Healthcare's Data Problem Has a Modern Solution
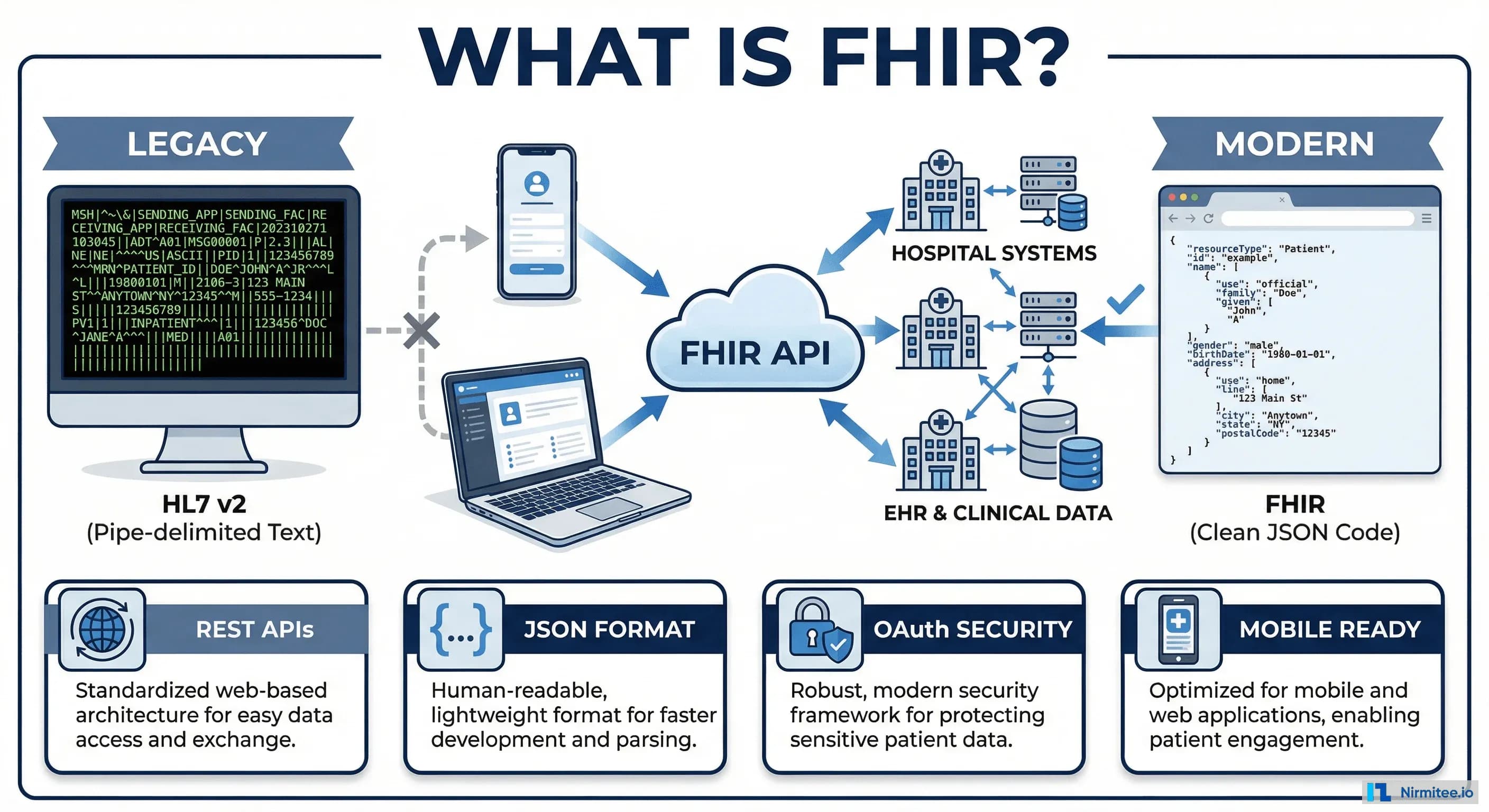
For decades, healthcare systems have communicated using HL7 v2 — a standard designed in the 1980s when fax machines were cutting-edge technology. It works, but it was built for a world of on-premise servers and batch processing. It knows nothing about mobile apps, cloud computing, real-time APIs, or patients who want their health data on their phones.
FHIR changes everything. It's the modern standard that brings healthcare data exchange into the 21st century — and if you're a healthcare leader, product manager, or technology decision-maker, understanding FHIR is no longer optional. CMS mandates it. Patients expect it. Your competitors are already building on it.
