Healthcare organizations lose an estimated $265.6 billion annually to administrative complexity, with revenue cycle inefficiencies accounting for a significant share of that waste. According to HFMA research, hospitals lose an average of 4.8% of net revenue to claim denials alone — tens of millions of dollars annually for large health systems.
The good news: the vast majority of these losses are preventable through automation. A 2026 HFMA survey found that 58% of healthcare practices have adopted or plan to adopt AI and automation in their revenue cycle operations this year, and early adopters are reporting 5:1 ROI from day one.
This guide breaks down the 12 core revenue cycle workflows that are ripe for automation — each with a detailed architecture overview, integration points (FHIR, HL7, EDI), and real ROI data from published research. Unlike surface-level listicles, we go deep into how each automation actually works at the system level.
Whether you are a CIO evaluating automation platforms, a revenue cycle director building a business case, or a health IT architect designing the integration layer, this guide gives you the technical depth and financial data to make informed decisions. We cover every standard you will encounter — EDI X12 (270/271, 278, 835, 837), FHIR R4 resources, HL7 v2 messages, and the CMS-0057-F regulatory requirements that are reshaping prior authorization in 2026 and beyond.
The State of RCM Automation in 2026
The revenue cycle automation landscape has shifted dramatically in the past two years. Three converging forces are driving adoption faster than ever:
Regulatory mandates are forcing digital transformation. The CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F) requires payers to implement FHIR-based prior authorization APIs by January 2027, with faster decision timelines already in effect as of January 2026. This regulatory push creates a standardized API layer that automation platforms can reliably build against, reducing the integration uncertainty that previously slowed adoption.
AI capabilities have matured from experimental to production-ready. Natural language processing for clinical coding, machine learning for denial prediction, and intelligent document processing for prior authorization packet assembly have all moved from pilot programs to scaled deployments. The technology is no longer the bottleneck — organizational readiness is.
The financial pressure is unsustainable. With three billion claims submitted annually in the US and denial rework costs approaching $20 billion industry-wide, manual revenue cycle management is no longer financially viable. Health systems operating with clean claim rates below 90% and denial rates above 10% are leaving millions on the table — money that automated organizations are capturing. The competitive gap between automated and manual revenue cycles is widening every quarter.
Understanding the Revenue Cycle Pipeline
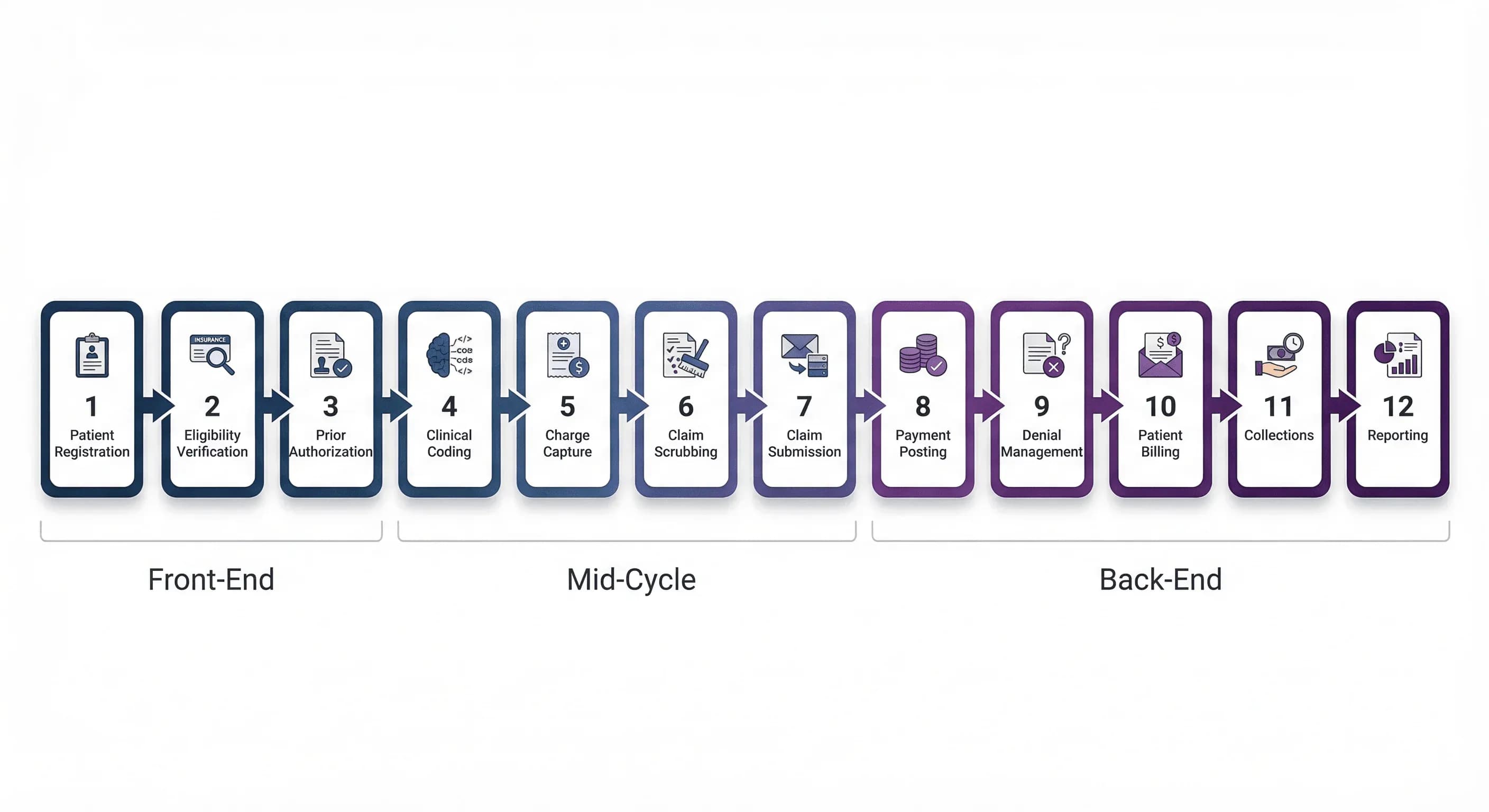
Before diving into individual workflows, it helps to understand the three phases of the revenue cycle:
