You have built something patients and providers actually need. Your pilot is promising. Investors are asking about your integration roadmap. And then someone drops the question that sends every healthtech founder spiraling: How are you going to integrate with Epic?
If you are building a healthcare startup in 2026, EHR integration is not a matter of if but when and how. And the how matters enormously. The wrong approach can burn through six months of runway, alienate your first hospital customers, or lock you into a technical architecture that cannot scale past your Series A.
This guide is the decision framework we wish existed when we started building healthcare integration systems. It is written for seed-to-Series B healthtech founders and CTOs who need to make this decision with incomplete information, limited budget, and an investor timeline breathing down their necks. We cover when to integrate (hint: not always day one), the three paths available to you, how to evaluate each against your specific situation, and the mistakes that kill startups who get this wrong.

When Should You Actually Integrate with an EHR?
The first mistake founders make is assuming EHR integration must happen immediately. It does not. And integrating too early — before you have validated your core product — is one of the most expensive forms of premature optimization in healthtech.
Do Not Integrate on Day One
EHR integration is a force multiplier for a product that works. It is not a substitute for product-market fit. If your clinical workflow is not validated, if providers are not actively using your standalone product, then spending six figures and six months on Epic integration is building a highway to a destination nobody wants to visit.
Here is how to think about timing:
- Pre-seed / Early seed: Use manual data entry, CSV uploads, or patient-reported data. Your goal is to validate the clinical workflow, not the data pipeline. If providers will not use your product with manual data entry, they will not use it with an EHR feed either.
