Choosing the Best AI Framework for Healthcare Applications
A Strategic Guide for Healthcare Leaders and AI Architects seeking to understand the strategic, technical, and regulatory factors in selecting the best AI framework for healthcare applications.
Artificial Intelligence in healthcare is no longer a futuristic concept. It is transforming healthcare systems by enabling advanced medical data analysis, automating clinical workflows, and leveraging big data to deliver actionable insights across the care continuum. Hospitals are using AI for early disease detection, payers are deploying fraud detection engines, pharmaceutical companies are accelerating drug discovery pipelines, and revenue cycle teams are automating billing validation.
The use of AI in healthcare systems, powered by big data, is projected to save the U.S. healthcare economy $150 billion annually by 2026.
Yet one foundational question remains underestimated:
Which AI framework is truly suitable for healthcare environments?
The answer is not simply “TensorFlow vs PyTorch.” Healthcare requires regulatory safety, explainability, interoperability, performance stability, and governance maturity. The wrong framework choice can create long-term compliance risks, clinician distrust, and operational inefficiencies.
This guide walks through the strategic, technical, and regulatory lens required to choose the right AI framework for healthcare applications.
Understanding AI in Healthcare: Start with the Right Foundation
Before evaluating tools, healthcare organizations must clearly define what they are solving. A critical first step is comprehensive data collection, which includes gathering historical data, clinical data, and other relevant health information.
This foundation enables organizations to implement AI effectively by ensuring that models are trained on robust, representative datasets that reflect real-world clinical scenarios. Clearly identifying the problem, understanding the available data, and aligning objectives are essential for successful AI adoption.
Finally, a systematic review of existing data sources and relevant literature is necessary to inform the selection and implementation of the best AI framework for healthcare applications.
Clinical Impact Comes First
AI in healthcare must tie back to measurable outcomes. Are you aiming to detect sepsis earlier? Predict hospital readmissions? Optimize clinical documentation workflows? Improve revenue cycle accuracy?
Without defining the clinical objective, framework evaluation becomes purely technical — and that’s a mistake.
For example, an early cancer detection model requires robust image processing support and multi-site validation capabilities. Predictive models play a crucial role in early detection and precision medicine by evaluating current and historical data to project future health events and identify at-risk patients sooner. Model performance is typically evaluated using metrics like AUROC, with predictive modeling in healthcare leveraging multimodal data to improve accuracy and clinical decision-making. In contrast, a claims automation system requires NLP capabilities and anomaly detection models with strong explainability.
Clarity of purpose determines framework fit. AI frameworks also enable personalized treatment options by analyzing genetic, clinical, and historical data, supporting the goals of precision medicine and tailored patient care.
Identify the Real Users
In healthcare, AI users are not just data scientists. They are:
- Physicians reviewing recommendations
- Nurses coordinating care
- Fraud analysts investigating claims
- Administrative teams managing billing
- Clinical team delivering direct patient care
- Medical staff managing patient needs and triage
Each user group has different expectations. Clinicians require transparency. Administrative teams prioritize efficiency. Researchers demand flexibility.
AI enables clinicians and the clinical team to focus on direct patient care by automating administrative tasks, streamlining workflows, and supporting early diagnosis. AI tools can enhance operational efficiency by automating repetitive tasks, significantly reducing the time medical staff spends on non-patient care activities.
Your framework must support these diverse workflows without compromising performance.
Map Data Complexity
Healthcare data is fragmented and multimodal. A typical deployment may involve:
- EHR data (structured records)
- Lab and diagnostic reports
- Imaging data
- Claims information
- Wearable or remote monitoring feeds
- Structured data
- Patient records
Organizing medical records and structured data using a data analytics platform is essential for extracting insights, supporting diagnosis, and improving patient outcomes. For example, AWS HealthLake uses machine learning to transform raw health data into the FHIR industry standard, enabling better data management and analytics.
An appropriate AI framework must support complex data pipelines, longitudinal patient tracking, and large-scale ingestion.
Compliance Is Non-Negotiable
Healthcare operates under strict regulatory oversight. Framework selection must consider:
- HIPAA requirements
- GDPR (for EU operations)
- Data residency constraints
- Security certifications such as SOC 2 and ISO 27001
Benefits and Challenges of AI Frameworks in Healthcare
The adoption of artificial intelligence frameworks in the healthcare industry is unlocking new possibilities for improving patient outcomes and transforming care delivery.
