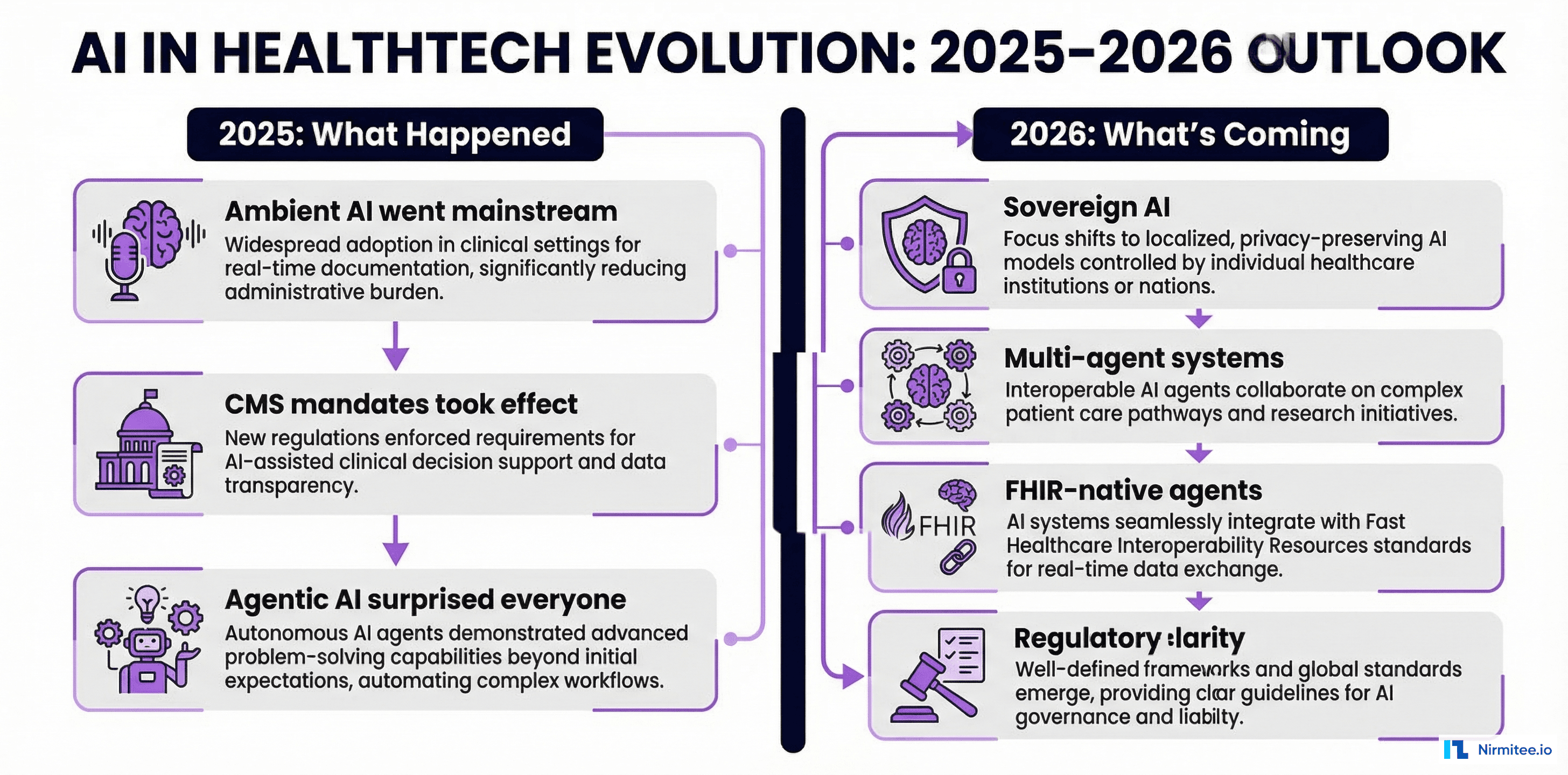
Your healthtech MVP works. You have a signed LOI from one hospital. Your demo is sharp. But then a health system CIO asks the question that stalls every promising startup: "Does it integrate with our Epic instance?"
That single question has killed more healthtech growth trajectories than funding shortfalls or regulatory hurdles combined. According to a 2024 KLAS Research report, 78% of hospital IT leaders will not evaluate a clinical tool that lacks certified EHR integration. If your product cannot speak the language of the hospital's electronic health record, you are not a vendor candidate — you are a pilot curiosity.
This guide breaks down exactly what happens after MVP when healthtech startups need to scale from one hospital connection to fifty, the real timelines and costs involved, the architectural patterns that separate successful integrations from failed ones, and how to navigate the certification gauntlets of Epic App Orchard and Oracle Health (formerly Cerner) CODE.
