
A 600-bed multi-specialty hospital in Mumbai recently ran an internal audit on its biomedical inventory. The official register listed 4,200 active assets. The physical count returned 3,640. Two hundred and twenty pieces of equipment — ranging from infusion pumps to portable ultrasound carts — were untraceable. The replacement value alone was over ₹3.6 crore.
This is not an outlier. It is the default state of hospital asset management in 2026.
Most hospitals carry crores of rupees in medical equipment. But the system they use to manage it — spreadsheets, paper logs, ward-level WhatsApp groups, and the institutional memory of a few long-tenured biomedical engineers — was designed for a world that no longer exists. The result is a quiet, recurring drain on capital, compliance, and clinical efficiency that rarely makes it onto a board deck, but always shows up on the P&L.
This guide is for the hospital owner, CIO, COO, CFO, and biomedical head who already suspects this is a problem and wants the full picture: what hospital asset management really means in 2026, why the old methods are failing, what a modern system actually does, and how to evaluate the right one for your facility.
What Is Hospital Asset Management?
Hospital asset management — sometimes called medical equipment management — is the structured discipline of tracking, maintaining, and optimising every physical asset a hospital owns — from MRI machines and ventilators down to wheelchairs and infusion pumps — across its entire lifecycle, from procurement to decommissioning.
Done well, it answers four questions, on demand, for any asset:
- Where is it right now? Building, floor, ward, bay — and is it currently in use, available, or under maintenance?
- How healthy is it? When was it last serviced, when is it due, and what is its breakdown history?
- How well is it being used? Active hours per day, idle time, and utilisation by department.
- Is it compliant? Calibration records, traceability, NABH evidence — available on demand, not assembled in panic before an audit.
If a hospital cannot answer those four questions in under sixty seconds, the asset management system is not working — regardless of what the binder on the biomedical head's desk says.
Why Traditional Asset Management Is Failing Modern Hospitals
Hospitals have been managing assets for decades. Spreadsheets, paper registers, and barcode-based inventory systems still run a meaningful share of the country's tertiary care. So what changed?
Three things. The volume, velocity, and complexity of clinical operations.
1. Equipment density has multiplied. A 300-bed Indian hospital today operates between 3,500 and 6,000 individual assets across clinical and non-clinical categories. Manual reconciliation at that scale is not slow — it is mathematically impossible to keep current.
2. Equipment moves constantly. Infusion pumps, ECG machines, portable monitors, and ventilators are routinely shuttled between wards. The asset register is built on a snapshot. Real life is a stream.
3. Compliance is no longer optional. NABH accreditation and JCI standards demand demonstrable evidence — not just records, but traceable, time-stamped, technician-attributed evidence — for calibration, maintenance, and physical verification. Spreadsheets do not produce evidence chains.
The cost of this failure is rarely visible in any single line item. It is distributed across:
- Search time. Nursing studies in Indian tertiary hospitals show staff lose 20 to 40 minutes per shift looking for equipment that should be available.
- Capex inflation. Procurement teams routinely buy "shortage" equipment that already exists — idle — in another department. (See: why Indian hospitals lose crores every year to poor equipment tracking.)
- Unplanned downtime. Preventive maintenance schedules drift; breakdowns become the trigger for service rather than the exception.
- Audit risk. Every NABH cycle becomes a fire drill, with biomedical and compliance teams reconstructing records under pressure.
None of these costs hit a single budget line. All of them hit the bottom line.
The 5 Capabilities of a Modern Hospital Asset Management System
A modern hospital asset management system is not a digital register. It is an operational layer that sits across biomedical, operations, finance, and IT — and produces evidence continuously, not on demand. Five capabilities define it.

1. Real-Time Asset Tracking
Real-time tracking — also called RTLS (real-time location services) — means the system knows where every tagged asset is, right now, without anyone having to scan, log, or update it manually. Modern platforms combine three technologies to achieve this:
- QR codes — for low-cost, universal verification using any smartphone or tablet. Best for routine checks and low-movement assets.
- RFID — for bulk verification at checkpoints. Up to 5,000 assets verified in a single audit cycle without individual scanning. (Different RFID tag types — UHF vs HF vs BLE — suit different assets.)
- BLE (Bluetooth Low Energy) — for high-value, high-mobility assets that need always-on visibility. Active tags broadcast continuously; the system knows where every infusion pump is, in real time, without anyone scanning anything.
For sterilisation environments, where adhesive QR labels degrade or fall off entirely, modern platforms support laser-etched permanent identification — the asset ID is engraved directly onto the equipment surface. No re-tagging, no degradation, no compliance gap. (Deep dive: types of asset labels and stickers for hospital equipment and the top 10 medical asset labels of 2026.)