- Front-End (Workflows 1-3): Patient access, eligibility, and authorization — everything before the clinical encounter
- Mid-Cycle (Workflows 4-7): Clinical coding, charge capture, claim preparation, and submission — translating care into billable claims
- Back-End (Workflows 8-12): Payment processing, denial management, patient billing, collections, and analytics — converting claims into cash
Each phase has distinct automation opportunities, integration requirements, and ROI profiles. Research from HFMA and McKinsey consistently shows that front-end automation delivers the fastest ROI because preventing errors early avoids costly rework downstream. However, back-end automation often delivers the largest absolute dollar recovery because it directly addresses revenue that has already been earned but not collected. The optimal strategy is to automate sequentially, starting with the highest-ROI workflows in each phase.
Let's examine all twelve workflows in detail, with the architecture, integration specifications, and financial data you need to build your automation roadmap.
1. Patient Registration and Eligibility Verification
The Problem
Manual patient registration is error-prone, with 71% of healthcare organizations identifying real-time insurance verification as their primary daily challenge. Incorrect demographics, expired insurance cards, and manual data entry errors cascade downstream, causing claim denials that cost $25-$35 per rework.
Architecture Overview
An automated registration and eligibility system connects the EHR's patient intake module to payer systems through the EDI 270/271 transaction standard. Here is how the data flows:
- Patient Check-In Trigger: When a patient arrives or schedules an appointment, the system automatically extracts demographics and insurance information from the EHR
- 270 Eligibility Request: The system generates an ANSI X12 270 eligibility inquiry and routes it to the appropriate payer through a clearinghouse or direct connection
- 271 Eligibility Response: The payer returns a 271 response containing coverage status, co-pay amounts, deductible information, and benefit details
- Coverage Parsing and Display: The automation engine parses the 271 response and presents a structured benefits summary to registration staff in real-time
Integration Points
- EDI 270/271: Standard eligibility inquiry/response transactions
- FHIR R4 Coverage Resource: Modern API-based eligibility queries using the
Coverage/$validateoperation - HL7 ADT Messages: Patient admission, discharge, and transfer events trigger automated re-verification
ROI Data
Organizations implementing real-time eligibility verification report a 20% reduction in eligibility-related denials and a 10x increase in processing speed compared to manual verification. FHIR-based workflows specifically are reducing eligibility-related denials by 30-40%. At scale, a 500-bed hospital processing 200,000 claims annually can save $1.2-1.8 million per year in avoided rework and accelerated collections through automated eligibility alone.
