Overview
When it comes to building scalable, secure, and interoperable healthcare systems, two names dominate the conversation - OpenEHR and HL7 FHIR. Although they are frequently mentioned together, their core objectives, architectures, and use cases differ significantly. If you're wondering which one to pick for your digital health platform, you're not alone.
This blog dives deep into what makes FHIR and OpenEHR unique, how they serve different purposes, and how to decide which one or even both may be right for your project.
Understanding Different Healthcare Domains
Before diving into FHIR and openEHR, it's essential to understand the core domains in healthcare IT that they support.
These include clinical and administrative use, data exchange, and longitudinal analysis. Each of these domains has different demands and workflows that influence the type of data architecture and standards best suited to support them.
Clinical and Administrative Workflows
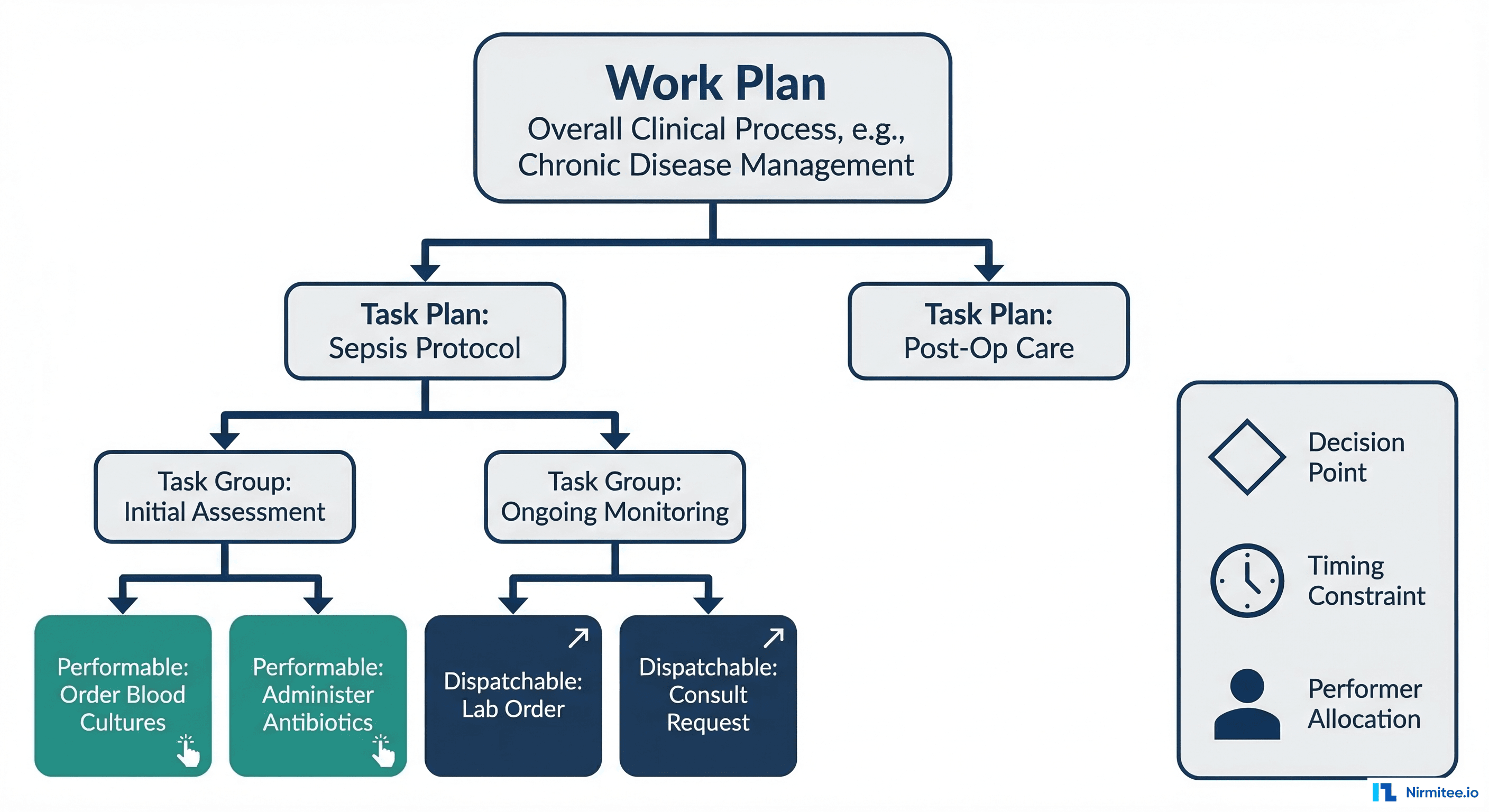
Clinical workflows involve patient care activities like recording vital signs, prescribing medications, or noting symptoms. Administrative workflows include scheduling, billing, or compliance documentation. These tasks require a system that can store, query, and retrieve detailed clinical data over time with high accuracy and granularity. This is where openEHR excels. It is designed to manage complex, longitudinal health records and is built with clinical persistence in mind.
