Remote Patient Monitoring for Heart Failure: Connected Devices, Clinical Alerts, and 39% Readmission Reduction
Executive Summary
A cardiology practice managing 500 heart failure patients faced a recurring crisis: 18% 30-day readmission rate. Patients were discharged from the hospital, sent home with instructions, and not seen again until their next appointment in 4-6 weeks — or until they showed up in the ER with decompensated heart failure. The gap between discharge and follow-up was a clinical blind spot where patients deteriorated silently.
We built a comprehensive Remote Patient Monitoring (RPM) platform — Bluetooth-connected devices (BP monitor, smart scale, pulse oximeter), a patient mobile app with daily vitals logging, a provider dashboard with real-time alerts and risk stratification, ML-powered deterioration detection, and integrated RPM billing (CPT 99453/99454/99457/99458).
Results: 30-day readmission rate dropped from 18% to 11% (39% reduction), the practice generated $44,500/month in RPM reimbursement, and an estimated $1.2M/year in avoided readmission costs for the health system.

The Problem: The Discharge-to-Follow-Up Blind Spot
- 18% readmission rate: nearly 1 in 5 heart failure patients readmitted within 30 days — costing $12,000+ per readmission and triggering CMS penalties
- No data between visits: patients went 4-6 weeks without any clinical monitoring. Weight gain (fluid retention), BP spikes, and O2 drops happened at home with nobody watching.
- Reactive care model: by the time patients felt sick enough to call or visit the ER, they were already in acute decompensation — requiring hospitalization that could have been prevented with earlier intervention
- Patient non-compliance invisible: were patients taking their diuretics? Following their sodium restriction? Nobody knew until the next office visit when damage was already done.
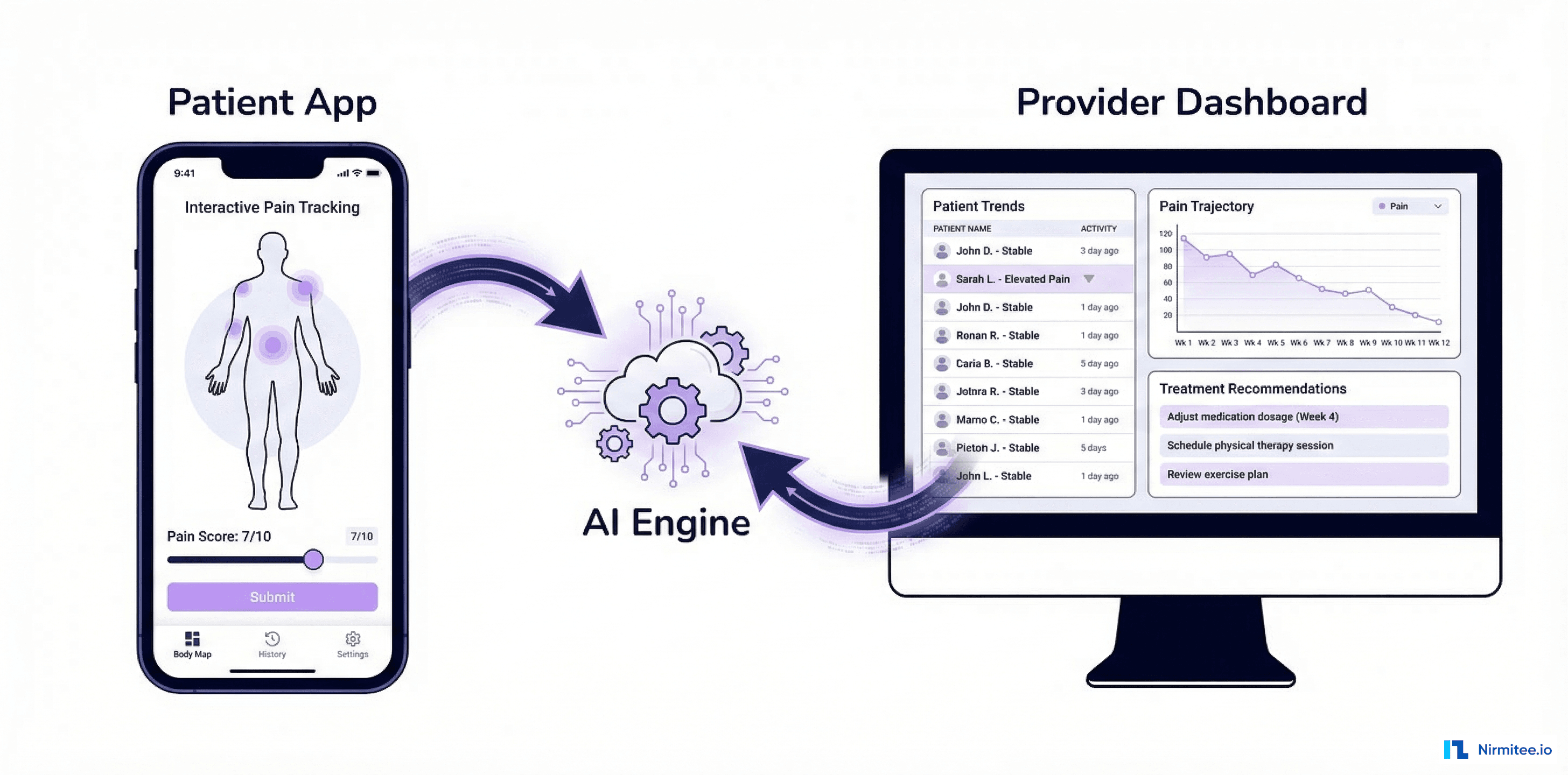
Provider Dashboard

The provider dashboard shows all 500 RPM patients risk-stratified: critical (red), high (orange), moderate (yellow), stable (green). Clicking any patient shows 30-day trending charts for BP, weight, O2, and heart rate. Alert banners highlight clinical concerns: "Weight gain 4 lbs in 3 days — possible fluid retention." Threshold configuration allows per-patient customization.
