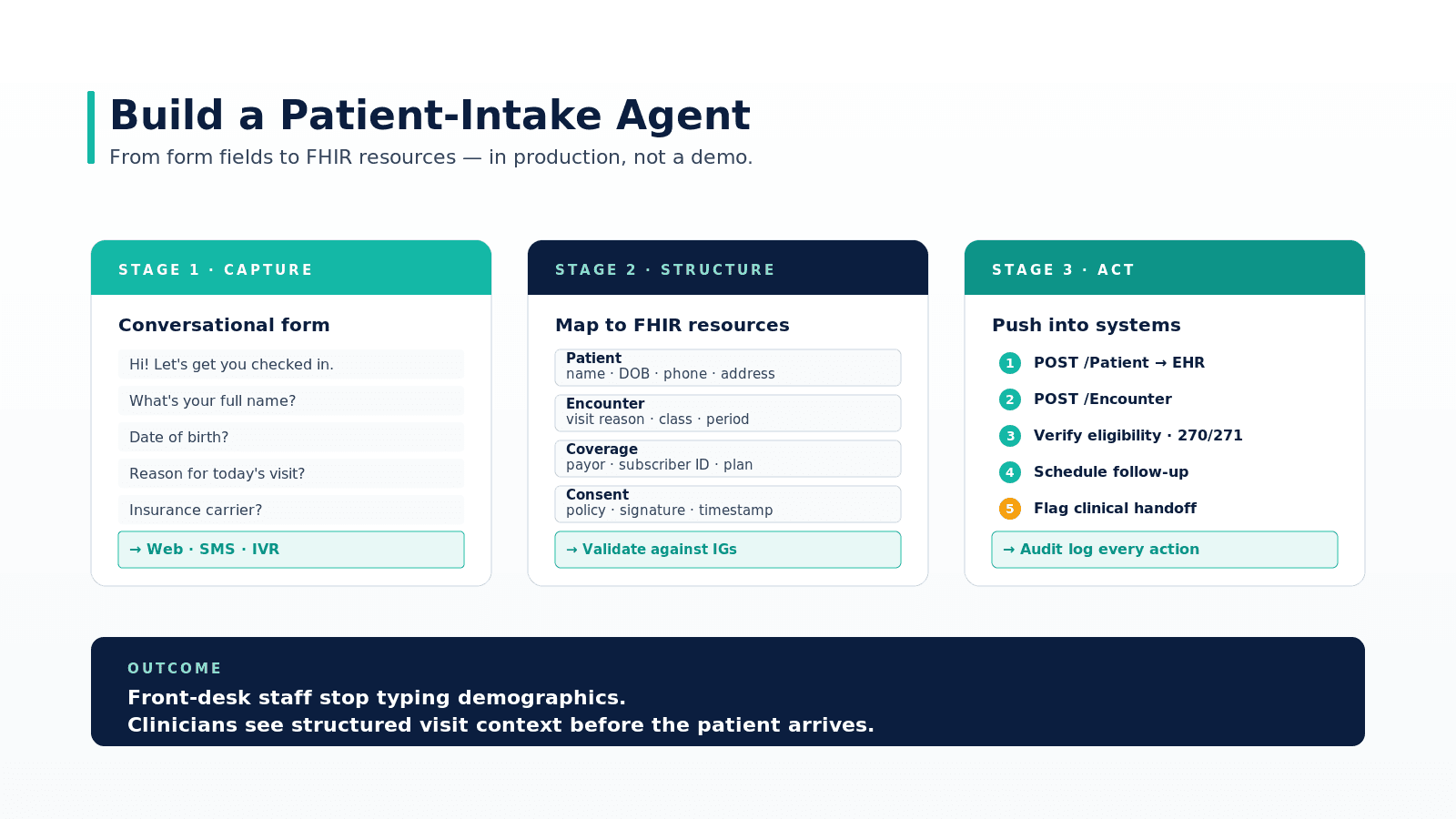
Patient scheduling in healthcare isn't a calendar problem. It's an orchestration challenge involving providers, rooms, equipment, insurance authorizations, patient preferences, and clinical protocols — all intersecting across unpredictable demand patterns. Yet most health systems still rely on scheduling tools designed for basic appointment booking: a patient calls, a front-desk staff member checks availability, an appointment gets created. The result? No-show rates between 5.5% and 50% depending on the setting, an estimated $150 billion in annual revenue loss across the U.S. healthcare system, and clinical teams operating well below capacity while patients wait weeks for care.
The gap between basic scheduling and intelligent orchestration represents one of the highest-ROI automation opportunities in healthcare operations today. Organizations that have deployed AI-powered scheduling systems are reporting no-show reductions of 15-40%, revenue recovery in the millions, and ROI exceeding 3,000% within the first year. This isn't theoretical — a primary care group in Northern California recovered $6.2 million in additional revenue in year one by implementing predictive scheduling with automated demand management.
This guide provides the complete architecture for building or selecting an AI-powered scheduling orchestration system — from no-show prediction ML models to FHIR-native integration patterns, multi-resource constraint solving, and automated waitlist management. Whether you're evaluating vendors or building custom, this is the technical blueprint.
