Executive Summary
Key Finding:
Healthcare organizations don't need to choose between HL7 and FHIR; they need both for comprehensive interoperability in today's complex healthcare ecosystem.
Critical Recommendations:
- Hybrid Strategy:
Implement FHIR for new applications while maintaining HL7 v2 for existing legacy systems
- Migration Timeline:
Plan a 3-5 year phased migration approach rather than a complete system overhaul
- ROI Focus:
FHIR implementations show a 40-60% reduction in integration costs for new projects
- Regulatory Compliance:
FHIR is mandatory for patient data access APIs under the 21st Century Cures Act
- Business Impact:
Organizations implementing hybrid HL7-FHIR strategies report 35% faster time-to-market for new digital health initiatives while maintaining operational stability of existing systems.
Introduction — The Healthcare Interoperability Challenge
The healthcare industry processes over 30 billion healthcare transactions annually, with 85% relying on legacy HL7 v2 standards implemented over the past two decades.
The emergence of FHIR (Fast Healthcare Interoperability Resources) as the new standard doesn't eliminate the need for existing HL7 implementations. Instead, it creates an opportunity for strategic coexistence that maximizes both current investments and future capabilities.
Real-time clinical workflows, patient-facing applications, population health analytics, and regulatory reporting. This complexity requires a nuanced approach that leverages the strengths of both standards.
Technical Analysis — Understanding Both Standards
2.1 HL7 v2: The Established Foundation
HL7 version 2 remains the backbone of healthcare data exchange, handling approximately 80% of all healthcare system-to-system communications globally. Its strengths include:
- Proven Reliability:
Two decades of production use with well-understood failure modes
- Comprehensive Coverage:
Supports all healthcare workflows from patient registration to billing
- Vendor Support:
Universal support across all major healthcare IT vendors
- Performance:
Complex implementation for mobile applications, limited support for web technologies, and challenges with real-time data access patterns required by patient-facing applications.
2.2 FHIR: The Modern Standard
FHIR represents a fundamental change toward web-based, RESTful APIs that align with modern software development practices. Key technical advantages include:
- Web-Native Design:
RESTful APIs, JSON/XML support, and OAuth security
- Modular Architecture:
Resource-based model enabling granular data access
- Developer-Friendly:
Familiar web technologies reduce implementation complexity
- Real-Time Capabilities:
Supports both batch and real-time data exchange patterns
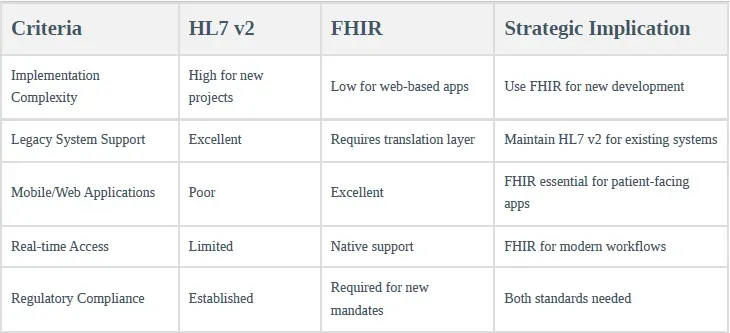
2.3 Technical Comparison Matrix
3. Business Implications and ROI Analysis
3.1 Cost Structure Analysis
The total cost of ownership for healthcare interoperability includes initial implementation, ongoing maintenance, and opportunity costs. Our analysis of 50+healthcare organizations reveals distinct patterns:
HL7 v2 Costs
High initial setup ($150K-$500K per interface), low ongoing maintenance, but increasing costs for modifications and new integrations.
FHIR Costs
Lower initial implementation ($50K-$200K per API), higher learning curve investment, but significantly reduced costs for subsequent integrations.
