The average US hospital generates 50 terabytes of clinical data per year across 16+ disconnected systems. Lab results arrive as HL7v2 ORU messages. Claims flow through X12 EDI. Radiology images are stored in PACS as DICOM. Clinical notes live in the EHR as unstructured text. Patient-reported outcomes come from mobile apps as FHIR QuestionnaireResponses. And someone in IT is responsible for making all of it accessible, accurate, and compliant.
Traditional data management approaches — ETL pipelines, data warehouses, manual reconciliation — were designed for a world where data arrived in batches and formats were predictable. Healthcare data in 2026 is neither. It arrives continuously, in dozens of formats, with quality issues that require clinical context to resolve (is a heart rate of 220 an error or a genuine SVT episode?).
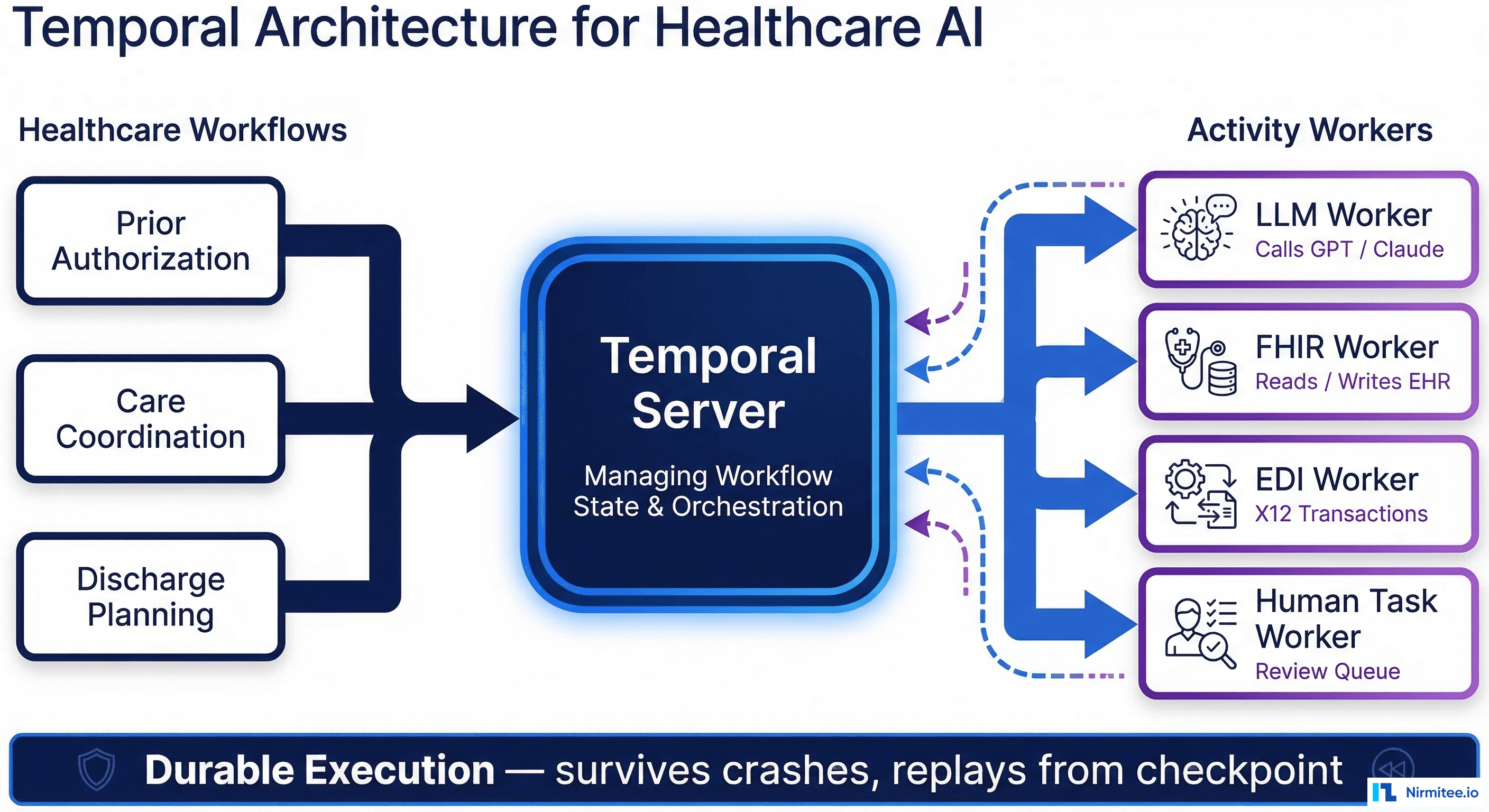
Agentic AI changes the equation. Instead of rigid pipelines that break when data deviates from expected patterns, AI agents can: interpret ambiguous data using clinical context, route information to the correct destination based on content (not just source), detect quality issues that rule-based validation misses, and maintain compliance by understanding what constitutes PHI across different data types.

