Overview
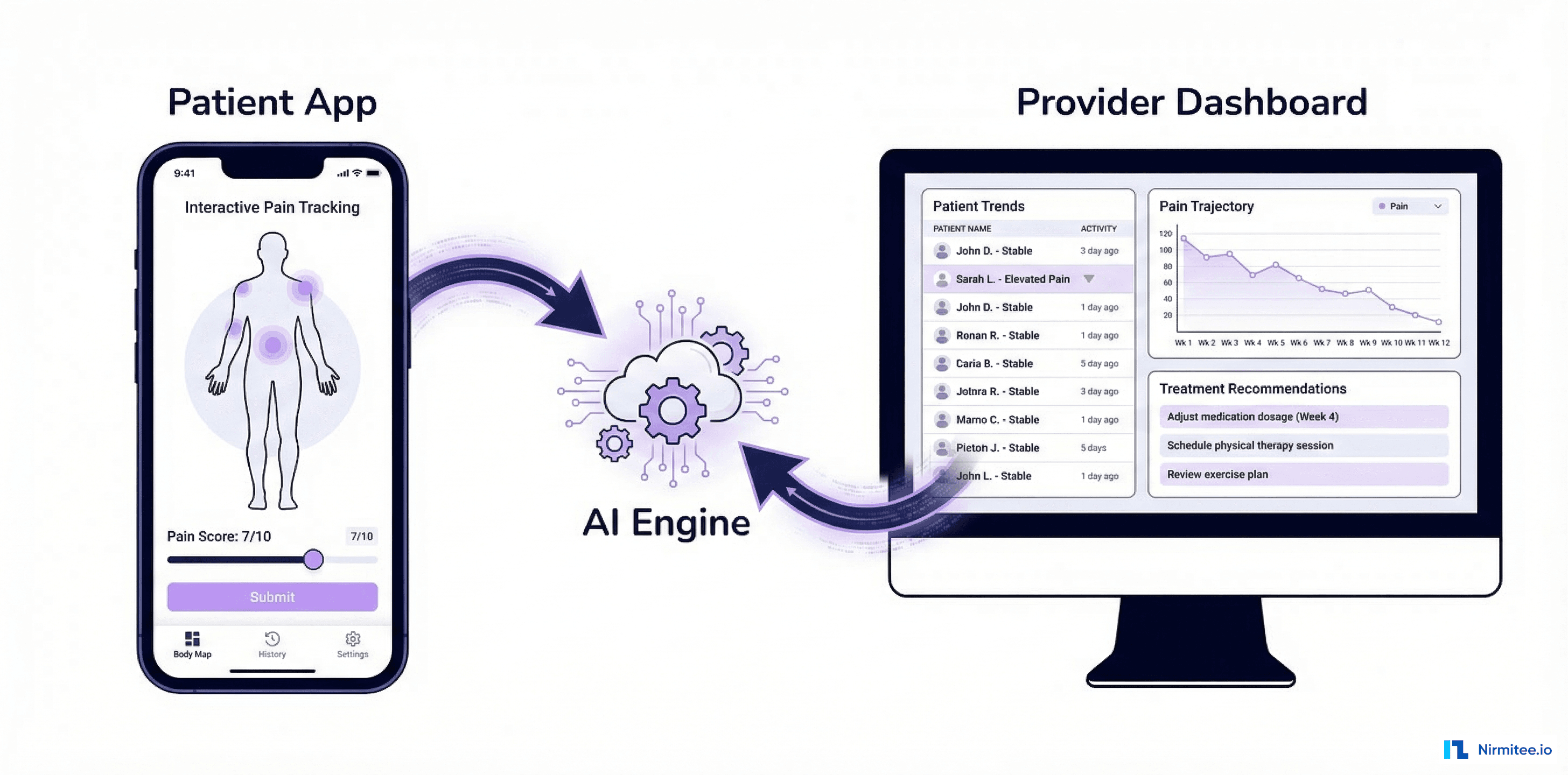
Remote Patient Monitoring (RPM) is changing how healthcare providers care for patients outside hospitals and clinics. Instead of waiting for patients to visit a doctor, RPM allows continuous tracking of vital signs, like blood pressure, heart rate, and oxygen levels, using smart medical devices.
One of our clients, a healthcare provider, was struggling with patient engagement, real-time health tracking, and managing large amounts of patient data. At Nirmitee, we developed a custom RPM software to solve these problems and improve patient care.