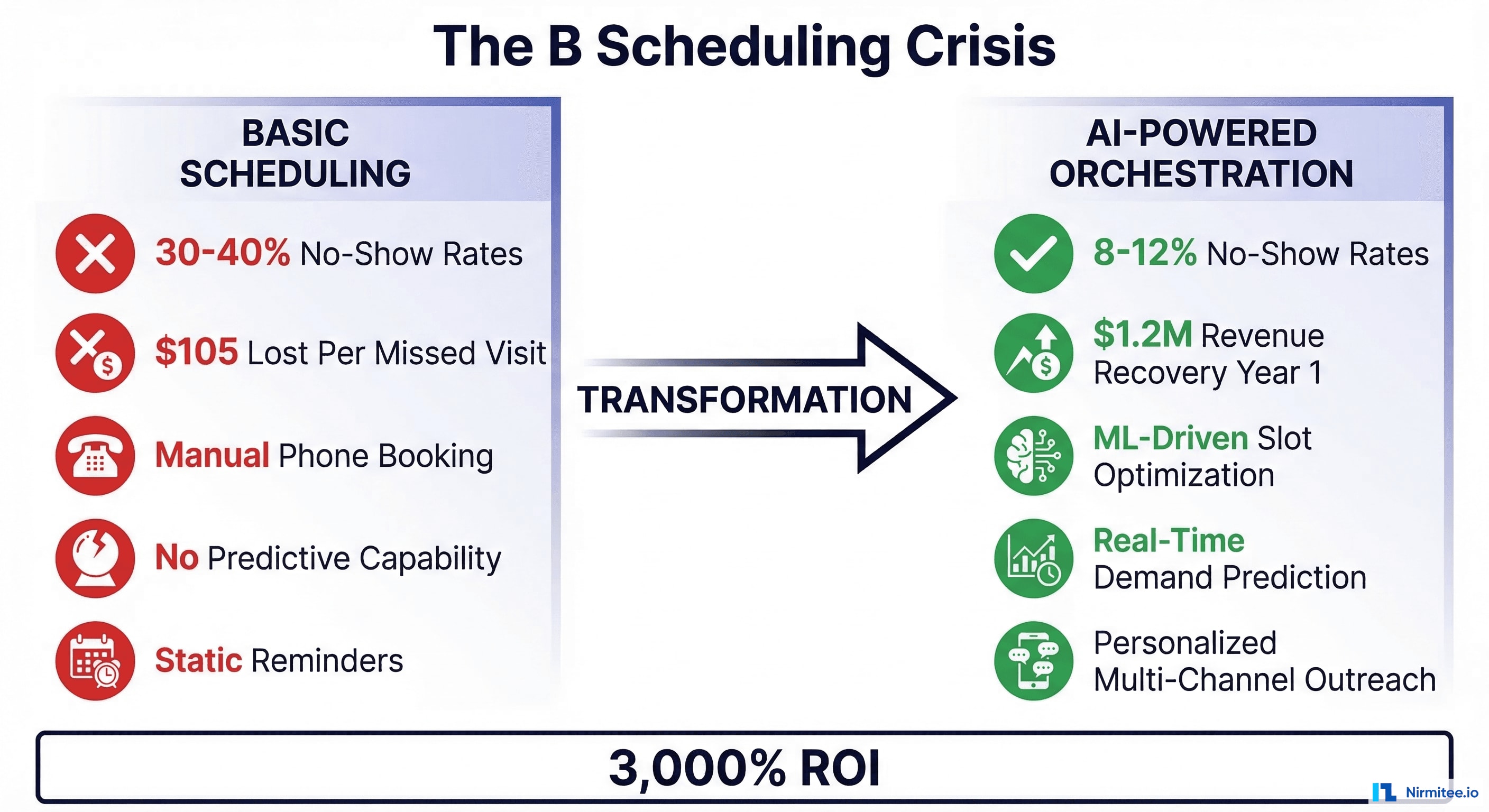
The Scheduling Problem: Why Basic Booking Fails at Scale
Healthcare scheduling operates under constraints that consumer scheduling tools (Calendly, Acuity) were never designed to handle. Understanding these constraints is essential before evaluating solutions.
The No-Show Epidemic
Patient no-shows aren't just inconvenient — they're a systemic operational failure with cascading effects:
- Financial impact: Each missed appointment costs a practice $150-$300 in lost revenue. For a mid-size practice with a 20% no-show rate, that translates to $90,000-$180,000 in annual revenue loss. Across the U.S., the aggregate figure reaches $150 billion annually (Healthcare Innovation Group).
- Clinical impact: Missed appointments delay diagnosis, disrupt care continuity, and worsen chronic disease outcomes. A 2025 study in PMC found that patients who frequently no-show have 2.3x higher emergency department utilization rates.
- Operational impact: Idle provider time, underutilized rooms and equipment, overstaffed shifts, and compressed availability for other patients create a cascade of inefficiency across the organization.
- Equity impact: No-show rates are disproportionately higher among patients facing transportation barriers, childcare constraints, and socioeconomic challenges — the populations most in need of consistent care.
Why Traditional Scheduling Falls Short
Traditional healthcare scheduling systems — including those embedded in major EHRs — typically offer:
- Calendar-based availability grids (provider blocks, location rooms)
- Template-driven scheduling rules (appointment types, durations)
- Basic automated reminders (single-channel, fixed timing)
- Manual waitlist management (staff calls down a list when cancellations occur)
What they lack is the intelligence layer: predictive modeling to anticipate no-shows before they happen, dynamic resource optimization that adapts to real-time demand, and automated workflows that fill cancellations in seconds rather than hours. This intelligence gap is where AI-powered orchestration delivers transformative value.
AI-Powered No-Show Prediction: The ML Architecture
The most impactful capability in intelligent scheduling is no-show prediction — using machine learning to assign a risk score to every upcoming appointment and trigger differentiated interventions based on that score. A 2025 comprehensive review in ScienceDirect analyzed 52 publications on ML-based no-show prediction, finding that ensemble models (XGBoost, Random Forest) consistently outperform simpler approaches, with AUC scores between 0.75 and 0.95.