The Healthcare Data Management Challenge
Healthcare data management is fundamentally harder than data management in other industries for five reasons:
- Fragmentation: The average hospital uses 16+ data systems that were never designed to talk to each other. Each system has its own data model, its own identifier scheme, and its own idea of what a "patient record" contains.
- Volume: A single ICU patient generates 1,440 data points per day from vital sign monitoring alone. Multiply by hundreds of patients across dozens of departments, and the data volume overwhelms manual management.
- Variety: HL7v2, FHIR R4, X12 EDI, DICOM, NCPDP SCRIPT, CDA/C-CDA, proprietary CSV exports, PDF scanned documents. No other industry deals with this many active data standards simultaneously.
- Quality: A study in BMC Medical Informatics found that 34% of clinical records have at least one missing required field. Duplicate patient records average 8-12% across health systems. Lab results use local codes instead of LOINC in 40-60% of cases.
- Compliance: Every piece of clinical data is potentially PHI under HIPAA. Every access must be logged. Every transfer must be encrypted. Every storage location must be covered by a BAA. The compliance surface is enormous.
How Agentic AI Transforms Data Management
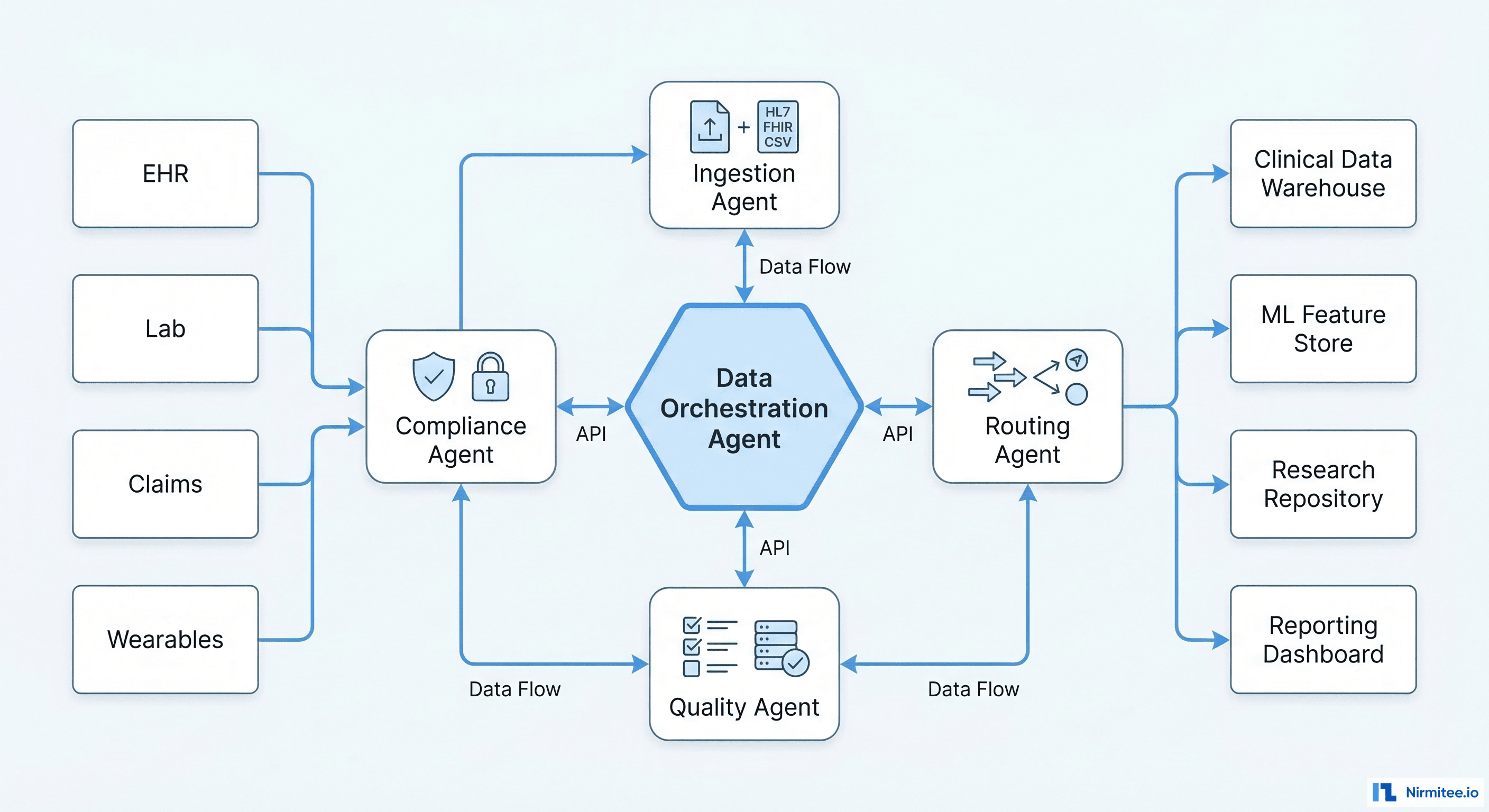
An agentic approach to healthcare data management deploys specialized AI agents for each stage of the data lifecycle:
Ingestion Agent
Handles incoming data from all sources. Unlike traditional ETL connectors that break when message formats deviate from specification, the Ingestion Agent can parse malformed HL7v2 messages (missing required segments, non-standard delimiters), extract structured data from unstructured sources (PDF lab reports, faxed referral letters), and route data based on content analysis rather than source identification.