2. Automated Breakdown & Maintenance Ticketing
The traditional breakdown workflow in most Indian hospitals looks like this: a nurse spots a fault, walks down to the biomedical office, finds someone, explains the problem verbally, and hopes for follow-up. The breakdown enters an informal queue with no timestamp, no SLA, and no audit trail.
A modern system replaces this with a structured workflow. A breakdown is reported through the app — or detected automatically via system alerts. A ticket is instantly created, timestamped, and assigned to the responsible team. Every action is logged. Resolution time is tracked. Repeat failures on the same asset are automatically flagged. The complete service history is attached to the asset record forever.
The shift is operational, not just digital. Maintenance becomes a discipline that is measured, not a crisis that is responded to.
3. Preventive Maintenance Scheduling
Preventive maintenance schedules exist in almost every hospital. The problem is execution. Reminders are missed. Technicians are busy. The schedule drifts. The next breakdown becomes the trigger.
A modern asset management system makes the PM system-driven, not human-memory-driven:
- Maintenance intervals are configured once per asset type — based on calendar, usage hours, or last service date.
- Tasks are auto-assigned to specific technicians before the due date.
- Completion is logged only when the responsible person actively closes the task — verbal confirmation does not count.
- The system computes a PM compliance rate — a single metric that tells management exactly how disciplined maintenance is, this month versus last.
4. Utilisation Tracking & ROI Visibility
This is where most hospitals discover their highest hidden cost. A typical utilisation profile across Indian tertiary care looks like this:
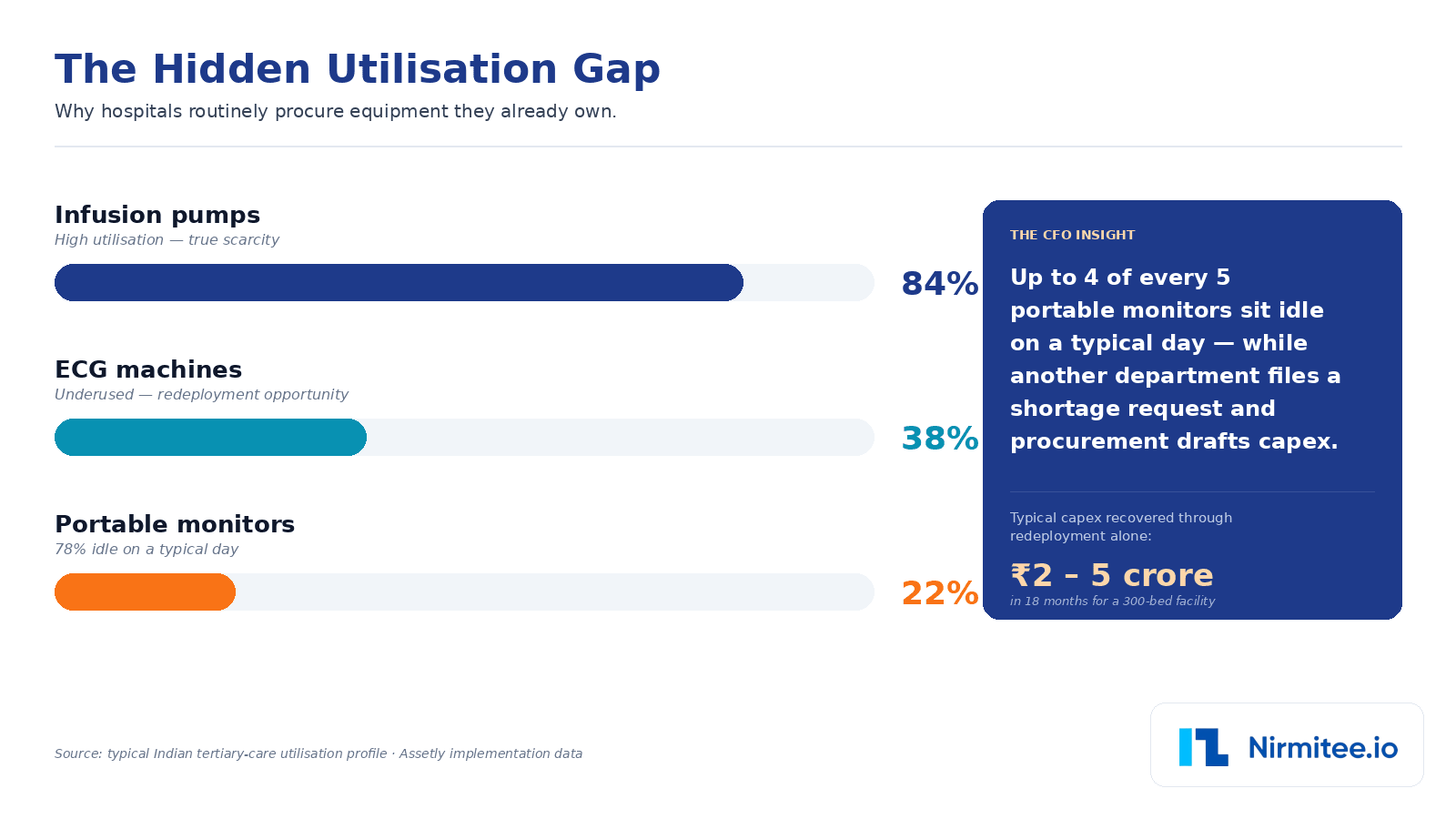
The 22% figure is the one that should make a CFO sit up. It means roughly four out of every five portable monitors a hospital owns are sitting idle on any given day, while another department is filing a shortage request and procurement is drafting a capex proposal.