What is FHIR? The Simple Explanation
FHIR (Fast Healthcare Interoperability Resources) is a healthcare data standard created by HL7 International that allows healthcare systems to exchange data using the same web technologies that power Google, Amazon, and every modern application you use daily.
Where HL7 v2 uses cryptic pipe-delimited text transmitted over specialized protocols, FHIR uses JSON (the universal data format of the web) transmitted over REST APIs (the same technology every web developer already knows). This single architectural choice is why FHIR has been adopted faster than any previous healthcare standard.
The four pillars that make FHIR different:
- REST APIs — Standard HTTP methods (GET, POST, PUT, DELETE) that any web developer can use. No specialized healthcare protocols required.
- JSON/XML — Human-readable data formats with rich tooling support across every programming language.
- OAuth 2.0 Security — The same security model used by Google, Facebook, and every major web platform. Built-in authorization and consent.
- Mobile-First Design — Designed from the ground up for mobile apps, patient portals, and cloud-native applications.
FHIR Resources: The Building Blocks
FHIR organizes all healthcare data into Resources — self-contained, well-defined data objects that represent real clinical and administrative concepts. Think of Resources as the "nouns" of healthcare — Patient, Encounter, Observation, Medication, Claim.
FHIR R4 defines over 150 resource types organized into categories:
- Foundation — The basics: Patient, Practitioner, Organization, Location. Every FHIR implementation starts here.
- Clinical — The clinical record: Condition (diagnoses), Observation (lab results, vitals), Procedure, DiagnosticReport, AllergyIntolerance.
- Financial — Revenue and coverage: Claim, Coverage, ExplanationOfBenefit, Account. Critical for payer integrations.
- Workflow — Operations: Encounter (visits), Appointment, ServiceRequest (orders), Task. The verbs of clinical workflow.
- Medications — The full medication lifecycle: Medication, MedicationRequest, MedicationDispense, Immunization.
You don't need all 150 resources. Most implementations start with 5-10 core resources and expand from there based on use cases.
How the FHIR API Works
If you've ever used a web API — or even if you haven't — FHIR's RESTful API is remarkably straightforward. Every resource type has a predictable URL pattern, and standard HTTP methods perform standard operations.
The core operations:
- READ —
GET /Patient/123— Retrieve a specific patient by ID. - SEARCH —
GET /Patient?name=Smith&birthdate=1980-01-01— Find patients matching criteria. - CREATE —
POST /Patient— Register a new patient record. - UPDATE —
PUT /Patient/123— Update an existing patient's information. - DELETE —
DELETE /Patient/123— Remove a patient record. - HISTORY —
GET /Patient/123/_history— View all previous versions of a record.
FHIR's search capabilities are particularly powerful. You can search across resources, include related data in a single request (using _include and _revinclude), paginate results, and filter by virtually any field. This eliminates the multiple round-trips that plague older integration approaches.
SMART on FHIR: The App Platform for Healthcare
SMART on FHIR (Substitutable Medical Applications, Reusable Technologies) is a framework that turns FHIR into an app platform — allowing third-party applications to launch securely within EHR systems, access patient data with proper authorization, and provide functionality that the EHR doesn't offer natively.
Think of it like the App Store for healthcare. Just as you install apps on your iPhone that extend its functionality, SMART on FHIR allows clinicians to launch specialized apps directly within their EHR workflow — clinical calculators, risk assessment tools, genomics viewers, care planning assistants — all with secure access to the patient's data.
The SMART launch sequence uses OAuth 2.0 with healthcare-specific extensions:
- Clinician clicks "Launch App" in their EHR
- EHR sends patient context (who is selected) to the app
- App requests specific data permissions (scopes) from the authorization server
- User consents to the access
- App receives a secure token
- App uses the token to call FHIR APIs and display relevant data
Epic, Cerner, and all major EHR vendors support SMART on FHIR app launches. There are now over 4,200 apps available through SMART on FHIR app galleries.
FHIR Use Cases: Who Benefits and How
FHIR serves three primary stakeholder groups, each with distinct use cases that are driving adoption.
For Providers (Hospitals, Health Systems, Clinics)
FHIR enables clinical decision support apps that analyze patient data in real-time, care coordination across facilities, standardized quality reporting to CMS and payers, and seamless referral management between specialists. The biggest win: reducing the manual chart review and phone calls that consume clinical staff time.