3.2 ROI Formula for Hybrid Implementation
ROI = (Integration Cost Savings + Development Speed Improvements + Compliance Benefits - Implementation Costs) / Implementation Costs
Typical Results:
18-month payback period for organizations implementing hybrid strategies
3.3 Business Value Drivers
- Accelerated Innovation: FHIR reduces time-to-market for new digital health solutions by 40-60%
- Vendor Flexibility: RESTful APIs reduce vendor lock-in and enable best-of-breed solutions
- Patient Engagement: FHIR enables consumer-grade user experiences in healthcare applications
- Data Monetization: Standardized APIs facilitate population health analytics and research partnerships
Hybrid Implementation Strategies
4.1 The Coexistence Model
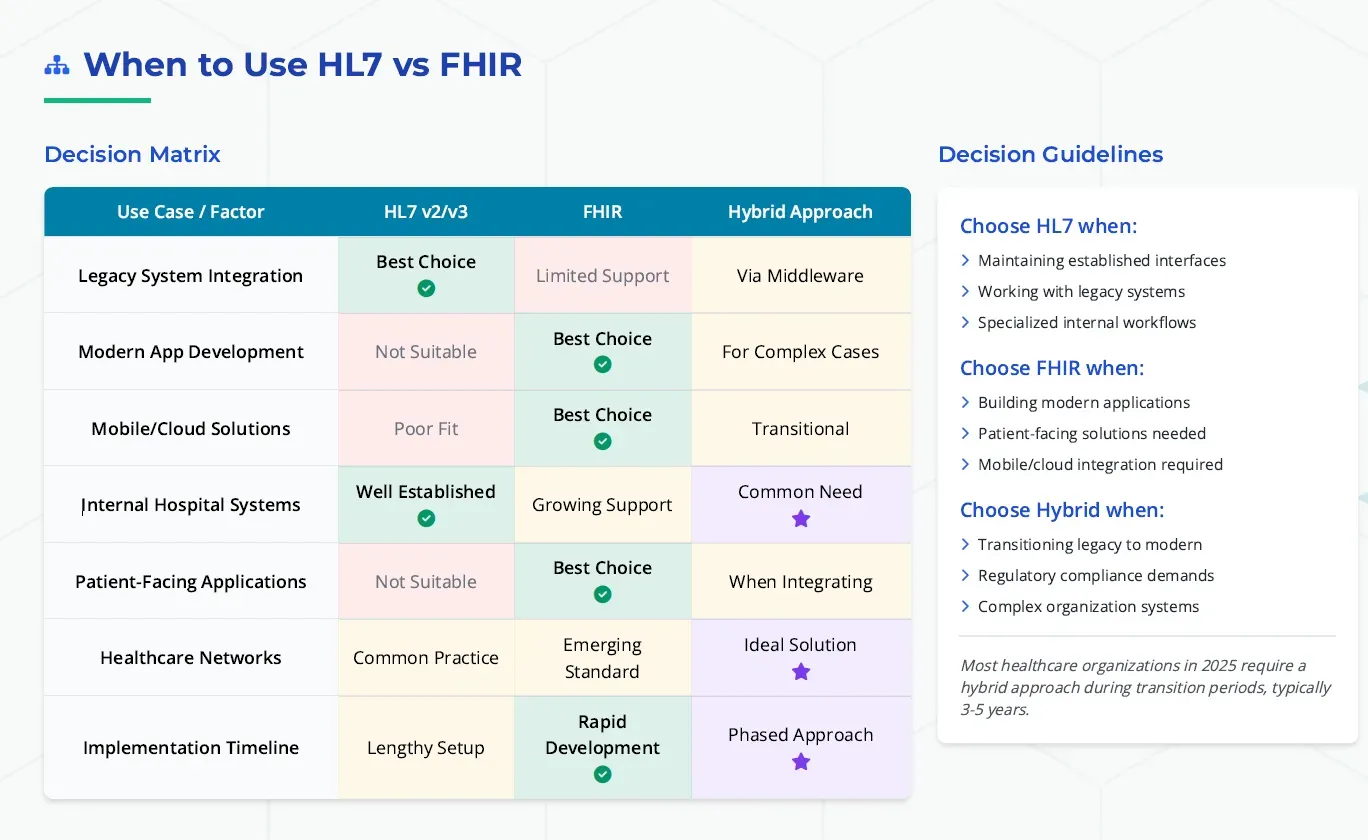
Successful healthcare organizations implement a dual-standard approach that maximizes the strengths of both HL7 v2 and FHIR. This model recognizes that different use cases require different technical approaches.