A concrete example: a lab system sends an ORU message with a non-standard OBX segment structure. A traditional Mirth Connect channel rejects the message and puts it in an error queue for manual review. The Ingestion Agent recognizes the clinical content (it is a CBC result), maps the non-standard fields to the correct LOINC codes, and processes the message — logging the deviation for the integration team to address with the lab vendor.
Quality Agent
Validates incoming data against clinical rules, not just structural rules. A structural validator checks whether a field is populated. The Quality Agent checks whether the value makes clinical sense — flagging a hemoglobin of 45 g/dL (likely a decimal error, should be 4.5), identifying duplicate lab orders that may indicate a system glitch, and detecting temporal inconsistencies (a discharge date before an admission date).
Routing Agent
Determines where data should go based on its content and the organizational data architecture. Clinical results go to the EHR and the clinical data warehouse. Claims data goes to the revenue cycle system. Research-eligible data (after de-identification) goes to the research repository. The Routing Agent maintains a dynamic routing table that adapts as new data consumers are added.
Compliance Agent
Monitors every data movement for HIPAA compliance. Detects PHI in unexpected locations (a patient name in a free-text field that should contain only codes), enforces minimum necessary access (flagging queries that pull more patient data than the requester's role requires), and maintains the audit trail that HIPAA mandates for every PHI access event.