For Payers (Insurance Companies, Medicare/Medicaid)
CMS mandates require payers to provide Patient Access APIs using FHIR, enabling members to download their claims and clinical data. FHIR also powers electronic prior authorization (cutting response times from days to minutes), provider directory APIs, and payer-to-payer data exchange when members switch insurers.
For Patients
FHIR puts patients in control of their health data. Apple Health and Google Health Connect use FHIR to pull medical records from hospital patient portals directly to smartphones. Patients can share records with new providers, check insurance coverage, book appointments, and request prescription refills — all through FHIR-powered apps.
FHIR Adoption: Where the Market Stands in 2026
FHIR adoption has reached a tipping point. The numbers tell the story:
- 96% of US hospitals now have FHIR-enabled EHR systems (up from 78% in 2023)
- FHIR API call volume has grown 380% between 2022 and 2025
- The healthcare interoperability market is projected to reach $85 billion by 2030
- CMS has mandated FHIR APIs for all Medicare and Medicaid participating payers
- FHIR R4 achieved normative (stable) status in 2019, meaning it's production-ready with backward compatibility guarantees
The bottom line: FHIR is no longer emerging technology. It's the standard. Organizations that haven't started their FHIR journey are falling behind.
Inside a FHIR Resource: Patient Record Decoded
To make FHIR tangible, let's look inside the most fundamental resource — the Patient resource. Understanding its structure helps you scope implementations and evaluate vendor capabilities.
Key field groups in a FHIR Patient resource:
- Identifiers — Medical Record Number (MRN), SSN, insurance member ID. A patient can have multiple identifiers from different systems.
- Demographics — Name (with family/given structure for international support), gender, birthDate, marital status.
- Contact — Phone, email, address with structured components (line, city, state, postal code, country).
- Communication — Preferred language for patient-facing communications.
- Emergency Contact — Relationship, name, and phone number for the patient's designated contact.
Every field follows a precisely defined structure with required data types, so there's no ambiguity about how to populate or read the data. This is one of FHIR's biggest advantages over HL7 v2, where field definitions were loose enough to allow incompatible implementations.
FHIR Implementation Roadmap
Implementing FHIR doesn't have to be overwhelming. The most successful organizations follow a phased approach that delivers value early and expands incrementally. For organizations with existing legacy systems, a FHIR Facade architecture is often the fastest path to exposing FHIR APIs without replacing core infrastructure.
Phase 1 — Assessment (2-4 weeks): Identify your highest-priority use cases. Map your existing data to FHIR resources. Choose a FHIR server (HAPI FHIR for open-source, or vendor-provided). Evaluate your EHR vendor's FHIR readiness.
Phase 2 — Pilot (4-6 weeks): Implement core resources (Patient, Encounter). Build read-only APIs first. Connect to your EHR vendor's test sandbox. Validate conformance using tools like Touchstone or Inferno.
Phase 3 — Production (6-8 weeks): Add remaining resources for your use cases. Implement write operations (create, update). Complete security audit and penetration testing. Load test at peak volumes.
Phase 4 — Scale (Ongoing): Add new integrations and partner connections. Monitor API performance and usage patterns. Plan upgrades to newer FHIR versions. Expand to cross-organizational exchange.
Total time to production: 12-18 weeks for a focused implementation. This is dramatically faster than traditional HL7 v2 integration projects because FHIR leverages existing web development tools, skills, and infrastructure.
What Should You Do Next?
FHIR is the future of healthcare data exchange — and increasingly, the present. Here's your action plan:
- Assess your EHR vendor's FHIR capabilities. Ask specifically about FHIR R4 support, SMART on FHIR app launch, and bulk data export.
- Identify your first FHIR use case. Patient access APIs (for CMS compliance) and clinical data exchange are the most common starting points.
- Understand your compliance obligations. If you participate in Medicare/Medicaid, FHIR APIs are mandatory — not optional.
- Build or partner. If you have web development talent, FHIR's learning curve is manageable. If not, partner with a team that has healthcare interoperability expertise.
For the foundational context on healthcare messaging standards, read our companion guide: What is HL7? The Complete Guide to Healthcare Data Exchange Standards. For practical integration guidance, see HL7 Integration: How It Works, Key Message Types, and Implementation Playbook.
Need help with FHIR implementation? Our healthcare integration team has helped organizations across the US build production FHIR APIs, achieve CMS compliance, and scale interoperable systems.