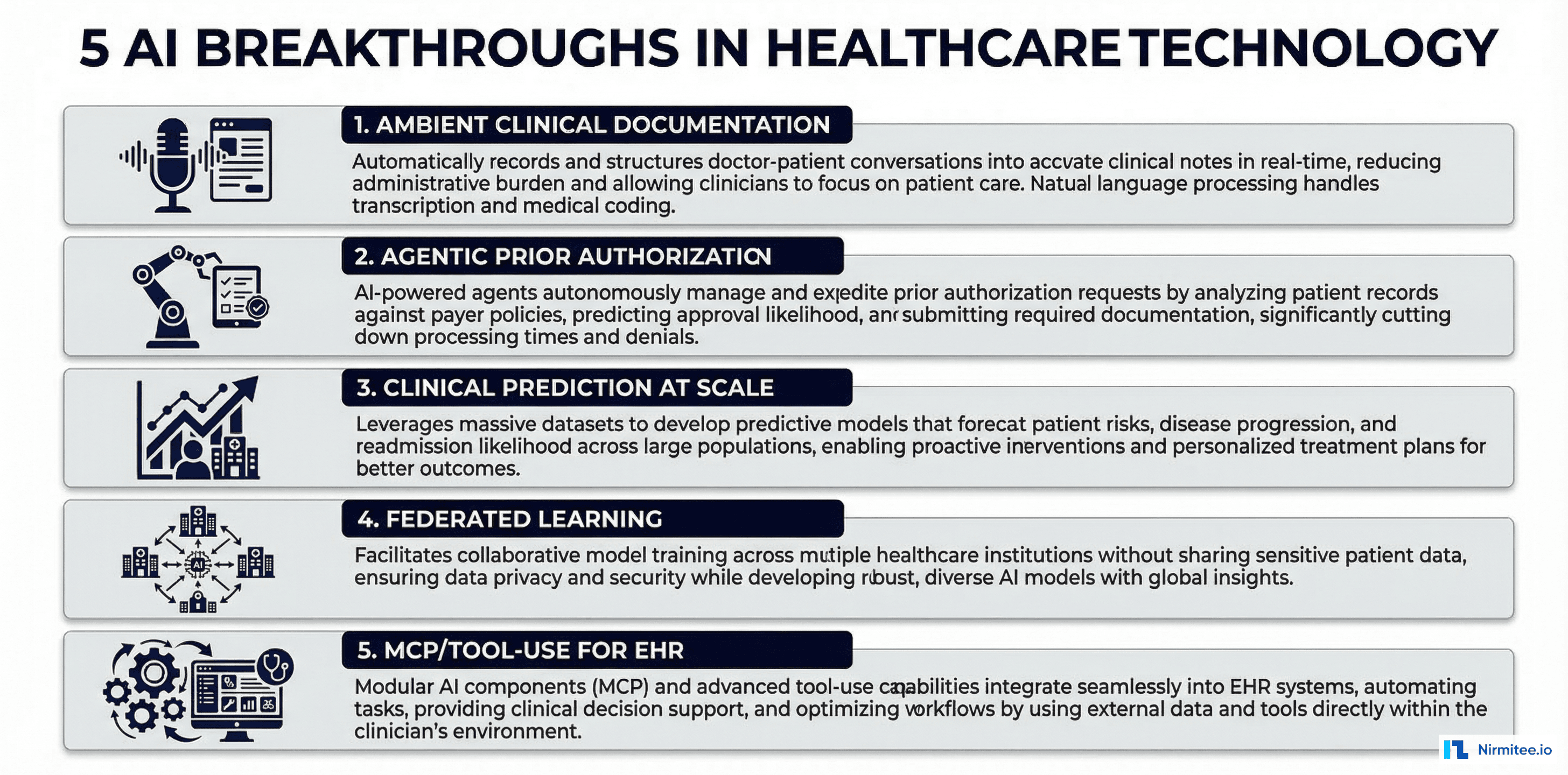
Five AI Breakthroughs That Are Reshaping Healthtech in 2026
The healthcare AI market will reach $45.2 billion by 2030, according to Grand View Research. But the real story is not the market size — it is the five specific breakthroughs that moved from research papers to production systems in 2025 and are now transforming how healthcare organizations operate.
These are not incremental improvements. Each breakthrough represents a fundamental shift in what AI can do inside clinical workflows. This article covers the technology, the companies shipping it, and the numbers that prove it works.

1. Ambient Clinical Documentation: The End of After-Hours Charting
Physician burnout is a measurable crisis. The AMA reports that physicians spend an average of 15.6 hours per week on documentation — nearly two full workdays. Ambient clinical documentation uses AI to listen to patient-clinician conversations in real time and generate structured clinical notes automatically.