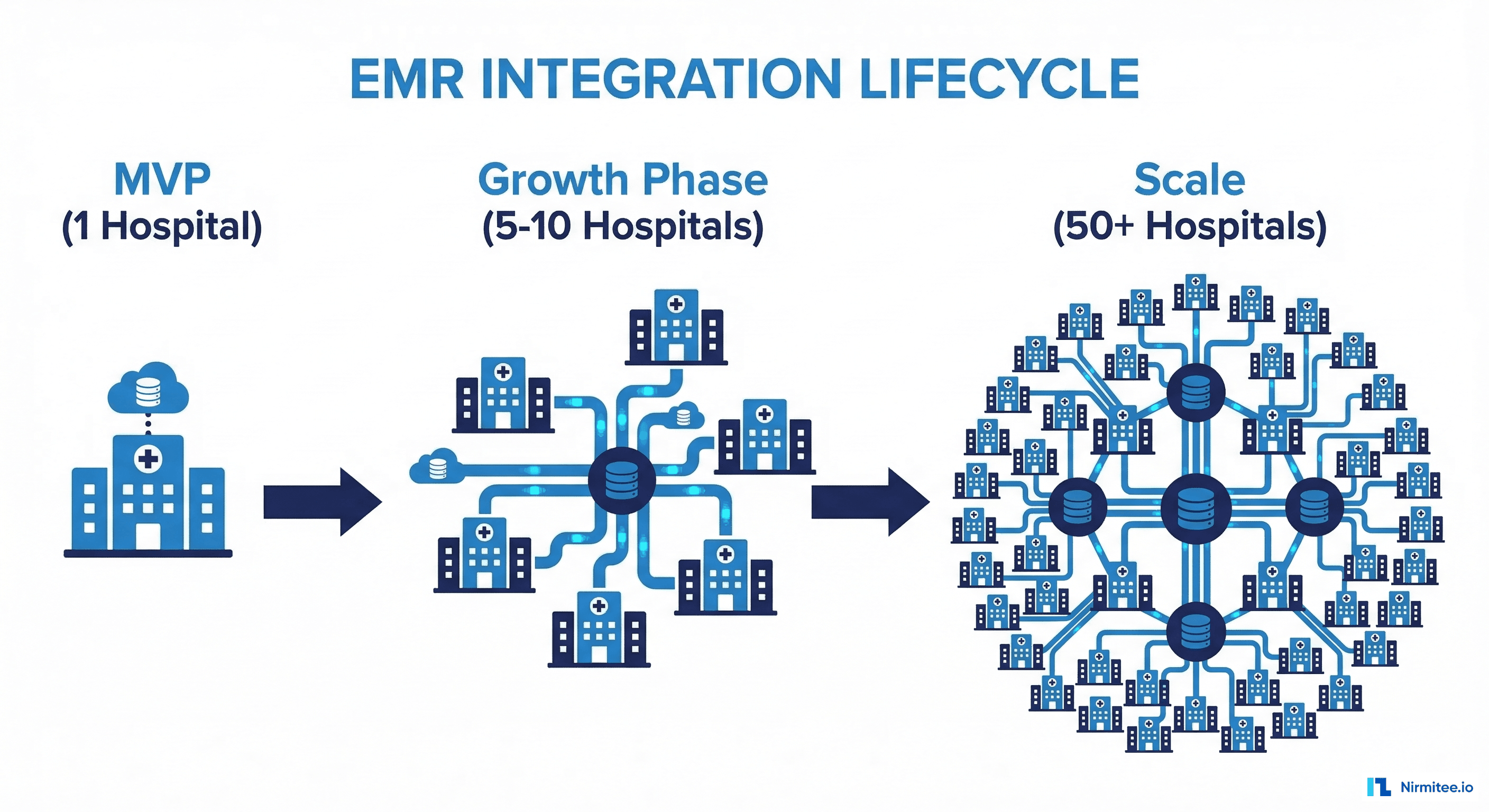
The Post-MVP Integration Gap: Why Startups Stall at 1-3 Hospitals
Most healthtech startups build their MVP with one of two approaches: a standalone system that exports CSV reports, or a lightweight FHIR-based read connection to a single EHR sandbox. Neither approach survives first contact with a production health system.
The gap between MVP-grade integration and production-grade EHR connectivity typically involves five dimensions that startups underestimate:
1. Authentication and Authorization Complexity
Your sandbox used a static bearer token. Production requires SMART on FHIR app launch sequences, OAuth 2.0 flows with PKCE, and patient-mediated access controls. Each EHR vendor implements these differently. Epic uses its own MyChart integration patterns. Oracle Health requires specific Millennium API authentication flows.
2. Data Model Translation
FHIR R4 is a standard in theory. In practice, each health system extends it differently. Epic bundles medications under MedicationRequest with custom extensions for pharmacy routing. Oracle Health uses different code systems for problem lists. Allscripts implements proprietary resource profiles for clinical documents.
3. Write-Back Requirements
Reading patient data is step one. Hospitals expect clinical decision support tools to write observations, notes, and orders back into the EHR. Write-back multiplies the integration complexity by 3-5x because you now need to handle conflict resolution, validation rules, and workflow state machines.
4. Certification and Marketplace Requirements
Epic App Orchard, Oracle Health CODE, and other vendor marketplaces require formal certification before a hospital can install your integration. These are not rubber stamps — they involve code review, security assessments, and functional testing against the vendor's validation suites.
5. Operational Monitoring
Production integrations fail. HL7v2 interfaces drop messages. FHIR endpoints return 429 rate limits during peak hours. You need monitoring, alerting, and retry logic that your MVP never required.

The Real Cost of EHR Integration: Numbers Nobody Publishes
Let us be direct about what post-MVP EHR integration actually costs. These numbers come from our work delivering EHR integrations across 40+ health systems.
| Cost Category | Epic | Oracle Health (Cerner) | Allscripts/MEDITECH |
|---|---|---|---|
| App Orchard / CODE enrollment | $5,000 - $15,000 | $3,000 - $10,000 | $2,000 - $8,000 |
| Development (sandbox + production) | $80,000 - $200,000 | $60,000 - $150,000 | $40,000 - $100,000 |
| Certification and testing | $15,000 - $50,000 | $10,000 - $30,000 | $5,000 - $20,000 |
| Per-hospital deployment | $5,000 - $15,000 | $3,000 - $10,000 | $2,000 - $8,000 |
| Annual maintenance (per EHR) | $20,000 - $60,000 | $15,000 - $40,000 | $10,000 - $25,000 |
| Total first-year cost | $125,000 - $340,000 | $91,000 - $240,000 | $59,000 - $161,000 |
These figures assume a single integration use case (such as clinical data read + write-back). Multi-workflow integrations — combining patient intake, clinical decision support, and billing — can double or triple these numbers.