This case study explains:
- The challenges the provider faced before using our RPM system.
- How our solution made healthcare monitoring easier.
- The real impact on both doctors and patients.
Challenges Before Implementing Our RPM Solution
Before adopting our custom Remote Patient Monitoring (RPM) solution, the healthcare provider faced significant operational and clinical challenges that affected both patient care and efficiency. Here's a detailed look at the four major problems they struggled with:
1. Delayed Health Monitoring & Late Interventions
One of the biggest problems was that patients were only monitored during clinic visits. This meant that their health data, such as blood pressure, glucose levels, and oxygen saturation, was checked only when they physically came in for an appointment, often weeks or even months apart.
Why Was This a Problem?
- Chronic conditions like diabetes, hypertension, and heart disease require continuous monitoring, not just periodic check-ups.
- Many patients don't experience obvious symptoms even when their condition is worsening.
- Doctors had to rely on patient-reported symptoms, which were often incomplete or inaccurate. Patients might forget details or downplay their issues.
- Without real-time data, early warning signs were missed, leading to avoidable hospitalizations and emergency room visits.
2. Lack of Integration Between Medical Devices & EHR Systems
Most patients with chronic illnesses use home medical devices like blood pressure monitors, glucometers, and pulse oximeters to track their health. However, the biggest gap was that these devices were not connected to the healthcare provider's system.
Why Was This a Problem?
- Disconnected devices meant that patient readings stayed in separate silos, either stored in the device itself or manually logged by patients.
- Doctors had no way to access this vital information in real time, making it difficult to track a patient's progress between visits.
- Nurses had to manually enter patient data into Electronic Health Records (EHRs), which was time-consuming and prone to errors.
- If a patient forgot to bring their logbook or misreported their readings, their doctor was left making critical decisions with incomplete data.
3. Low Patient Engagement & Confusion About Health Data
Even when patients had access to existing RPM systems, engagement remained frustratingly low. Many patients abandoned their devices after a few weeks, leading to poor adherence and gaps in monitoring.
Why Was This a Problem?
- Many patients, especially older adults, found existing RPM devices complicated to set up and use.
- They struggled with technical issues, like connecting devices to apps or syncing data with their doctor's system.
- Patients were often confused by the health data shown on their devices; they didn't know what their numbers meant or when they should be concerned.
- Without motivation or reminders, patients simply stopped using their devices, making RPM programs ineffective.
4. Too Much Data, Not Enough Insights for Doctors
While the goal of RPM is to streamline patient monitoring, many healthcare providers found themselves overwhelmed by too much raw data without clear insights.
Why Was This a Problem?
- Every small fluctuation in a patient's vitals triggered an alert. Over time, these alerts became excessive, leading to alert fatigue among doctors.
- Physicians were bombarded with hundreds of notifications daily, making it harder to prioritize truly urgent cases.
- Instead of providing actionable insights, RPM systems simply dump large volumes of data on doctors, increasing their workload rather than reducing it.
These four challenges, delayed monitoring, lack of device integration, low patient engagement, and overwhelming data overload, were making it difficult for the healthcare provider to deliver proactive, high-quality care. Without real-time tracking and automated insights, patients were experiencing avoidable hospitalizations, doctors were overworked, and RPM adoption was failing.
To address these gaps, we developed a tailored RPM solution that not only streamlined monitoring and improved data accuracy but also enhanced patient engagement and empowered doctors with meaningful insights, all while ensuring a smooth, secure integration with existing healthcare systems.
