The $56 Billion Problem: Getting Medical Devices to Speak FHIR
Every ICU bed has 10-15 connected medical devices. Ventilators, infusion pumps, patient monitors, pulse oximeters — each generating continuous streams of clinical data. Yet in most hospitals, this data lives in isolated silos, manually transcribed by nurses, or lost entirely once the device screen refreshes.
The Internet of Medical Things (IoMT) market is projected to reach $56 billion by 2028, growing at 15.8% CAGR. The technology to capture device data exists. What's missing is the interoperability layer that transforms raw device signals into standardized, computable clinical data — and that layer is FHIR.
This guide covers the complete device-to-FHIR integration pipeline: from IEEE 11073 at the bedside to FHIR Observations in the EHR, including the new R6 DeviceAlert resource that finally gives clinical alerts a proper FHIR representation.

The Medical Device Communication Landscape
Before we can map device data to FHIR, we need to understand how devices actually communicate. The landscape is fragmented — and that fragmentation is exactly why FHIR matters as a unification layer.
IEEE 11073: The Gold Standard for Bedside Devices
The IEEE 11073 family of standards defines how medical devices exchange data. The two most important sub-standards are:
- IEEE 11073-10201 (Domain Information Model) — Defines the object model: Medical Device System (MDS), Virtual Medical Device (VMD), Channel, and Numeric/Waveform observations
- IEEE 11073-20701 (SDC/Service-oriented Device Connectivity) — The modern, service-oriented protocol for device-to-device and device-to-gateway communication over TCP/IP
SDC (Service-oriented Device Connectivity) is the current-generation protocol replacing the older IEEE 11073-20601 (optimized for Bluetooth personal health devices). SDC uses DPWS (Devices Profile for Web Services) and MDPWS, supporting real-time streaming with sub-second latency.
Protocol Comparison
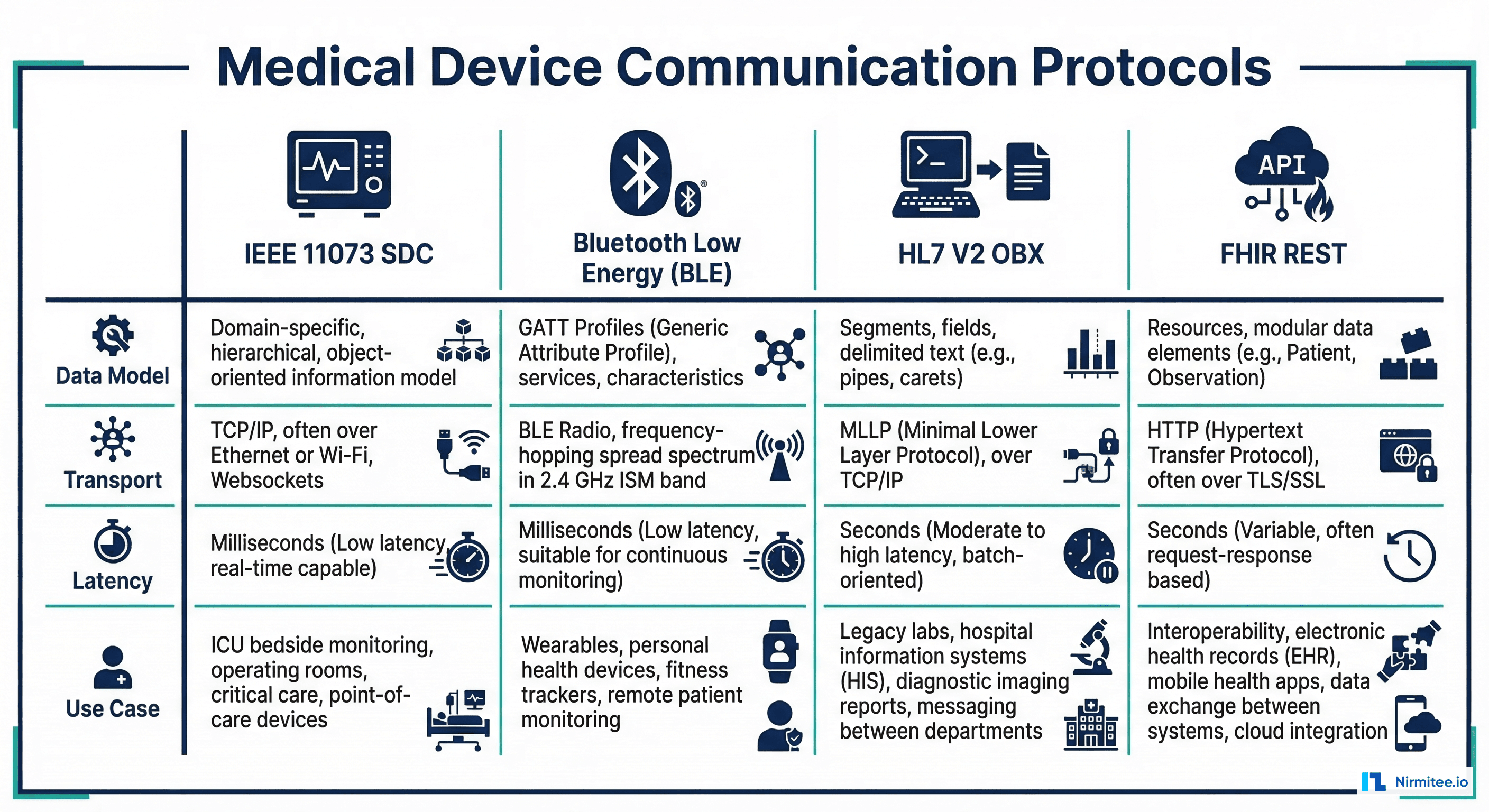
| Protocol | Transport | Latency | Primary Use Case | FHIR Mapping Complexity |
|---|---|---|---|---|