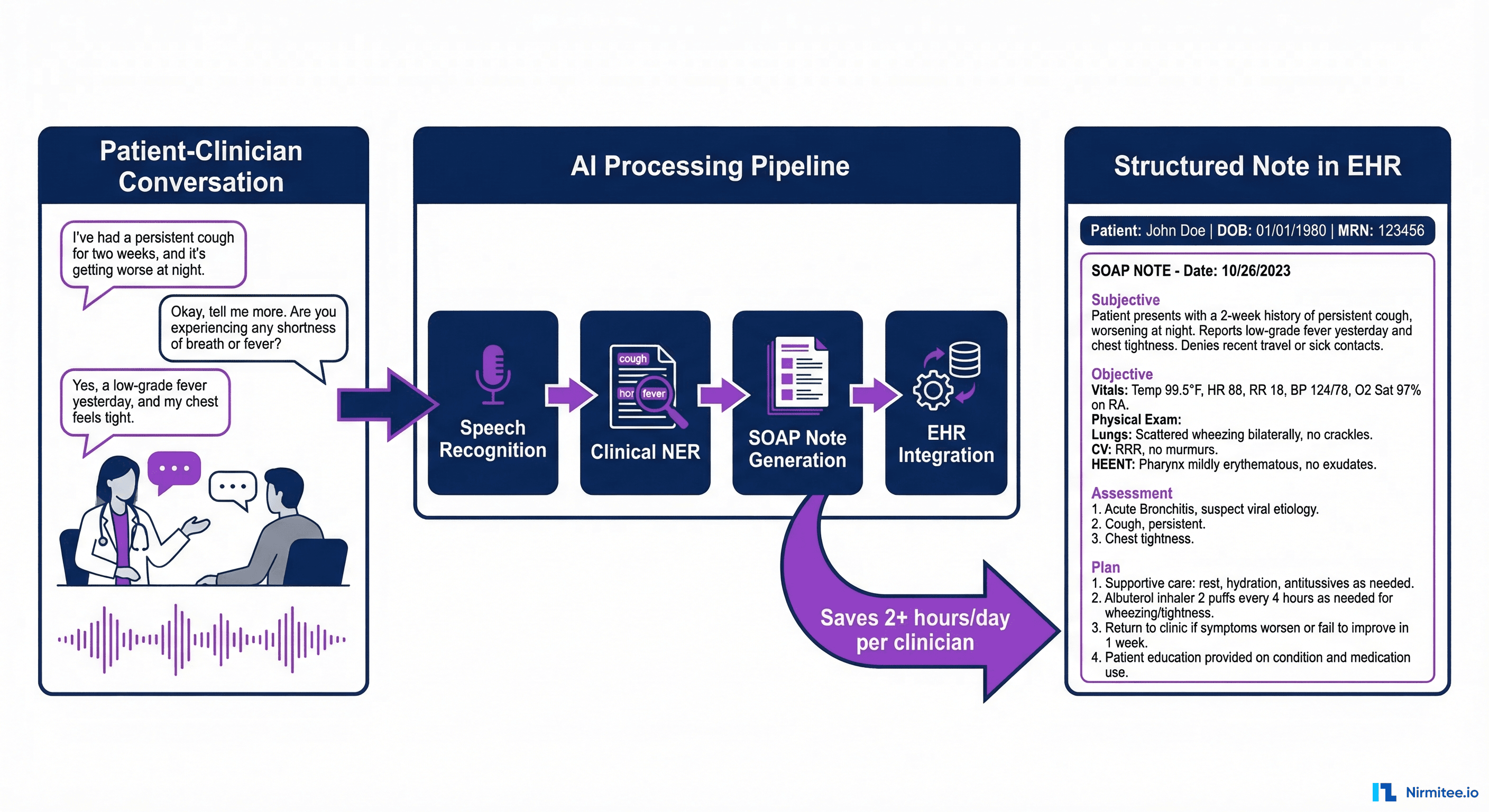
How It Works in Production
The technology stack behind ambient documentation has three layers:
- Speech recognition — Specialized medical ASR (Automatic Speech Recognition) models trained on clinical conversations. These are not general-purpose transcription tools. They handle medical terminology, medication names, and multi-speaker dialogue. Models from Nuance (Microsoft) and Abridge achieve 95%+ word error rate accuracy on clinical speech.
- Clinical NLP extraction — Named entity recognition pulls out diagnoses, medications, procedures, allergies, and assessment data from the transcript. The system maps extracted entities to standard terminologies: ICD-10 for diagnoses, RxNorm for medications, SNOMED CT for clinical findings.
- SOAP note generation — A large language model synthesizes the extracted information into a structured SOAP note (Subjective, Objective, Assessment, Plan) formatted for the specific EHR system. The note is presented to the clinician for review and one-click approval.