2. Insurance Verification and Benefits Discovery
The Problem
Even after confirming active coverage, staff must determine specific benefit details: deductibles met, out-of-pocket maximums, in-network status, and service-specific coverage limits. This often requires manual calls to payers, with average hold times of 15-20 minutes per call.
Architecture Overview
Automated benefits discovery extends the eligibility check into a comprehensive coverage analysis:
- Multi-Payer Lookup: The system queries multiple payers simultaneously when a patient has coordination of benefits (primary, secondary, tertiary)
- Coverage Parsing Engine: Structured parsing of 271 service-type segments extracts procedure-specific benefits including copay, coinsurance, prior auth requirements, and visit limits
- Financial Estimation: Combining parsed benefits with scheduled procedure codes (CPT/HCPCS) to generate patient responsibility estimates before the visit
- Automated Alerts: Flagging authorization requirements, out-of-network situations, or coverage gaps before the patient arrives
Integration Points
- FHIR ExplanationOfBenefit: The
ExplanationOfBenefitresource provides standardized benefit information through the CMS Patient Access API - X12 278: Authorization requirements discovered during benefits check feed directly into prior authorization workflows
- Real-Time Pharmacy Benefit (RTPB): For medication-related services, integration with pharmacy benefit managers through NCPDP standards
ROI Data
Automated benefits discovery reduces front-desk call volume by 60-70% and improves patient financial estimates accuracy from roughly 50% to over 90%, significantly reducing patient billing surprises and improving collections. The downstream impact is substantial: accurate pre-visit estimates reduce patient complaints by 40% and increase point-of-service collections by 25-30%, because patients are prepared for their financial responsibility before they arrive.
3. Prior Authorization Automation
The Problem
Prior authorization is the single most labor-intensive administrative task in healthcare. The average authorization requires 12 minutes of staff time, with complex cases taking hours. One health system reported spending 2,841 staff hours annually on prior auth alone. The CMS estimates $15 billion in savings over 10 years as prior authorization goes digital.
Architecture Overview
Modern prior authorization automation leverages the CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F), which mandates FHIR-based APIs by January 2027:
- Clinical Data Extraction: NLP engines extract relevant clinical information from physician notes, lab results, and imaging reports
- Packet Assembly: AI assembles the prior authorization request with all required clinical documentation, matching payer-specific requirements
- FHIR Da Vinci PAS Submission: The system submits the request through the
Claim/$submitoperation using the Da Vinci Prior Authorization Support (PAS) Implementation Guide - Status Tracking: Automated polling or webhook-based notifications track the authorization through approval, denial, or pend states
- Appeal Generation: For denied requests, the system auto-generates appeal letters incorporating additional clinical evidence
Integration Points
- Da Vinci PAS (Prior Authorization Support): FHIR-based prior auth submission and status checking
- X12 278: Legacy EDI-based authorization request/response for payers not yet supporting FHIR
- CMS-0057-F Compliance: Beginning January 2026, payers must respond to urgent requests within 72 hours and standard requests within 7 calendar days
ROI Data
One health system achieved an 83% clean submission rate for prior authorizations and reduced authorization turnaround times by 80%, saving $644,000 in avoided write-offs annually. Organizations automating prior auth report a 60% reduction in staff time per authorization. The regulatory trajectory is clear: CMS expects prior authorization to become fully electronic and API-driven by 2027, meaning organizations that invest in FHIR-based PA automation now will be positioned for compliance while their competitors scramble to adapt. The key technical consideration is ensuring your PA automation supports both the Da Vinci PAS FHIR API (for payers already compliant) and legacy X12 278 transactions (for the transition period).
4. AI-Assisted Clinical Coding
The Problem
Clinical coding — translating patient encounters into ICD-10-CM diagnosis codes and CPT/HCPCS procedure codes — is a specialized, labor-intensive process. Certified coders are in short supply, and even experienced coders achieve only 85-90% first-pass accuracy. Coding errors directly cause denials, underpayment, and compliance risk.