The hidden cost is time. A startup that begins Epic certification in January typically cannot go live in a production environment until July or August. That is six to eight months of sales pipeline friction where every hospital prospect says, "Call us when you are on App Orchard."
Architecture Patterns for Scaling from 1 to 50 Hospital Connections
The architectural decisions you make at the post-MVP stage determine whether adding hospital #50 costs $5,000 or $50,000. Here are the three patterns we see in successful healthtech scaling:
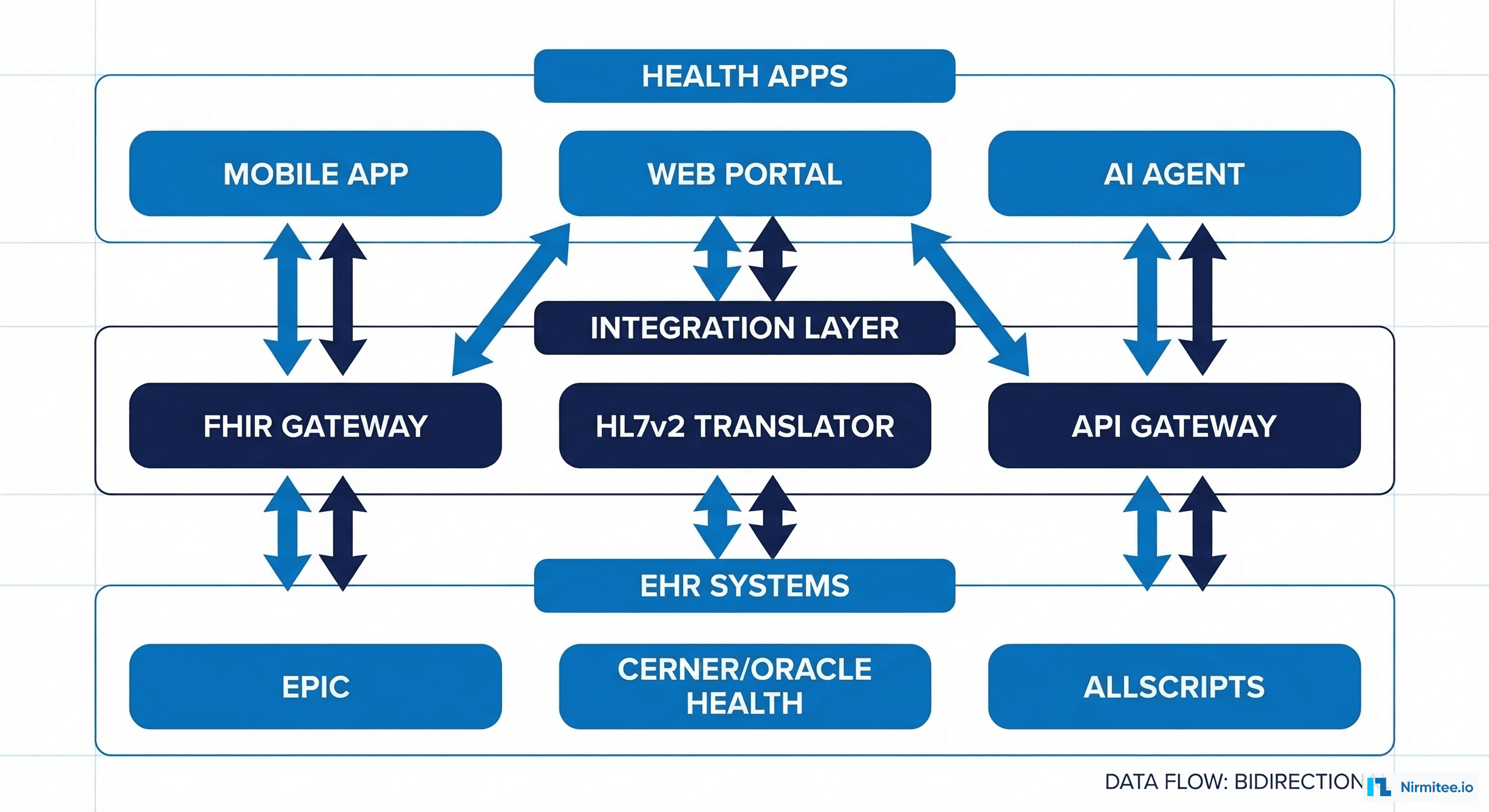
Pattern 1: Abstracted FHIR Gateway
Build a middleware layer that normalizes all EHR interactions into a single internal API. Your application code never touches Epic or Cerner APIs directly — it speaks to your FHIR Gateway, which translates requests into vendor-specific calls.
// Abstracted FHIR Gateway - your app calls this
GET /api/patients/{patientId}/medications
// Gateway translates to Epic:
GET https://epic-fhir.hospital.org/api/FHIR/R4/MedicationRequest
?patient={epicPatientId}
&_include=MedicationRequest:medication
// Or to Oracle Health (Cerner):
GET https://fhir.cerner.com/r4/{tenantId}/MedicationRequest
?patient={cernerPatientId}
&_count=100This pattern pays for itself after the third hospital. Each new EHR connection becomes a configuration exercise rather than a development project. We implemented this approach for a clinical documentation startup that grew from 3 to 27 hospital connections in 14 months.