Data Exchange
Interoperability is key to modern healthcare. Hospitals, labs, insurance companies, and specialists must share patient data efficiently and securely. This is where HL7 FHIR performs exceptionally well. FHIR is tailored for data exchange and supports common use cases like patient referrals, lab order transmissions, or health insurance claims through RESTful APIs and standard resource models.
Longitudinal Analysis
For researchers and public health officials, being able to analyze patient data over time is critical. This is where the OMOP Common Data Model comes into play.OMOP is not a clinical data model but an analytical one. It structures data in a way that's ideal for large-scale statistical analysis, like identifying trends across populations or understanding treatment effectiveness.
Understanding FHIR
FHIR (Fast Healthcare Interoperability Resources) is developed by HL7 and is a standard designed for exchanging healthcare information electronically. Built on modern web standards like REST, JSON, and XML, FHIR is accessible and easy to implement for developers.
The primary goal of FHIR is to make it easier to share healthcare data between systems. It is particularly useful in contexts where information needs to be retrieved quickly and efficiently across organizational boundaries. FHIR uses modular "resources" to represent discrete data elements such as Patient, Observation, or MedicationRequest, and allows for flexibility and scalability through these building blocks.
FHIR's success lies in its pragmatism: it follows the 80/20 rule, meaning it aims to cover 80% of common use cases with standard resources while leaving the remaining 20% to be handled through extensions. This makes it ideal for projects that require fast development, flexible data exchange, and straightforward integration with existing systems.
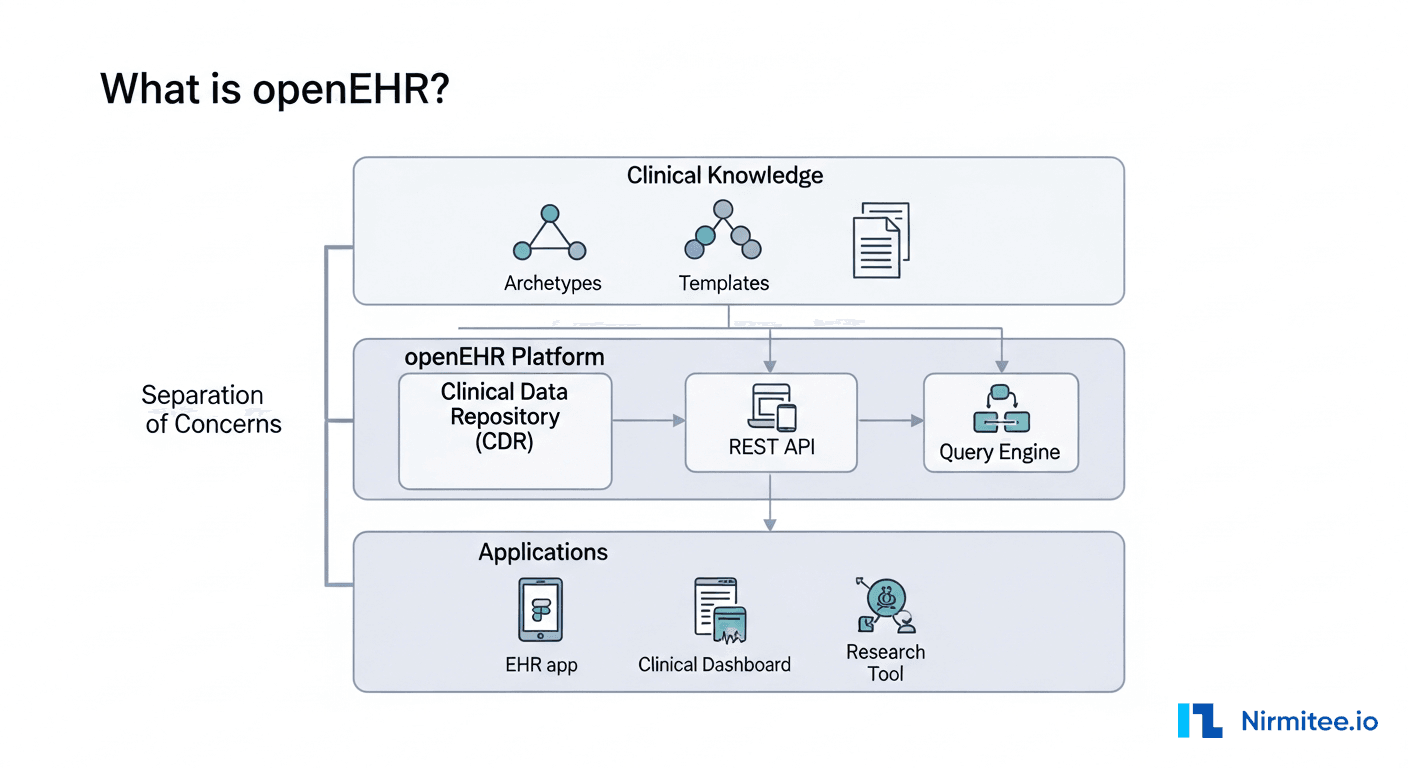
Understanding OpenEHR
OpenEHR, on the other hand, is focused on the long-term persistence and structure of health records. It provides a robust framework for capturing and storing rich clinical data using a two-level modeling approach: the Reference Model and Archetypes.
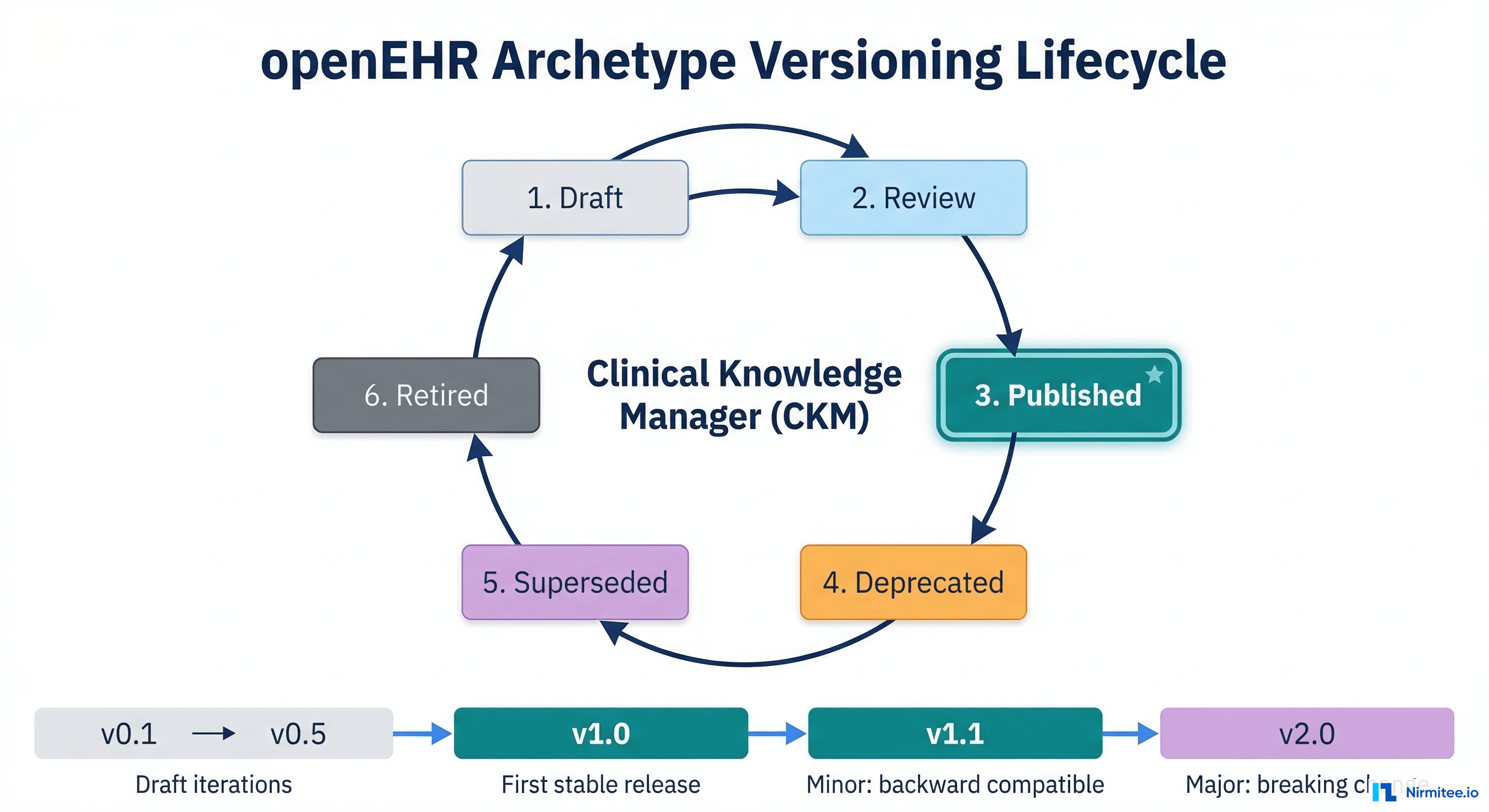
Archetypes are reusable and standardized clinical content models that ensure consistency and interoperability across different implementations. With over 800 active archetypes, openEHR allows for highly detailed clinical documentation that can evolve over a patient's lifetime.
OpenEHR is not just a data storage format but a full-stack health information platform. It supports complex queries, semantic interoperability, and longitudinal data management, making it highly suited for EHR systems, chronic disease management platforms, and other scenarios requiring precise and comprehensive data capture. [Read more - What is OpenEHR and How to Use It in Healthcare Software Development]
The Difference Between FHIR and openEHR
The fundamental difference between FHIR and openEHR lies in their primary purpose. FHIR is primarily designed for data exchange, while openEHR is designed for data persistence and structuring.
According to a comparative analysis from Allwell-Brown and Eneimi (2016), FHIR's main goal is to facilitate EHR data exchange. It focuses on making interoperability easier by using modular resources.