Architecture Overview
AI-assisted coding systems use NLP and machine learning to suggest codes from clinical documentation:
- Document Ingestion: Clinical notes, operative reports, pathology results, and radiology reports are ingested from the EHR
- Medical NLP Processing: Specialized NLP models extract clinical entities — diagnoses, procedures, laterality, severity — from unstructured text
- Code Suggestion Engine: Extracted entities are mapped to appropriate ICD-10-CM, CPT, and HCPCS codes with confidence scores
- Compliance Validation: Suggested codes are checked against NCCI bundling edits, LCD/NCD medical necessity requirements, and modifier rules
- Human-in-the-Loop Review: High-confidence codes (above 95%) can be auto-accepted; lower-confidence suggestions are routed to certified coders for review
Integration Points
- FHIR Claim Resource: Coded encounters populate the
Claim.diagnosisandClaim.procedureelements - ICD-10-CM/PCS API: Real-time code lookup and validation against the current CMS code sets
- HL7 DFT (Detailed Financial Transaction): Coded charges transmitted from coding system to billing
ROI Data
AI-assisted coding improves first-pass accuracy to 95-97%, reduces coding turnaround time by 40-50%, and captures an estimated $1.5 million in additional annual revenue per 10,000 discharges through reduced under-coding. The compliance benefits are equally significant: AI coding systems maintain audit-ready documentation trails, flag potential upcoding risks before submission, and ensure consistent application of coding guidelines across all providers. Organizations using AI-assisted coding report a 70% reduction in external audit findings related to coding accuracy.
5. Charge Capture Automation
The Problem
Revenue leakage from missed charges is one of healthcare's most persistent problems. Studies estimate that 1-5% of net revenue is lost to missed charge capture, often because physicians forget to document billable services or charges fail to flow from clinical systems to billing.
Architecture Overview
- Clinical Activity Monitoring: The system monitors EHR activity — orders placed, procedures documented, medications administered — and compares against expected charges
- Charge Description Master (CDM) Validation: Each captured charge is validated against the facility's CDM for correct pricing, code mapping, and revenue code assignment
- Gap Detection: AI compares documented clinical activities against submitted charges to identify unbilled services
- Automated Alerts: Missing charges trigger real-time alerts to the responsible provider or department for review
Integration Points
- HL7 DFT/P03: Charge posting transactions from ancillary systems (lab, radiology, pharmacy)
- FHIR ChargeItem: Modern charge capture using the
ChargeItemresource with references to the originating encounter and procedure - CDM Integration: Bi-directional sync between the charge master and coding systems for accurate pricing
ROI Data
Automated charge capture recovers an estimated 2-3% of previously lost revenue. For a health system with $500 million in net patient revenue, that represents $10-15 million annually. The most effective charge capture systems go beyond simple alerts: they use historical patterns to predict which types of encounters are most likely to have missed charges. For example, the system might learn that orthopedic surgeries with fluoroscopy guidance frequently miss the fluoroscopy charge, or that E&M visits with in-office procedures often fail to capture the supply codes. This predictive approach catches revenue leakage that simple rules-based systems miss entirely.
6. Claim Scrubbing and Validation
The Problem
Claims submitted with errors are denied, returned, or underpaid. The average clean claim rate in healthcare is approximately 82%, meaning nearly 1 in 5 claims requires rework. Each denied claim costs $25-$35 to rework for commercial payers and up to $47.77 for Medicare Advantage.
Architecture Overview
Automated claim scrubbing applies hundreds of validation rules before a claim is submitted:
- Demographic Validation: Verifying patient information matches payer records (name, DOB, subscriber ID formatting)
- Coding Edits: Checking for NCCI bundling conflicts, code-to-code edits, modifier requirements, and age/gender specificity
- Medical Necessity: Validating that diagnosis codes support the procedures billed, using LCD/NCD rules
- Payer-Specific Rules: Applying payer-specific billing requirements, timely filing limits, and authorization matching
- Error Correction: For common errors, automatically correcting and flagging for review rather than simply rejecting
Integration Points
- EDI 837P/837I: Professional and institutional claim formats validated against ANSI X12 standards
- FHIR Claim/$validate: Pre-submission validation using FHIR-based payer APIs
- Clearinghouse APIs: Direct integration with clearinghouses for real-time edit checking before submission
ROI Data
Automated claim scrubbing can increase clean claim rates from 82% to 97-98%, preventing 85% of avoidable denials. For a system submitting 100,000 claims annually, this eliminates approximately 15,000 rework cycles, saving over $500,000 per year. The most sophisticated scrubbing engines also apply payer-specific contract terms: they know that Payer A requires modifier 25 on E&M services billed with minor procedures, while Payer B bundles those same services. This payer-specific intelligence is what separates advanced scrubbing from basic edit checking, and it is the primary driver of the 97%+ clean claim rates that leading organizations achieve.