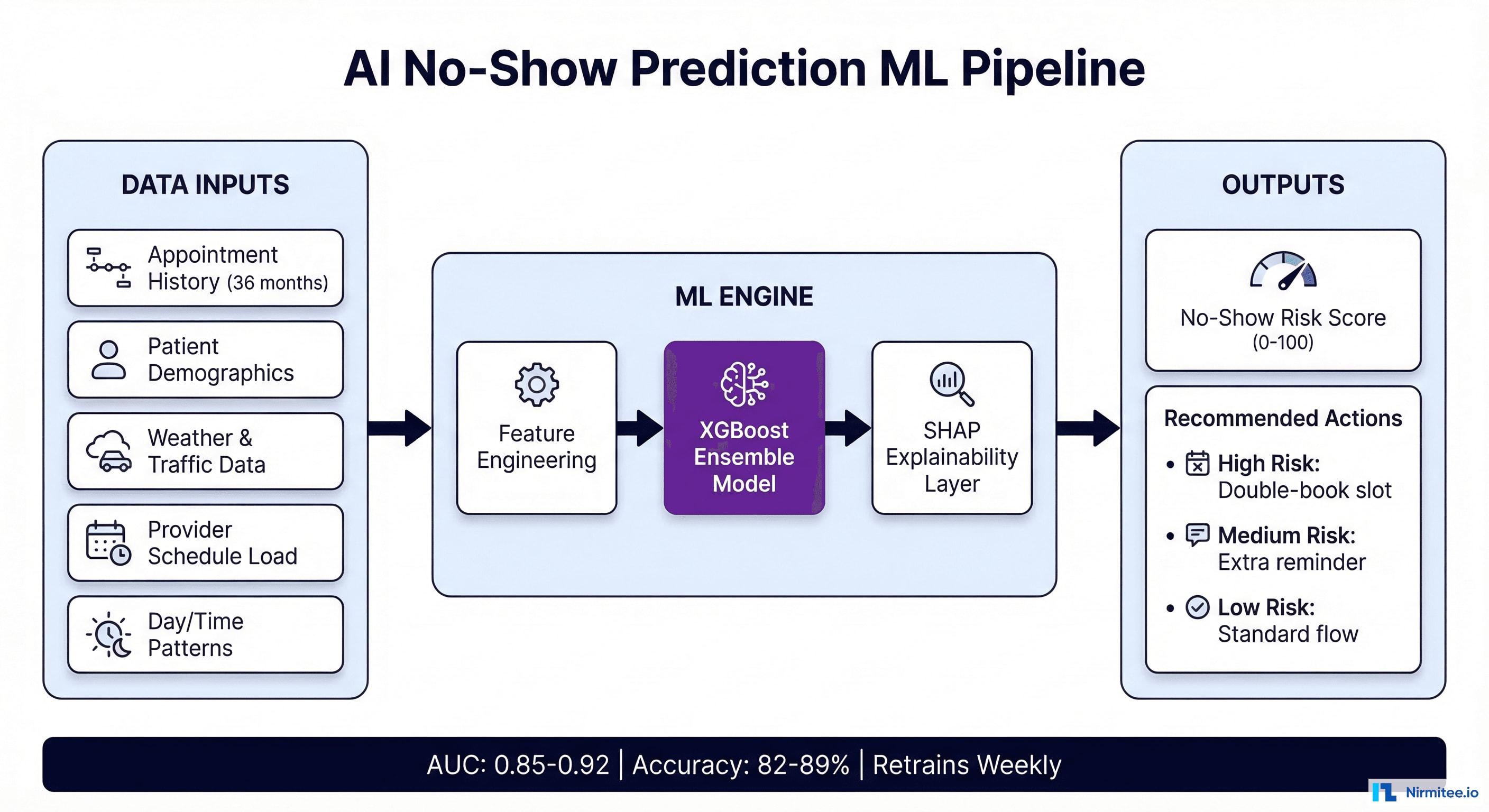
Feature Engineering: What the Model Needs
The predictive accuracy of a no-show model depends heavily on the features available. Based on published research and production deployments, the highest-signal features fall into five categories:
1. Historical appointment behavior (highest signal)
- Patient's no-show rate over past 12-36 months
- Number of same-day cancellations in past 6 months
- Average lead time between scheduling and attendance
- Pattern of no-shows by day-of-week and time-of-day
2. Appointment characteristics
- Appointment type (new patient vs. follow-up vs. procedure)
- Lead time (days between scheduling and appointment date)
- Whether the appointment was patient-initiated or provider-ordered
- Number of prior reschedules for this appointment
3. Temporal and environmental factors
- Day of week and time of day (Monday mornings and Friday afternoons show higher no-show rates)
- Season and weather conditions (severe weather increases no-shows by 8-15%)
- Holiday proximity and school schedule alignment
- Distance from patient address to facility
4. Patient demographics and access factors
- Insurance type (Medicaid populations show 2-3x higher no-show rates than commercial)
- Transportation access indicators
- Patient portal engagement level
- Communication preference (SMS vs. voice vs. email responsiveness)
5. Provider and scheduling context
- Provider-specific no-show rates (some providers consistently see lower no-shows)
- Clinic location and parking availability
- Same-day appointment availability (patients with flexible rescheduling options no-show less)
Model Architecture and Performance
Production no-show prediction systems typically employ an ensemble approach:
# Simplified no-show prediction pipeline
from xgboost import XGBClassifier
from sklearn.model_selection import TimeSeriesSplit
# Feature matrix: appointment + patient + temporal features
features = [
'historical_noshow_rate', 'lead_time_days', 'day_of_week',
'hour_of_day', 'appointment_type', 'insurance_category',
'distance_miles', 'prior_reschedules', 'portal_engagement_score',
'weather_severity_forecast', 'provider_noshow_rate'
]
# XGBoost with time-series aware cross-validation
model = XGBClassifier(
n_estimators=500,
max_depth=6,
learning_rate=0.05,
scale_pos_weight=3.5, # Handle class imbalance
eval_metric='auc'
)
# Train with temporal split (no data leakage from future)
tscv = TimeSeriesSplit(n_splits=5)
model.fit(X_train[features], y_train)
# Output: probability of no-show (0.0 to 1.0)
risk_scores = model.predict_proba(X_upcoming)[:, 1]A January 2026 study demonstrated that XGBoost models with SHAP explainability achieve 82-89% accuracy while providing interpretable risk factor breakdowns for each prediction — critical for clinical workflow integration where staff need to understand why a patient is flagged as high-risk.