A modern system quantifies this for every tracked asset: active hours per day, idle time, department-level comparison, and redeployment alerts when one ward is chronically idle while another requests more. For a hospital with ₹50 crore of medical equipment, redeployment alone typically recovers ₹2-5 crore of effective capex in the first eighteen months.
5. Audit-Ready NABH Compliance
NABH accreditation — alongside CDSCO and bio-medical waste rules in India — requires hospitals to demonstrate systematic asset management — calibration records tied to each asset, maintenance logs without gaps, physical verification, and utilisation documentation. In most hospitals, this is assembled in the four weeks before an audit, by people who have day jobs.
A modern asset management platform produces compliance evidence as a by-product of daily operation. Calibration is logged when it happens. Maintenance is logged when it is performed. Physical verification — using QR or RFID — completes hundreds or thousands of asset checks in a single day, not three weeks.
The shift is structural: the hospital is audit-ready on day one, and every day after.
Choosing the Right Tracking Technology: QR vs RFID vs BLE
One of the most common questions hospital leaders ask is which tracking technology to deploy. The honest answer is that the right answer is usually all three, applied selectively. Each has a clear sweet spot.

- Use QR codes for the broad base of assets that need routine, periodic verification — chairs, beds, non-critical equipment, consumables. Zero hardware dependency. Any smartphone is a reader.
- Use RFID in high-volume zones — central stores, sterilisation supply, emergency department — where bulk verification matters more than per-asset visibility. A single RFID checkpoint can read thousands of tags in minutes. (Hardware deep dive: RFID readers and antenna placement.)
- Use BLE for high-value, high-mobility assets — infusion pumps, portable ventilators, ultrasound carts, telemetry units — where the cost of "where is it?" is measured in clinical delay, not just inconvenience.
The wrong question is "QR or RFID or BLE?" The right question is "which assets justify which technology?" — and a good asset management platform supports all three on the same backbone, with the same dashboard.
The Hidden Cost of Not Doing This
It is easy to defer an asset management upgrade. There is no fire. The hospital is not failing. Patients are being treated. So leadership keeps the project on the "next quarter" list — for several years running.
The deferred cost compounds quietly. For a typical 300-bed hospital, the conservative annual cost of not having modern asset management looks like this:
- ₹40-60 lakh in equipment loss, theft, and untraceable write-offs. (How hospitals recover 30%+ of equipment ROI with real-time tracking.)
- ₹1-2 crore in avoidable capex — equipment purchased to plug a "shortage" that was actually a redeployment problem.
- ₹30-50 lakh in unplanned downtime — lost OT slots, deferred procedures, locum technician costs.
- 15-25% additional staff time spent on search, manual logging, and audit reconstruction.
None of this hits the books as "asset management failure." It hits the books as procurement, depreciation, overtime, and vendor service charges. Which is exactly why it persists.
Implementation: What a Real Rollout Looks Like
The single biggest objection to deploying a hospital asset management platform is the implementation burden — the fear that the biomedical and operations teams will be tied up for months collecting data, tagging assets, and reconciling records.
A well-run implementation removes that burden. Here is what a modern, end-to-end rollout looks like — including how Assetly delivers it:

- Asset Data Collection. A vendor team walks the facility and captures every medical and non-medical asset — manufacturer, model, serial number, location, department, condition. The hospital's internal team stays focused on clinical operations.
- Data Cleaning & Standardisation. Raw data is de-duplicated, normalised, and structured. Naming conventions are standardised across departments. The asset register becomes a single source of truth, not five overlapping ones.