7. Claim Submission and Tracking
The Problem
Even clean claims can fail at submission due to incorrect routing, clearinghouse outages, or payer system rejections. Without real-time tracking, rejected claims can sit unworked for days or weeks, risking timely filing limits.
Architecture Overview
- EDI 837 Generation: The billing system generates properly formatted 837P (professional) or 837I (institutional) claim files
- Intelligent Routing: Claims are routed to the correct clearinghouse or direct payer connection based on payer ID, line of business, and claim type
- Submission Monitoring: Real-time tracking of claim acceptance through 999 acknowledgments and 277CA status responses
- Rejection Handling: Rejected claims are auto-analyzed, corrected when possible, and resubmitted without manual intervention
Integration Points
- EDI 837/999/277: Claim submission, acknowledgment, and status notification transactions
- FHIR Claim/$submit: For payers supporting FHIR-based claim submission
- Direct Data Entry (DDE): Automated portal submission for payers without EDI capability
ROI Data
Automated submission and tracking reduces the average claim lifecycle from 45 days to 21 days and decreases the rate of claims lost to timely filing limits by 90%. The critical capability here is real-time visibility: when a claim is rejected at the clearinghouse level (a 999 acknowledgment with errors), the automation system should immediately reroute it for correction rather than letting it sit in a queue. Many organizations discover that 5-8% of their claims are rejected at the clearinghouse but not worked for days because staff check rejection reports only periodically. Real-time rejection handling closes this gap completely.
8. Payment Posting and Reconciliation
The Problem
Payment posting — matching incoming payments to their corresponding claims — is one of the highest-volume back-office tasks. A mid-size hospital processes thousands of ERA (Electronic Remittance Advice) transactions daily, each containing multiple claim-level payment details that must be reconciled.
Architecture Overview
- ERA/835 Ingestion: Electronic remittance files (EDI 835) are received from payers and clearinghouses
- Auto-Matching: Payments are matched to open accounts receivable using claim number, patient ID, and service dates
- Variance Detection: The system identifies underpayments, overpayments, and contractual adjustments by comparing expected payment (from fee schedules and contracts) against actual payment
- Automated Posting: Matched payments with no variances are automatically posted to the patient account. Variances are flagged for review
- Bank Reconciliation: ERA payments are reconciled against bank deposits (EFT) to ensure completeness
Integration Points
- EDI 835: Electronic remittance advice for automated payment detail delivery
- FHIR PaymentReconciliation: Modern payment posting using the
PaymentReconciliationresource - EFT/ACH: Electronic fund transfer integration for bank deposit matching
ROI Data
Automated payment posting handles 80-85% of ERA transactions without human intervention, reducing posting staff requirements by 60-70%. Mayo Clinic reported saving 30 FTE positions and $700,000 in vendor costs through AI-powered revenue cycle automation including payment posting. A critical feature of advanced payment posting automation is contract variance detection: the system compares each payment against the expected reimbursement from payer contracts and fee schedules. When a payer consistently underpays a specific procedure code by even 2-3%, the automation flags this pattern for contract negotiation — revenue that would otherwise go unnoticed for months or years. Organizations implementing contract variance detection recover an additional 1-2% of net revenue through identification of systematic underpayments.
9. Denial Management and Appeals
The Problem
Denial rates continue climbing industry-wide, with many organizations experiencing initial denial rates of 10-15%. The average cost to rework a commercial denial is $63.76, and the total administrative cost of denial rework across the industry has reached nearly $20 billion annually. As payers increasingly use AI to drive denials higher, providers must fight back with automation.