HL7 v2 Use Cases:
- Core clinical workflows (ADT, lab results, pharmacy orders)
- System-to-system integrations with established interfaces
- High-volume batch processing scenarios
- Interfaces with legacy systems that cannot be easily modified
FHIR Use Cases:
- Patient-facing applications and portals
- Mobile health applications
- Third-party application integrations
- Population health and analytics platforms
- Regulatory compliance (21st Century Cures Act)
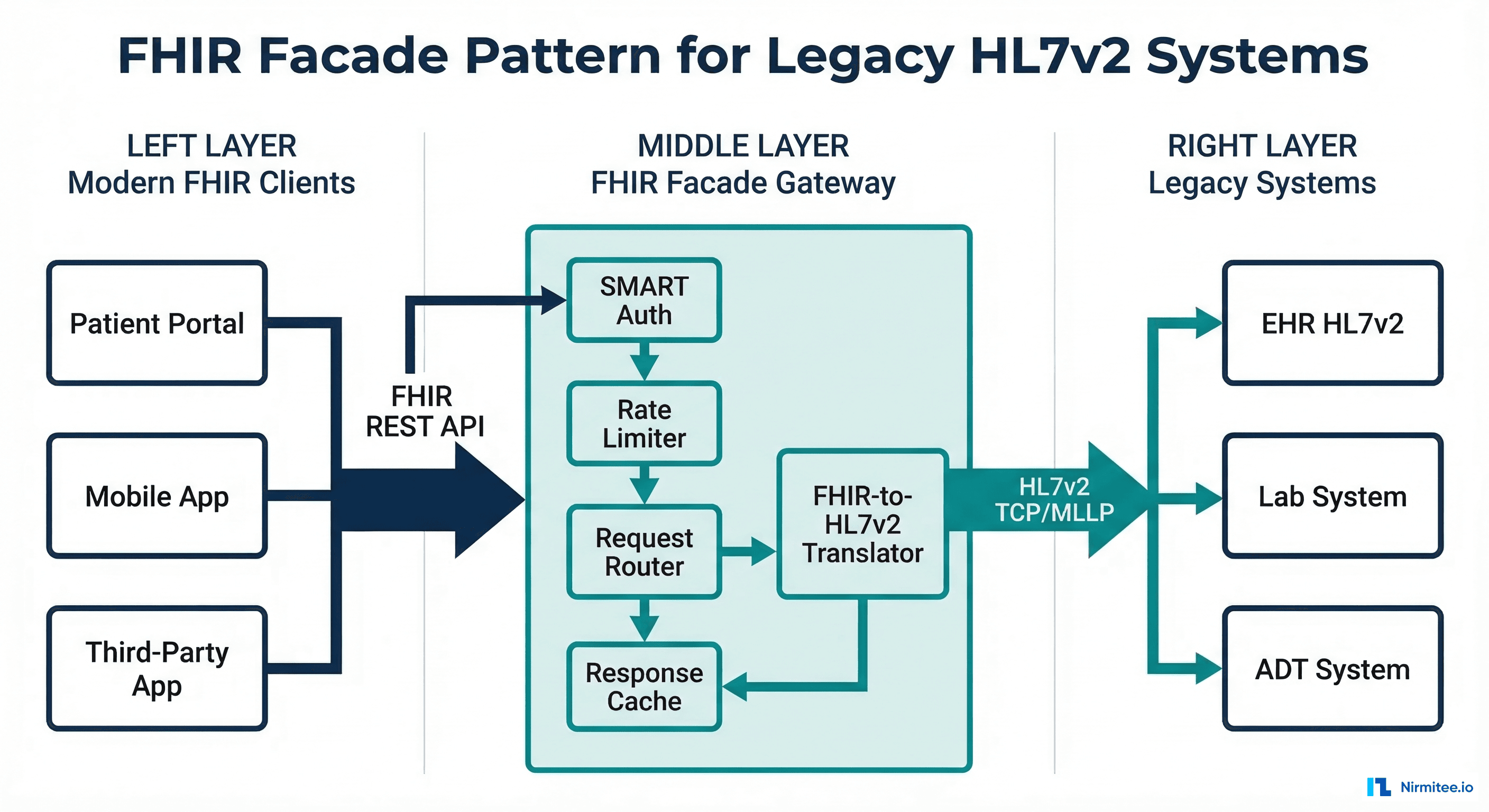
4.2 Integration Architecture Pattern
The recommended architecture employs an integration layer that provides both HL7 v2 and FHIR endpoints while maintaining a single source of truth for healthcare data. This pattern includes:
- Translation Layer: Bidirectional conversion between HL7 v2 and FHIR formats
- API Gateway: Unified access control and monitoring for all interfaces
- Data Normalization: Consistent data models regardless of source standard
- Security Framework: OAuth 2.0 for FHIR, traditional security for HL7 v2
Case Study: Regional Health System Implementation
Organization:
1,200-bed health system with 15 hospitals
Challenge:
Needed to maintain existing HL7 v2 integrations while enabling patient access APIs
Solution:
Implemented FHIR layer on top of existing HL7 v2 infrastructure
Results:
Maintained 100% uptime of existing integrations
Reduced new integration time from 6 months to 2 months
Achieved regulatory compliance 18 months ahead of deadline
$2.3M cost avoidance over 3 years
Migration Approaches and Best Practices
For hands-on implementation, see our complete Mirth Connect guide and practical HL7v2-to-FHIR migration roadmap.