Pattern 2: Event-Driven Integration with Message Queues
For workflows that involve bidirectional data exchange — such as RPM data flowing into EHRs — an event-driven architecture using Kafka or similar message brokers provides the reliability and scalability that direct API calls cannot.
// Event-driven EHR write-back pattern
{
"topic": "ehr.writeback.observations",
"key": "patient-12345",
"value": {
"resourceType": "Observation",
"status": "final",
"code": {
"coding": [{
"system": "http://loinc.org",
"code": "85354-9",
"display": "Blood pressure panel"
}]
},
"targetEHR": "epic",
"targetFacility": "memorial-general",
"retryPolicy": {
"maxAttempts": 3,
"backoffMs": 5000
}
}
}Pattern 3: Hybrid Mirth + FHIR
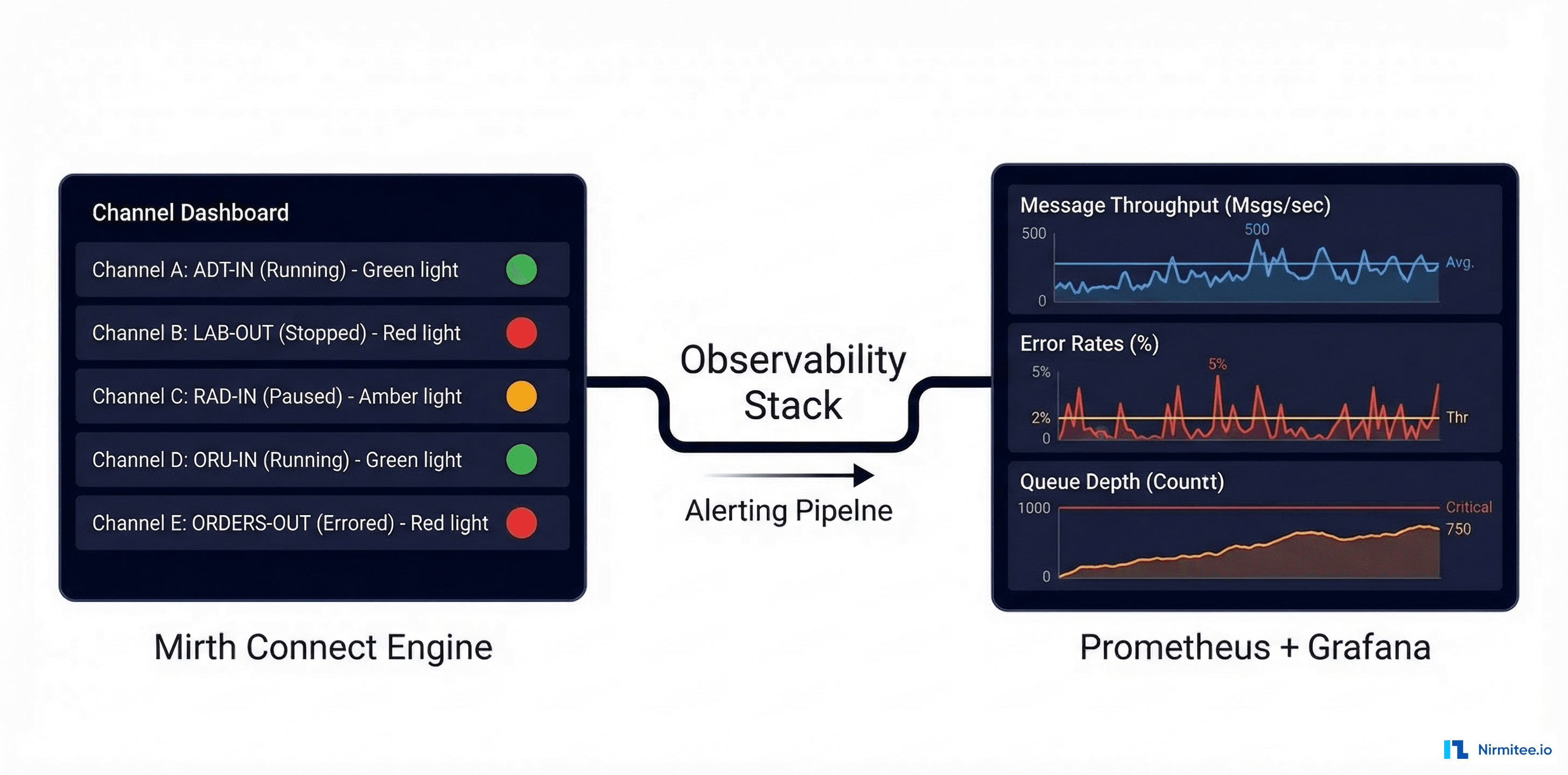
Many hospitals still run HL7v2 interfaces for ADT feeds, lab results, and orders. A production integration strategy must handle both FHIR (for modern APIs) and HL7v2 (for legacy interfaces). Mirth Connect serves as the HL7v2 protocol translator while your FHIR Gateway handles REST-based interactions.
This hybrid approach is particularly relevant for startups integrating with mid-market health systems that run a mix of modern and legacy EHR versions. We detail this architecture in our Mirth Connect channel design patterns guide.