Companies and Numbers
| Company | Product | Key Metric | EHR Integration |
|---|---|---|---|
| Nuance/Microsoft | DAX Copilot | 70% reduction in documentation time | Epic, Oracle Health |
| Abridge | Abridge for Clinicians | 2.5 hours saved per clinician per day | Epic (integrated into MyChart) |
| Nabla | Nabla Copilot | 3x faster note completion | FHIR-based, multi-EHR |
| Suki | Suki Assistant | 72% reduction in note time | Epic, Oracle Health, athenahealth |
At Nirmitee, we have built ambient documentation pipelines that integrate with EHR systems via FHIR DocumentReference resources. The critical engineering challenge is not the AI model — it is the EHR integration layer that maps generated notes into the correct chart sections.
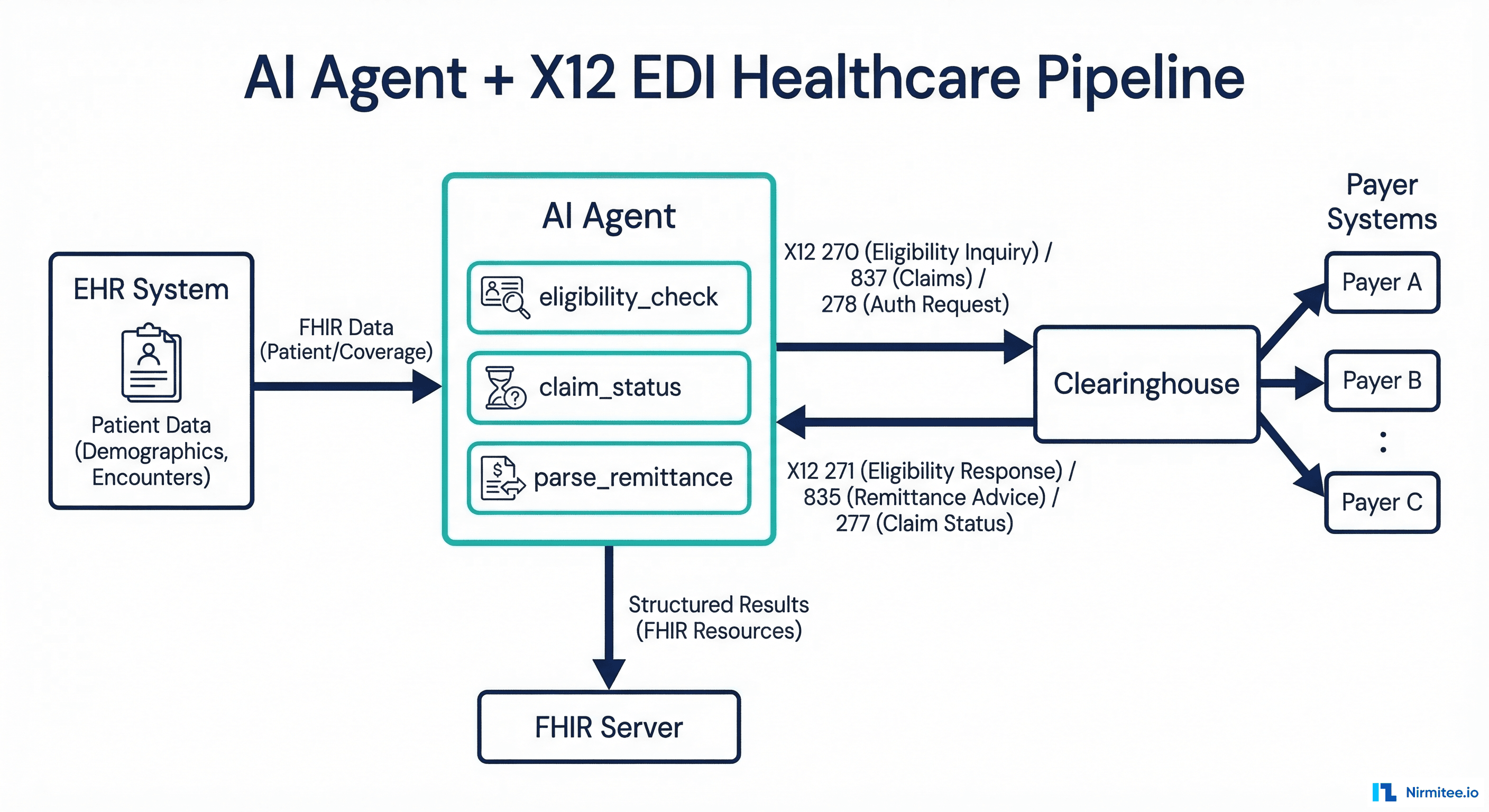
2. Agentic Prior Authorization: From 14 Days to 30 Seconds
Prior authorization is the most wasteful process in healthcare administration. According to AMA survey data, practices complete an average of 45 prior auth requests per physician per week, each taking 20+ minutes of staff time. A full 93% of physicians report care delays due to prior auth.