| IEEE 11073 SDC | TCP/IP (DPWS) | ~10-50ms | ICU bedside monitoring | Medium (well-defined model) |
| Bluetooth LE (11073-20601) | BLE radio | ~20-100ms | Personal health devices, wearables | Low (simple profiles) |
| HL7 V2 (OBX segments) | MLLP/TCP | ~1-5s | Legacy lab equipment, vitals | Medium (V2-to-FHIR mapping) |
| Serial/RS-232 | Serial port | ~100ms | Older devices, point-of-care | High (proprietary formats) |
| FHIR REST | HTTP/HTTPS | ~100-500ms | Modern devices, cloud gateways | None (native) |
FHIR Resources for Medical Devices
FHIR provides a comprehensive resource model for representing devices, their measurements, and their alerts. Understanding this model is the foundation of any device integration project.
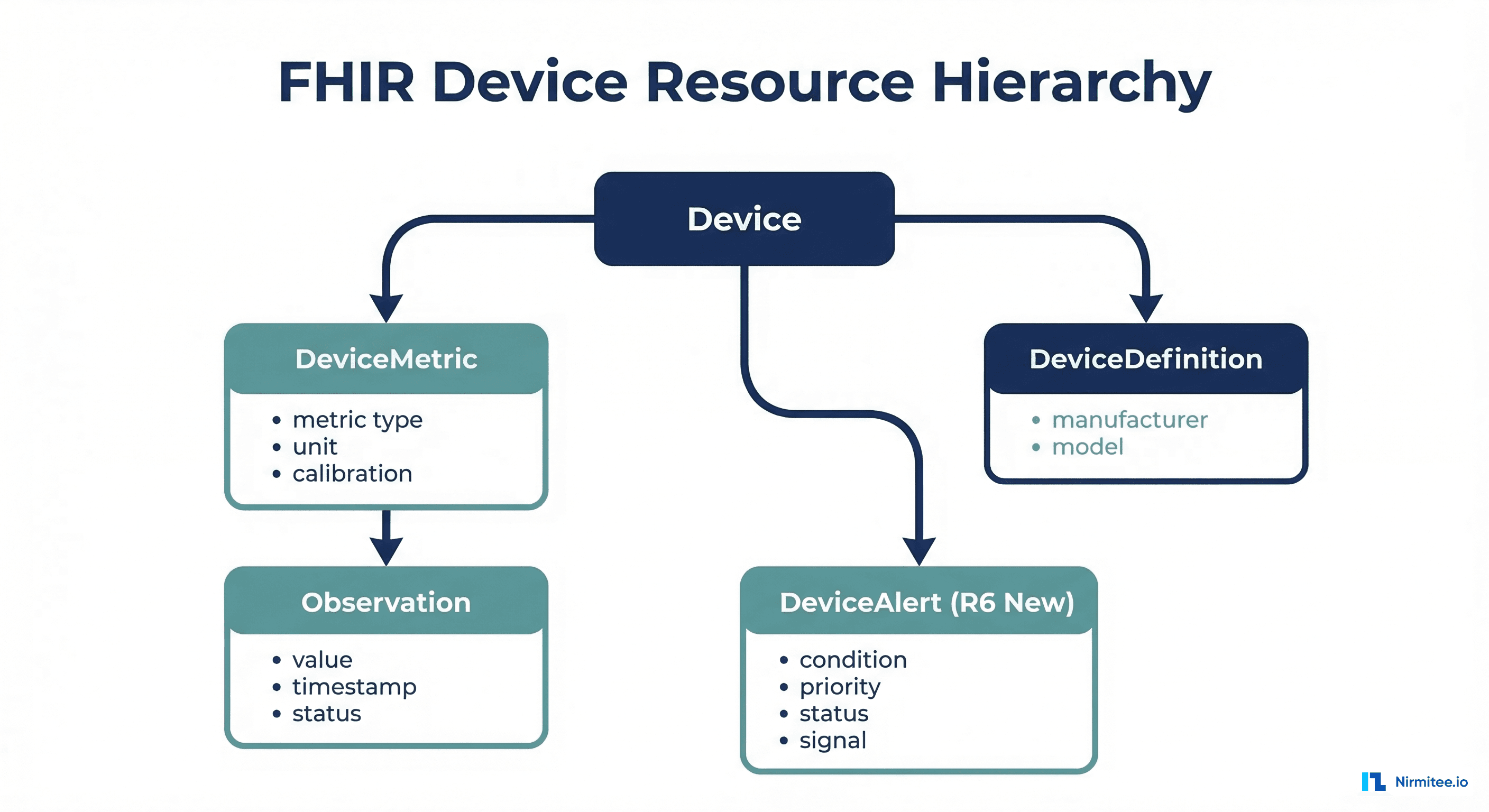
Device Resource
The Device resource represents a physical medical device. It captures identity, classification, and operational status:
{
"resourceType": "Device",
"id": "bedside-monitor-icu-204",
"identifier": [
{
"system": "urn:oid:1.2.840.10004.1.1.1.0.0.1.0.0.1.2680",
"value": "PM-7000X-SN-20241587"
}
],
"udiCarrier": [
{
"deviceIdentifier": "00844588003288",
"carrierHRF": "(01)00844588003288(11)241015(17)291015(10)A213B1(21)1234"
}
],
"status": "active",
"manufacturer": "Philips Healthcare",
"modelNumber": "IntelliVue MX800",
"serialNumber": "SN-20241587",
"type": {
"coding": [
{
"system": "urn:iso:std:iso:11073:10101",
"code": "69965",
"display": "Patient Monitor"
}
]
},
"location": {
"reference": "Location/icu-bed-204"
},
"patient": {
"reference": "Patient/patient-john-smith"
}
}DeviceMetric Resource
The DeviceMetric represents a specific measurement capability of a device — like "SpO2 channel" or "invasive blood pressure channel":
{
"resourceType": "DeviceMetric",
"id": "spo2-metric-icu204",
"type": {
"coding": [
{
"system": "urn:iso:std:iso:11073:10101",
"code": "150456",
"display": "SpO2"
}
]
},
"unit": {
"coding": [
{
"system": "urn:iso:std:iso:11073:10101",
"code": "262688",
"display": "%"
}
]
},
"device": {
"reference": "Device/bedside-monitor-icu-204"
},
"operationalStatus": "on",
"category": "measurement",