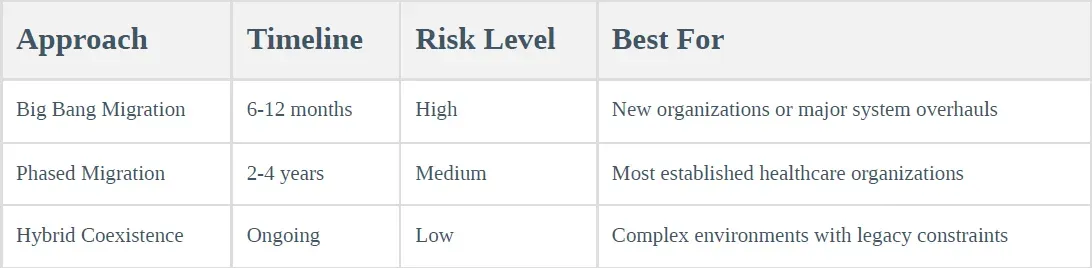
5.1 Migration Strategy Options
Healthcare organizations have three primary migration approaches, each with distinct risk-reward profiles:
5.2 Recommended Phased Approach
Phase 1 (Months 1-6): Foundation
- Implement FHIR infrastructure and basic Patient/Observation resources
- Establish a security framework and developer tools
- Train development teams on FHIR concepts and tools
Phase 2 (Months 7-18): Patient Access
- Deploy patient-facing FHIR APIs for regulatory compliance
- Implement mobile applications using FHIR resources
- Establish monitoring and analytics for FHIR usage
Phase 3 (Months 19-36): Internal Modernization
- Begin replacing selected HL7 v2 interfaces with FHIR APIs
- Implement real-time clinical decision support using FHIR
- Deploy population health analytics platforms
Phase 4 (Years 3-5): Optimization
- Complete migration of non-critical HL7 v2 interfaces
- Implement advanced FHIR capabilities (subscriptions, bulk data)
- Optimize performance and reduce technical debt
5.3 Critical Success Factors
Executive Leadership:
C-level sponsorship is essential for successful migration programs
Staff Training:
Budget 15-20% of project costs for comprehensive team training
Vendor Partnerships:
Ensure all major vendors have committed FHIR roadmaps
Data Governance:
Establish clear policies for data access and security across both standards
Future Roadmap and Strategic Recommendations
6.1 Industry Trends and Projections
Based on current adoption patterns and regulatory requirements, we project the following timeline for FHIR adoption:
- 2024 - 2025
Universal deployment of patient access FHIR APIs - 2026 - 2027
FHIR becomes the primary standard for new integrations - 2028 - 2030
HL7 v2 transitions to maintenance mode for legacy systems - 2030+
FHIR dominates new development, with HL7 v2 supporting critical legacy workflows
6.2 Strategic Technology Investments
Immediate Priorities (Next 12 Months):
- Deploy FHIR infrastructure for regulatory compliance
- Implement OAuth 2.0 security framework
- Establish API management and monitoring capabilities
- Begin staff training and capability development
Medium-Term Investments (1-3 Years):
- Implement translation layers for HL7 v2 to FHIR conversion
- Deploy patient-facing applications using FHIR