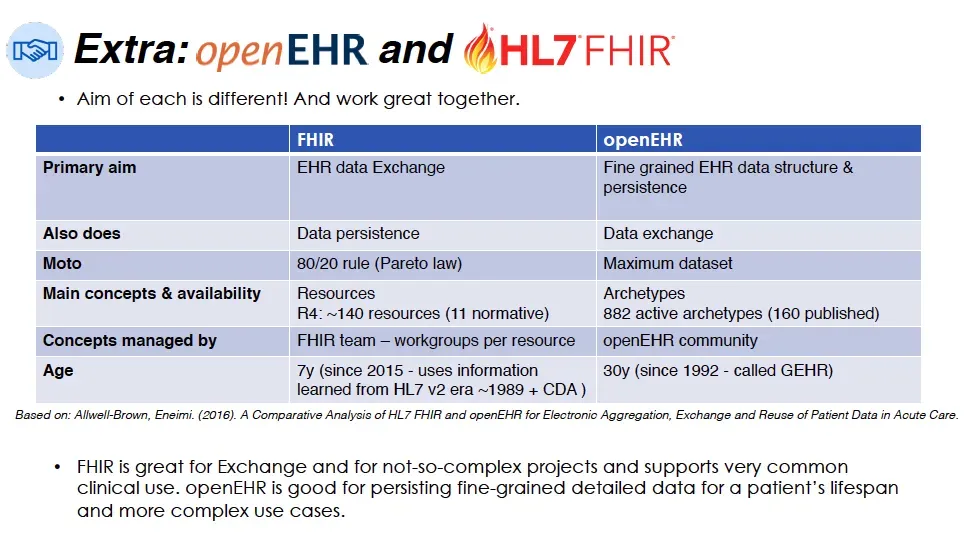

OpenEHR, in contrast, aims to provide a fine-grained data structure for persisting health information. It has been in development since the early 1990s and now features over 800 archetypes, with 160 of them officially published. These archetypes are managed by the openEHR community, and they represent a rich set of reusable clinical models.
FHIR is managed by the HL7 FHIR team, with workgroups organized per resource. It is highly developer-friendly and well-suited for lightweight, API-driven applications. openEHR, by contrast, requires more upfront planning and modeling but rewards that investment with highly reusable, scalable, and semantically rich data structures.
To summarize:
- FHIR is ideal for data exchange, especially in short-term and cross-institutional scenarios.
- OpenEHR is ideal for data persistence, especially in long-term, patient-centric systems where detailed data is needed.
The Right Choice: openEHR or FHIR?
Choosing between openEHR and FHIR depends heavily on your project's goals.
If your priority is interoperability, the ability to exchange information between hospitals, labs, pharmacies, and other systems, FHIR should be your go-to choice. It's fast, lightweight, and supported widely across modern health IT systems.
For example, a lab results app or a telemedicine platform that needs to fetch patient data from multiple EHR systems could benefit from FHIR's standardized APIs.
If your project requires clinical depth and long-term data integrity, openEHR is the better fit. Systems like chronic care management platforms, mental health apps, or full-scale EHRs benefit from openEHR's robust data models. The ability to model clinical processes and store detailed records that evolve makes it ideal for comprehensive, longitudinal care.
Utilizing Both: OpenEHR + FHIR
Interestingly, it's not always a matter of either/or. Many systems successfully use both standards to leverage their strengths. A popular architectural approach is to use openEHR as the system of record, storing all the clinical data in its richly structured archetypes, while exposing selected data through FHIR APIs for external systems to access.
This combination provides the best of both worlds: deep, reusable clinical content through openEHR and flexible, developer-friendly interoperability through FHIR. This dual strategy aligns with real-world healthcare needs, where both data depth and exchange are critical.
OMOP: When to Use It and How It Differs?
OMOP (Observational Medical Outcomes Partnership) is a common data model designed for health research. Unlike openEHR and FHIR, which focus on clinical workflows and interoperability, OMOP is optimized for analytics.
OMOP transforms clinical data into a standardized format that supports observational research, comparative effectiveness studies, and large-scale data analysis. It resembles a SQL-like structure and comes with built-in vocabularies and coding systems.
Use OMOP when your goal is population-level insights, such as studying treatment outcomes across thousands of patients, not for direct clinical care. In some implementations, data from openEHR or FHIR-based systems is transformed into OMOP for secondary use in research environments.
Conclusion
FHIR and openEHR each bring something unique to the table. FHIR shines in lightweight, fast-paced data exchange. openEHR provides a foundation for detailed, patient-centric clinical data persistence. The right choice depends on your use case.
For exchange, go FHIR. For persistence and modeling, go openEHR. And when needed, integrate both. By understanding their strengths and working with them in tandem, you can build a healthcare solution that's not just compliant and functional, but also future-ready.
Struggling with healthcare data exchange? Our Healthcare Interoperability Solutions practice helps organizations connect clinical systems at scale. We also offer specialized Healthcare Software Product Development services. Talk to our team to get started.