"measurementFrequency": {
"value": 1,
"unit": "Hz"
},
"calibration": [
{
"type": "two-point",
"state": "calibrated",
"time": "2026-03-15T08:00:00Z"
}
]
}Device-Sourced Observations
Vitals captured from devices are stored as FHIR Observations with a reference back to the Device. The device element distinguishes device-sourced data from manually entered values:
{
"resourceType": "Observation",
"id": "spo2-reading-20260316-143022",
"status": "final",
"category": [
{
"coding": [
{
"system": "http://terminology.hl7.org/CodeSystem/observation-category",
"code": "vital-signs"
}
]
}
],
"code": {
"coding": [
{
"system": "http://loinc.org",
"code": "2708-6",
"display": "Oxygen saturation in Arterial blood"
},
{
"system": "urn:iso:std:iso:11073:10101",
"code": "150456",
"display": "SpO2"
}
]
},
"subject": {
"reference": "Patient/patient-john-smith"
},
"effectiveDateTime": "2026-03-16T14:30:22Z",
"valueQuantity": {
"value": 97,
"unit": "%",
"system": "http://unitsofmeasure.org",
"code": "%"
},
"device": {
"reference": "Device/bedside-monitor-icu-204"
}
}IEEE 11073 to FHIR Mapping
Translating from the IEEE 11073 domain model to FHIR is the core technical challenge. Here's the definitive mapping:

| IEEE 11073 Concept | IEEE 11073 Code | FHIR Resource | Key FHIR Fields |
|---|---|---|---|
| Medical Device System (MDS) | Object class 1 | Device | identifier, manufacturer, model, serialNumber |
| Virtual Medical Device (VMD) | Object class 2 | Device (child) | parent reference to MDS Device |
| Channel | Object class 3 | DeviceMetric | type, unit, device reference |
| Numeric Observation | Object class 6 | Observation | valueQuantity, device reference, effectiveDateTime |
| Compound Numeric | Object class 7 | Observation (component) | component[] for multi-value (e.g., BP systolic/diastolic) |
| RT Sample Array (Waveform) | Object class 9 | Observation (SampledData) | valueSampledData with period, dimensions, data |
| Enumeration Observation | Object class 8 | Observation | valueCodeableConcept for device modes/states |
| Alert Condition | Attribute 68480 | DeviceAlert (R6) | condition, priority, status |