Risk-Stratified Intervention Protocol
The prediction model's value is realized through differentiated interventions based on risk tiers:
| Risk Tier | Score Range | Automated Actions | Expected Impact |
|---|---|---|---|
| Low Risk | 0.0 - 0.15 | Standard reminder (SMS, 48hr + 24hr before) | Maintains <5% no-show rate |
| Medium Risk | 0.15 - 0.40 | Enhanced outreach: SMS + voice call + email; transportation assistance offer; confirm-or-cancel prompt 72hr before | Reduces no-shows by 25-35% |
| High Risk | 0.40 - 0.70 | Personal outreach from care team; offer telehealth alternative; double-book the slot with a waitlist patient; pre-appointment engagement | Reduces no-shows by 40-55% |
| Very High Risk | 0.70 - 1.0 | Same-day confirmation required (auto-cancel if unconfirmed by 2 hours prior); slot automatically released to waitlist | Recovers 60-80% of otherwise lost slots |
Multi-Resource Scheduling: Beyond Provider Calendars
The most operationally complex — and highest-value — scheduling challenge in healthcare isn't booking a single provider appointment. It's orchestrating multiple resources simultaneously: the right provider, the right room, the right equipment, the right support staff, and the right pre-authorization — all aligned to a single patient visit window.

The Constraint Problem
Consider a surgical consult that requires:
- An orthopedic surgeon (available Tuesday/Thursday afternoons)
- A pre-op exam room with imaging capability
- A radiology technician for concurrent imaging
- Equipment: portable ultrasound unit (shared across 3 departments)
- Insurance pre-authorization completion (avg. 3-5 business days)
- Patient preference: prefers mornings, needs wheelchair-accessible room
A basic scheduling system treats these as sequential manual checks. An AI orchestration engine solves them as a constraint satisfaction problem — evaluating all permutations simultaneously and presenting the optimal options in seconds.
Implementation Architecture
Multi-resource scheduling systems typically employ a constraint solver backed by a resource availability engine:
# Multi-resource constraint solving pseudocode
def find_optimal_slots(appointment_request):
constraints = {
'provider': get_provider_availability(request.provider_id),
'room': get_room_availability(
request.room_type,
request.accessibility_requirements
),
'equipment': get_equipment_availability(request.equipment_ids),
'staff': get_support_staff_availability(request.staff_roles),
'authorization': check_insurance_authorization_status(
request.patient_id,
request.procedure_code
),
}
# Patient preferences as soft constraints
preferences = {
'time_of_day': request.patient.preferred_time,
'day_of_week': request.patient.preferred_days,
'location': request.patient.preferred_location,
'provider_continuity': request.patient.usual_provider,
}
# Solve using constraint propagation + branch-and-bound
solutions = constraint_solver.solve(
hard_constraints=constraints,
soft_constraints=preferences,
optimization_target='minimize_patient_wait + maximize_utilization',
time_horizon_days=14,
max_solutions=5
)
return rank_solutions(solutions, patient_preference_weights)Provider Load Balancing
Intelligent scheduling doesn't just find available slots — it distributes patient load across providers to prevent burnout and optimize outcomes:
- Panel balancing: New patients distributed based on provider panel size, specialty match, and current workload
- Complexity weighting: High-acuity appointments count more against provider capacity than routine follow-ups
- Break compliance: System enforces minimum breaks between appointments, longer blocks for procedures
- Same-day buffer: Reserves 10-15% of each provider's schedule for same-day urgent slots, adjusted dynamically based on historical demand patterns
Automated Waitlist Management
Manual waitlist management — where staff members call down a list when a cancellation occurs — is one of the most labor-intensive and least effective processes in healthcare operations. By the time a staff member reaches an available patient, the cancelled slot has often passed. Automated waitlist systems transform this from a 4-6 hour manual process into a 90-second automated workflow with fill rates jumping from 25-30% to 70-90% (PMC, 2025).

How It Works
- Real-time cancellation detection: EHR webhooks or polling detect slot openings within seconds of cancellation
- Priority-based matching: Waitlist patients are scored by urgency (clinical need + time waiting + appointment type match + scheduling flexibility)
- Instant multi-channel outreach: Top-ranked patients receive SMS/push/voice notification within 30 seconds, with a direct link to confirm the slot
- First-responder booking: The first patient to accept gets the slot; others are notified it's been filled
- Cascade logic: If the top-priority patient doesn't respond within the configured window (typically 15-30 minutes), the system automatically offers to the next patient
- Analytics feedback: Response rates, fill times, and conversion metrics feed back into the priority algorithm
ROI of Automated Waitlists
For a multi-provider practice with 100 appointments/day and a 15% cancellation rate:
- Manual process: 15 cancellations/day x 25% fill rate = 3.75 slots recovered = $750/day
- Automated process: 15 cancellations/day x 80% fill rate = 12 slots recovered = $2,400/day
- Net improvement: $1,650/day = $412,500 annually in recovered revenue
Patient Self-Scheduling Portals: Design That Converts
Self-scheduling adoption has grown steadily, from 4% to 15% of kept appointments in organizations that offer it (PMC, 2022). But the difference between a portal that achieves 5% adoption and one that reaches 40%+ lies entirely in design and integration quality.