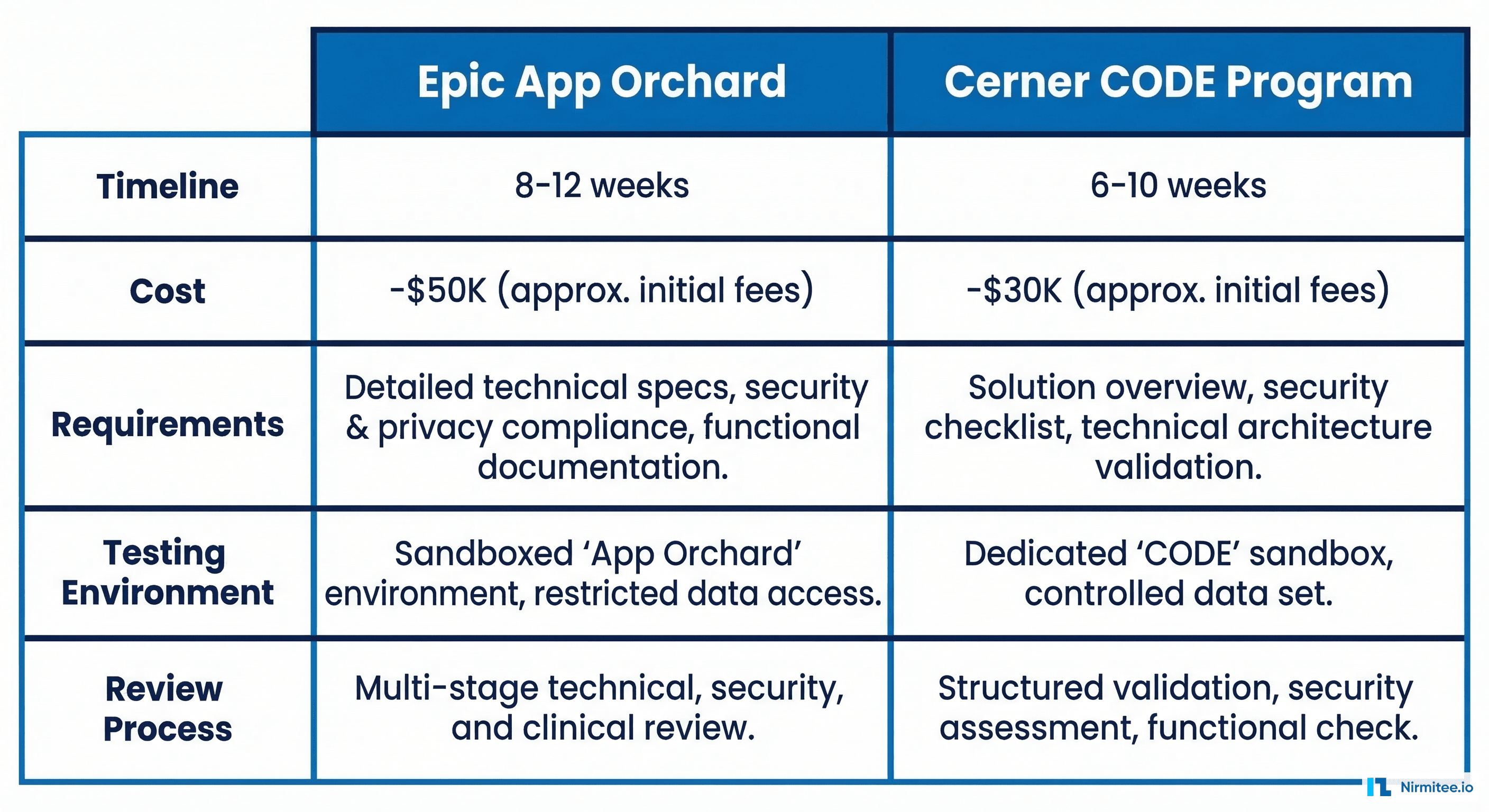
Navigating Epic App Orchard: A Realistic Timeline
Epic controls roughly 38% of the US hospital EHR market. If you are building a healthtech product that serves hospitals, Epic integration is not optional — it is table stakes.
Here is what the App Orchard certification process actually looks like:
Week 1-2: Application and enrollment. You submit your application describing your product, intended use cases, and requested FHIR scopes. Epic reviews this within 5-10 business days. Approval is not guaranteed — Epic rejects applications that duplicate existing marketplace offerings.
Week 3-8: Sandbox development. You receive access to Epic's FHIR sandbox environment. This is where you build and test your integration against synthetic patient data. The sandbox closely mirrors production, but there are differences in data volume, response times, and edge cases that will surface later.
Week 9-14: Technical review. Epic's team reviews your integration code, security practices, and FHIR resource usage patterns. They check for proper error handling, rate limit compliance, and adherence to their SMART on FHIR implementation guide. This is where most startups get stuck — Epic sends back revision requests that add 2-4 weeks.
Week 15-18: Connection hub testing. You test against Epic's connection hub, which simulates real hospital environments with production-like data volumes.
Week 19-22: Marketplace listing and first customer go-live. Once approved, your app appears on App Orchard. But each hospital still needs to enable it, configure local security policies, and complete their own testing — which adds another 2-4 weeks per site.
Total realistic timeline: 22-30 weeks from application to first production patient.
Oracle Health (Cerner) CODE Program: What Changed After the Oracle Acquisition
The Oracle acquisition of Cerner in 2022 reshaped the CODE program significantly. Here is the current landscape:
Oracle Health has been migrating from Cerner's legacy Millennium APIs to a more standardized FHIR R4 implementation. The CODE program now emphasizes:
- FHIR-first development: New applications should use the FHIR R4 API wherever possible. Legacy Millennium APIs are still available but Oracle is deprecating them on a rolling basis.
- Oracle Cloud Infrastructure (OCI) hosting: Oracle is pushing partners toward OCI for hosting integrated applications. While not mandatory, OCI-hosted applications receive faster review cycles.