| Alert Signal | Attribute 68481 | DeviceAlert (R6) | signal type (audible, visual), manifestation |
Implementation: Python Gateway
Here's a practical IEEE 11073 to FHIR translation gateway that converts incoming device data into FHIR resources:
"""IEEE 11073 to FHIR Translation Gateway"""
import json
from datetime import datetime, timezone
from dataclasses import dataclass
from typing import Optional
# IEEE 11073 nomenclature to LOINC mapping
IEEE_TO_LOINC = {
"150456": {"code": "2708-6", "display": "Oxygen saturation (SpO2)"},
"150037": {"code": "8867-4", "display": "Heart rate"},
"150087": {"code": "76536-0", "display": "Respiratory rate"},
"150021": {"code": "8480-6", "display": "Systolic blood pressure"},
"150022": {"code": "8462-4", "display": "Diastolic blood pressure"},
"150023": {"code": "8478-0", "display": "Mean blood pressure"},
"150364": {"code": "8310-5", "display": "Body temperature"},
}
@dataclass
class DeviceReading:
device_id: str
patient_id: str
ieee_code: str
value: float
unit: str
timestamp: str
alert_priority: Optional[str] = None
def reading_to_observation(reading: DeviceReading) -> dict:
"""Convert a device reading to a FHIR Observation."""
loinc = IEEE_TO_LOINC.get(reading.ieee_code, {})
observation = {
"resourceType": "Observation",
"status": "final",
"category": [{
"coding": [{
"system": "http://terminology.hl7.org/CodeSystem/observation-category",
"code": "vital-signs",
"display": "Vital Signs"
}]
}],
"code": {
"coding": [
{
"system": "http://loinc.org",
"code": loinc.get("code", ""),
"display": loinc.get("display", "")
},
{
"system": "urn:iso:std:iso:11073:10101",
"code": reading.ieee_code
}
]
},
"subject": {"reference": f"Patient/{reading.patient_id}"},
"effectiveDateTime": reading.timestamp,
"valueQuantity": {
"value": reading.value,
"unit": reading.unit,
"system": "http://unitsofmeasure.org",
"code": reading.unit
},
"device": {"reference": f"Device/{reading.device_id}"}
}
return observation
def reading_to_device_alert(reading: DeviceReading, condition_text: str) -> dict:
"""Convert an alert reading to a FHIR DeviceAlert (R6)."""