High-Converting Self-Scheduling Features
- Intelligent appointment type matching: Rather than forcing patients to choose from clinical appointment types they don't understand ("Est. Pt. F/U 15 min"), use symptom-based or reason-based selection ("Follow up on my back pain") that maps to the correct appointment type, duration, and provider pool behind the scenes
- Real-time insurance verification: Verify coverage and display copay estimates before the patient selects a slot — not after. Nothing kills conversion like a surprise eligibility denial post-booking
- Provider matching with transparency: Show provider photos, specialties, languages spoken, and patient satisfaction scores. Patients who choose their provider no-show 23% less than those assigned randomly
- Multi-visit bundling: For patients needing labs + imaging + consult, offer bundled scheduling that books all visits in sequence with optimal gap times
- Waitlist opt-in: "Want an earlier appointment? Join our waitlist" — with estimated wait time and automatic notification when slots open
- Confirmation + preparation: Immediately after booking, send appointment prep instructions, forms to complete in advance, directions, and parking information. Pre-engaged patients are 35% less likely to no-show
SMS, Voice, and Multi-Channel Reminder Automation
Appointment reminders are the lowest-hanging fruit in scheduling automation — and the data is clear: AI-optimized multi-channel reminders reduce no-shows by 30-50% compared to single-channel approaches (CallMyDoc, 2025).
Optimal Reminder Cadence (Research-Backed)
| Timing | Channel | Content | Action Required |
|---|---|---|---|
| 7 days before | Appointment details + preparation instructions + forms to complete | Pre-visit checklist link | |
| 3 days before | SMS | Confirm/Reschedule/Cancel with one-tap buttons | Confirm or manage appointment |
| 1 day before | SMS + Push | Final reminder with directions, parking, copay estimate | Confirm attendance |
| 2 hours before | SMS | "We're ready for you at [time]. Running on time / [X] min delay" | Arrival notification |
| Post-no-show | SMS + Voice | Missed appointment notification + easy rescheduling link | Reschedule with one tap |
AI-Optimized Channel Selection
Not every patient responds to the same channel. An intelligent system learns individual preferences:
- Track open rates, response rates, and confirmation rates by channel per patient
- A/B test message timing and content variations continuously
- Escalate channels based on non-response: if SMS gets no reply within 4 hours, trigger a voice call
- Respect communication preferences and opt-out status (TCPA compliance is non-negotiable)
- Use NLP for conversational responses: "Can you move me to Thursday?" triggers an automated reschedule flow rather than requiring a phone call
EHR Integration: Epic Cadence, Oracle Health, and Open APIs
No scheduling automation system operates in isolation. Deep integration with the EHR's native scheduling module is the difference between a standalone tool and a system-wide platform. Here's how the major EHR scheduling systems integrate.
Epic Cadence Integration
Epic Cadence is the dominant outpatient scheduling module in U.S. health systems. Integration pathways include:
- FHIR R4 APIs (open.epic.com): Schedule, Slot, and Appointment resources for reading availability and booking appointments. Supports the
$findoperation for availability queries. - HL7v2 SIU (Scheduling Information Unsolicited): Real-time ADT-style messages for appointment creation, modification, and cancellation events. SIU^S12 (new appointment), SIU^S14 (modification), SIU^S15 (cancellation).
- Epic MyChart Integration: Patient-facing scheduling flows that surface directly within MyChart, maintaining a unified patient experience.
- Cadence Link: Epic's native patient self-scheduling that can be embedded in external portals via web components.
Oracle Health (Cerner) Integration
- FHIR R4 APIs: Oracle Health's Millennium platform exposes Schedule, Slot, and Appointment FHIR resources through its open API platform.
- HL7v2 SIU/SRM messaging: Scheduling request and notification messages for bidirectional appointment synchronization.
- Oracle Health Scheduling Management: The scheduling module supports template-based scheduling with resource allocation and conflict detection.
EHR-Agnostic Integration Pattern
For organizations running multiple EHRs or planning for interoperability, the recommended architecture uses a scheduling abstraction layer:
# EHR-agnostic scheduling adapter pattern
class SchedulingAdapter:
"""Abstract interface for EHR scheduling integration"""
def get_available_slots(self, provider_id, date_range, appointment_type):
"""Query EHR for available appointment slots"""
raise NotImplementedError
def book_appointment(self, slot_id, patient_id, appointment_details):
"""Create appointment in EHR scheduling system"""
raise NotImplementedError
def cancel_appointment(self, appointment_id, reason_code):
"""Cancel appointment and trigger waitlist automation"""
raise NotImplementedError
def subscribe_to_changes(self, callback_url, event_types):
"""Register webhook for real-time scheduling events"""
raise NotImplementedError
class EpicCadenceAdapter(SchedulingAdapter):
"""Epic Cadence implementation via FHIR R4 + SIU v2"""
pass
class OracleHealthAdapter(SchedulingAdapter):
"""Oracle Health/Millennium implementation via FHIR R4"""
passFHIR Scheduling Resources: The Interoperability Foundation
The HL7 FHIR standard defines three core resources for scheduling interoperability, designed to be compatible with the iCalendar specification. For organizations building scheduling automation, FHIR provides the standardized data model that enables cross-system scheduling, patient self-scheduling, and third-party integrations. Learn more about building healthcare AI solutions on interoperable foundations.