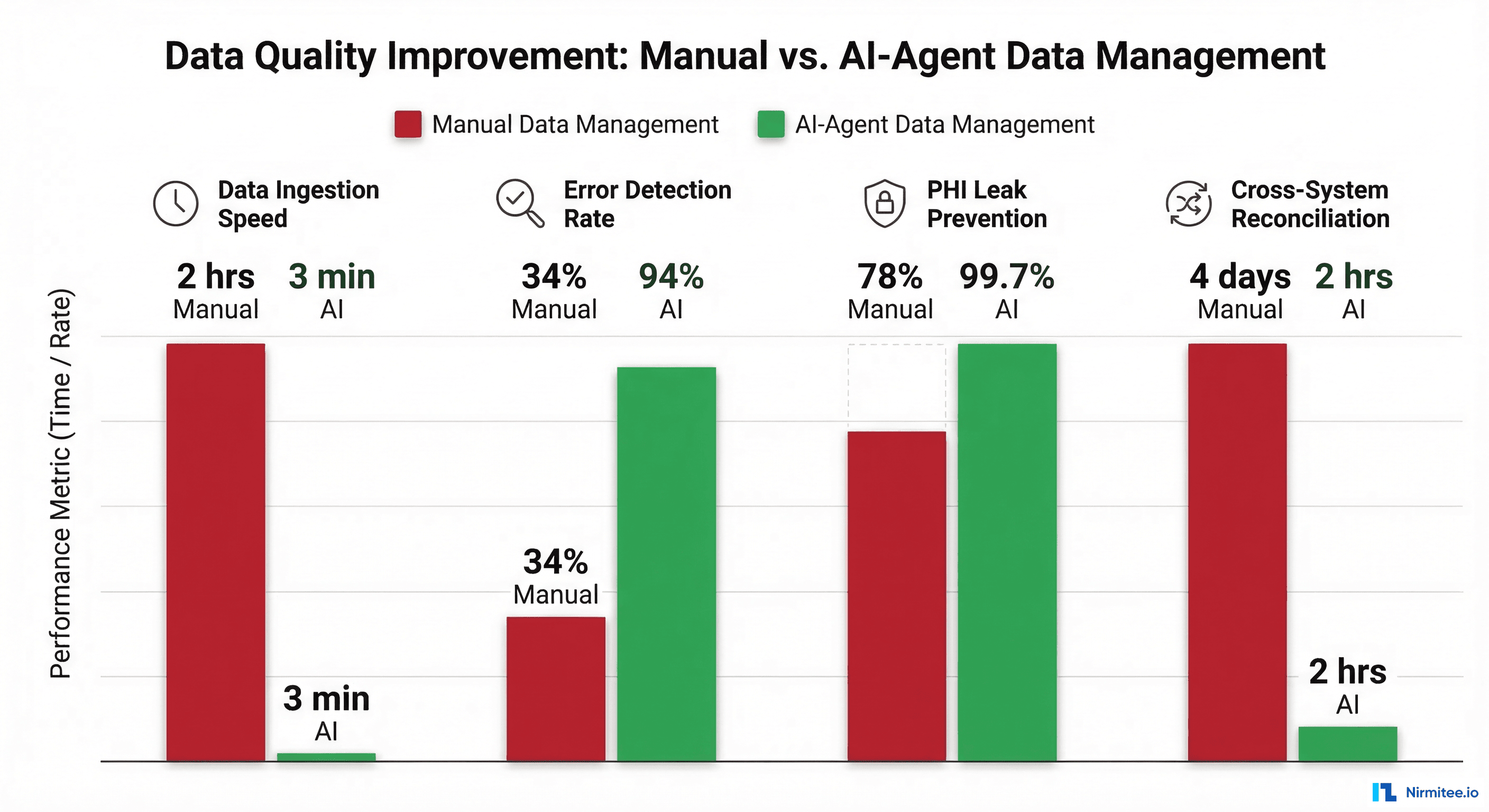
Measurable Impact
| Metric | Manual/Rules-Based | Agent-Augmented | Improvement |
|---|---|---|---|
| Data ingestion (new source onboarding) | 2-4 weeks | 2-3 days | 85% faster |
| Data quality error detection rate | 34% | 94% | 2.8x |
| PHI leak prevention (unintended exposure) | 78% | 99.7% | Near-zero leaks |
| Cross-system reconciliation time | 4 days | 2 hours | 98% faster |
| Integration error queue volume | 1,200/day | 180/day | -85% |
| Data engineer manual intervention | 6 hrs/day | 45 min/day | -88% |
The most significant operational impact is the reduction in integration error queues. Traditional integration engines put non-conforming messages into error queues that require manual review. With 1,200 errors per day, the integration team was perpetually behind. The AI agents resolve 85% of these automatically by applying clinical context to understand and fix data quality issues that rigid validation rules cannot handle.
At Nirmitee, we build healthcare data infrastructure with FHIR-native pipelines, HL7-to-FHIR migration, and AI-augmented data management. If you are drowning in integration errors and data quality issues, talk to our team.
Building interoperable healthcare systems is complex. Our Healthcare Interoperability Solutions team has deep experience shipping production integrations. We also offer specialized Agentic AI for Healthcare services. Talk to our team to get started.