facilities, departments, roles
- Import your initial asset register from the audit
- Set up user accounts with appropriate role-based permissions
- Configure maintenance schedules for critical equipment categories
- Establish your QR code or barcode labeling scheme
Phase 2: Rollout (Days 31–60)
Week 5–6: Staff Training and Pilot
Choose one department — ideally one with engaged leadership and moderate asset complexity — for your pilot:
- Train department staff on scanning, reporting, and basic system navigation
- Train biomedical engineering on work order management and maintenance logging
- Tag all assets in the pilot department with QR codes
- Run the pilot for two weeks, collecting feedback and refining processes
Week 7–8: Expand and Optimize
- Address issues discovered during the pilot
- Roll out to 2–3 additional departments
- Begin entering historical maintenance records for critical assets
- Set up automated reports and dashboard views for department heads
Phase 3: Scale (Days 61–90)
Week 9–10: Full Deployment
- Extend to all remaining departments
- Complete QR tagging across the facility
- Activate automated maintenance reminders and escalation workflows
- Enable mobile access for field technicians
Week 11–12: Measure and Refine
- Run your first utilization and compliance reports
- Calculate initial ROI metrics — time saved, purchases avoided, maintenance compliance rate
- Present findings to leadership with data-backed recommendations
- Plan Phase 2 enhancements (integration with ERP, predictive maintenance, multi-facility expansion)
Common Mistakes to Avoid
After working with healthcare organizations of all sizes, certain implementation pitfalls come up repeatedly:
- Trying to track everything at once. Start with high-value, high-risk assets. Expand to furniture and low-value items only after core processes are running smoothly.
- Ignoring change management. The best software in the world fails if staff do not use it. Invest in training, communicate the why, and celebrate early wins.
- Choosing generic over healthcare-specific. A warehouse inventory system will not handle maintenance compliance, clinical workflows, or regulatory audit requirements. Choose a platform built for healthcare.
- Treating implementation as an IT project. Asset management is an operational initiative. Clinical engineering, nursing leadership, and facilities management should drive adoption, not just IT.
- Neglecting data quality. Garbage in, garbage out. Invest time upfront in clean, accurate data entry — serial numbers, purchase dates, warranty terms, and maintenance histories.
- Skipping the pilot phase. Going live across an entire hospital simultaneously maximizes risk and minimizes your ability to learn and adjust.
Measuring Success: Key Metrics to Track
Once your system is operational, track these metrics to demonstrate value and identify improvement opportunities:
- Equipment uptime rate — target 95%+ for critical assets
- Preventive maintenance completion rate — target 90%+ for regulatory compliance
- Mean time to repair (MTTR) — should decrease as preventive maintenance reduces emergency failures
- Asset utilization rate — identifies underused equipment candidates for redeployment
- Cost per asset — total cost of ownership including purchase, maintenance, and operational costs
- Audit readiness score — percentage of assets with complete, current documentation
- Staff time saved — hours recovered from equipment searching, manual record-keeping, and paper-based processes
The Bottom Line
Hospital asset management in 2026 is not about tracking equipment — it is about enabling better patient care through operational excellence. When clinicians can find the equipment they need, when maintenance is proactive rather than reactive, when compliance documentation is a click rather than a filing cabinet, the entire organization performs better.
The technology exists today. The implementation path is proven. The ROI is measurable within 90 days. The only question is whether your organization will make the shift from reactive asset chaos to proactive asset intelligence — or continue paying the hidden costs of doing nothing.
Start small, start with what matters most, and let the data make the case for expansion. Your patients, your staff, and your budget will all benefit.
Share
Related Posts
NABH Asset Management Compliance: A Complete Guide for Indian Hospitals
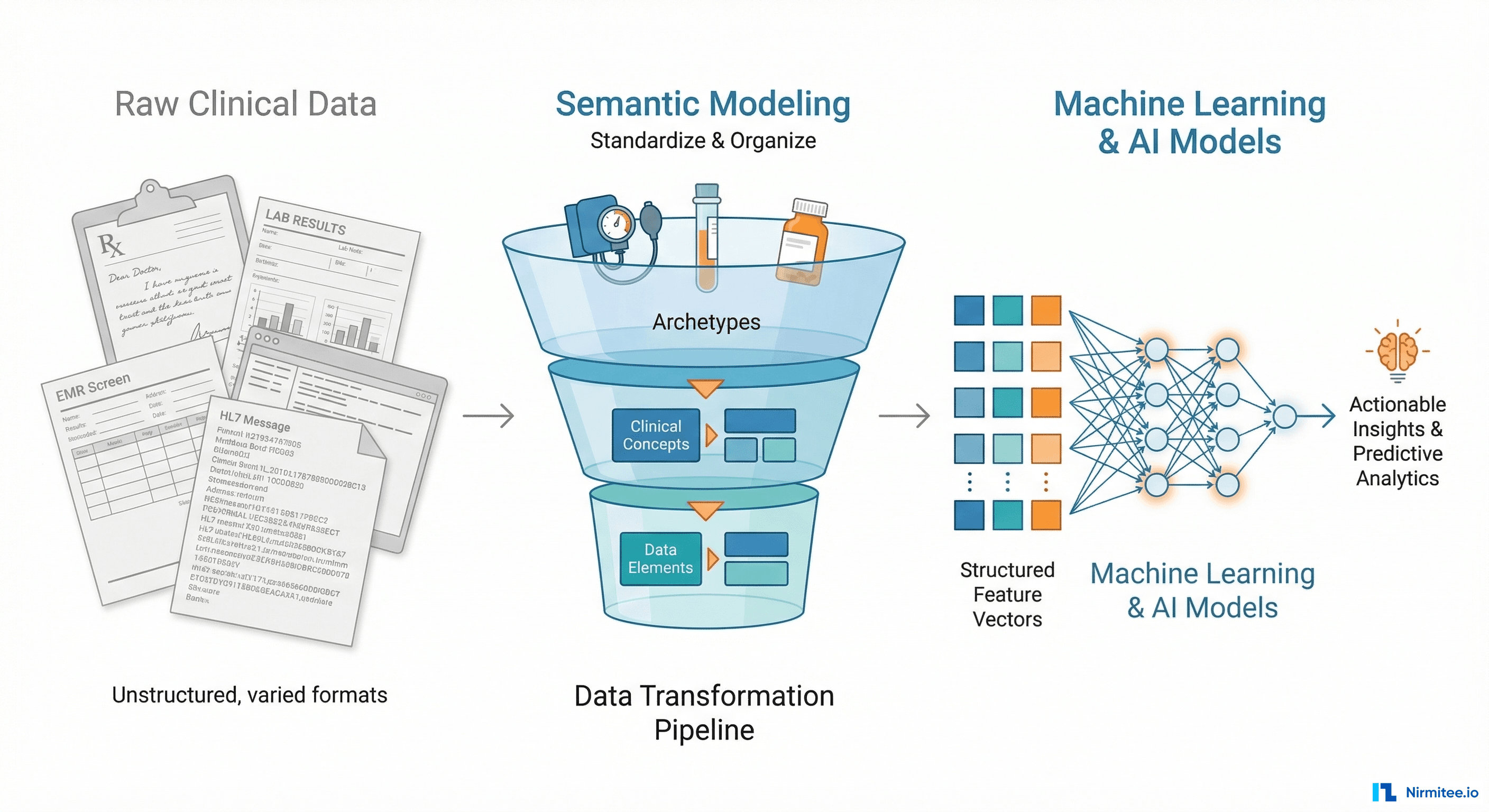
Why openEHR Makes Your Clinical Data AI-Ready (And Most EHR Architectures Don't)