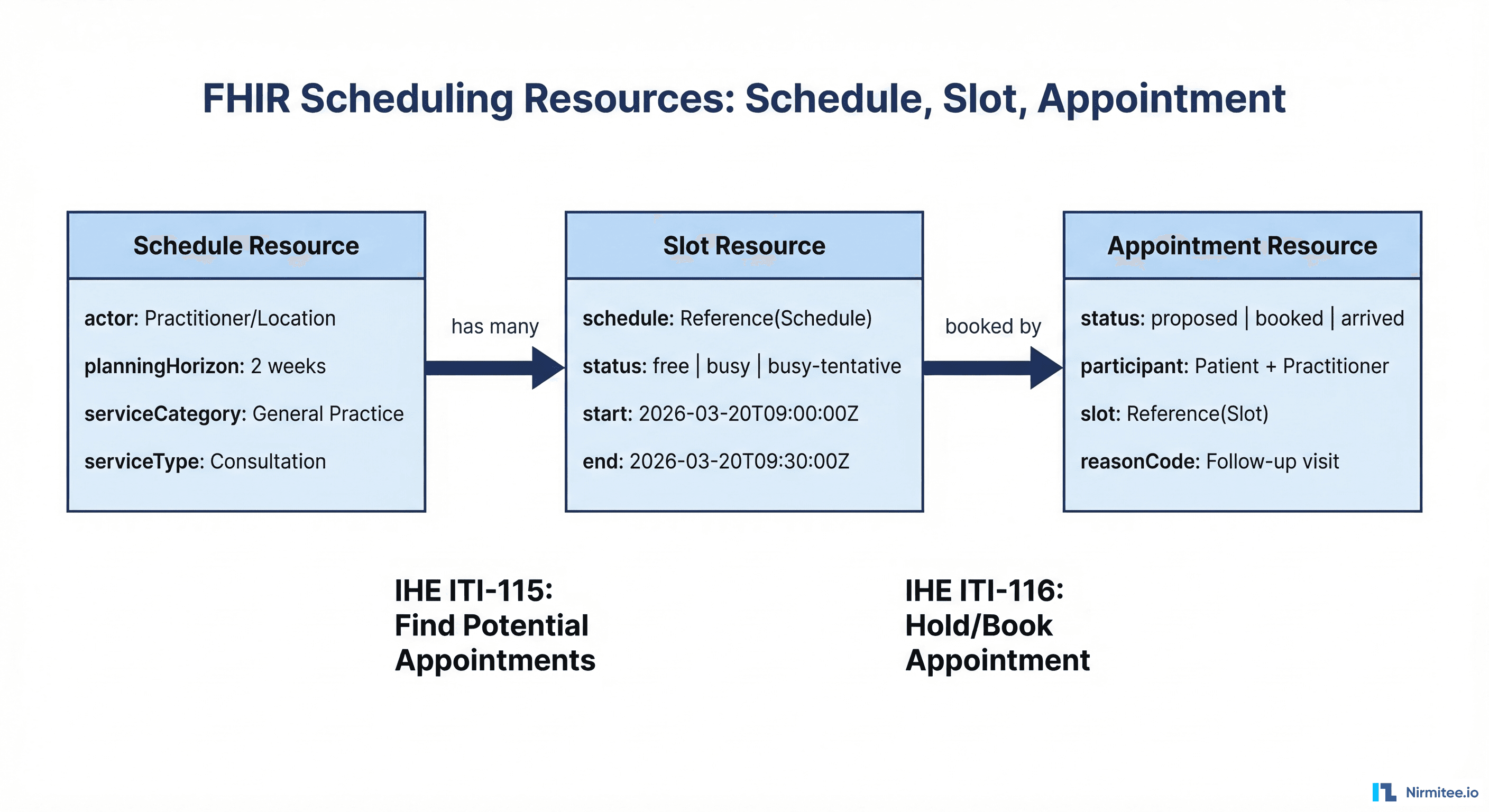
Schedule Resource
The Schedule resource defines a container for time slots — it represents a provider's, location's, or device's overall availability pattern:
{
"resourceType": "Schedule",
"id": "schedule-dr-smith-orthopedics",
"active": true,
"serviceCategory": [{
"coding": [{"system": "http://terminology.hl7.org/CodeSystem/service-category", "code": "17", "display": "General Practice"}]
}],
"serviceType": [{
"coding": [{"system": "http://terminology.hl7.org/CodeSystem/service-type", "code": "124", "display": "Orthopedic Consultation"}]
}],
"actor": [
{"reference": "Practitioner/dr-smith", "display": "Dr. Sarah Smith, MD"},
{"reference": "Location/clinic-a-room-4", "display": "Clinic A, Room 4"}
],
"planningHorizon": {
"start": "2026-03-19T00:00:00Z",
"end": "2026-04-02T00:00:00Z"
}
}Slot Resource
Slots represent individual bookable time windows within a Schedule. Each Slot has a status indicating its availability:
{
"resourceType": "Slot",
"id": "slot-2026-03-20-0900",
"schedule": {"reference": "Schedule/schedule-dr-smith-orthopedics"},
"status": "free",
"start": "2026-03-20T09:00:00Z",
"end": "2026-03-20T09:30:00Z",
"serviceType": [{
"coding": [{"code": "124", "display": "Orthopedic Consultation"}]
}]
}Appointment Resource
The Appointment resource represents a booked (or proposed) meeting. It references one or more Slots and includes participant details:
{
"resourceType": "Appointment",
"id": "appointment-12345",
"status": "booked",
"serviceType": [{
"coding": [{"code": "124", "display": "Orthopedic Consultation"}]
}],
"slot": [{"reference": "Slot/slot-2026-03-20-0900"}],
"participant": [
{
"actor": {"reference": "Patient/patient-jane-doe"},
"status": "accepted"
},
{
"actor": {"reference": "Practitioner/dr-smith"},
"status": "accepted"
}
],
"start": "2026-03-20T09:00:00Z",
"end": "2026-03-20T09:30:00Z",
"reasonCode": [{"text": "Follow-up for knee replacement evaluation"}]
}IHE Scheduling Profile Operations
The IHE ITI Scheduling profile (based on FHIR R4) standardizes two key operations for cross-organizational scheduling:
- ITI-115: Find Potential Appointments — Query available appointment opportunities across providers and locations using the
Appointment/$findoperation - ITI-116: Hold/Book Appointment — Reserve and confirm an appointment slot, transitioning from
proposedtobookedstatus
These operations enable patient self-scheduling portals and third-party scheduling platforms to interact with any FHIR-compliant EHR without custom integration per system. This is especially relevant for organizations pursuing agentic AI workflows in healthcare where scheduling is one of multiple automated capabilities.