- Late seed / Pre-Series A: Build a FHIR-ready data model internally. Design your database schema around FHIR resources (Patient, Observation, Condition, MedicationRequest) even if you are not pulling data from EHRs yet. This costs almost nothing and saves months later.
- Series A / Growth: This is when EHR integration becomes a competitive necessity. You have paying customers, a validated workflow, and hospitals asking about integration as a condition of enterprise contracts. Now is the time to invest.
The reality is that EMR integrations after the MVP stage make a massive difference in hospital onboarding — but the operative phrase is after the MVP stage. Get the product right first.
The Three Signals That Say "Integrate Now"
You are ready for EHR integration when at least two of these are true:
- Enterprise deals are stalling on integration. You are hearing "we love this, but our IT team needs it to pull from Epic" in procurement conversations. Integration is the gap between pilot and contract.
- Manual data entry is creating clinical risk. Providers are re-keying data from the EHR into your system, creating transcription errors that could affect patient safety. This is not just inefficient — it is a liability.
- You have the budget to do it properly. EHR integration is not a weekend hack. If you cannot allocate $50,000-$200,000 and 2-6 months of engineering time (or equivalent), you are not ready. Underfunded integration attempts produce unreliable systems that damage your reputation with hospital IT teams.
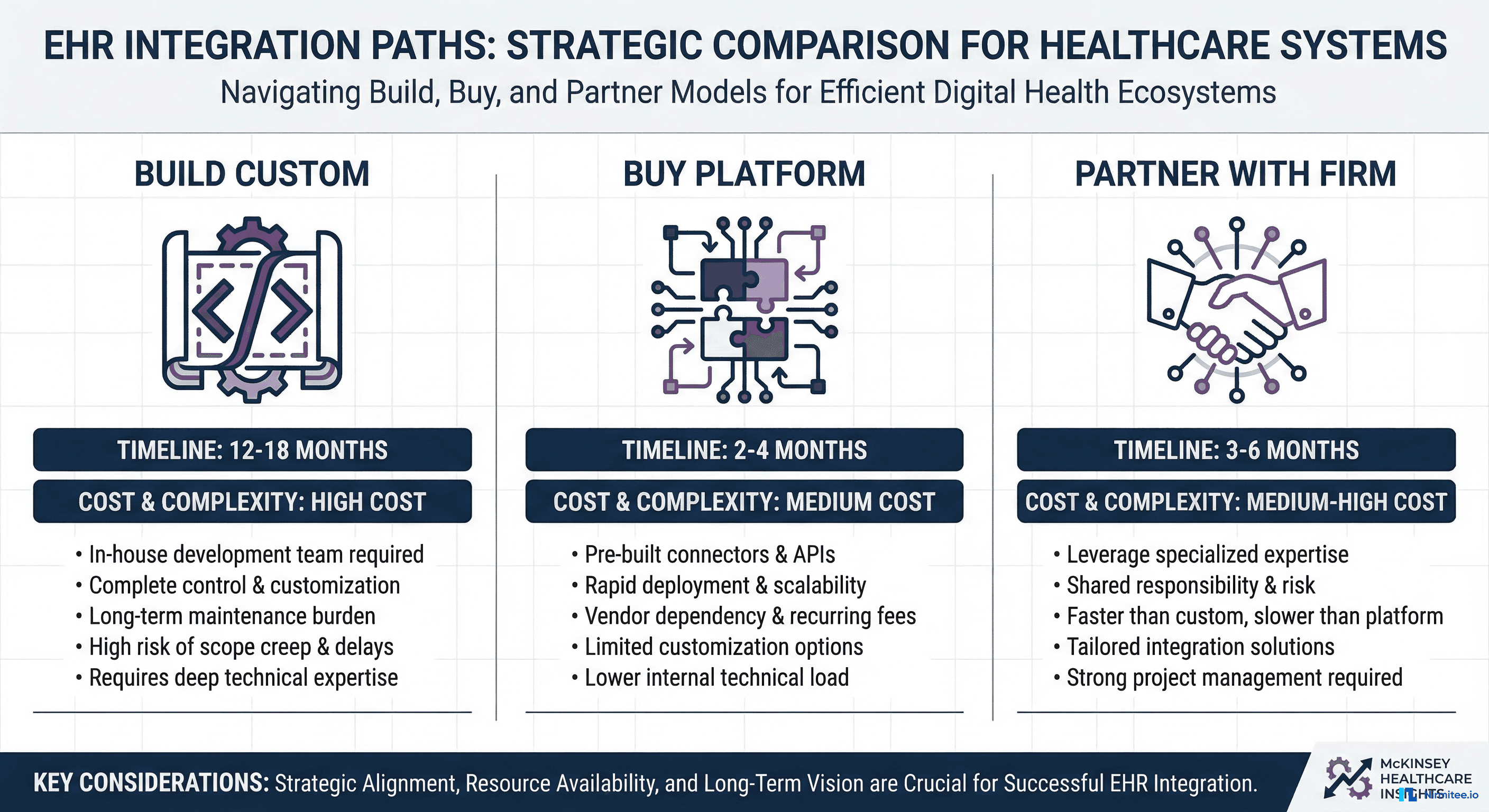
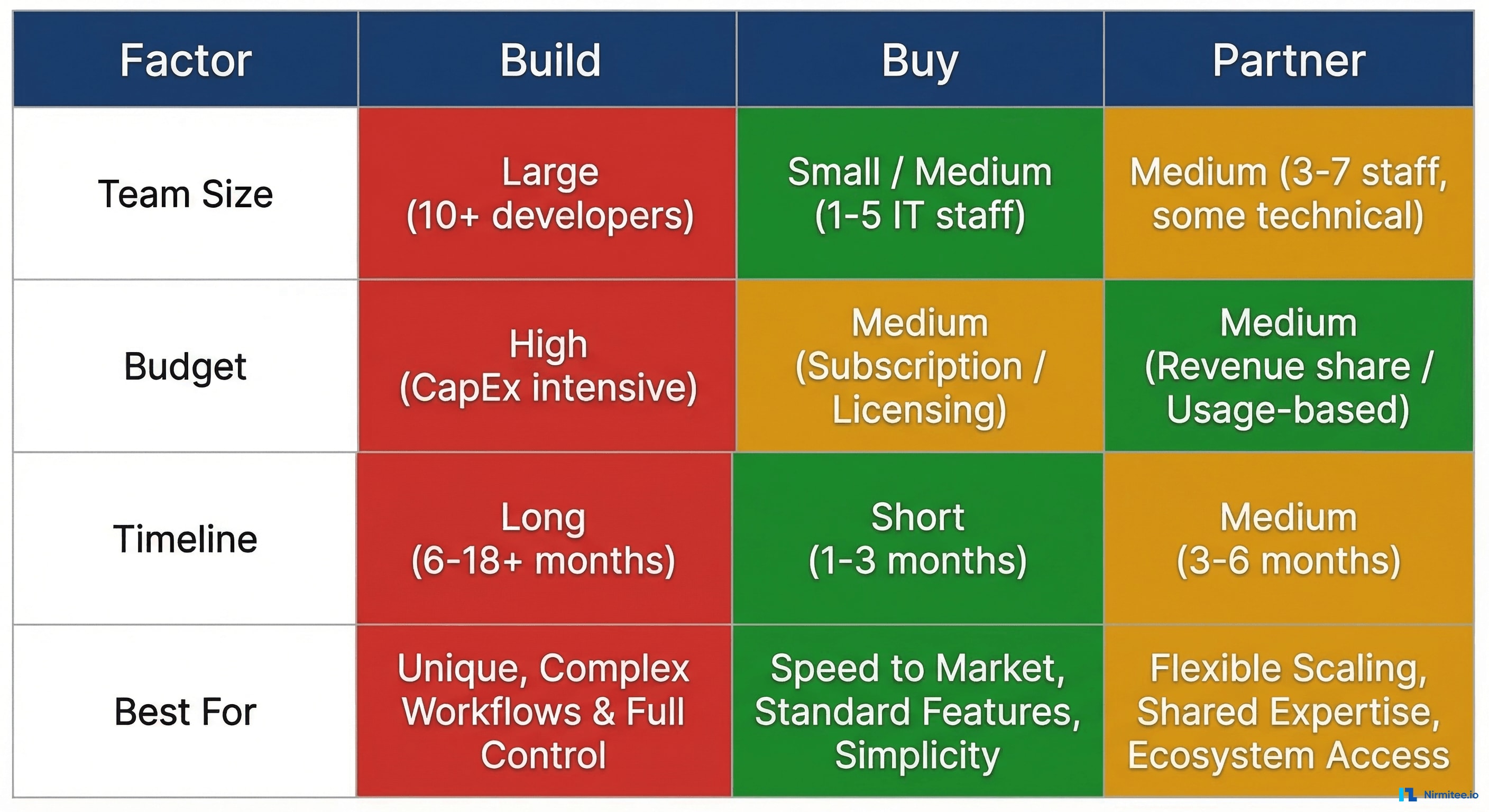
The Three Paths: Build, Buy, or Partner
Once you have decided to integrate, you face a three-way fork. Each path has genuine advantages and real trade-offs. There is no universally correct answer — the right choice depends on your team, timeline, budget, and how central EHR data is to your core product.