return {
"resourceType": "DeviceAlert",
"status": "active",
"subject": {"reference": f"Patient/{reading.patient_id}"},
"device": {"reference": f"Device/{reading.device_id}"},
"condition": {
"coding": [{
"system": "urn:iso:std:iso:11073:10101",
"code": "68480"
}],
"text": condition_text
},
"priority": reading.alert_priority or "warning",
"timing": {
"event": [reading.timestamp]
}
}
# Usage example
reading = DeviceReading(
device_id="bedside-monitor-icu-204",
patient_id="patient-john-smith",
ieee_code="150456",
value=88.0,
unit="%",
timestamp=datetime.now(timezone.utc).isoformat(),
alert_priority="critical"
)
obs = reading_to_observation(reading)
alert = reading_to_device_alert(reading, "SpO2 below threshold (88%)")
print(json.dumps(obs, indent=2))The Integration Architecture
A production device-to-FHIR system requires several components working together. Here's the architecture we recommend for hospital deployments:
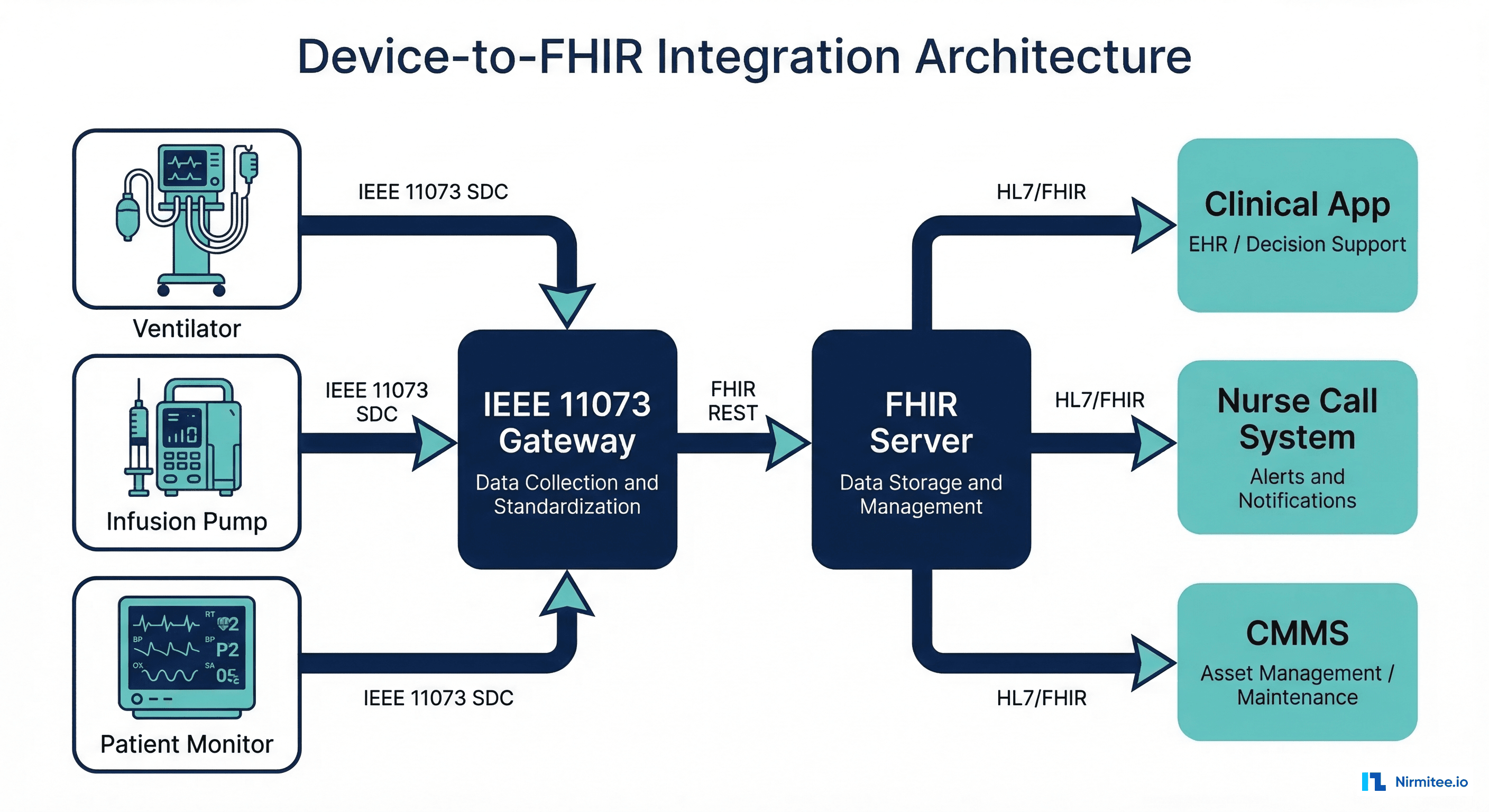
Component Breakdown
- Bedside Devices — Patient monitors (Philips, GE, Draeger), ventilators (Hamilton, Maquet), infusion pumps (BD Alaris, Baxter) generate raw IEEE 11073 data streams
- IEEE 11073 Gateway — Receives SDC streams, maintains device inventory, handles reconnection and buffering. Open-source options include sdc11073 (Python) and OpenICE
- FHIR Translation Layer — Maps IEEE 11073 objects to FHIR resources using the mapping table above. Handles batching (typically 1-second observation windows) and deduplication
- FHIR Server — Persists Observations, manages Device resources, serves queries. Must handle high write throughput (hundreds of observations per second per ICU)
- Clinical Applications — Real-time dashboards, nurse call integration, CMMS (Computerized Maintenance Management System) for device lifecycle management
Handling High-Frequency Data
A single patient monitor generates data every 1-2 seconds. An ICU with 20 beds means 200+ observations per second. Strategies for handling this volume include:
- Batch bundling — Collect observations in 5-10 second windows and POST as FHIR Bundles (type: batch)
- Observation windowing — Store min/max/mean per minute rather than every individual reading
- Async processing — Use message queues (Kafka, RabbitMQ) between the gateway and FHIR server
- FHIR subscriptions — For real-time alerting, use FHIR Subscription resources instead of polling
For teams building the FHIR server component, our guide on reading CapabilityStatements explains how to verify that the target server supports the required Device and Observation interactions.