- Establish population health analytics platforms
- Begin selective migration of high-value HL7 v2 interfaces
6.3 Risk Mitigation Strategies
Healthcare organizations must address several key risks when implementing dual-standard strategies:
- Technical Complexity: Invest in robust testing and validation frameworks
- Staff Capability: Implement comprehensive training programs and external partnerships
- Vendor Dependencies: Establish clear FHIR requirements in all vendor contracts
- Security Concerns: Deploy zero-trust security models for API access
Implementation Framework
7.1 Governance Structure
Successful dual-standard implementations require dedicated governance with clear accountability:
- Executive Steering Committee: C-level oversight and strategic direction
- Technical Architecture Board: Standards compliance and technical decisions
- Clinical Advisory Group: Workflow impact assessment and user experience
- Security Council: Risk assessment and security framework oversight
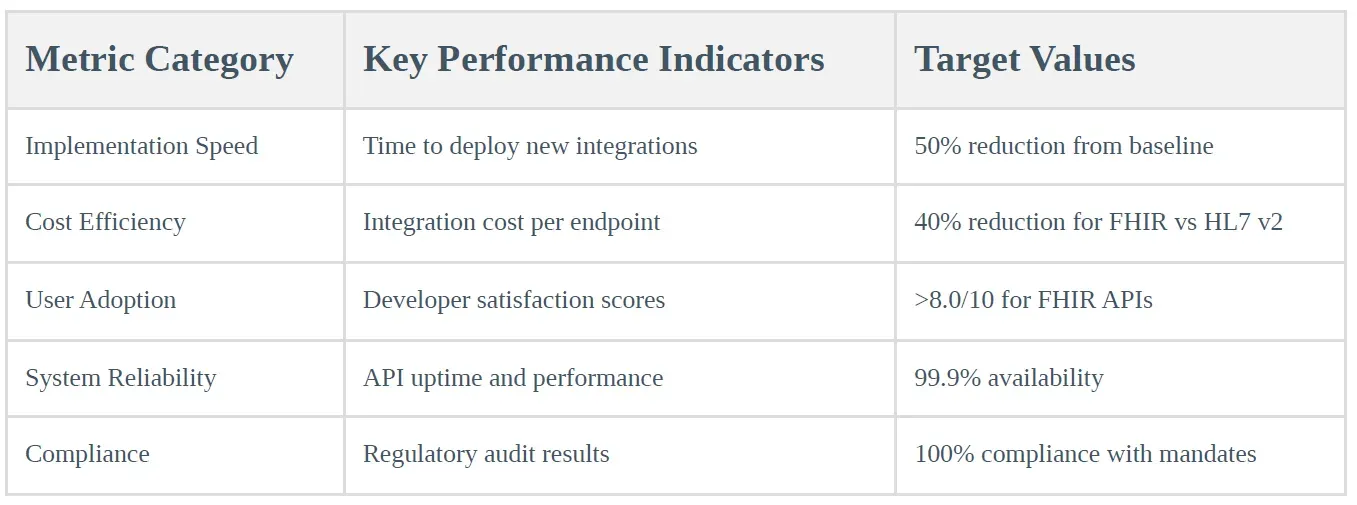
7.2 Performance Metrics and KPIs
7.3 Resource Planning
Typical resource requirements for hybrid HL7-FHIR implementations:
- Technical Staff: 2-3 FTE dedicated to FHIR development and maintenance
- Training Budget: $150K-$300K for comprehensive team education
- Infrastructure: $200K-$500K for API management and security platforms
- Vendor Support: 15-25% premium for dual-standard vendor support
Case Study: Academic Medical Center Transformation
Organization:
800-bed academic medical center with research requirements
Challenge:
Support clinical research while maintaining operational systems
Solution:
Implemented FHIR for research data access while maintaining HL7 v2for clinical operations
Results:
300% increase in research data accessibility
$1.8M in new research grants enabled by FHIR capabilities
Zero disruption to existing clinical workflows
65% reduction in time to provision research data access
Conclusion and Actionable Insights
The question facing healthcare IT leaders is not whether to choose HL7 or FHIR, but how to strategically implement both standards to maximize organizational capabilities and ROI. The evidence clearly demonstrates that hybrid approaches deliver superior outcomes compared to single-standard strategies.