- Streamlined certification: The CODE certification process has been shortened to 6-10 weeks for FHIR-only integrations, down from 10-16 weeks under the legacy program.
The practical impact for startups: if you are starting fresh, build your Cerner integration on FHIR R4. If you have an existing Millennium-based integration, plan a migration timeline because those APIs will not be supported indefinitely.
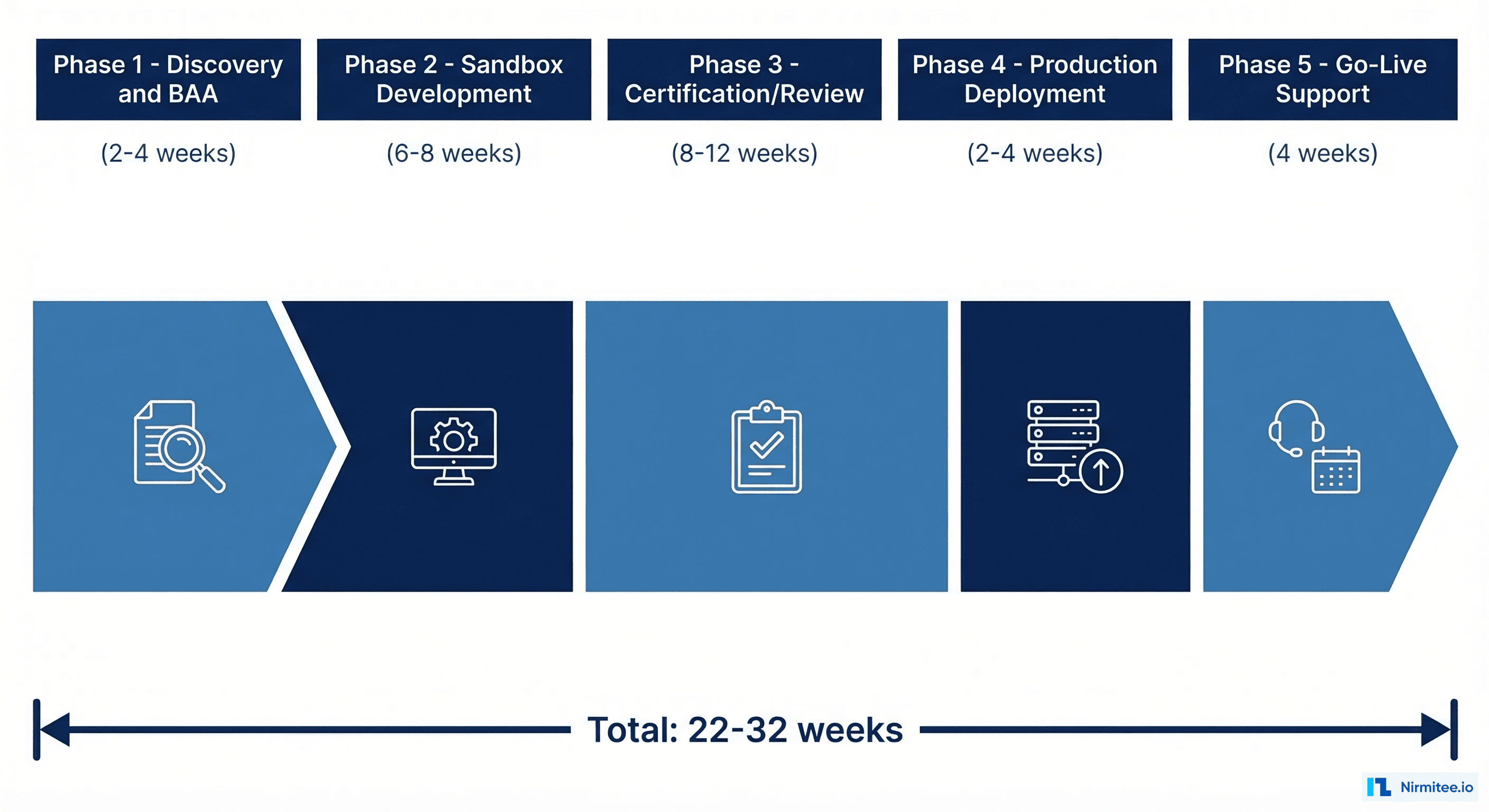
The Integration Team You Actually Need
Startups consistently underestimate the team required for production EHR integration. Here is what a realistic integration team looks like:
| Role | FTE Required | Why They Matter |
|---|---|---|
| Integration Engineer | 1.5 - 2.0 | Builds and maintains FHIR/HL7v2 connections, handles vendor-specific quirks |
| Security/Compliance Lead | 0.5 | Manages BAAs, security reviews, HIPAA compliance documentation |
| QA/Validation Engineer | 0.5 - 1.0 | Writes and executes test suites against EHR sandboxes and production |
| Project Manager (EHR-experienced) | 0.5 | Coordinates with hospital IT teams, manages certification timelines |
| DevOps/SRE | 0.5 | Handles monitoring, alerting, and infrastructure for integration middleware |
That is 3.5 to 4.5 FTEs dedicated to integration. For a Series A healthtech startup, this is a significant portion of the engineering team. This is exactly why many startups choose to partner with specialized integration firms rather than building this capability in-house.
Common Integration Failures and How to Avoid Them
After delivering 40+ EHR integration projects, we have cataloged the failure patterns that repeat across startups:
Failure 1: Building for Sandbox, Not Production
Epic's sandbox returns clean, consistent FHIR responses. Production returns messy data with missing fields, unexpected code systems, and resources that do not conform to published profiles. Build your data parsing with defensive coding from day one — assume every field can be null, every code system can be unexpected, and every response can be paginated.