The New R6 DeviceAlert Resource
FHIR R6 introduces the DeviceAlert resource — a long-awaited addition that gives medical device alerts their own first-class representation. Previously, device alerts were awkwardly modeled as Observations with special codes or as DetectedIssue resources, neither of which captured the full semantics of clinical device alarms.

Why DeviceAlert Matters
Alert fatigue is a recognized patient safety crisis. The Joint Commission estimates that 85-99% of clinical alarms are non-actionable. Proper alert modeling in FHIR enables:
- Alert analytics — Track alarm frequency, response times, and outcomes per device/patient/unit
- Alert prioritization — Distinguish critical (immediate life threat) from advisory (informational) alarms
- Alert routing — Direct alarms to the right clinician based on patient assignment and alert type
- Alert suppression tracking — Document when and why alarms are silenced (regulatory requirement)
DeviceAlert Structure
{
"resourceType": "DeviceAlert",
"id": "alert-spo2-critical-20260316",
"status": "active",
"subject": {
"reference": "Patient/patient-john-smith"
},
"device": {
"reference": "Device/bedside-monitor-icu-204"
},
"condition": {
"coding": [
{
"system": "urn:iso:std:iso:11073:10101",
"code": "68480",
"display": "Physiological alert condition"
}
],
"text": "SpO2 below critical threshold"
},
"priority": "critical",
"signal": [
{
"type": "annunciation",
"activeDuration": "PT45S",
"indication": {
"coding": [
{
"system": "http://terminology.hl7.org/CodeSystem/device-alert-indication",
"code": "alarm"
}
]
}
}
],
"timing": {
"event": ["2026-03-16T14:30:22Z"]
},
"derivedFrom": [
{
"reference": "Observation/spo2-reading-20260316-143022"
}
]
}Real-Time Vitals Streaming Architecture
For clinical dashboards that need sub-second updates, a pure REST-based approach (POST Observation, GET query) introduces too much latency. Modern implementations use a hybrid approach:
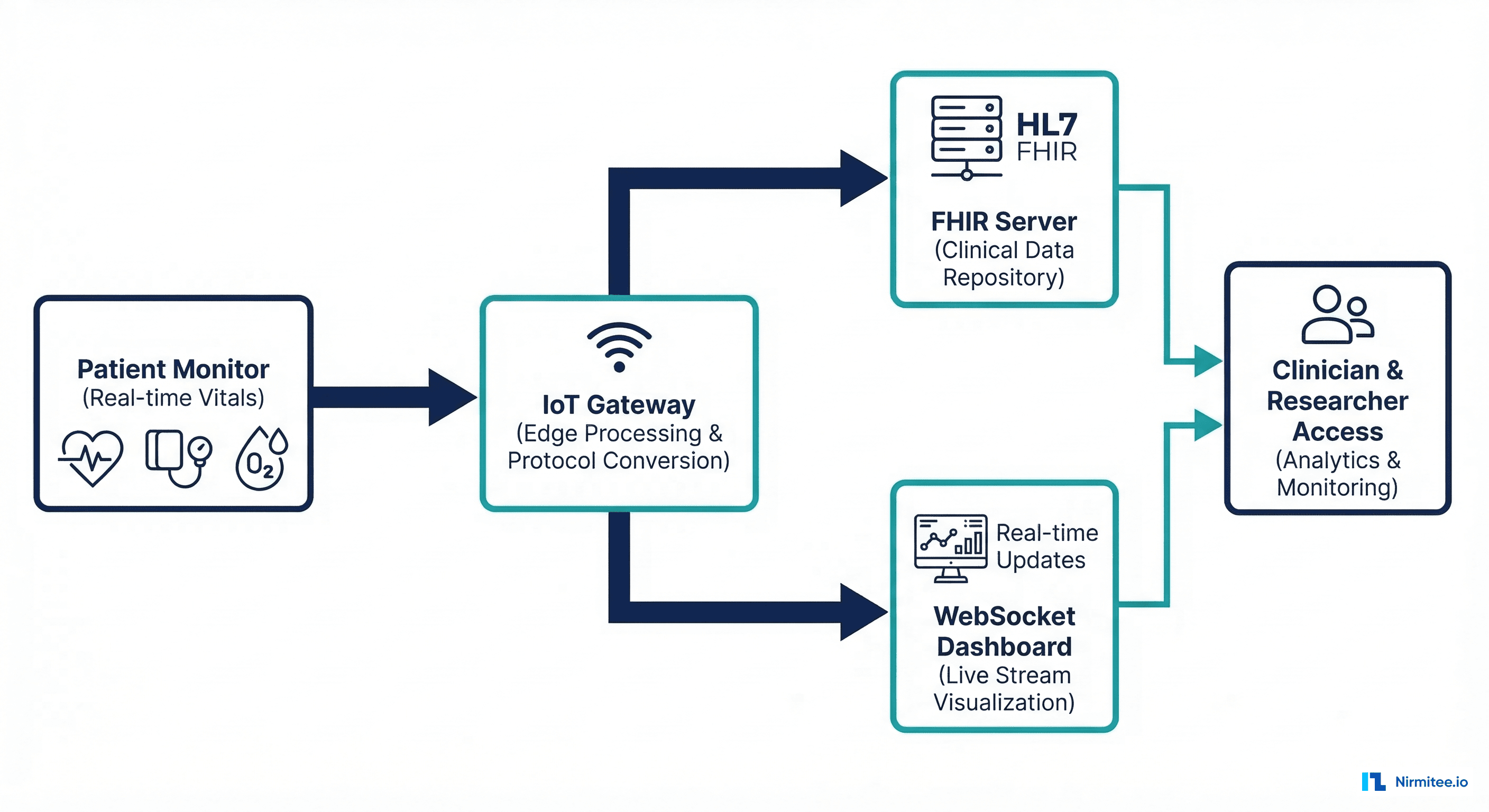
"""Real-time vitals streaming with WebSocket + FHIR persistence."""
import asyncio
import json
import websockets
from datetime import datetime, timezone
class VitalsStreamProcessor:
def __init__(self, fhir_base_url, ws_port=8765):
self.fhir_url = fhir_base_url
self.ws_port = ws_port
self.connected_clients = set()
self.observation_buffer = []
self.FLUSH_INTERVAL = 5 # seconds
self.ALERT_THRESHOLDS = {
"150456": {"low": 90, "critical_low": 85}, # SpO2
"150037": {"low": 50, "high": 120, # Heart rate
"critical_low": 40, "critical_high": 150},
}
async def process_reading(self, reading_json):
"""Process incoming device reading."""
reading = json.loads(reading_json)
# 1. Generate FHIR Observation
observation = self._to_observation(reading)
self.observation_buffer.append(observation)
# 2. Check alert thresholds
alert = self._check_thresholds(reading)
if alert:
await self._broadcast(json.dumps({
"type": "alert",
"data": alert
}))
# 3. Broadcast to WebSocket clients
await self._broadcast(json.dumps({
"type": "vital",
"data": {
"patient_id": reading["patient_id"],
"code": reading["ieee_code"],
"value": reading["value"],
"unit": reading["unit"],
"timestamp": reading["timestamp"]
}
}))
def _check_thresholds(self, reading):
"""Check if reading triggers an alert."""
thresholds = self.ALERT_THRESHOLDS.get(reading["ieee_code"])
if not thresholds:
return None
value = reading["value"]
if value <= thresholds.get("critical_low", float("-inf")):
return {"priority": "critical", "condition": f"Below critical low"}
if value >= thresholds.get("critical_high", float("inf")):
return {"priority": "critical", "condition": f"Above critical high"}
if value <= thresholds.get("low", float("-inf")):
return {"priority": "warning", "condition": f"Below low threshold"}
if value >= thresholds.get("high", float("inf")):
return {"priority": "warning", "condition": f"Above high threshold"}
return None
async def _broadcast(self, message):
"""Send message to all connected WebSocket clients."""
if self.connected_clients:
await asyncio.gather(
*[client.send(message) for client in self.connected_clients]
)This architecture delivers real-time updates to clinical dashboards via WebSocket while simultaneously batching observations for FHIR server persistence. The alert evaluation layer runs in-line, ensuring critical alarms reach clinicians within milliseconds of detection.