Path 1: Build Custom Integration
What it means: Your engineering team builds and maintains direct connections to EHR systems using their native APIs — FHIR R4, HL7v2 interfaces, or proprietary SDKs.
Realistic cost: $500,000 - $2,000,000+ over 12-18 months for a single major EHR (Epic or Oracle Health). This includes engineering salaries, sandbox licensing, certification costs, and the ongoing maintenance burden.
Realistic timeline: 12-18 months for deep, bidirectional integration. 6-9 months if you are only doing read-only data access via FHIR.
What you need on your team:
- 3-5 engineers with FHIR R4 and HL7v2 experience (these are rare — median salary $180K-$220K in the US)
- A compliance/security engineer who understands HIPAA, ONC certification, and the information blocking rules
- A project manager with health system implementation experience
When to choose this path:
- EHR integration is your product or a core differentiator (you are building an EHR, a clinical decision support tool, or a data platform)
- You need deep, bidirectional data flows — writing orders back to the EHR, updating clinical notes, triggering CDS alerts
- You are planning to connect to dozens or hundreds of health systems and need full control over the integration layer
- You have raised Series A+ and can afford the engineering investment
When to avoid this path:
- You are pre-Series A with a small engineering team
- You only need read-only access to patient demographics, conditions, and medications
- You need to be live with multiple EHR vendors in less than 6 months
Path 2: Buy an Integration Platform
What it means: You use a middleware platform — Redox, Health Gorilla, 1upHealth, Particle Health, or Zus Health — that provides a normalized API layer across multiple EHR systems.
Realistic cost: $50,000 - $200,000/year depending on volume, number of connections, and data types. Most platforms charge per-connection or per-message fees on top of a base subscription.
Realistic timeline: 2-4 months to first production connection. The platform handles the EHR-specific translation; you build to their API once.
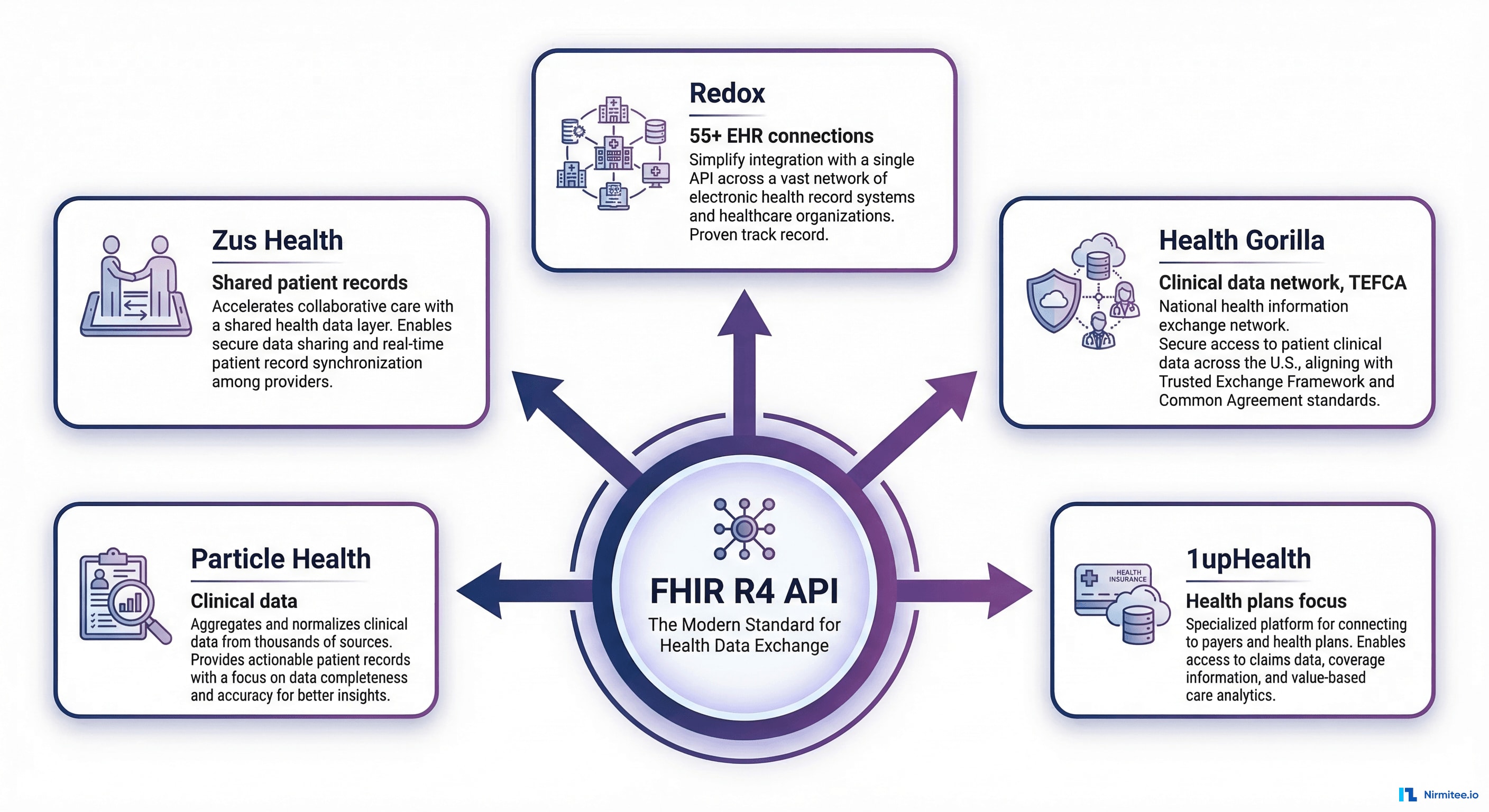
Platform landscape in 2026:
| Platform | Best For | EHR Connections | Key Differentiator |
|---|---|---|---|
| Redox | Broad EHR connectivity | 55+ EHR systems | Largest network of pre-built connections; strong HL7v2 + FHIR |
| Health Gorilla | Clinical data access | TEFCA-enabled network | First dual-designated QHIN/QHIO; strong for labs, ADT, pharmacy data |