Our RPM Solution: A Tailored Approach
To tackle the challenges of delayed health monitoring, disconnected devices, low patient engagement, and data overload, we built a custom Remote Patient Monitoring (RPM) solution that is seamless, accurate, and easy to use. Here's how our approach transformed healthcare monitoring: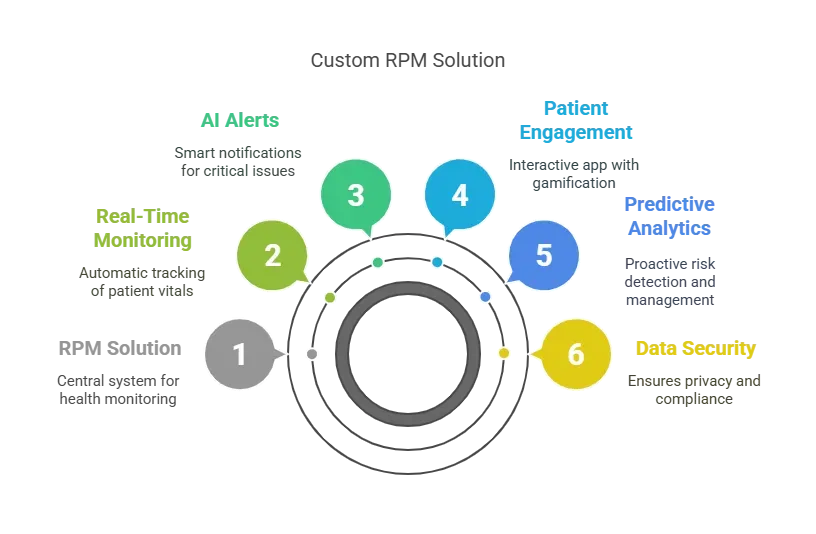
1.Real-Time Health Monitoring With Smart Devices
Our software is compatible with Bluetooth and IoT-enabled medical devices, allowing for automatic, real-time tracking of patient vitals.
How It Works:
Patients use smart medical devices like blood pressure monitors, glucose meters, and pulse oximeters at home. These devices sync automatically with our RPM system via Bluetooth and Wi-Fi connectivity. The readings are automatically uploaded to the patient's Electronic Health Record (EHR), eliminating manual data entry.
Result: Doctors get timely, accurate health data, reducing the chances of missed warning signs and unnecessary hospital visits.
2. AI-Powered Smart Alerts
Unlike traditional RPM systems that bombard doctors with endless notifications, our AI-driven alert system ensures that doctors are only notified when it truly matters.
How It Works:
The AI analyzes patient data trends over time. It filters out insignificant fluctuations and only alerts doctors when a pattern indicates a serious health risk. Doctors can customize alert thresholds based on each patient's condition and risk level.
Result: Doctors experience less alert fatigue and can focus on truly high-risk patients.
3. Easy-to-Use Patient App With Gamification
We built an intuitive mobile app that makes it easier for patients to track their health, understand their data, and stay engaged with their treatment.
Key Features:
- Simple Device Setup: Patients can easily pair their medical devices with the app in just a few taps.
- Visual Health Insights: Instead of complex numbers, the app presents easy-to-read charts and color-coded indicators to show whether a reading is normal, slightly off, or critical.
- Reminders & Notifications: Patients receive friendly reminders to take their readings, preventing missed check-ins.
- Gamification for Engagement: We introduced reward-based motivation to keep patients engaged.
Result: Patients stay actively involved in their own health monitoring, leading to better adherence and improved outcomes.
4. Predictive Analytics for Preventive Care
Our AI-powered predictive analytics helps doctors detect potential health risks before they become emergencies.
How It Works:
The system analyzes long-term trends in patient data. If patterns suggest an increased risk of heart failure, respiratory distress, or a stroke, the doctor is notified before the situation becomes critical. Predictive insights allow proactive treatment adjustments, reducing emergency hospitalizations.
Result: Fewer emergency hospital visits, improved patient safety, and better chronic disease management.
5. Data Security & HIPAA Compliance
Patient data security is a top priority, especially in remote healthcare. Our system follows strict compliance regulations to ensure privacy and data protection.
Security Measures Implemented:
- End-to-End Encryption: All data is securely transmitted to prevent unauthorized access.
- HIPAA Compliance: The software meets all HIPAA regulations, ensuring patient privacy.
- Multi-Factor Authentication (MFA): Adds an extra layer of security for both doctors and patients accessing the system.
Result: Healthcare providers trust the system, and patients feel confident knowing their health data is secure and private.
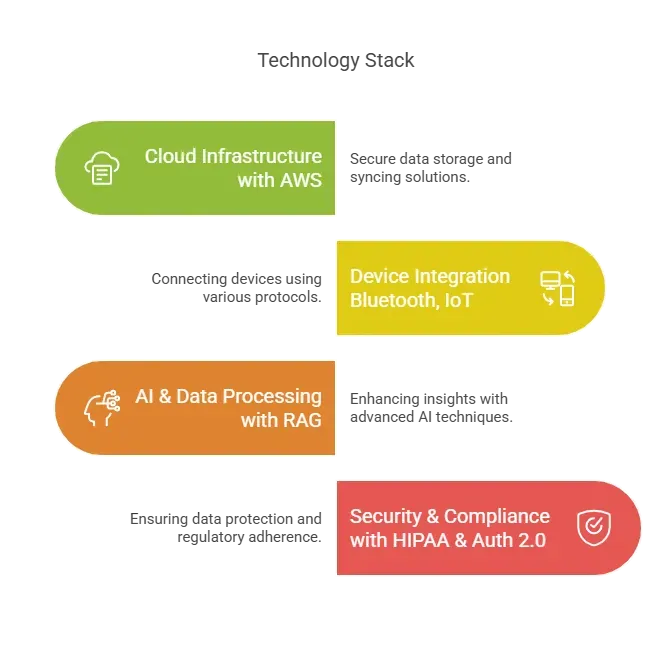
Technology Stack
- Cloud Infrastructure: AWS for secure data storage & real-time syncing.