Patient Mobile App

The patient app guides daily health monitoring with a friendly checklist: take BP reading, log weight, take medications, record symptoms. Vital signs cards show current readings with normal/warning/critical color coding. Secure messaging connects patients directly to their care team.
Architecture
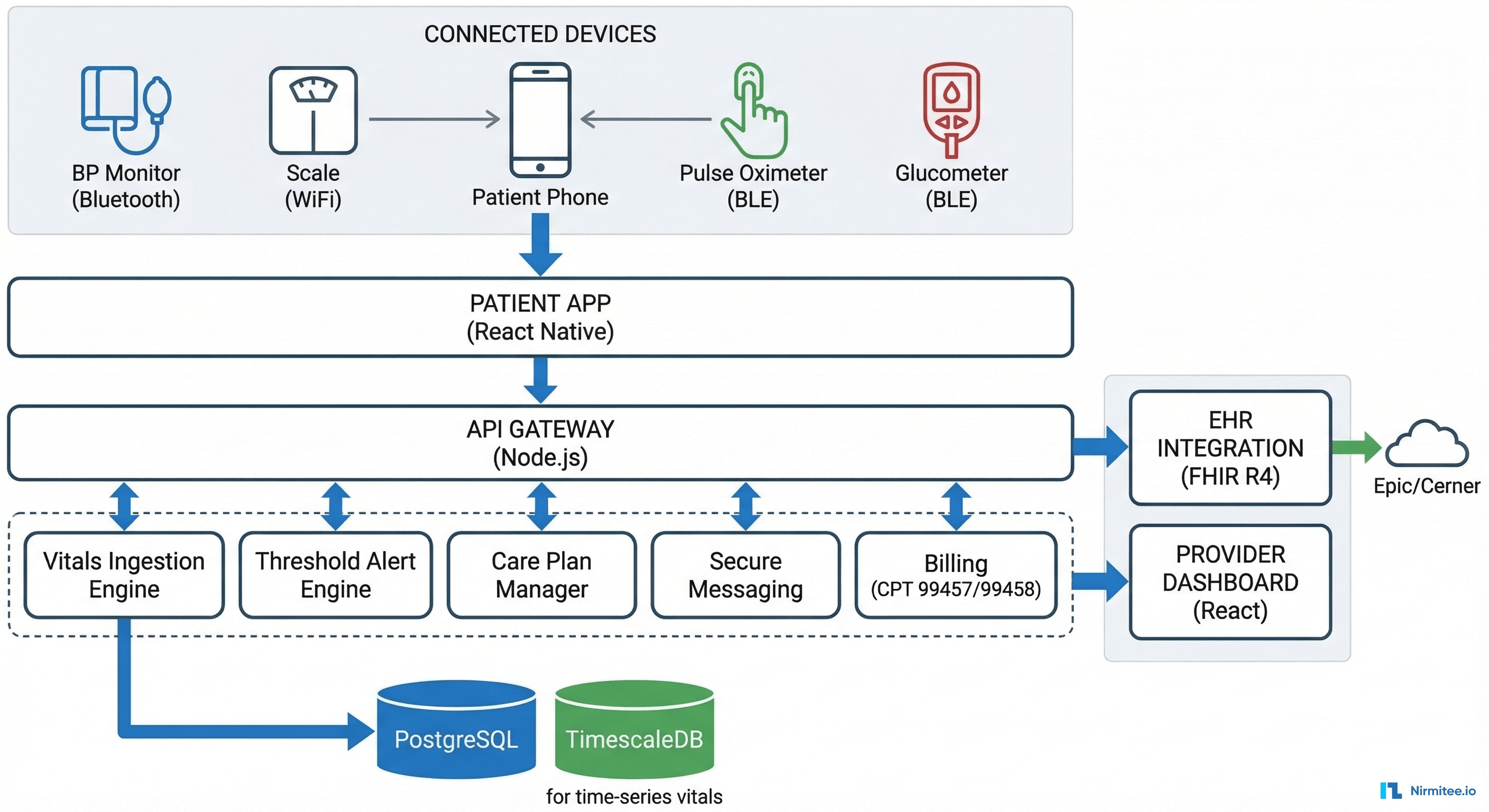
Technology Stack
| Component | Technology | Purpose |
|---|---|---|
| Patient App | React Native + BLE | Device pairing, vitals sync, daily tasks, messaging |
| Provider Dashboard | React + D3.js | Patient monitoring, alerts, trending, population view |
| Backend | Node.js (Express) | API gateway, alert engine, care plan management |
| Vitals DB | TimescaleDB | Time-series vital signs storage and querying |
| Clinical DB | PostgreSQL | Patient profiles, care plans, alert rules, billing |
| Device Integration | Bluetooth LE + WiFi | BP monitors, scales, pulse oximeters, glucometers |