| 1upHealth | Health plans / payers | FHIR-first | Claims + clinical data combination; CMS interoperability rule compliance |
| Particle Health | Clinical data retrieval | Nationwide network | Point-of-care clinical data from 300M+ patient records |
| Zus Health | Shared patient context | Aggregated view | Embeddable patient record with data from multiple sources |
When to choose this path:
- You need to connect to multiple EHR systems quickly (Epic, Oracle Health/Cerner, Meditech, Allscripts, athenahealth)
- Your integration needs are primarily read-only or standard data exchange patterns (ADT feeds, lab results, clinical documents)
- You want to minimize the healthcare-specific engineering burden on your team
- You need to show investors a credible integration story without hiring a FHIR team
When to avoid this path:
- You need deep write-back capabilities that the platform does not support
- Your use case requires custom HL7v2 message handling that does not map to the platform's normalized model
- You are cost-sensitive and the per-message fees will be prohibitive at scale
Path 3: Partner with a Healthcare Integration Firm
What it means: You engage a specialized healthcare IT consulting or engineering firm to design, build, and potentially maintain your EHR integrations. The firm brings domain expertise, existing EHR vendor relationships, and a team that has done this before.
Realistic cost: $150,000 - $400,000 for initial integration build-out, plus $3,000 - $10,000/month for ongoing maintenance and support.
Realistic timeline: 3-6 months for a production-ready integration, depending on complexity and EHR vendor responsiveness.
When to choose this path:
- You need deep, complex integrations but do not want to build a permanent healthcare engineering team
- Your product requires custom clinical workflows — prior authorization automation, clinical decision support, care coordination — that off-the-shelf platforms cannot handle
- You want someone who has navigated Epic's App Orchard review process or Oracle Health's certification before
- You are building EHR integrations that require understanding of both the technical and clinical sides
When to avoid this path:
- Your integration needs are simple and well-served by an off-the-shelf platform
- You want to own the full integration stack internally for competitive reasons
- You cannot afford the upfront project cost
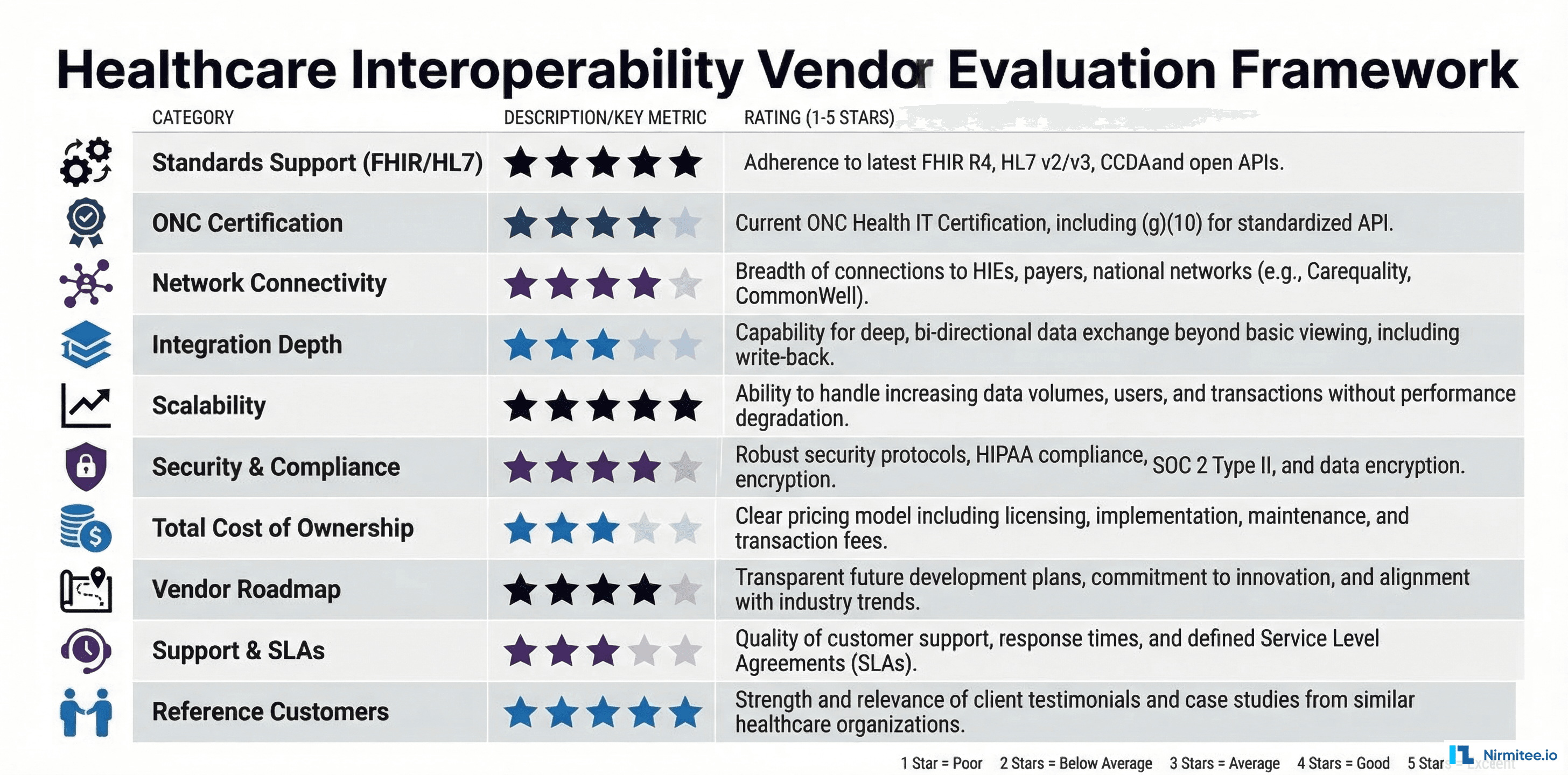