Integration with Nurse Call and CMMS Systems
Medical device integration extends beyond the EHR. Two critical downstream systems are:
Nurse Call Integration
When a DeviceAlert fires with critical priority, the system should automatically trigger the nurse call system. The FHIR Subscription mechanism enables this:
{
"resourceType": "Subscription",
"status": "active",
"reason": "Route critical device alerts to nurse call",
"criteria": "DeviceAlert?priority=critical&status=active",
"channel": {
"type": "rest-hook",
"endpoint": "https://nursecall.hospital.internal/api/alert",
"payload": "application/fhir+json"
}
}CMMS Integration
Device lifecycle management — maintenance schedules, calibration tracking, recall notifications — uses the Device resource's status and DeviceMetric's calibration fields. A CMMS integration polls for devices needing recalibration:
# Find devices with calibration due
GET /DeviceMetric?calibration-state=unspecified&_include=DeviceMetric:device
# Find devices with inactive status (needs maintenance)
GET /Device?status=inactive&location=Location/icu-wing-aFor teams handling the authentication layer for these integrations, our guide on SMART on FHIR authorization covers the backend service authorization flow used by system-to-system integrations.

Waveform Data in FHIR
High-frequency waveform data (ECG, invasive blood pressure, capnography) uses the FHIR SampledData type within Observations:
{
"resourceType": "Observation",
"code": {
"coding": [{
"system": "http://loinc.org",
"code": "76282-3",
"display": "Heart rate by Electrocardiogram lead"
}]
},
"valueSampledData": {
"origin": {
"value": 0,
"unit": "mV"
},
"period": 4,
"dimensions": 1,
"data": "0.2 0.3 0.5 0.8 1.2 1.8 2.1 1.5 0.8 0.3 0.1 -0.1 -0.2 0.0 0.1"
},
"device": {
"reference": "Device/bedside-monitor-icu-204"
}
}The period field (in milliseconds) defines the sampling interval. For a 250 Hz ECG, the period would be 4ms. The data field contains space-separated decimal values. For a 12-lead ECG, dimensions would be 12, with values interleaved: lead1-sample1, lead2-sample1, ..., lead12-sample1, lead1-sample2, etc.
Frequently Asked Questions
What FHIR resources represent medical devices?
FHIR uses three primary resources for medical devices: Device (the physical device with identity, manufacturer, UDI), DeviceMetric (a measurement capability like SpO2 or heart rate), and Observation (actual readings with a device reference). FHIR R6 adds DeviceAlert for clinical alarms. DeviceDefinition provides catalog-level device information (not instance-specific).
How does IEEE 11073 relate to FHIR?
IEEE 11073 is the communication protocol used by bedside medical devices. FHIR is the interoperability standard used by EHRs and clinical applications. A gateway translates between them: IEEE 11073's Medical Device System maps to FHIR Device, its Numeric Observations map to FHIR Observations, and its Alert Conditions map to FHIR DeviceAlert (R6). The IEEE 11073 nomenclature codes (like 150456 for SpO2) are used alongside LOINC codes in FHIR Observation.code.
What is the FHIR R6 DeviceAlert resource?
DeviceAlert is a new resource introduced in FHIR R6 (currently in ballot) that provides a dedicated representation for medical device alarms. It includes fields for priority (critical, warning, advisory), condition (what triggered the alert), signal (audible/visual characteristics), and timing. Previously, device alerts were modeled as Observations or DetectedIssue resources, which lacked the semantic richness needed for alert management and fatigue analysis.
How do you handle high-frequency device data in FHIR?
For numeric vitals (1-2 readings/second), batch observations in 5-10 second FHIR Bundle transactions. For waveform data (250+ samples/second), use FHIR's SampledData type which stores multiple samples in a single Observation. For real-time clinical displays, use WebSocket streaming alongside FHIR persistence rather than polling. Message queues (Kafka, RabbitMQ) between the device gateway and FHIR server absorb traffic bursts.
What is the biggest challenge in medical device FHIR integration?
The biggest challenge is protocol diversity. Most hospitals have devices from 10+ manufacturers, each using different communication protocols (IEEE 11073 SDC, serial, HL7 V2, proprietary). Building or configuring gateways for each protocol requires deep domain expertise. The second challenge is data volume — ICU devices generate orders of magnitude more data than any other clinical source, requiring careful architectural decisions about what to persist, summarize, or stream.
Can wearable devices send data to FHIR servers?
Yes. Consumer wearables (Apple Watch, Fitbit, Garmin) typically use Bluetooth LE with IEEE 11073-20601 profiles or proprietary APIs. Mobile health platforms (Apple HealthKit, Google Health Connect) can export data as FHIR Observations. The SMART Health Links specification supports sharing device-generated health data. The challenge is data quality — consumer-grade devices have different accuracy and calibration standards than clinical devices.