| Alert Engine | Node.js + Redis | Real-time threshold monitoring, escalation rules |
| EHR Integration | FHIR R4 (Epic, Cerner) | Push vitals to patient chart, pull medications/conditions |
| Billing | Custom + clearinghouse | CPT 99453/99454/99457/99458 tracking and claims |
Clinical Alert Management
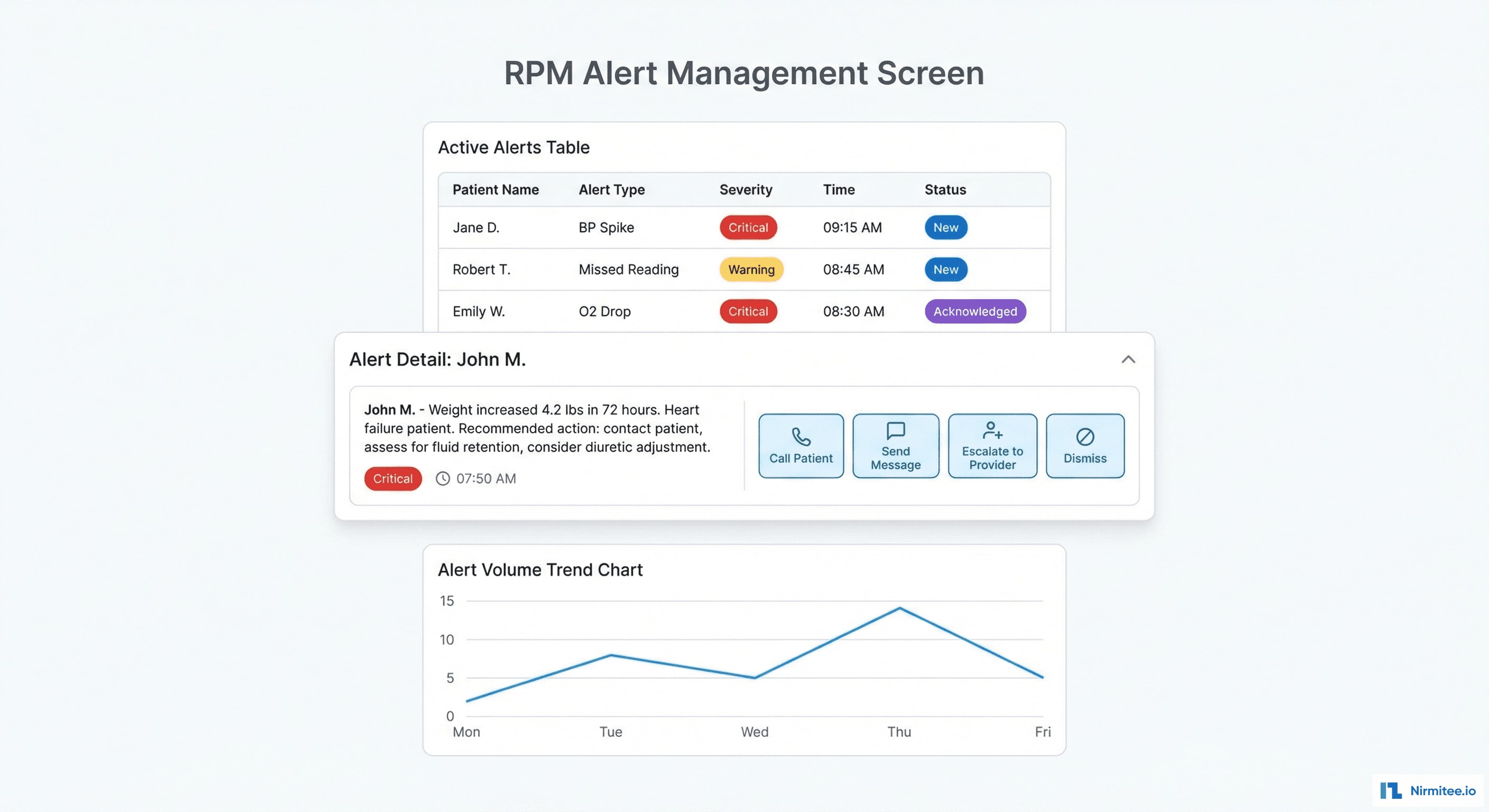
The alert engine monitors every vital sign against patient-specific thresholds:
- Weight gain >3 lbs in 72 hours: heart failure fluid retention alert → call patient, assess symptoms, consider diuretic adjustment
- BP >160/100 on 2 consecutive readings: hypertensive urgency → medication review, same-day telehealth
- O2 <92% sustained: hypoxemia alert → immediate phone assessment, possible ER referral
- Missed readings >48 hours: non-compliance alert → outreach to re-engage patient
Device Onboarding
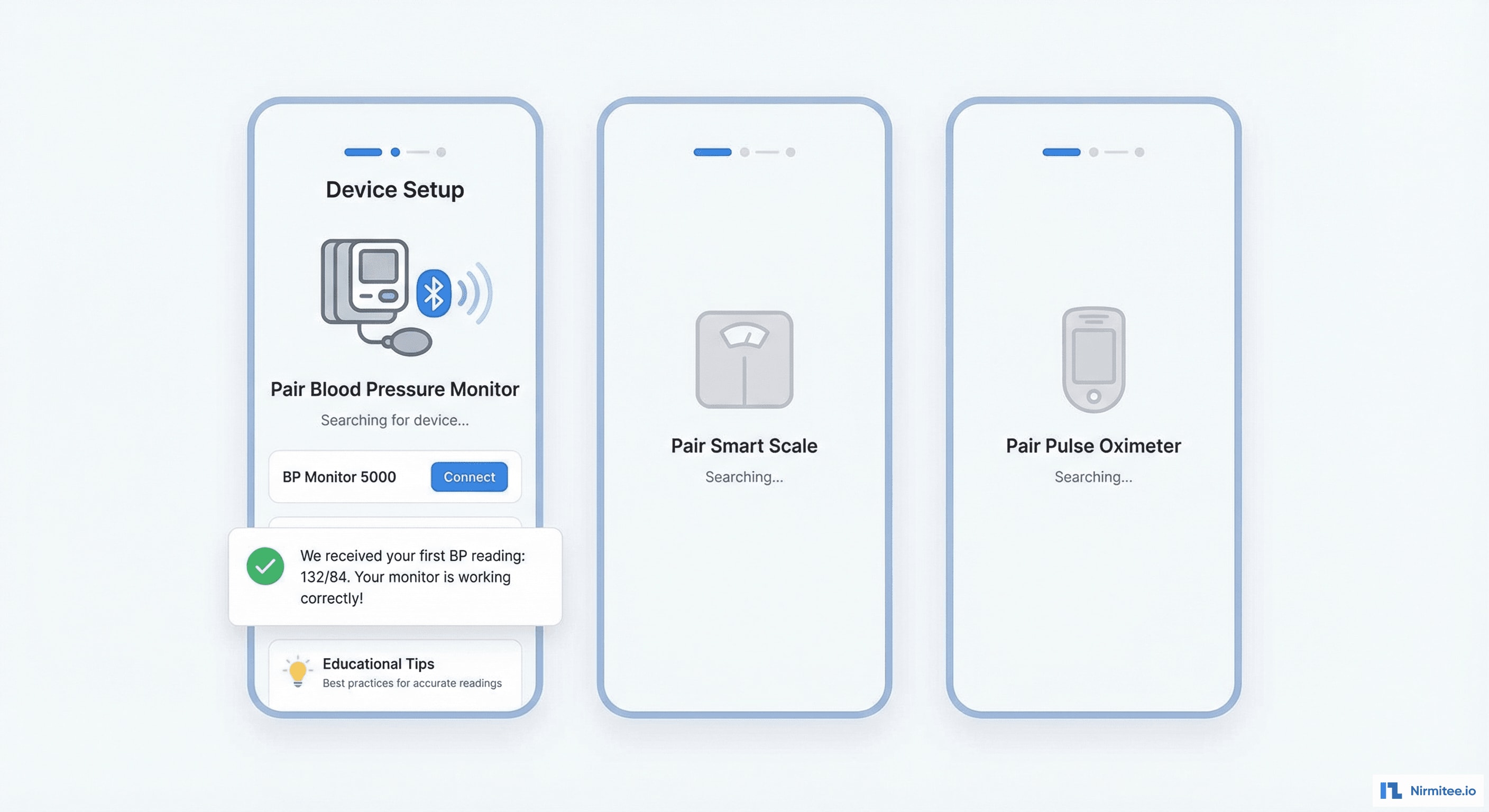
Patient-friendly device setup wizard: scan → pair → test reading → confirm. Under 5 minutes per device. Supports major RPM-certified devices from Omron, Withings, Masimo, and iHealth.
Population Health Overview