One thing to watch for: not all "healthcare integration firms" are equal. Look for firms that build on open standards (FHIR R4, SMART on FHIR, US Core profiles) rather than proprietary middleware. Ask to see their approach to avoiding common integration mistakes. If they cannot articulate how they handle information blocking compliance, HIPAA security requirements, and ONC certification, keep looking.
Navigating Epic and Oracle Health: What Startups Actually Need to Know
Epic and Oracle Health (formerly Cerner) together represent over 60% of the US hospital market. If you are building for health systems, you will almost certainly need to integrate with one or both. Here is what the vendor marketing pages do not tell you.
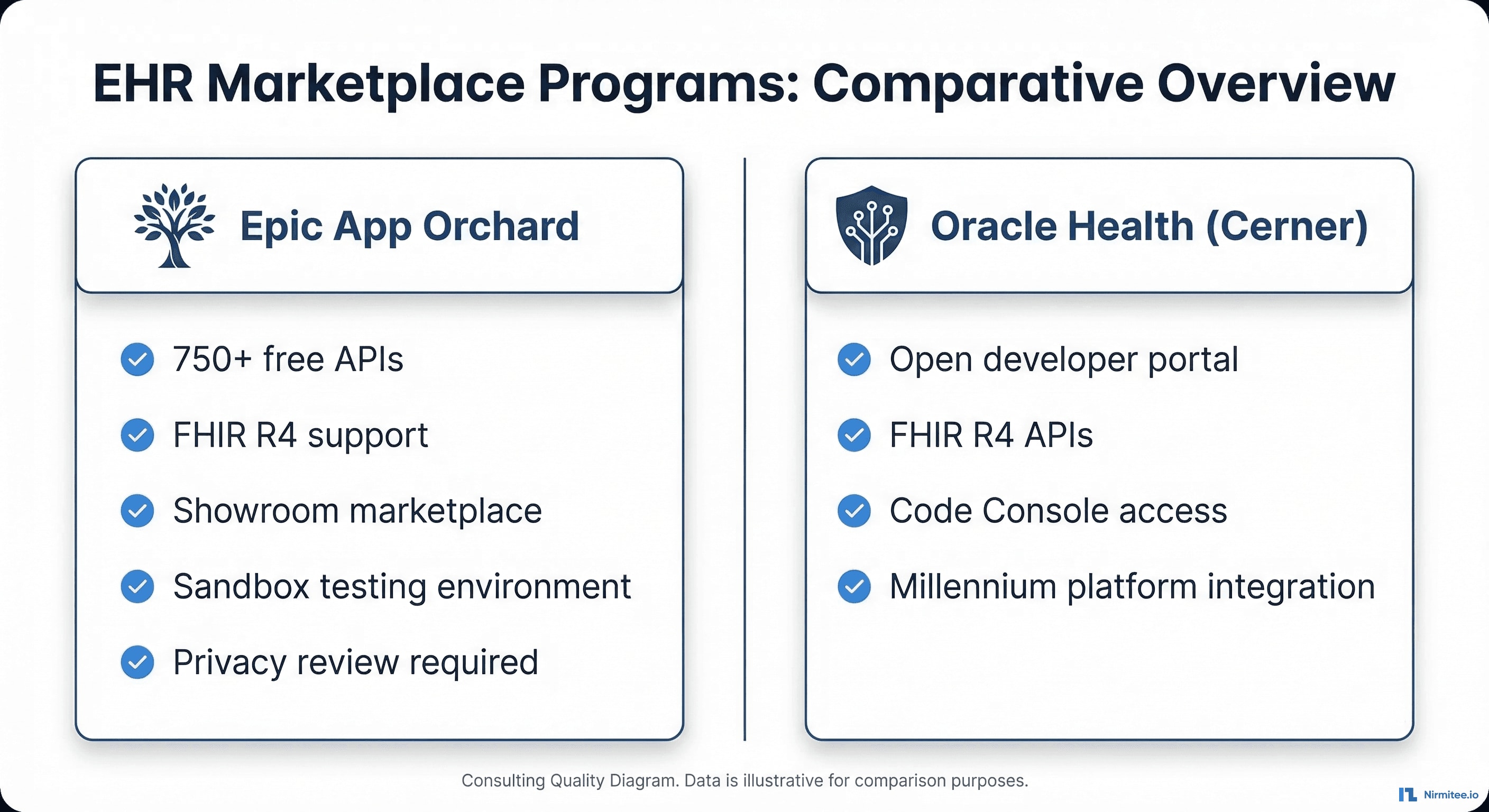
Epic: Open.Epic and the Showroom (formerly App Orchard)
Epic provides over 750 no-cost FHIR APIs through its Open.Epic developer portal. This is genuinely good news for startups — you can start building and testing against Epic's sandbox without any upfront cost or contractual commitment.
What the process actually looks like:
- Register on open.epic.com — Create a developer account. Free, takes 5 minutes.
- Access the sandbox — Epic's testing environment simulates a live EHR. You can test FHIR R4 API calls, SMART on FHIR authentication flows, and data retrieval against synthetic patient data.
- Build your integration — Develop against Epic's FHIR R4 APIs using standard OAuth 2.0 / SMART on FHIR for authentication. Epic supports both patient-facing (standalone launch) and provider-facing (EHR launch) apps.
- Apply for the Showroom — If you want to be listed in Epic's marketplace (which makes it dramatically easier for health systems to find and deploy your app), you need to go through Epic's review process. This includes a privacy and security review, functional testing, and demonstration that your app meets Epic's quality standards.
- Get deployed at a health system — Even with Showroom listing, each individual health system must approve and configure your app. This is where real-world deployment timelines stretch from weeks to months, depending on the health system's IT governance process.
Timeline reality check: From first API call to live production deployment at a health system, plan for 6-12 months minimum. The technical integration itself might take 2-3 months. The review process, security assessments, and health system IT approval cycles take the rest.