Failure 2: Ignoring Rate Limits
Epic enforces strict rate limits on FHIR API calls. If your application queries patient data for a population health dashboard, you will hit these limits within minutes. Design your architecture with caching layers and batch query patterns from the start.
Failure 3: Underestimating HL7v2 Requirements
Many hospitals still require HL7v2 ADT feeds for patient admission, discharge, and transfer events. If your product needs real-time patient census data, you likely need both FHIR (for clinical data) and HL7v2 (for operational events). Planning a dual-protocol strategy early prevents costly rework.
Failure 4: No Fallback Strategy
EHR APIs go down. Epic's FHIR endpoints experience planned maintenance windows. Oracle Health has documented outage patterns during upgrade cycles. Your application needs graceful degradation — cached data, queued write-backs, and clear user messaging when live EHR data is unavailable.
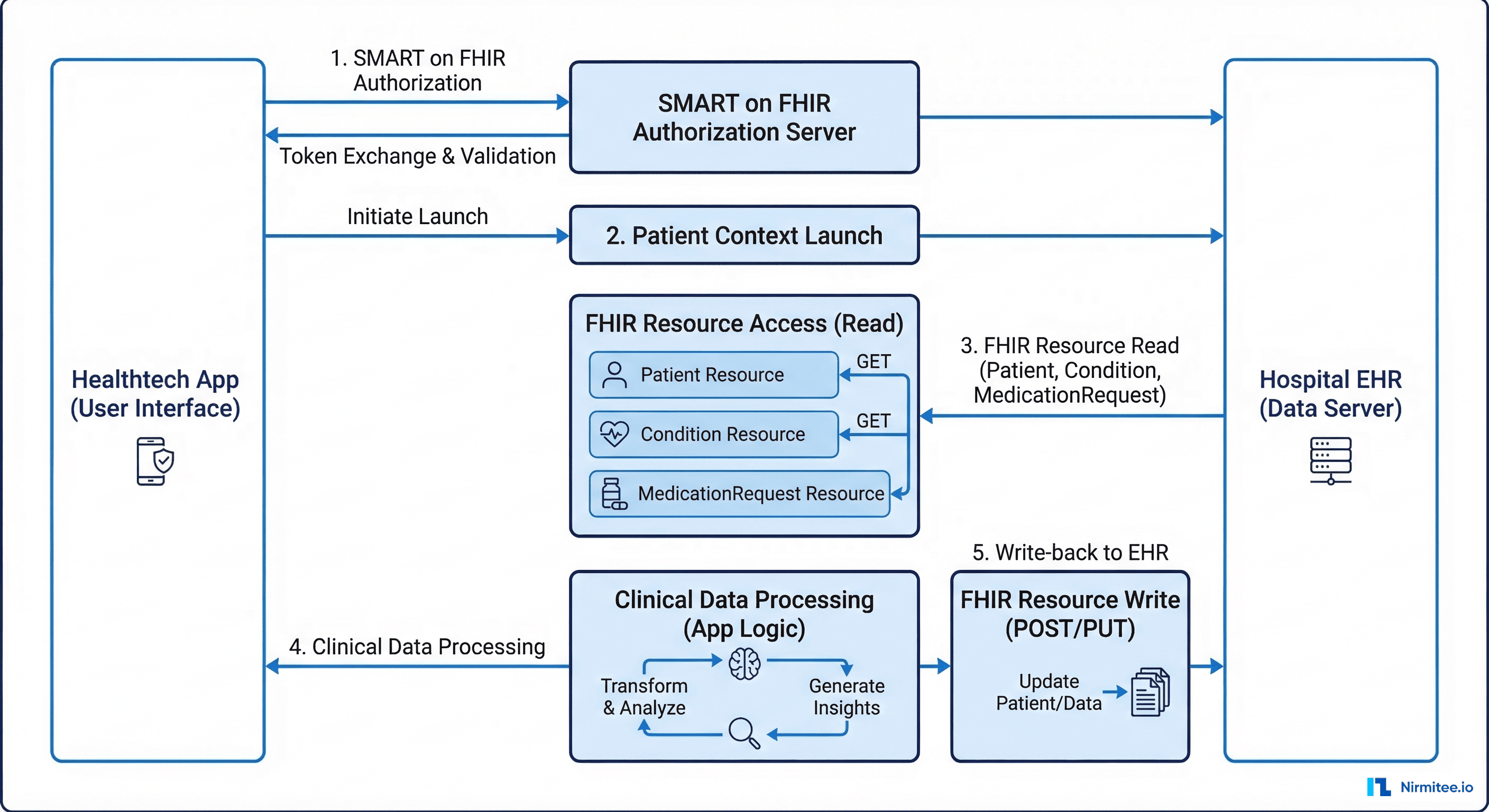
Measuring Integration ROI: The Metrics That Matter
EHR integration is expensive. Here is how to measure whether the investment is paying off:
- Sales cycle reduction: Track average days from first demo to signed contract, before and after EHR certification. Our clients typically see a 40-60% reduction in sales cycle length once they achieve App Orchard certification.
- Hospital onboarding velocity: Measure days from contract signature to first production patient. With a mature integration platform, this should decrease from 90+ days to 20-30 days.
- Integration maintenance burden: Track engineering hours spent on integration issues per hospital per month. A well-architected integration platform reduces this to under 2 hours per hospital per month.
- Data completeness rate: Measure the percentage of required clinical data fields that are successfully populated from the EHR. Target 95%+ for core demographics and 85%+ for clinical data.