By leveraging advanced AI tools, healthcare providers can analyze vast amounts of patient data—from electronic health records and medical imaging to real-time monitoring feeds—to generate actionable insights and develop personalized treatment plans. These capabilities enable clinicians to make more informed decisions, tailor interventions to individual patient needs, and ultimately enhance the quality of patient care.
AI solutions also streamline clinical workflows and reduce the administrative burden on medical professionals. Automated data analysis, documentation, and scheduling free up valuable time, allowing healthcare staff to focus on direct patient interactions and complex clinical decision-making. For healthcare organizations, this translates into greater operational efficiency and improved resource allocation.
However, integrating artificial intelligence into healthcare is not without its challenges. Ensuring the privacy and security of sensitive patient data is paramount, as is addressing the risk of bias in AI-driven recommendations.
Healthcare organizations must also invest in robust infrastructure, ongoing staff training, and continuous maintenance to support the deployment and evolution of AI frameworks. Overcoming these hurdles is essential for realizing the full potential of AI in delivering better patient outcomes and more efficient healthcare services.
Key Criteria for Choosing an AI Framework
Once foundational clarity is established, evaluation can move to technical criteria. When assessing the best AI framework for healthcare applications, it is crucial to consider the role of advanced algorithms, machine learning, and deep learning, as these technologies drive innovation in diagnostics, predictive modeling, and operational automation.
Major cloud providers now offer managed AI frameworks specifically tailored for health data, streamlining compliance and scalability. Additionally, advanced analytics within these frameworks enable predictive insights, improve operational efficiency, and support informed decision-making in healthcare environments.
Explainability and Trust
Healthcare cannot rely on opaque “black-box” systems. Physicians must understand why a system recommended a diagnosis or flagged a patient as high risk. Human oversight is essential in clinical support tools, ensuring that AI complements—rather than replaces—healthcare professionals' judgment and decision-making.
AI tools can also enhance clinical workflows and decision-making, improving efficiency and outcomes across the healthcare ecosystem.
Modern AI frameworks should support:
- Feature importance outputs
- Model confidence scoring
- Explainability libraries such as SHAP or LIME
- Transparent inference logging
Trust determines adoption. Without interpretability, AI remains unused — even if technically accurate.
Privacy and PHI Handling
AI systems process Protected Health Information (PHI). Health systems must prioritize a unified data platform to ensure secure and effective AI implementation, as fragmented data can hinder both compliance and performance. The framework must integrate with:
- Encryption standards (at rest and in transit)
- Role-based access controls
- Audit trails
- Secure key management systems
Healthcare organizations face significant compliance risks when using generic AI tools that lack built-in controls for data security. If the framework cannot align with enterprise security practices, it should not be deployed in healthcare settings.
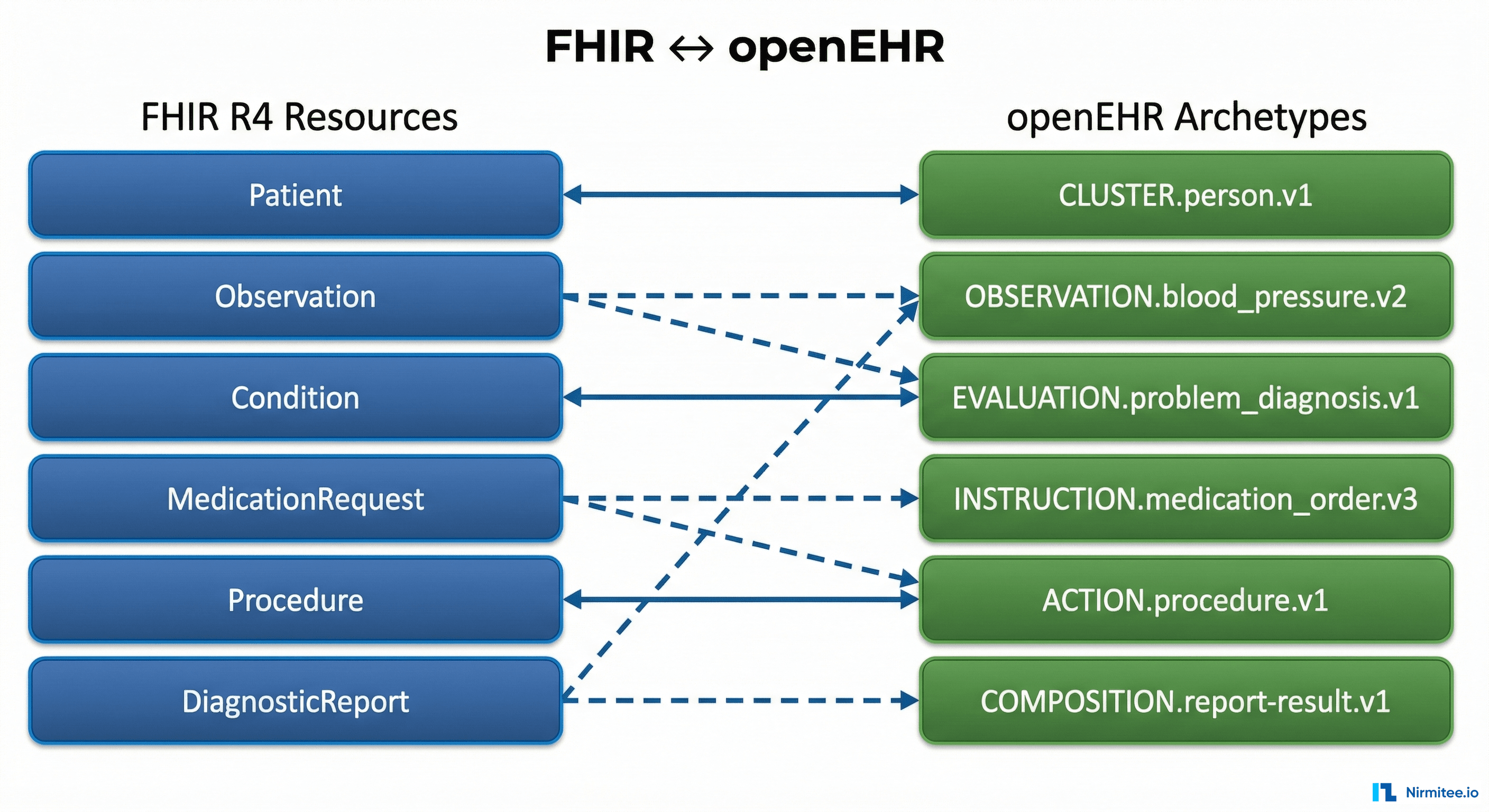
Interoperability with EHR Systems
Healthcare ecosystems run on HL7 and FHIR standards. Frameworks must either natively support or integrate with systems capable of handling:
- HL7 v2 messaging
- FHIR RESTful APIs
- Secure integration gateways
Interoperability is especially critical for extracting and summarizing clinical notes from EHRs, where large language models can automate documentation and generate concise summaries to support care teams. Transformer models excel in natural language processing for summarizing EHR data and generating patient education materials.
Poor interoperability leads to siloed AI, which defeats its purpose.
Deployment Scalability and Latency
Clinical workflows are time-sensitive. AI outputs must return in seconds, not minutes.
Frameworks should support:
- Cloud-native deployment
- Kubernetes orchestration
- Horizontal scaling
- Edge inference (if required for devices or bedside applications)
Workflow automation is essential for enabling real-time risk prediction, such as analyzing patient data to predict hospital readmissions and mortality, and for supporting efficient clinical workflows.
High-performance inference is critical for emergency settings.
Ensuring Reliable Data Analysis and Validation
Healthcare AI fails not because of model architecture, but because of validation weaknesses. Reliable data analysis and validation are critical, and this is where healthcare analytics platforms play a vital role.
These platforms support healthcare leaders in analyzing, interpreting, and leveraging data to improve patient care, operational efficiency, and strategic decision-making. AI-driven analytics can help healthcare teams analyze their performance and identify opportunities for improvement, further enhancing operational efficiency.
Additionally, predictive analytics in healthcare uses AI to forecast health events and implement proactive care interventions, enabling more effective and timely patient care.
Cross-Site Validation
Models trained in one hospital often fail in another due to demographic or operational differences.
A recent survey conducted by leading healthcare AI researchers highlights that cross-site validation is critical for ensuring model generalizability and reliability across diverse clinical settings.
Organizations must require:
- Multi-institution validation
- Bias testing across age, race, and gender
- External benchmarking studies
Monitoring for Model Drift
Healthcare data distributions evolve. Treatment protocols change. Patient demographics shift.
Your AI framework must integrate monitoring capabilities to detect:
- Performance degradation
- Data distribution drift
- Unexpected prediction anomalies
Continuous monitoring is essential for patient safety.