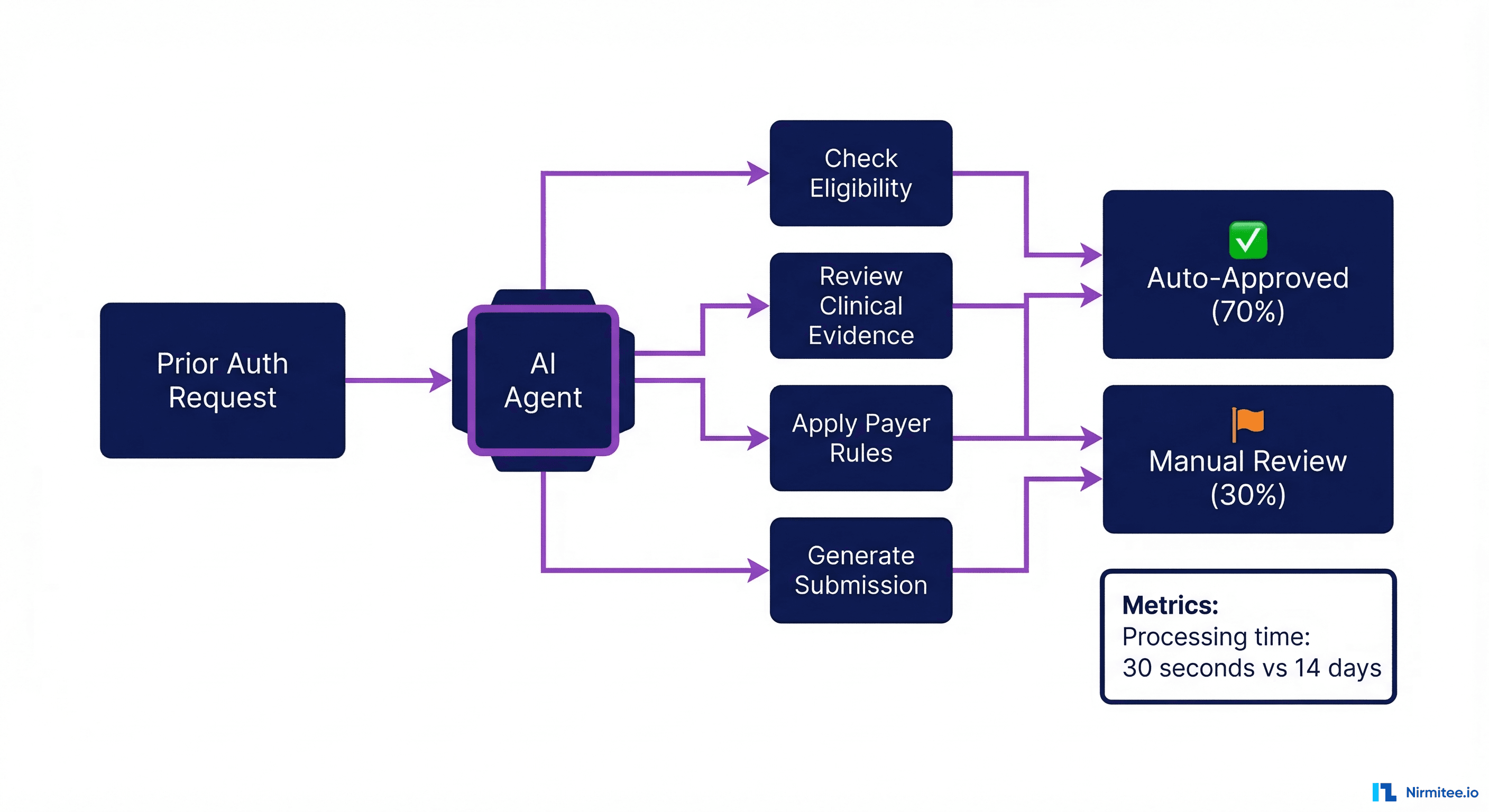
What Makes This Agentic
Traditional RPA (robotic process automation) scripts followed hard-coded rules to fill forms. Agentic AI prior authorization systems reason about the clinical context, select the right evidence from the patient record, and adapt to payer-specific requirements without manual configuration.
The agentic workflow:
- Trigger — A medication order or procedure request fires an event in the EHR. The AI agent receives the FHIR ServiceRequest.
- Evidence gathering — The agent queries the patient record for relevant diagnoses, lab results, imaging, prior treatments, and medication history. It uses FHIR search to pull Condition, Observation, and MedicationRequest resources.
- Rule matching — The agent retrieves the payer's clinical criteria for the requested service. For Medicare, this means matching against LCD/NCD policies. For commercial payers, the agent pulls criteria from the payer's API (where available) or from a maintained rules database.
- Decision — If the clinical evidence meets the payer criteria, the agent auto-approves and submits electronically. If evidence is insufficient, the agent identifies the specific gaps and requests them from the care team.