8.1 Key Takeaways
- Coexistence is Strategic
Both standards serve distinct but complementary purposes in modern healthcare IT architectures - FHIR is Inevitable
Regulatory requirements and market demands make FHIR adoption mandatory, not optional - Migration is a Marathon
Successful transitions require 3-5 year timelines with phased implementation approaches - ROI is Demonstrable
Organizations report 18-24 month payback periods for well-executed hybrid strategies
8.2 Immediate Action Items
For Healthcare CIOs
- Conduct a comprehensive assessment of current HL7 v2 interfaces and their strategic value
- Establish FHIR implementation timeline aligned with regulatory deadlines
- Secure executive sponsorship and a dedicated budget for a dual-standard strategy
- Begin vendor discussions regarding FHIR roadmaps and support commitments
The healthcare industry stands at an inflection point where interoperability standards are converging toward web-native, patient-centric approaches. Organizations that embrace this transition through strategic dual-standard implementations will gain competitive advantages in patient engagement, operational efficiency, and clinical innovation.
Success requires thoughtful planning, adequate investment, and recognition that both HL7 and FHIR have roles to play in the future of healthcare data exchange. The organizations that thrive will be those that view this not as a migration challenge, but as a strategic opportunity to modernize their digital health capabilities while preserving the stability of their existing operations.
Frequently Asked Questions
1. How long should our migration from HL7 to FHIR take?
A complete migration from HL7 to FHIR should follow a 35 years phased approach, beginning with foundational infrastructure and security in the first six months, followed by rolling out patient-facing APIs for compliance within the next year. Internal modernization and selective HL7 interface replacement should occur over the next 18 - 24 months, with optimization and advanced FHIR capabilities completed in the final phase. This gradual strategy minimizes disruption, mitigates risk, and ensures seamless operational continuity while preparing for future scalability.
2. What are the risks of maintaining both standards?
Operating both HL7 and FHIR simultaneously introduces risks such as technical complexity, data mismatches, and increased security challenges. Translation layers between the two standards can lead to workflow inconsistencies if not carefully managed, while handling different security models - traditional HL7 protocols and FHIR's OAuth 2.0 - adds vulnerability points. Without strong governance and vendor alignment, organizations risk compliance issues, higher maintenance costs, and slower innovation.
3. Which middleware solutions best support hybrid environments?
The ideal middleware for a hybrid HL7-FHIR environment is a translation-centric integration layer that supports bidirectional data flow. It should feature robust HL7-to-FHIR conversion, an API gateway for unified access management, and a normalization layer to ensure data consistency. Advanced platforms also provide monitoring, analytics, and dual security support - FHIR's OAuth 2.0 and legacy HL7 protocols - enabling healthcare organizations to modernize systems without disrupting critical legacy workflows.
4. How will regulatory changes affect our hybrid approach?
Regulatory requirements are rapidly pushing healthcare organizations toward FHIR-first strategies, with mandates like the 21st Century Cures Act enforcing patient data access through standardized FHIR APIs. While HL7 remains vital for legacy workflows, regulatory deadlines will increasingly prioritize FHIR for all new integrations. A hybrid model provides a safe transition path, but it must be continuously updated to stay aligned with evolving compliance rules, avoiding last-minute overhauls and costly penalties.
Operating both HL7 and FHIR simultaneously introduces risks such as technical complexity, data mismatches, and increased security challenges. Translation layers between the two standards can lead to workflow inconsistencies if not carefully managed, while handling different security models - traditional HL7 protocols and FHIR's OAuth 2.0 - adds vulnerability points. Without strong governance and vendor alignment, organizations risk compliance issues, higher maintenance costs, and slower innovation.
The ideal middleware for a hybrid HL7-FHIR environment is a translation-centric integration layer that supports bidirectional data flow. It should feature robust HL7-to-FHIR conversion, an API gateway for unified access management, and a normalization layer to ensure data consistency.
Advanced platforms also provide monitoring, analytics, and dual security support - FHIR's OAuth 2.0 and legacy HL7 protocols - enabling healthcare organizations to modernize systems without disrupting critical legacy workflows.
Regulatory requirements are rapidly pushing healthcare organizations toward FHIR-first strategies, with mandates like the 21st Century Cures Act enforcing patient data access through standardized FHIR APIs.
While HL7 remains vital for legacy workflows, regulatory deadlines will increasingly prioritize FHIR for all new integrations.
A hybrid model provides a safe transition path, but it must be continuously updated to stay aligned with evolving compliance rules, avoiding last-minute overhauls and costly penalties.
Need expert help with healthcare data integration? Explore our Healthcare Interoperability Solutions to see how we connect systems seamlessly. Talk to our team to get started.