- Device Integration: Bluetooth, IoT protocols (BLE, Wi-Fi, MQTT).
- AI & Data Processing: RAG (Retrieval-Augmented Generation) for accurate insights. We utilize RAG to enhance the accuracy and relevance of insights by combining our internal data with external knowledge sources. This allows us to provide contextually rich and precise information to healthcare providers, improving their decision-making.
- Security & Compliance: HIPAA-compliant encryption, OAuth 2.0 for authentication.
Impact: How Our RPM Software Transformed Patient Care
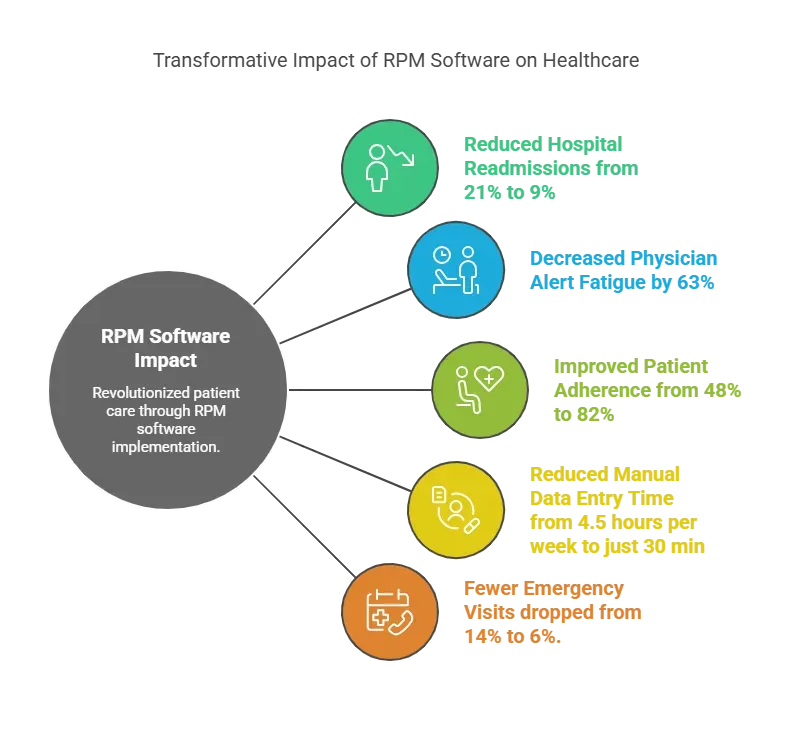
The results were game-changing for both patients and providers.
- Hospital readmissions dropped from 21% to 9%, reducing unnecessary hospital stays by 57%.
- Physician alert fatigue decreased by 63%, making it easier for doctors to focus on critical cases.
- Patient adherence to RPM improved from 48% to 82%, meaning more patients actively monitored their health.
- Time spent on manual data entry reduced from 4.5 hours per week to just 30 minutes, freeing up doctors and nurses to focus on patient care.
- Emergency visits for RPM patients dropped from 14% to 6%, thanks to early interventions.
 One patient, a 68-year-old with chronic heart failure, avoided a potentially life-threatening hospitalization when the system detected a sudden drop in oxygen saturation levels, prompting a timely intervention by their care team.
One patient, a 68-year-old with chronic heart failure, avoided a potentially life-threatening hospitalization when the system detected a sudden drop in oxygen saturation levels, prompting a timely intervention by their care team.
Conclusion
By automating remote patient monitoring, improving engagement, and reducing data overload, our custom RPM software empowered doctors to deliver better care while helping patients take control of their health. With real-time data, AI-powered alerts, and predictive analytics, the healthcare provider shifted from reactive to proactive care, preventing hospitalizations and improving patient outcomes.