- Submission — The agent generates the prior auth submission in the payer's required format (often X12 278 or a custom portal submission) and tracks the response.
Production Results
- Cohere Health — Processes 20M+ prior auth decisions per year. Their AI platform reduced average decision time from 14 days to under 30 seconds for auto-eligible cases. 70% of requests are auto-approved without human review.
- Olive AI — Before its 2023 restructuring, it achieved 85% accuracy in predicting prior auth outcomes. The technology is now deployed through multiple successor companies.
- Waystar — Their authorization management platform reduced denials by 30% and cut staff time per request by 75%.
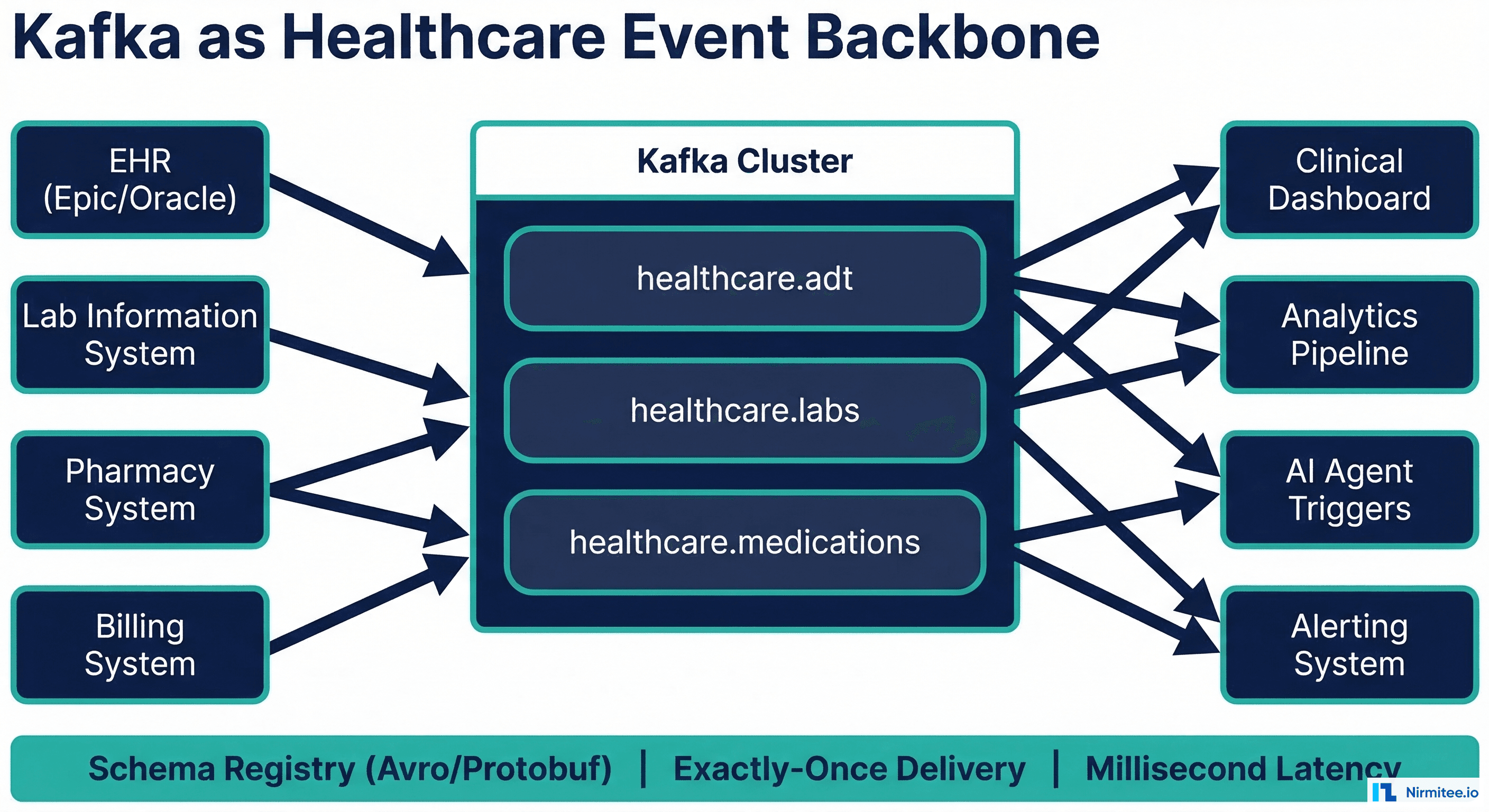
3. Clinical Prediction at Scale: Population Health Gets Real
Clinical prediction models have existed in academic settings for decades. What changed in 2025 is the infrastructure to deploy them across entire health systems — not as research prototypes, but as real-time scoring engines integrated into clinical workflows.