Comparing Popular AI Frameworks for Healthcare
Different frameworks serve different strategic needs. In healthcare, the best AI frameworks leverage deep learning, generative AI models, and advanced algorithms to drive innovation across diagnostics, drug discovery, and clinical operations.
These technologies enable higher accuracy in medical imaging, automate clinical documentation, and support predictive analytics for better patient outcomes.
Key frameworks include MONAI, the industry standard for deep learning in medical imaging, initiated by NVIDIA and King's College London. For drug discovery, DeepChem is widely used, while AlphaFold stands out for its high-accuracy protein structure prediction, essential in pharmaceutical research.
Generative Adversarial Networks (GANs) are increasingly adopted to generate synthetic medical data, supporting model training while protecting patient privacy. For unstructured clinical text, the most widely used framework is developed by John Snow Labs. Other notable tools include Dax Copilot for ambient clinical documentation and Convolutional Neural Networks (CNNs) for advanced imaging analysis.
TensorFlow
TensorFlow is widely used for production-grade deployments. It offers strong model serving capabilities, scalability, and enterprise integrations. TensorFlow supports advanced machine learning models in healthcare, powering frameworks like DeepChem and DeepNeuralNetQSAR that use machine learning to identify chemical compounds in drug discovery. It is often chosen when stability and operational maturity are primary concerns.
PyTorch
PyTorch excels in research flexibility. Academic institutions and research hospitals favor it for rapid experimentation and model innovation. Its flexible architecture enables researchers to experiment with different machine learning models and data modalities, optimizing model performance for healthcare applications. It provides dynamic computation graphs that allow deeper customization.
Hugging Face
For Natural Language Processing tasks such as clinical note summarization, medical transcription enhancement, and chatbot systems, Hugging Face offers state-of-the-art pretrained models and fine-tuning tools.
Hugging Face supports large language models (LLMs) and transformers like BERT and GPT, which are widely used in healthcare for analyzing clinical text, generating summaries of complex patient records, and automating clinical documentation and administrative workflows.
ONNX
ONNX provides cross-platform inference compatibility. It enables models to move between frameworks while maintaining performance consistency — useful in heterogeneous healthcare IT environments.
Commercial Platforms: The Case of IBM Watson Health (Now Merative)
Enterprise healthcare providers often evaluate commercial platforms such as Merative (formerly IBM Watson Health), which is recognized as a leading healthcare analytics platform and data analytics platform. Merative leverages AI to analyze clinical and patient data, supporting diagnoses and treatment planning for improved patient outcomes.
These platforms offer:
- Integrated healthcare workflows
- Compliance certifications
- Pre-built healthcare use cases
- Vendor-backed support
However, organizations must request:
- Real healthcare case studies
- Performance benchmarks
- Transparency into model limitations
- Vendor compliance documentation
Commercial convenience does not remove the need for due diligence.
Generative AI in Healthcare: Opportunities and Risks
Generative AI introduces powerful capabilities such as:
- Clinical documentation automation
- Patient communication drafting
- Medical coding suggestions
Generative AI models, including large language models and generative adversarial networks (GANs), are increasingly used in healthcare for automating administrative tasks, content creation, and clinical summarization. DAX Copilot, for example, reduces clinician burnout by automatically drafting documentation.
Generative AI has also proven useful for administrative use cases, helping providers automate routine communications and draft documentation efficiently. Additionally, GANs are used to create synthetic data for training AI models while protecting patient privacy.
But it also introduces risk.
Healthcare organizations must assess:
- Hallucination mitigation mechanisms
- Red-team testing results
- Human-in-the-loop workflows
- Output auditing systems
Generative AI must support clinician oversight — autonomy without supervision is unacceptable in medical environments.
Specialized Use Cases: Drug Discovery and Clinical Trials
AI frameworks supporting pharmaceutical research must integrate with:
- Molecular modeling libraries
- Bioinformatics pipelines
- Genomic datasets
AI plays a crucial role in drug development and discovery by accelerating the identification of new treatments, such as through patient stratification and molecular data analysis.
For example, Aiddison is an AI-assisted drug discovery tool from Merck that identifies molecules for drug development, while BioMorph is an AI tool that uses predictive analytics to analyze data sets and predict compound effects on cell health. AI supports drug discovery by analyzing chemical structures and predicting potential drug candidates, streamlining the process of bringing new therapies to market.
Clinical trial optimization systems should measure:
- Cohort selection accuracy
- Recruitment speed
- Dropout prediction
- Protocol adherence
Frameworks must support scientific rigor and reproducibility.