Architecture Overview
Modern denial management systems use AI to classify, prioritize, and resolve denials:
- Denial Ingestion: Denials are captured from ERA 835 CARC/RARC codes, payer portal scraping, and manual entry
- Auto-Classification: Machine learning models categorize denials by type (clinical, technical, administrative), root cause, and payer
- Prioritization: AI scores each denial by recovery probability, dollar amount, and filing deadline to create optimized worklists
- Appeal Generation: For common denial categories, the system auto-generates appeal letters incorporating relevant clinical documentation, regulatory citations, and contractual references
- Trend Analysis: Pattern detection across denied claims identifies systemic issues — such as a specific procedure code consistently denied by a particular payer — for upstream process improvement
Integration Points
- EDI 835 CARC/RARC: Claim Adjustment Reason Codes and Remittance Advice Remark Codes for denial classification
- FHIR ClaimResponse: Adjudication details including denial reasons and appeal instructions
- Payer Portal APIs: Automated appeal submission through payer-specific portal integrations
ROI Data
AI-powered denial management can auto-appeal 40% of denials, improve recovery rates to 65%, and reduce days-to-resolution from 12 days to 5 days. HFMA data shows that data-driven denial prevention can recover up to $10 million per $1 billion in patient revenue. The most impactful aspect of AI-driven denial management is the feedback loop: every denied claim becomes training data that improves upstream processes. If the system detects that 30% of MRI denials from a specific payer are due to missing clinical documentation, it automatically triggers enhanced documentation requirements in the prior authorization workflow for that payer-procedure combination. This closed-loop approach transforms denial management from a reactive cost center into a proactive revenue protection system, and it is why organizations with mature denial AI consistently see their denial rates decline year-over-year even as industry averages climb.
10. Patient Billing and Financial Experience
The Problem
Patient responsibility now accounts for 30% or more of hospital revenue, yet patient collections rates hover around 50-60%. Confusing bills, delayed statements, and lack of payment options drive both bad debt and patient dissatisfaction.
Architecture Overview
- Consolidated Statement Generation: Automation combines multiple encounters and payer payments into a single, clear patient statement
- Multi-Channel Delivery: Statements are delivered through the patient's preferred channel — print, email, patient portal, SMS, or mobile app
- Payment Plan Engine: AI-driven financial counseling tools assess patient financial capacity and offer appropriate payment plans, charity care, or Medicaid eligibility screening
- Self-Service Portal: Patients can view bills, make payments, set up payment plans, and request financial assistance through a digital portal
Integration Points
- FHIR Patient and Account: Patient financial data accessible through standard FHIR APIs
- Payment Gateway APIs: Integration with payment processors for credit card, ACH, and digital wallet payments
- CMS Price Transparency: Machine-readable files and patient-facing price estimator tools
ROI Data
Digital-first patient billing increases collection rates by 15-25% and reduces statement costs by 40-60% compared to paper-only billing. Organizations offering payment plans collect 2-3x more in patient responsibility than those without. The patient experience dimension is increasingly important as consumer satisfaction scores influence hospital reimbursement through value-based programs. A seamless digital billing experience — where patients receive a clear statement, can ask questions through chat, and pay through their preferred method — directly improves HCAHPS scores in the discharge information domain. Leading organizations are moving beyond traditional patient statements to proactive financial navigation, where AI identifies patients who may qualify for financial assistance programs and automatically connects them to resources before the bill becomes a collections issue.
11. Collections Optimization with AI
The Problem
Traditional collections follow a one-size-fits-all approach: send a series of increasingly urgent letters, then write off or send to external collections. This approach is both ineffective (low recovery rates) and harmful to patient relationships.
Architecture Overview
- Payment Propensity Scoring: Machine learning models score each account based on likelihood of payment, incorporating demographics, payment history, insurance type, and balance amount
- Segmented Outreach: AI determines the optimal outreach strategy for each segment — digital nudges for high-propensity accounts, financial counseling for mid-tier, and early write-off for accounts with near-zero recovery probability
- Optimal Timing: Analytics determine the best day, time, and channel for each outreach attempt based on historical response patterns
- Automated Workflows: SMS reminders, email follow-ups, and portal notifications are triggered automatically based on the AI-determined schedule
Integration Points
- FHIR Account Resource: Standardized patient account balance and payment history data
- Communication APIs: Twilio/SMS, email, and push notification integrations for multi-channel outreach
- External Collections Integration: Automated handoff to collection agencies with full account documentation when internal efforts are exhausted
ROI Data
AI-prioritized collections improve patient payment recovery by 20-35% compared to traditional methods, while reducing outreach costs by 45% through elimination of low-value contact attempts. Early financial counseling referrals reduce bad debt write-offs by 15-20%. An advanced capability gaining traction in 2026 is behavioral scoring combined with empathetic outreach design: the AI not only determines when and how to contact a patient, but also tailors the message tone and content based on the patient's financial situation. Patients with high balances from emergency visits receive empathetic language with prominent financial assistance options, while patients with small balances from routine visits receive a simple payment reminder. This nuanced approach improves both recovery rates and patient satisfaction simultaneously, avoiding the adversarial dynamic that traditional collections creates.