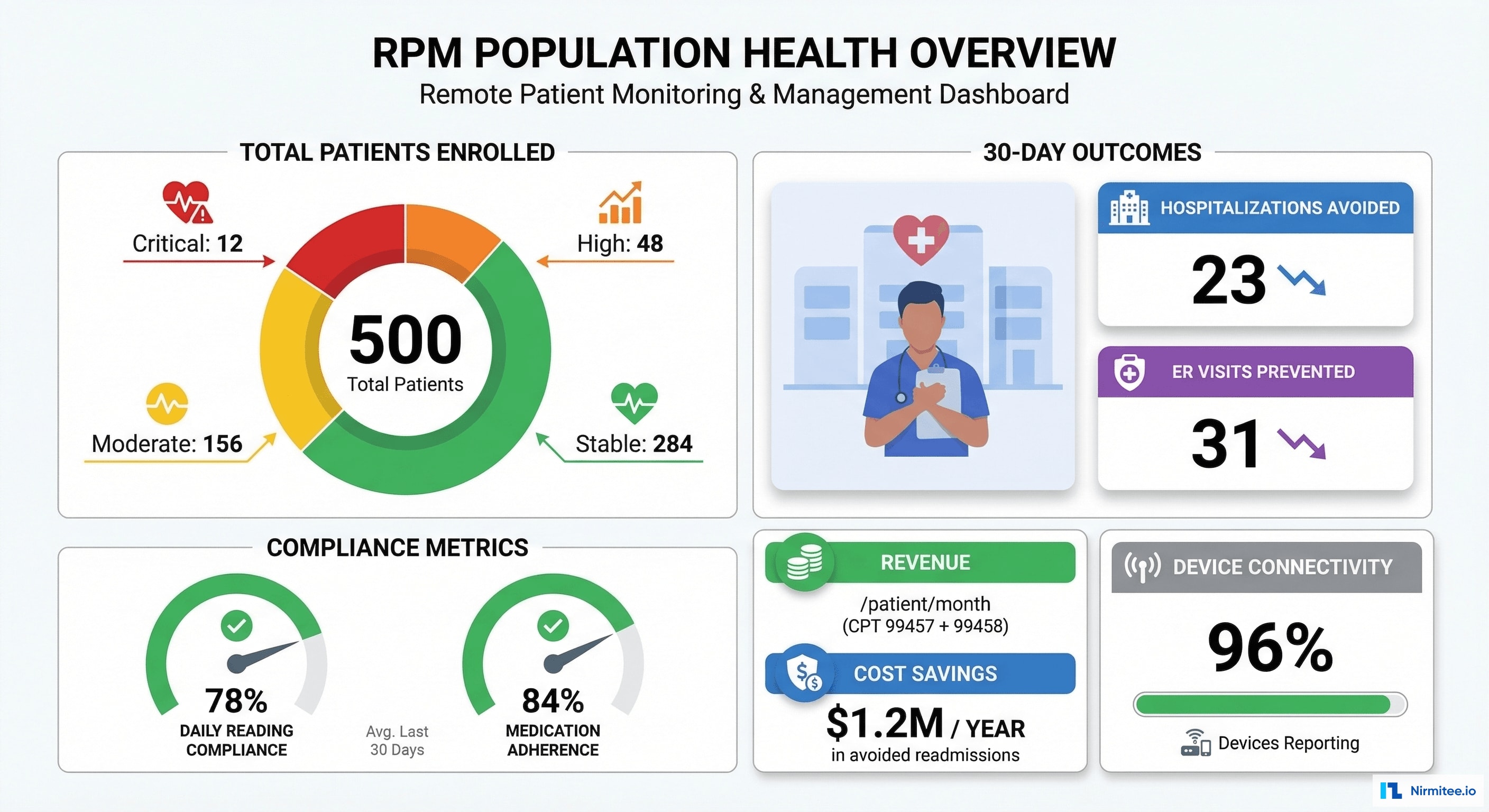
Practice-wide RPM metrics: 500 patients enrolled, risk tier distribution, 30-day outcomes (23 hospitalizations avoided, 31 ER visits prevented), compliance rates, revenue tracking, and device connectivity status.
RPM Billing
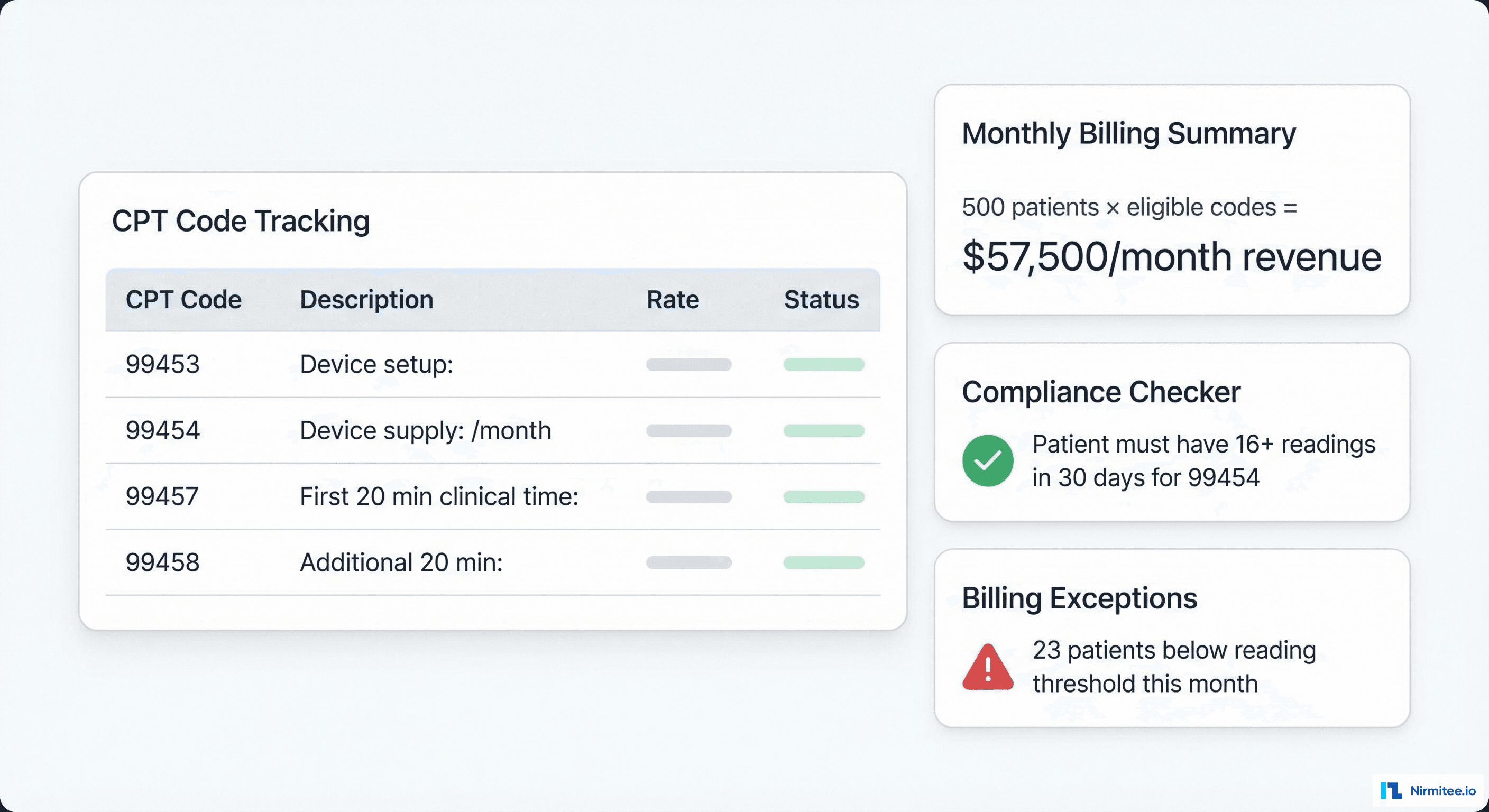

RPM is one of the few areas where CMS explicitly reimburses for remote monitoring. The billing module tracks eligibility for each CPT code:
| CPT Code | Description | Rate | Requirement |
|---|---|---|---|
| 99453 | Initial device setup + education | $21 | One-time per patient |
| 99454 | Device supply + data transmission | $55/month | 16+ readings in 30 days |
| 99457 | Clinical staff time (first 20 min) | $52/month | 20+ min of monitoring/month |
| 99458 | Additional 20 min clinical time | $42/month | Additional 20 min increments |
The platform auto-tracks reading counts and clinical time to ensure billing compliance. $44,500/month in RPM revenue for 500 patients.
Results

| Metric | Before RPM | After RPM | Impact |
|---|---|---|---|
| 30-day readmission rate | 18% | 11% | 39% reduction |