Operational Use Cases: Fraud Detection and Administrative Automation
AI is also transforming financial operations in healthcare.
Fraud detection requires robust anomaly detection modules capable of detecting unusual billing patterns.
AI-powered workflow automation can handle repetitive and administrative tasks such as scheduling, billing, and managing electronic health records (EHRs), which helps improve operational efficiency and reduces the burden on clinicians. Administrative automation should demonstrate measurable improvements in:
- Claims processing time
- Error reduction rates
- Staff workload reduction
AI can automate essential administrative tasks such as patient scheduling and data management, further streamlining healthcare workflows and reducing provider burnout.
Operational ROI must be clearly quantified.
Patient Safety and Security in AI-Driven Healthcare
As AI tools become increasingly embedded in clinical decision support and patient care, safeguarding patient safety and data security is more critical than ever.
Healthcare providers and organizations must ensure that AI models are transparent, explainable, and subject to rigorous oversight. Implementing human-in-the-loop processes allows medical professionals to review, validate, and, if necessary, override AI-generated recommendations, reducing the risk of errors and maintaining high standards of care.
Robust security protocols are essential to protect sensitive patient information from unauthorized access or breaches. This includes strong encryption, access controls, and regular security audits.
By prioritizing both the safety of clinical decision-making and the security of patient data, healthcare organizations can build trust in AI solutions and ensure that technology enhances, rather than compromises, patient care.
Case Studies and Research Highlights
Recent research and real-world case studies underscore the transformative impact of AI in healthcare. For instance, a study published in the Journal of the American Medical Association (JAMA) demonstrated that an AI-powered diagnostic tool could detect breast cancer from mammography images with remarkable accuracy, in some cases surpassing the performance of experienced radiologists.
This not only improves patient outcomes through earlier detection but also streamlines clinical workflows by assisting medical professionals in interpreting complex imaging data.
Another notable example comes from a study in Nature Medicine, where a predictive analytics platform was used to identify patients at high risk of hospital readmission. By flagging these individuals early, healthcare providers were able to intervene proactively, reducing unnecessary readmissions and improving overall patient care.
These examples highlight the potential of AI in healthcare to deliver measurable improvements in patient outcomes and operational efficiency, while also pointing to the need for continued research and innovation in this rapidly evolving field.
Collaboration and Partnerships in Healthcare AI
The successful implementation of AI in healthcare relies on strong collaboration and strategic partnerships across the industry. Healthcare organizations, technology companies, and research institutions are increasingly joining forces to accelerate the development of AI solutions that address real-world clinical challenges.
For example, IBM Watson Health has partnered with leading healthcare providers to create AI-powered clinical decision support tools, while collaborations with companies like Google have advanced the use of AI in medical imaging analysis.
These partnerships enable the pooling of expertise, data, and resources, resulting in more accurate, effective, and scalable AI solutions tailored to the needs of healthcare providers and patients. By working together, stakeholders in the healthcare sector can drive innovation, improve patient outcomes, and ensure that artificial intelligence is harnessed responsibly and effectively to transform care delivery.
Governance, Deployment, and Adoption Strategy
Even the most powerful AI framework fails without structured governance.
Health systems face significant challenges when they implement AI, including limited staff capacity, a lack of specialized talent, and the need for strategic planning to ensure successful adoption. The integration of AI into existing healthcare workflows can be complex and requires careful planning to avoid disruption and maintain quality of care.
Healthcare organizations must:
- Define AI model approval committees
- Establish validation protocols
- Create incident-response playbooks
- Train healthcare professionals on responsible usage
AI adoption is as much cultural as it is technical.
Recommended Roadmap for Implementation
A safe healthcare AI rollout typically follows this structure:
- Define a minimal viable clinical use case
- Ensure comprehensive data collection from diverse sources (structured, unstructured, and real-time device data) to enable robust predictive modeling and analytics
- Run a controlled pilot
- Conduct a multidisciplinary review to validate clinical, technical, and compliance perspectives
- Implement AI by integrating tools into clinical workflows and data systems, using phased deployment and collaboration with specialized solution providers
- Monitor with structured performance checkpoints
Rushing AI into healthcare settings without governance invites risk.
Final Thoughts
Choosing the right AI framework for healthcare is not about selecting the most popular open-source library. It is about aligning technology with clinical safety, regulatory compliance, operational scalability, and clinician trust.
Healthcare AI is not just software deployment. It is a system transformation.
The organizations that succeed will be those that combine technological sophistication with governance discipline and clinical partnership.