Key limitation: Epic's FHIR APIs are read-heavy. Writing data back to Epic (placing orders, updating notes, creating resources) requires more advanced integration patterns and often involves Epic's proprietary APIs or HL7v2 interfaces, not just FHIR.
Oracle Health (Cerner): The Post-Acquisition Landscape
Oracle's acquisition of Cerner has reshaped the developer experience. The legacy Cerner Code Console and fhir.cerner.com documentation have been consolidated under Oracle Health's developer portal.
What startups need to know:
- FHIR R4 APIs are available through Oracle Health's developer portal. The Millennium platform supports standard FHIR resources.
- The developer ecosystem is in transition. Oracle is actively modernizing Cerner's infrastructure, which means APIs, documentation, and developer tools are changing. Build against stable, documented endpoints and expect some migration work as Oracle rolls out updates.
- Oracle Health's marketplace is less mature than Epic's Showroom. Getting listed requires working with Oracle's vendor services team, and the process is less standardized than Epic's.
- Sandbox access is available through the developer portal. Quality is generally good for testing basic FHIR reads, but edge cases and write operations may require working directly with a partner health system's test environment.
Strategic consideration: If your target customers are primarily Epic shops, focus there first. If you are selling to a mix of EHR environments, you will eventually need both — and this is where integration platforms (Path 2) or experienced partners (Path 3) save significant time.
Realistic Timeline Expectations
Every founder asks: "How long will this take?" The honest answer depends on what you are building, which path you choose, and how responsive your EHR vendor and health system partners are.

Basic Read-Only Integration (3-6 Months)
You are pulling patient demographics, conditions, medications, allergies, and lab results from the EHR via FHIR R4 APIs. No write-back. No custom clinical workflows.
- Month 1-2: Sandbox setup, FHIR API exploration, authentication implementation (SMART on FHIR), data model mapping
- Month 2-4: API development, error handling, data transformation, unit and integration testing
- Month 4-6: Health system IT review, security assessment, pilot deployment, production go-live
Moderate Integration with Write-Back (6-9 Months)
You are reading patient data and writing back structured data — lab results, clinical notes, or care plan updates. This requires bidirectional FHIR or HL7v2 interfaces.