Scheduling Analytics and Continuous Optimization
An AI scheduling system generates a continuous stream of data that enables ongoing optimization — but only if you're measuring the right metrics.
Key Performance Indicators
| Metric | Baseline (Manual) | Target (AI-Optimized) | Measurement |
|---|---|---|---|
| No-show rate | 18-30% | 8-12% | Weekly by provider, location, appointment type |
| Schedule utilization | 65-75% | 85-92% | Daily: booked slots / available slots |
| Cancellation fill rate | 20-30% | 70-90% | Real-time: filled cancellations / total cancellations |
| Time-to-third-available | 12-21 days | 5-10 days | Weekly by specialty and location |
| Self-scheduling adoption | 5-10% | 25-40% | Monthly: self-scheduled / total scheduled |
| Patient satisfaction | 3.2/5 | 4.3+/5 | Post-visit survey, scheduling-specific question |
| Revenue per provider hour | Varies | +15-25% | Monthly: total revenue / total provider hours |
Optimization Feedback Loops
The analytics layer should drive three automated optimization cycles:
- Model retraining (weekly): No-show prediction models retrain on the latest 12-36 months of appointment data, incorporating new features and adjusting for drift
- Template optimization (monthly): Scheduling templates (slot durations, appointment type mixes, buffer times) adjust based on actual utilization patterns and patient demand signals
- Capacity planning (quarterly): Longer-term demand forecasting informs hiring, facility planning, and service line expansion decisions
Vendor Comparison: Build vs. Buy in 2026
The healthcare scheduling automation market includes both point solutions and platform plays. Here's how the leading vendors compare across the capabilities that matter most for AI-powered orchestration. For more context on where scheduling fits within broader automated patient communication strategies, see our detailed guide.
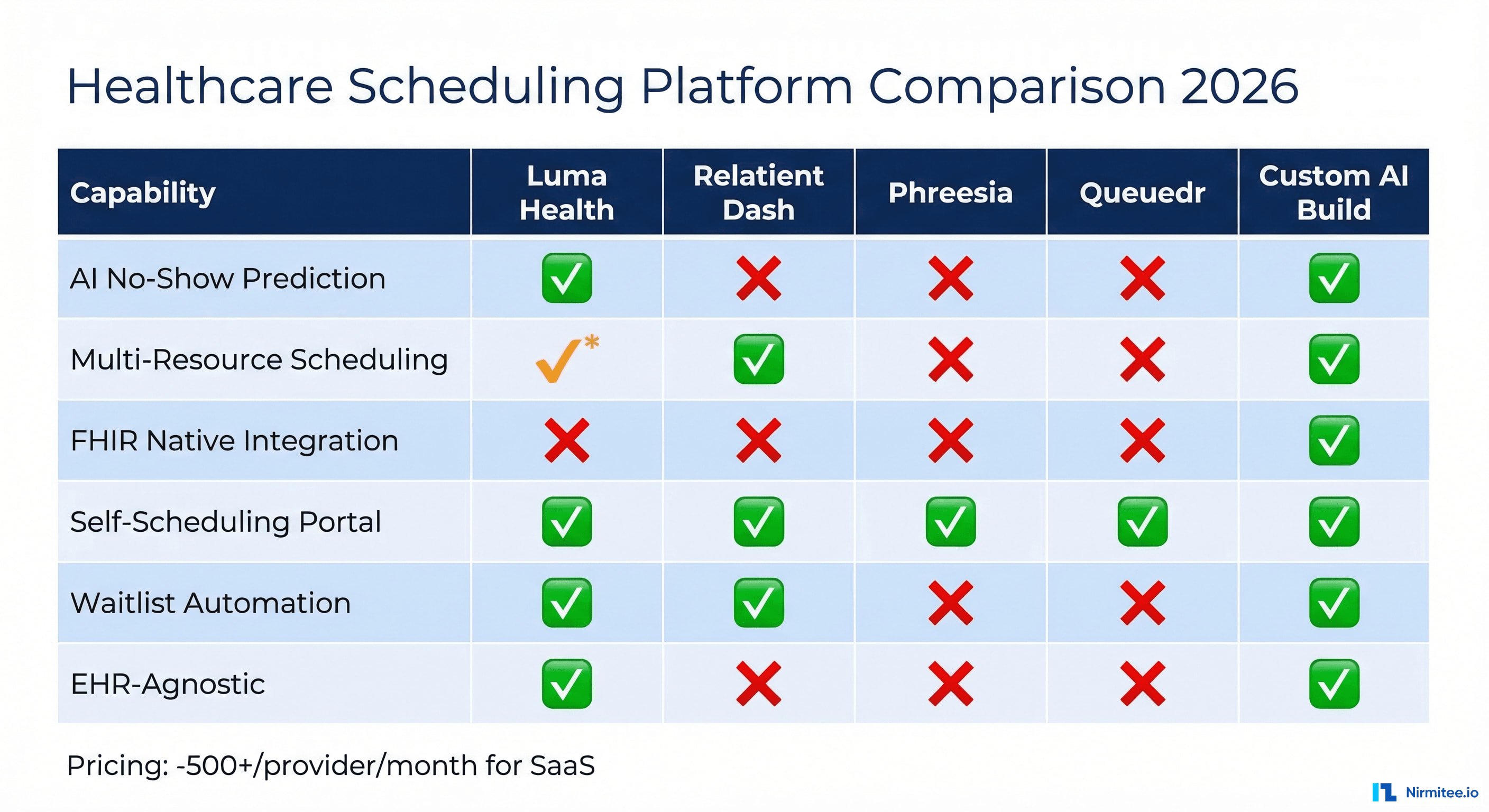
Luma Health
- Strengths: Patient success platform with strong waitlist automation, multi-channel outreach, and broad EHR integration (Epic, Oracle Health, athenahealth, eClinicalWorks)
- AI capabilities: Predictive analytics for no-show risk, automated waitlist management with priority scoring
- Best for: Multi-location practices and health systems wanting turnkey scheduling + patient engagement
- Limitation: Limited customization of ML models; constrained to Luma's prediction engine
Relatient (Dash Scheduling)
- Strengths: KLAS-ranked leader in patient self-scheduling; rules-driven scheduling that handles complex multi-provider, multi-visit workflows. 92% user satisfaction rating
- AI capabilities: Rules-based optimization (not ML-driven); strong scheduling logic engine
- Best for: Large practices with complex scheduling requirements across multiple specialties and locations
- Limitation: Heavier implementation; less AI/ML sophistication than Luma or custom builds
Phreesia
- Strengths: Market leader in patient intake and registration; scheduling is part of a broader patient access platform including digital check-in and payment collection
- AI capabilities: Limited scheduling-specific AI; strength is in intake workflow automation
- Best for: Organizations prioritizing intake efficiency alongside scheduling; strong payment workflow integration
- Limitation: Scheduling is not the primary product — less depth than dedicated scheduling platforms
Queuedr
- Strengths: Focused specifically on waitlist management and cancelled appointment recovery; lightweight integration model