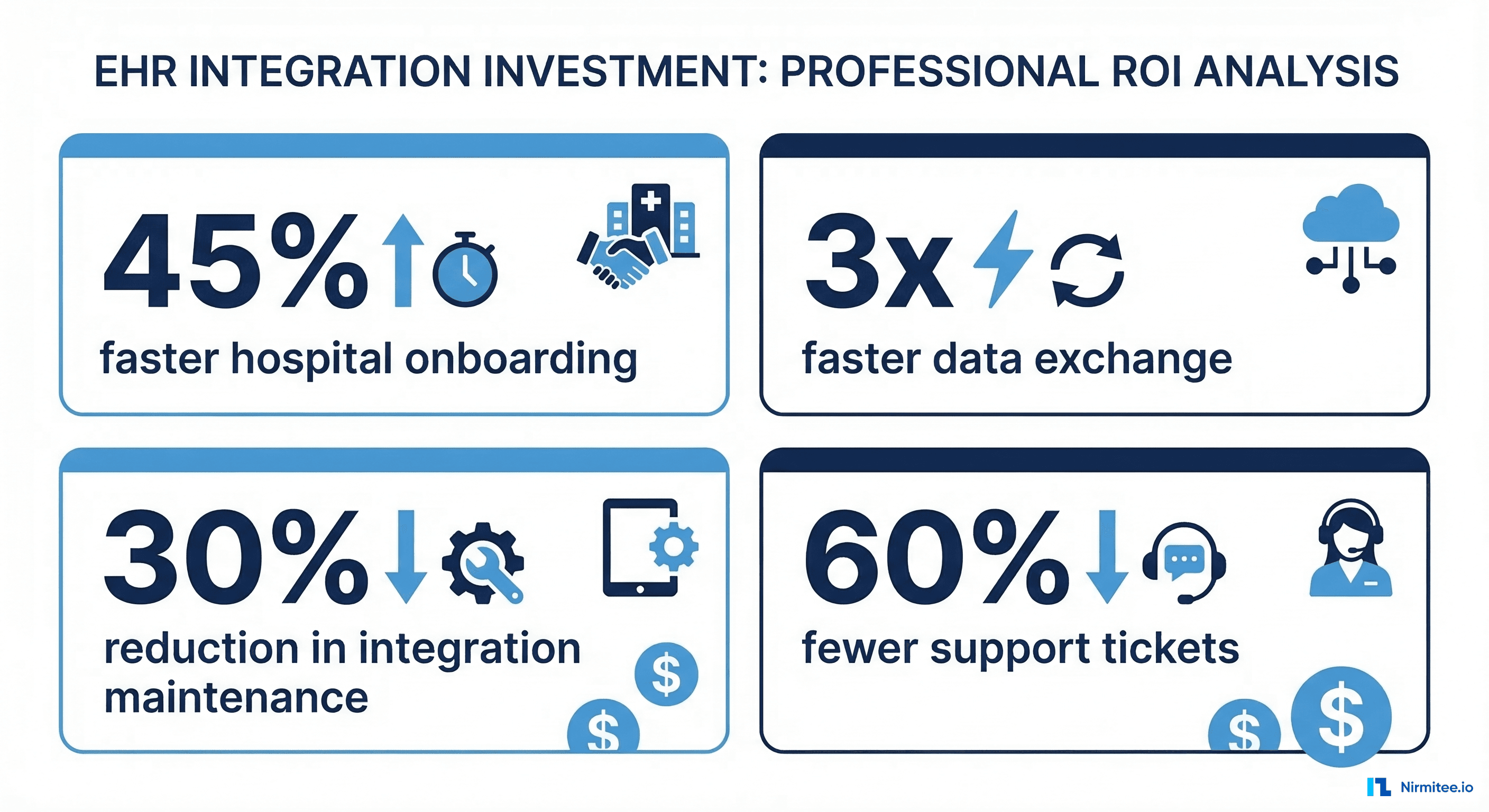
The Strategic Decision: Build vs. Partner for EHR Integration
Every healthtech startup faces this choice. Here is a framework for deciding:
Build in-house if: EHR integration is your core product differentiator, you have raised Series B or later with $5M+ allocated to integration, and you can hire experienced healthcare integration engineers (a scarce talent pool).
Partner with a specialized firm if: Integration is a means to an end (you need it for market access, not as a product feature), you are pre-Series B and need to preserve cash runway, or you need to be on Epic and Cerner within 6 months rather than 18.
Many of the fastest-growing healthtech companies take a hybrid approach: partner for the initial certification and first 5-10 hospital deployments, then gradually bring integration expertise in-house as the business scales.
Next Steps for Your Healthtech Startup
If you are sitting at the post-MVP stage with hospital contracts contingent on EHR integration, here is the priority sequence:
- Audit your target market: Determine which EHR systems your target hospitals run. If 60%+ are Epic shops, start there.
- Architect for multi-EHR from day one: Even if you start with one vendor, build the abstraction layer now. It is 10x cheaper than retrofitting later.
- Begin certification early: Start the App Orchard or CODE application process immediately — the review timeline runs in parallel with your development work.
- Plan for HL7v2 alongside FHIR: Most health systems need both. Do not assume FHIR-only will suffice.
- Budget realistically: Allocate $150K-$300K and 6-9 months for your first production EHR integration. Anything less is a setup for missed deadlines.
Nirmitee has delivered EHR integrations for 40+ healthtech startups scaling past their MVP stage. Our team handles the full lifecycle — from Epic App Orchard certification through production deployment and ongoing maintenance. If your growth is blocked by integration timelines, reach out to our integration team or explore our healthcare engineering services to see how we can accelerate your path to production.