12. Reporting, Analytics, and KPI Dashboards
The Problem
Most revenue cycle teams operate on 30-60 day old data, making it impossible to identify and respond to emerging problems before they become financial crises. Monthly reporting cycles mean denial spikes, coding bottlenecks, or payer behavior changes go undetected for weeks.
Architecture Overview
- Real-Time Data Pipeline: Events from across the revenue cycle — registration, coding, claim submission, payment, denials — flow into a centralized analytics engine in real-time
- KPI Calculation Engine: Automated calculation of core revenue cycle KPIs including Days in AR, Clean Claim Rate, Denial Rate, Net Collection Rate, Cost to Collect, and Cash as a Percentage of Net Revenue
- Predictive Analytics: Machine learning models forecast cash collections, identify at-risk accounts, and predict denial probability for pending claims
- Drill-Down Dashboards: Interactive visualizations allow revenue cycle leaders to drill from system-wide KPIs down to individual payer, department, or provider-level performance
Integration Points
- FHIR Bulk Data Export:
$exportoperations for extracting large datasets for analytics processing - HL7 ADT/DFT/SIU: Real-time event feeds from clinical and financial systems
- BI Tool APIs: Integration with Tableau, Power BI, or custom dashboards for visualization
ROI Data
Organizations with real-time revenue cycle analytics reduce Days in AR by 8-12 days, improve net collection rates by 2-4 percentage points, and identify revenue recovery opportunities worth $2-5 million annually that would have been missed with retrospective reporting. The most transformative analytics capability is predictive denial modeling: before a claim is even submitted, the system scores its probability of denial based on historical patterns for that payer, procedure, provider, and patient combination. Claims flagged as high-denial-risk can be reviewed, strengthened with additional documentation, or routed through enhanced scrubbing before submission. Organizations implementing pre-submission denial prediction report a 25-30% reduction in initial denial rates within the first year. Combined with the traditional reporting KPIs, this predictive layer turns the analytics function from a backward-looking scorecard into a forward-looking revenue protection system.
Implementation Strategy: Where to Start
You do not need to automate all 12 workflows simultaneously. The highest-impact starting points, ranked by typical ROI and implementation speed:
- Eligibility Verification (Workflow 1-2): Fastest to implement, immediate denial reduction, minimal clinical workflow disruption
- Claim Scrubbing (Workflow 6): High ROI, rule-based automation is mature and reliable
- Payment Posting (Workflow 8): High volume, well-defined rules, rapid payback
- Denial Management (Workflow 9): Significant financial recovery, AI models improve over time
- Prior Authorization (Workflow 3): High staff time savings, regulatory tailwinds from CMS-0057-F
For most organizations, implementing workflows 1-2 and 6-8 delivers 80% of available automation value with 20% of total implementation effort.
A critical success factor that many organizations overlook is change management. Automation changes how revenue cycle staff work, and resistance is natural. The most successful implementations start with a clear communication plan: automation is not about eliminating jobs, but about eliminating the most tedious, repetitive parts of jobs so that skilled staff can focus on higher-value activities like payer negotiation, complex case resolution, and process improvement. Organizations that invest in training and communicate the "why" behind automation consistently report higher adoption rates and faster ROI realization than those that simply deploy technology and expect compliance.
The Integration Architecture: Making It All Work Together
Individual workflow automation delivers value, but the real transformation happens when workflows are connected. The key architectural principles:
- Event-Driven Architecture: Each workflow publishes events (patient registered, claim submitted, payment posted) that downstream workflows subscribe to, eliminating batch processing delays
- FHIR as the Integration Backbone: Using FHIR R4 resources as the common data model across workflows ensures interoperability and future-proofs against vendor changes. Learn more about US payer integration standards including EDI and FHIR
- Human-in-the-Loop Design: Every automated workflow should include exception handling that routes complex cases to human experts, with the AI handling routine cases. This is the foundation of agentic AI in revenue cycle management
- Continuous Learning: Machine learning models in coding, denial management, and collections should improve over time based on outcomes data
The goal is not to replace revenue cycle staff, but to redirect their expertise from routine processing to exception handling, payer negotiation, and strategic improvement. Organizations that take this approach report higher staff satisfaction alongside improved financial performance.