| ER visits (heart failure) | 4.2/patient/year | 2.1/patient/year | 50% reduction |
| Data points between visits | 0 | ~90/patient/month | Continuous monitoring |
| Daily reading compliance | N/A | 78% | Strong patient engagement |
| Time to clinical intervention | Days to weeks (next visit) | Hours (alert-driven) | Same-day response |
| RPM revenue | $0 | $44,500/month | $534K/year new revenue |
| Avoided readmission costs | N/A | $1.2M/year | System-level savings |
| Patient satisfaction | 3.6/5 | 4.5/5 | 25% improvement |
Timeline
| Phase | Duration | Deliverables |
|---|---|---|
| Phase 1 | 5 weeks | Device integration (BLE), patient app, vitals ingestion, TimescaleDB setup |
| Phase 2 | 5 weeks | Provider dashboard, alert engine, threshold configuration, EHR integration (FHIR) |
| Phase 3 | 4 weeks | Population health view, RPM billing module, secure messaging, care plan manager |
| Phase 4 | 3 weeks | Device onboarding for 100 pilot patients, staff training, billing validation, go-live |
Total: 4.25 months with 3 engineers + 1 clinical project manager.
Lessons Learned
- Weight is the #1 vital sign for heart failure RPM. Weight gain is the earliest detectable sign of fluid retention — 2-3 days before symptoms appear. The smart scale was the single most clinically valuable device in the RPM kit.
- 16 readings/month is the billing threshold — but clinical value needs daily. CMS requires 16+ readings for CPT 99454 reimbursement. But clinical benefit requires near-daily monitoring. We designed the app to encourage daily readings (gamified streak), ensuring both billing and clinical needs are met.
- Alerts must be actionable, not just informational. "BP elevated" is noise. "BP 168/98 on 2 consecutive readings for John M., heart failure patient on lisinopril 20mg — consider increasing to 40mg or adding amlodipine" is actionable. The alert engine includes clinical context and suggested responses.
- RPM pays for itself. $534K/year in RPM reimbursement + $1.2M/year in avoided readmissions vs. platform and staff costs of ~$300K/year. The ROI is overwhelming — and it improves patient outcomes simultaneously.
Was this case study helpful?