- Month 1-3: Architecture design, sandbox development, write-back API implementation, HL7v2 message development if needed
- Month 3-6: Integration testing with health system test environment, data validation, error recovery, clinical workflow testing with end users
- Month 6-9: Security review, compliance verification, staged rollout, production monitoring
Deep Bidirectional Integration (9-12+ Months)
You are deeply embedded in the clinical workflow — triggering CDS alerts, placing orders, managing referrals, or automating prior authorization. This is where Epic integration complexity really shows.
- Month 1-4: Detailed workflow analysis with clinical stakeholders, architecture design, sandbox development, custom interface development
- Month 4-8: Iterative testing with clinical end users, HL7v2 + FHIR hybrid integration, EHR vendor review and certification, compliance and security assessment
- Month 8-12+: Pilot deployment at 1-2 sites, clinical validation, production scaling, ongoing optimization
The hidden timeline killer: Health system IT departments. Even when your technical integration is complete, getting through a health system's IT governance, security review, and change management process can add 2-4 months. Factor this into every estimate you give to investors and customers.
ONC Certification: Do You Need It?
The short answer: probably not right away, but you need to understand the landscape.
ONC Health IT Certification is required for EHR systems and certain health IT modules that health systems use to meet federal requirements (Promoting Interoperability, MIPS). If you are building a certified EHR or a module that plugs into the certification ecosystem, you will eventually need ONC certification.
If you are building a standalone application that reads data from EHRs (a clinical analytics tool, a patient engagement app, a care coordination platform), you likely do not need ONC certification. You need to:
- Support FHIR R4 APIs and US Core profiles for data access
- Implement SMART on FHIR for authentication and authorization
- Comply with HIPAA security and privacy requirements
- Understand and comply with the information blocking rules (21st Century Cures Act) — you cannot build features that restrict, delay, or block patient access to their data
If you are building a health IT module that health systems will use for certified workflows (e.g., clinical decision support, computerized physician order entry, electronic prescribing), you may need to go through the ONC certification process. This involves:
- Testing by an ONC-Authorized Testing Laboratory (ONC-ATL)
- Certification by an ONC-Authorized Certification Body (ONC-ACB)
- Ongoing surveillance and maintenance of certification
- Timeline: 6-12 months from initial application to certification, plus $50,000-$150,000 in testing and certification fees
The practical takeaway for most startups: Focus on building FHIR R4-compliant interfaces with SMART on FHIR authentication. This positions you to work with certified EHR systems without requiring your own ONC certification. When you grow to the point where certification is needed, your standards-based architecture makes the process dramatically simpler.
Seven Mistakes That Kill Healthcare Startup EHR Integrations
We have seen these patterns destroy timelines, burn budgets, and damage startup-hospital relationships. Every one of them is avoidable.

1. Underestimating the Effort
The single most common mistake. Founders see "FHIR API" and think it is like integrating with Stripe or Twilio. It is not. Healthcare data is messy, inconsistent, and governed by complex regulations. Every health system configures their EHR differently. The same FHIR resource can contain radically different data depending on how the system was implemented.
Reality check: Budget 2-3x what you think the integration will cost, and 1.5-2x the timeline. If your estimate is "one engineer, three months," you probably need two engineers and six months.
2. Skipping Sandbox Testing
Founders sometimes try to go directly to a partner health system's test environment, skipping the EHR vendor's sandbox entirely. This is a mistake because sandbox environments are designed for development iteration — you can break things, test edge cases, and experiment without affecting a health system's patience or goodwill.
What to do: Spend at least 4-6 weeks in the EHR vendor's sandbox before touching a health system's test environment. Document every API call, response format, and edge case you discover.
3. Ignoring Information Blocking Rules
The 21st Century Cures Act's information blocking provisions are actively enforced as of 2026. If your product restricts, delays, or makes it harder for patients or providers to access health data, you are potentially in violation — with penalties of up to $1 million per violation for health IT developers.
What to do: Design your integration to facilitate data access, not restrict it. Support standard data export formats. Do not build features that lock health data inside your system. Understand the eight exceptions to the information blocking rule so you know what is and is not permitted.
4. Building Before Product-Market Fit
We covered this above, but it bears repeating: EHR integration is a force multiplier, not a product strategy. If providers are not using your standalone product, adding an EHR integration will not fix the underlying problem.
5. Not Planning for Ongoing Maintenance
EHR integrations are not set-and-forget. EHR vendors release updates that break existing integrations. Health systems change their configurations. FHIR specifications evolve. Plan for 15-20% of initial development cost as annual maintenance.
6. Choosing the Wrong Integration Approach
A startup that needs to connect to 15 different EHR systems should not be building custom integrations for each one. A startup whose core product is a clinical decision support tool embedded in the EHR workflow probably should not be relying on a generic middleware platform that does not support deep CDS hooks.