The Infrastructure Shift
The breakthrough is not better models. It is a better deployment infrastructure. Health systems now use medallion data architectures to maintain clean, versioned feature stores from EHR data. Models run on FHIR-connected inference services that score patients in real time and deliver results through CDS Hooks.
| Prediction Domain | Model Input | Outcome | Impact |
|---|---|---|---|
| Sepsis early warning | Vitals, labs, nursing notes | 4-6 hour advance warning | 30% mortality reduction (Epic Sepsis Model) |
| Readmission risk | Demographics, diagnoses, utilization | Risk score at discharge | 15-20% readmission reduction |
| Deterioration detection | Continuous vitals monitoring | 1-2 hour advance warning | Rapid response activation |
| No-show prediction | Scheduling history, demographics | Appointment adherence score | 10-25% reduction in no-shows |
| Length of stay | Admission data, clinical trajectory | Predicted discharge date | Better bed management |
The CDS Hooks Integration Pattern
The standard mechanism for delivering AI predictions into the clinical workflow is CDS Hooks, an HL7 specification that triggers decision support at specific points in the EHR workflow. When a clinician opens a patient chart or signs an order, the EHR fires a CDS Hook event to external services that return actionable cards.
{
"hookInstance": "d1577c69-dfbe-44ad-bd63-3d74a6b95524",
"hook": "patient-view",
"context": {
"userId": "Practitioner/123",
"patientId": "Patient/456"
},
"cards": [{
"summary": "Sepsis Risk: HIGH (Score 8.2/10)",
"indicator": "critical",
"detail": "This patient has elevated lactate (4.2), rising WBC trend, and tachycardia. Consider sepsis bundle initiation.",
"source": { "label": "Sepsis Prediction Model v3.1" },
"suggestions": [{
"label": "Order Sepsis Bundle",
"actions": [{
"type": "create",
"resource": {
"resourceType": "ServiceRequest",
"code": { "text": "Sepsis Bundle Protocol" }
}
}]
}]
}]
}4. Federated Learning: Training on Hospital Data Without Moving It
Healthcare AI has a fundamental data problem: the best training data lives inside hospital EHRs, and HIPAA regulations make it extremely difficult to centralize that data for model training. Federated learning solves this by bringing the model to the data instead of the data to the model.

How Federated Learning Works in Healthcare
- Global model distribution — A central server sends the current model weights to participating hospitals.
- Local training — Each hospital trains the model on its local patient data. No patient data leaves the hospital network.