- AI capabilities: Automated waitlist matching and notification sequencing
- Best for: Practices wanting to solve the waitlist/cancellation problem without replacing their entire scheduling stack
- Limitation: Narrow scope — doesn't address no-show prediction, self-scheduling, or multi-resource optimization
Custom AI Build
- Strengths: Full control over ML models, feature engineering, and integration architecture; FHIR-native by design; can incorporate proprietary data sources
- AI capabilities: Unlimited — custom no-show prediction, demand forecasting, constraint solving, NLP-based scheduling
- Best for: Health systems with engineering capacity and unique scheduling complexity that off-the-shelf tools can't address
- Limitation: 6-12 month build timeline; requires ML engineering, healthcare domain expertise, and ongoing model operations
- Estimated cost: $300K-$800K initial build + $100K-$200K/year for MLOps and maintenance
Decision Framework
| Factor | Buy (SaaS Vendor) | Build (Custom) |
|---|---|---|
| Time to value | 4-8 weeks | 6-12 months |
| Upfront cost | $99-500/provider/month | $300K-$800K |
| ML customization | Limited to vendor models | Full control |
| EHR integration depth | Pre-built connectors | Custom, unlimited depth |
| Competitive differentiation | Same tools as competitors | Proprietary advantage |
| Ongoing maintenance | Vendor-managed | Internal team required |
Implementation Roadmap: From Pilot to Scale
A phased approach minimizes risk while delivering early value:
Phase 1: Foundation (Weeks 1-6)
- Deploy automated multi-channel reminders (SMS + email + voice)
- Implement basic no-show prediction using historical data
- Launch patient self-scheduling for 2-3 high-volume appointment types
- Expected impact: 15-20% no-show reduction, 10% increase in schedule utilization
Phase 2: Intelligence (Weeks 7-16)
- Train and deploy full ML no-show prediction model
- Implement risk-stratified intervention protocols
- Launch automated waitlist management
- Expand self-scheduling to all appointment types
- Expected impact: 30-40% no-show reduction, 20% increase in cancellation fill rate
Phase 3: Orchestration (Weeks 17-26)
- Deploy multi-resource scheduling with constraint solver
- Implement provider load balancing and panel optimization
- Add demand forecasting for capacity planning
- Build analytics dashboard with optimization recommendations
- Expected impact: 85%+ schedule utilization, 25% improvement in time-to-third-available
The Bottom Line: Scheduling as a Strategic Capability
Healthcare scheduling automation in 2026 isn't about replacing phone calls with online booking. It's about building an intelligent orchestration layer that predicts demand, optimizes resources, recovers revenue from cancellations, and continuously improves through data-driven feedback loops.
The organizations that treat scheduling as a strategic capability — investing in AI prediction, multi-resource optimization, and automated patient engagement — are seeing measurable returns: no-show rates cut in half, millions in recovered revenue, and patients who actually get the care they need, when they need it.
The technical building blocks are mature: FHIR scheduling resources provide the interoperability standard, ML models achieve 82-89% prediction accuracy, and automated waitlist systems fill cancellations in 90 seconds. The question isn't whether to automate scheduling — it's whether to buy a platform or build a competitive advantage.