- System Configuration. The platform is configured to the hospital's actual structure — departments, asset categories, maintenance intervals, escalation rules, user roles, and reporting hierarchies.
- QR Generation & Physical Tagging. Unique QR codes are generated and physically affixed by the implementation team. Sterilisation-zone equipment is laser-marked. Every asset leaves this phase with a permanent, scannable identity.
- Training & Go-Live Support. Biomedical, operations, and IT teams are trained. The vendor team is on-site for the first days of live operation to handle teething issues directly.
From go-live, the hospital's internal team is responsible only for day-to-day usage — scanning, logging, and operating. No technical overhead. No ongoing data management burden. (For phased rollouts in large facilities: how to implement RFID asset tracking in a large hospital without disrupting operations.)
What Changes for Each Team — A Before-and-After Snapshot
The clearest way to evaluate any asset management platform is to ask what changes for each function, the day after go-live.
- Biomedical team: From maintenance logs in spreadsheets and breakdowns discovered late — to auto-ticketing, scheduled PM, and complete service history per asset. (How hospitals give biomedical teams back 30% of their day.)
- Operations: From shift time built around equipment search — to real-time location on a live floor map, with duplicate requests flagged instantly.
- Finance / CFO: From capex decisions based on verbal shortage reports — to utilisation-backed redeployment recommendations before any procurement.
- CIO / IT: From multiple disconnected registers and integration gaps — to a single configurable platform with clean data flowing in.
- Owners / Auditors: From NABH prep as a quarterly crisis — to compliance evidence built daily, with 500-5,000 assets verifiable in a single day.
A Real-World Snapshot: What Visibility Actually Buys
Consider a 450-bed multi-specialty hospital in Pune that deployed a modern asset management platform across three phases over six months. Within the first quarter post go-live:
- The hospital identified 47 portable monitors and 23 ECG machines that had been duplicated across departments, paused a ₹1.8 crore procurement order that was already approved.
- Average time to locate a high-mobility asset dropped from ~12 minutes to under 30 seconds.
- Preventive maintenance compliance rose from 58% to 91% within four months.
- NABH re-accreditation evidence was assembled in three working days — down from the previous cycle's six weeks.
The hospital did not become more efficient because someone worked harder. It became more efficient because the visibility existed for the first time.
How to Evaluate a Hospital Asset Management Platform
If you are evaluating vendors, the right questions are not the ones in the typical RFP. Use these instead — and pair them with our full vendor evaluation framework for Indian hospitals:
- Does the platform support QR, RFID, and BLE on the same backbone — or only one?
- Does it handle laser-etched identification for sterilisation zones?
- Is the preventive maintenance system-driven, with a measurable PM compliance metric?
- Does it produce NABH-aligned evidence as a by-product of operation, not as a separate report?
- Does the vendor handle Phase 1 to Phase 5 of implementation — or do they hand the hospital a login and a manual?
- Can the platform integrate with existing HIS, ERP, and procurement systems — or is it a silo?
- What is the dashboard utilisation report a CFO will actually use, monthly?
If a vendor cannot answer those seven questions clearly in a 60-minute discovery call, the platform is not ready for your hospital — regardless of feature lists.
Key Takeaways
- Hospital asset management in 2026 is no longer a register problem — it is an operational layer that drives capex efficiency, maintenance discipline, and audit readiness.
- Spreadsheets and paper registers fail at modern equipment density, mobility, and compliance demands. The cost is hidden in procurement, downtime, and audit prep — not in any single budget line.
- A modern system delivers five capabilities together: real-time tracking, automated ticketing, scheduled PM, utilisation visibility, and continuous NABH-ready compliance.
- The right tracking technology is not QR or RFID or BLE — it is all three, applied selectively to the right asset class.
- The biggest ROI line is rarely the obvious one. It is the redeployment of idle equipment that prevents the next round of unnecessary capex.
Ready to See What Visibility Looks Like in Your Hospital?
Assetly is a hospital asset management platform purpose-built for the operational reality of Indian tertiary care — with QR, RFID, BLE, and laser-marked tracking on a single backbone, NABH-aligned compliance built in, and end-to-end implementation handled by our team.
Hospitals deploying Assetly typically see ₹35–80 lakh in Year 1 savings, 340% three-year ROI, and 99.2% tracking accuracy — with a typical 3-4 month payback. A 250-bed multi-specialty hospital we work with saved ₹42 lakh in Year 1; a 120-bed specialty hospital saved ₹28 lakh in 8 months and cut NABH audit prep from 4 weeks to 4 days. If you are responsible for the next NABH cycle, the next capex review, or the next biomedical audit, the conversation starts with a single discovery call. We will assess your hospital's current asset management state and return a customised implementation plan.