Technology Stack Considerations
When building or selecting an RCM automation platform, the technology stack matters significantly for long-term success. Key architectural decisions include:
- Integration Engine: Choose a platform that natively supports EDI X12 (for legacy payer connections), FHIR R4 (for modern interoperability), and HL7 v2 (for EHR integration). Avoid platforms that support only one standard — the healthcare ecosystem requires all three for comprehensive coverage
- Rules Engine: Claim scrubbing and eligibility validation require a rules engine that can be updated without code changes. Payer requirements change frequently, and the ability to add new validation rules in days rather than weeks is a competitive advantage
- Machine Learning Infrastructure: For AI-powered workflows (coding, denial prediction, collections scoring), the platform needs model training, versioning, and monitoring capabilities. Models that are never retrained on your organization's data will underperform over time
- Workflow Orchestration: An event-driven architecture with message queuing (Apache Kafka, RabbitMQ, or cloud-native equivalents) ensures that workflows are decoupled, scalable, and resilient. When the payment posting service is processing a high-volume ERA file, the claim submission service should not be affected
- Security and Compliance: HIPAA compliance is non-negotiable. The platform must encrypt data at rest and in transit, implement role-based access control, maintain comprehensive audit logs, and support BAA agreements with all cloud service providers
If you are evaluating revenue cycle automation for your organization, explore our approach to custom RCM software development — built on FHIR-native architecture with the integration depth described in this guide.
Frequently Asked Questions
What is the typical ROI timeline for revenue cycle automation?
Most organizations see measurable ROI within 3-6 months for rule-based automation (eligibility, claim scrubbing, payment posting). AI-powered workflows like clinical coding and denial management typically reach full ROI within 9-12 months as models train on organization-specific data. Early adopters report a 5:1 ROI ratio from day one for high-volume workflows like eligibility verification.
Do we need to replace our existing EHR to implement RCM automation?
No. Modern RCM automation platforms are designed to integrate with existing EHR systems through standard interfaces — HL7 v2 messages, FHIR APIs, EDI transactions, and database-level integration. The key is choosing an automation platform that supports your EHR's available integration methods. Most workflows can be automated without modifying EHR core functionality.
How does CMS-0057-F impact prior authorization automation?
The CMS Interoperability and Prior Authorization Final Rule (CMS-0057-F) requires impacted payers to support FHIR-based prior authorization APIs by January 1, 2027. As of January 2026, faster decision timelines are already in effect: 72 hours for urgent requests and 7 calendar days for standard requests. This creates a regulatory tailwind for automation — payers must accept electronic submissions and respond within defined timeframes, making automation more reliable and predictable.
What percentage of revenue cycle workflows can be fully automated without human oversight?
For straightforward, rule-based workflows (eligibility verification, payment posting, claim scrubbing), 80-85% of transactions can be processed without human intervention. For AI-dependent workflows (clinical coding, denial management), the fully automated rate is typically 50-65%, with the remainder requiring human review. The industry consensus is that a human-in-the-loop model produces the best outcomes — AI handles volume, humans handle complexity.
What are the key metrics to track when measuring RCM automation success?
The five most important metrics are: Clean Claim Rate (target: 97%+), Days in Accounts Receivable (target: under 35 days), Denial Rate (target: under 5%), Cost to Collect (target: under 3% of net revenue), and Net Collection Rate (target: 96%+). Additionally, track staff productivity (claims processed per FTE) and patient satisfaction with the billing experience. Real-time dashboards monitoring these KPIs are essential for measuring automation impact. Beyond these core metrics, track automation coverage rate — the percentage of total transactions handled end-to-end by automation without human intervention. This metric, often called the "touchless rate," is the single best indicator of automation maturity. Leading organizations target 75%+ touchless rate for rule-based workflows and 50%+ for AI-dependent workflows within 18 months of deployment. Finally, measure exception resolution time — how quickly human staff resolve the cases that automation routes to them. Automation should make human work faster, not just less frequent.