- Gradient aggregation — Hospitals send only model weight updates (gradients) back to the central server. The server aggregates these updates using secure aggregation protocols.
- Model improvement — The central server updates the global model with the aggregated gradients and redistributes it. This cycle repeats.
The result: a model trained on data from thousands of hospitals without any single hospital sharing its patients' records. According to research published in Nature Medicine, federated models for brain tumor segmentation achieved performance equivalent to centralized training while keeping all patient data local.
Production Implementations
- NVIDIA FLARE — NVIDIA's federated learning framework is deployed across 20+ healthcare institutions for medical imaging models. Their collaboration with the American College of Radiology trains mammography AI across participating sites.
- Google Health + HCA Healthcare — A federated learning partnership trains patient deterioration models across HCA's 180+ hospitals, one of the largest federated healthcare deployments.
- Owkin — A French healthtech company runs federated learning for oncology drug development across major cancer centers, including Memorial Sloan Kettering and Gustave Roussy.
5. MCP and Tool-Use: LLMs That Can Actually Do Things in the EHR
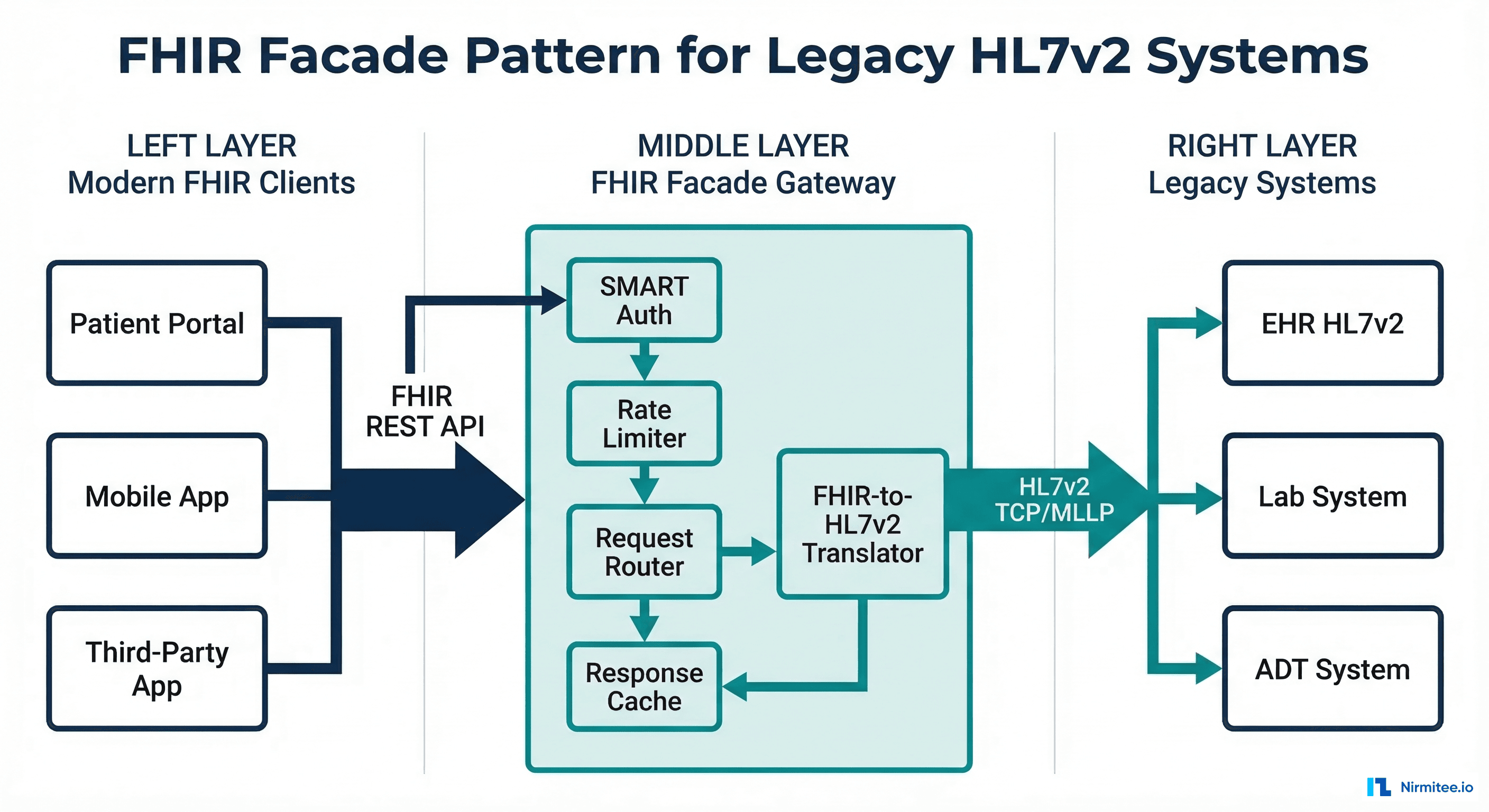
The most transformative breakthrough of 2025-2026 is the shift from AI that suggests to AI that acts. The Model Context Protocol (MCP), introduced by Anthropic, and similar tool-use frameworks give LLMs the ability to call structured APIs as part of their reasoning process.
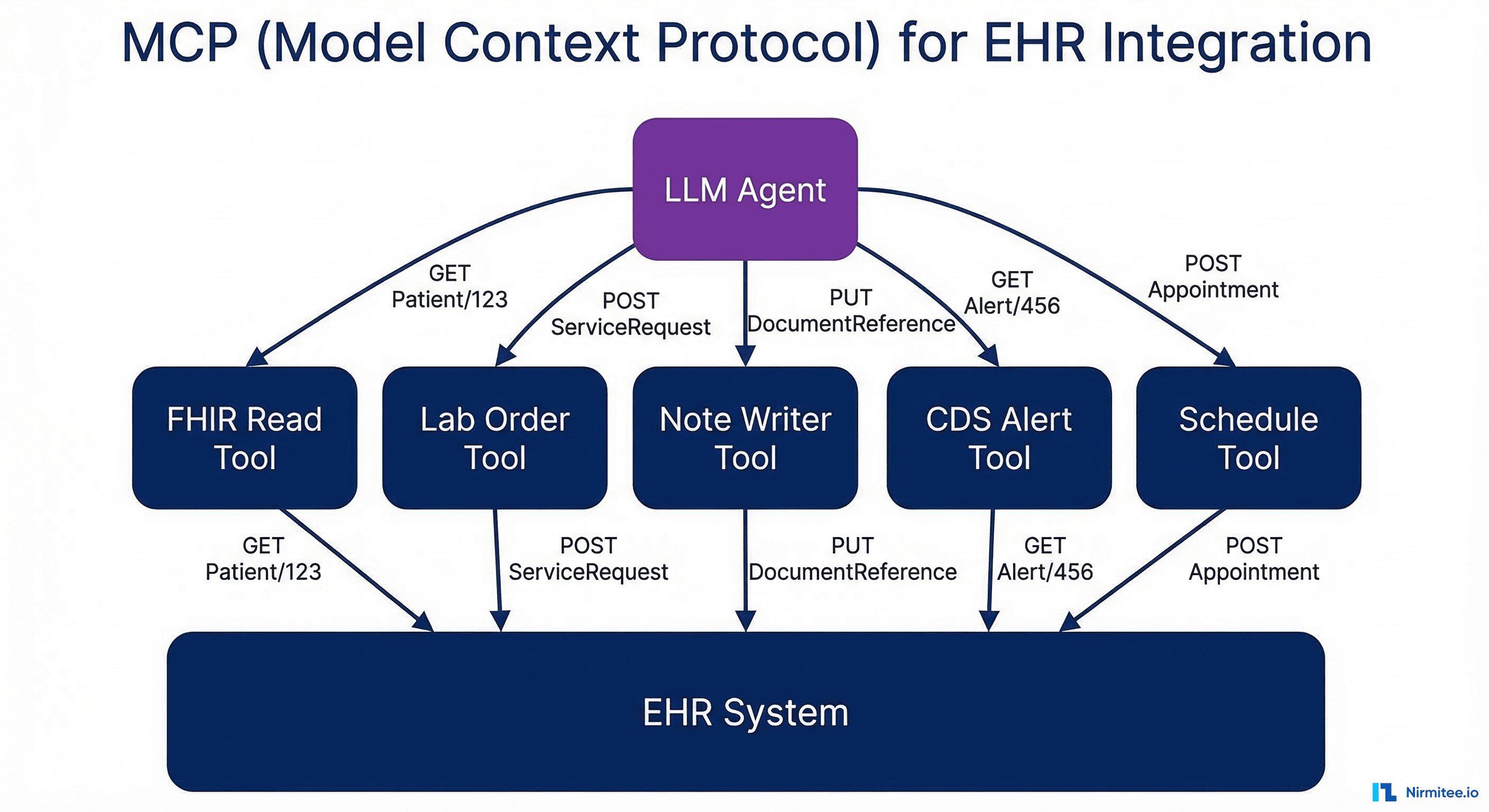 EHR integration" width="1200">
EHR integration" width="1200">
What MCP Enables for Healthcare
An MCP-enabled AI agent connected to a FHIR server can:
- Read patient records — Query FHIR resources (Patient, Observation, MedicationRequest, Condition) using structured search parameters. The agent understands which resources to query based on the clinical question.
- Write clinical data — Create new FHIR resources like DocumentReference (clinical notes), ServiceRequest (orders), and Communication (patient messages) through properly authenticated API calls.
- Orchestrate workflows — Chain multiple FHIR operations together. Example: Check if a patient has an active medication, look up the latest lab values for monitoring that medication, and draft a dosage adjustment recommendation.
- Query external knowledge — Access drug interaction databases, clinical guidelines, and payer coverage policies as additional tool calls within the same reasoning chain.
The Engineering Challenge
Connecting an LLM to healthcare APIs requires careful guardrails. At Nirmitee, our approach to building healthcare AI agents includes:
- Scoped tool access — Each agent has a defined set of FHIR resources it can read and write. A documentation agent cannot modify medication orders. A scheduling agent cannot read clinical notes.
- Human-in-the-loop for writes — All write operations go through a clinician approval step. The agent drafts the action; the clinician confirms it.
- Audit trail — Every tool call is logged with the agent's reasoning chain, the input parameters, and the output. This creates a complete audit trail for regulatory review.
- Deterministic validation — Before any FHIR write operation, a non-AI validation layer checks data types, required fields, and business rules. The AI reasons; the validation layer enforces.
What This Means for Healthtech Leaders
These five breakthroughs share a common thread: they are moving from demonstrations to deployments. If you are a VP of Product or CTO at a healthtech company, here is what to prioritize:
- Start with ambient documentation — It has the clearest ROI (measurable time savings per clinician per day) and the most mature vendor ecosystem. Integration requires SMART on FHIR and FHIR DocumentReference write access.
- Invest in FHIR infrastructure now — Every breakthrough listed here depends on clean, accessible FHIR APIs. Organizations without a FHIR strategy will be unable to adopt any of these technologies.
- Build agentic capabilities incrementally — Start with read-only agents that answer clinical questions from the patient record. Add write capabilities only after establishing confidence in the agent's reasoning quality.
- Evaluate federated learning for your data assets — If you have clinical data across multiple sites, federated learning lets you train better models without the legal complexity of data centralization.
- Watch MCP adoption closely — MCP is emerging as the standard for connecting LLMs to healthcare APIs. Early adoption positions your platform as an AI-native healthcare system.
Build AI-Native Healthcare with Nirmitee
At Nirmitee, we help healthtech companies build production AI systems that integrate with EHRs, meet regulatory requirements, and deliver measurable clinical outcomes. From scalable architecture to AI agent development, our team bridges the gap between AI research and healthcare production systems.
Contact our team to discuss how these AI breakthroughs can accelerate your product roadmap.
Shipping healthcare software that scales requires deep domain expertise. See how our Healthcare Software Product Development practice can accelerate your roadmap. We also offer specialized Agentic AI for Healthcare services. Talk to our team to get started.