What to do: Use the decision matrix above. Be honest about your team's capabilities, your budget, and your timeline. There is no shame in buying or partnering — the goal is to ship, not to prove you can build everything from scratch.
7. Ignoring the Human Side
Every EHR integration ultimately involves people — hospital IT teams, clinical champions, procurement committees, compliance officers. The technical integration is only half the battle. You need someone on your team who can navigate the relationship dynamics of health system partnerships.
What to do: Invest in customer success and implementation support from day one. The startups that win enterprise health system contracts are the ones that make IT directors' lives easier, not harder.
Your Integration Roadmap: A Practical Checklist
Whether you choose to build, buy, or partner, this checklist applies to every healthtech startup approaching EHR integration.
Before You Start
- Validate that EHR integration will meaningfully improve your product's value proposition (not just "nice to have")
- Identify your first 2-3 target health systems and confirm which EHR platforms they use
- Budget appropriately: minimum $50K for platform approach, $150K+ for custom build or partner engagement
- Assign a dedicated project owner (not a part-time engineer who is also building features)
Architecture Decisions
- Design your internal data model around FHIR R4 resources from day one — even before you connect to any EHR
- Implement SMART on FHIR authentication (OAuth 2.0 + OIDC) as your standard auth pattern
- Build a data transformation layer that can normalize data from different EHR sources into your internal format
- Plan for both FHIR R4 (modern, growing) and HL7v2 (legacy, still dominant for ADT and orders) interfaces
Compliance and Security
- Complete a HIPAA security risk assessment before your first production integration
- Document your information blocking compliance posture — how does your product facilitate (not restrict) data access?
- Implement audit logging for all EHR data access
- Get a SOC 2 Type II audit on your roadmap — most health systems will require it for enterprise contracts
Go-to-Market
- Register on Open.Epic (free) and Oracle Health's developer portal even before you start building — familiarize your team with the documentation and sandbox
- Build relationships with health system IT directors at your target accounts early — they are the gatekeepers
- Create a clear integration architecture document you can share with health system IT teams during procurement
- Plan for 2-4 months of health system IT review and security assessment after your technical integration is complete
The Bottom Line for Founders
EHR integration is not optional for healthcare startups that want to sell to health systems. But it is also not the insurmountable obstacle that some founders fear. The key is making the right decision at the right time with the right approach for your specific situation.
If your core product is the EHR integration itself, build it. If you need broad connectivity fast, buy a platform. If you need deep clinical workflows but do not have the team, partner with a firm that has done it before.
Whatever path you choose, build on open standards — FHIR R4, SMART on FHIR, US Core profiles. The regulatory environment (ONC certification, information blocking enforcement, TEFCA) is pushing relentlessly toward standardization. Startups that build on open standards today will have a structural advantage over those that lock themselves into proprietary integrations.
And remember: the health systems you are selling to have seen dozens of startups promise seamless integration and fail to deliver. The ones that win are the ones that show up with a realistic timeline, a credible technical approach, and the humility to ask the right questions before they start building.
Frequently Asked Questions
How much does EHR integration cost for a startup?
Costs vary dramatically by approach. Using an integration platform (Redox, Health Gorilla, 1upHealth) typically costs $50,000-$200,000 per year. Building custom integrations runs $500,000-$2,000,000+ over 12-18 months. Partnering with a healthcare integration firm costs $150,000-$400,000 for initial build-out plus $3,000-$10,000/month for ongoing support. The right choice depends on your team size, timeline, and how central EHR data is to your core product.
How long does it take to integrate with Epic?
For basic read-only FHIR API access (patient demographics, conditions, medications), plan for 3-6 months from first API call to production deployment. For bidirectional integration with write-back capabilities, plan for 6-12 months. The biggest timeline variable is not the technical development — it is the health system IT review, security assessment, and deployment approval process, which can add 2-4 months beyond technical completion.
Do I need ONC certification for my healthtech startup?
Most healthtech startups do not need ONC certification initially. ONC certification is required for certified EHR modules used in federal programs (Promoting Interoperability, MIPS). If you are building a standalone application that reads data from EHRs via FHIR APIs, you do not need ONC certification — but you do need to comply with HIPAA, support FHIR R4/US Core profiles, and understand the information blocking rules under the 21st Century Cures Act.
What is the difference between FHIR and HL7v2 for startups?
FHIR R4 is the modern, RESTful API standard for healthcare data exchange — think JSON over HTTPS, similar to any modern web API. HL7v2 is the legacy messaging standard that still handles the majority of real-time clinical data exchange (ADT notifications, lab results, orders). Most startups should build FHIR-first for new integrations, but be prepared to handle HL7v2 for use cases where FHIR coverage is incomplete — particularly real-time ADT feeds and order workflows. Many health systems will require both.
Should I use Redox, Health Gorilla, or build my own integration?
Use Redox if you need broad EHR connectivity (55+ systems) and standard data exchange patterns. Use Health Gorilla if you need clinical data access through TEFCA-enabled nationwide networks, especially for labs and pharmacy data. Build your own if EHR integration is your core product differentiator and you have the engineering team to maintain it. For complex clinical workflows that off-the-shelf platforms cannot handle, consider partnering with a specialized healthcare integration firm that builds on open standards.