Interoperability is the holy grail of healthtech; everyone talks about it, everyone wants it, but have we actually achieved it? Or is it just a distant dream, one we're forever chasing but never quite reaching?
The concept sounds simple enough: health systems and applications should be able to exchange and use patient data seamlessly, no matter where it's stored or how it's formatted. But in a world where data is fragmented across multiple systems, platforms, and standards, is true interoperability even a reality?
What Defines True Interoperability?
True interoperability isn't just about transferring data from one system to another; it's about ensuring that the data is accessible, understood, and usable across different platforms and environments. It's not just that a hospital's EHR system can share data with a patient's health app, but that the data flows seamlessly, meaningfully, and is usable by both the provider and the patient.
Have We Really Achieved It?
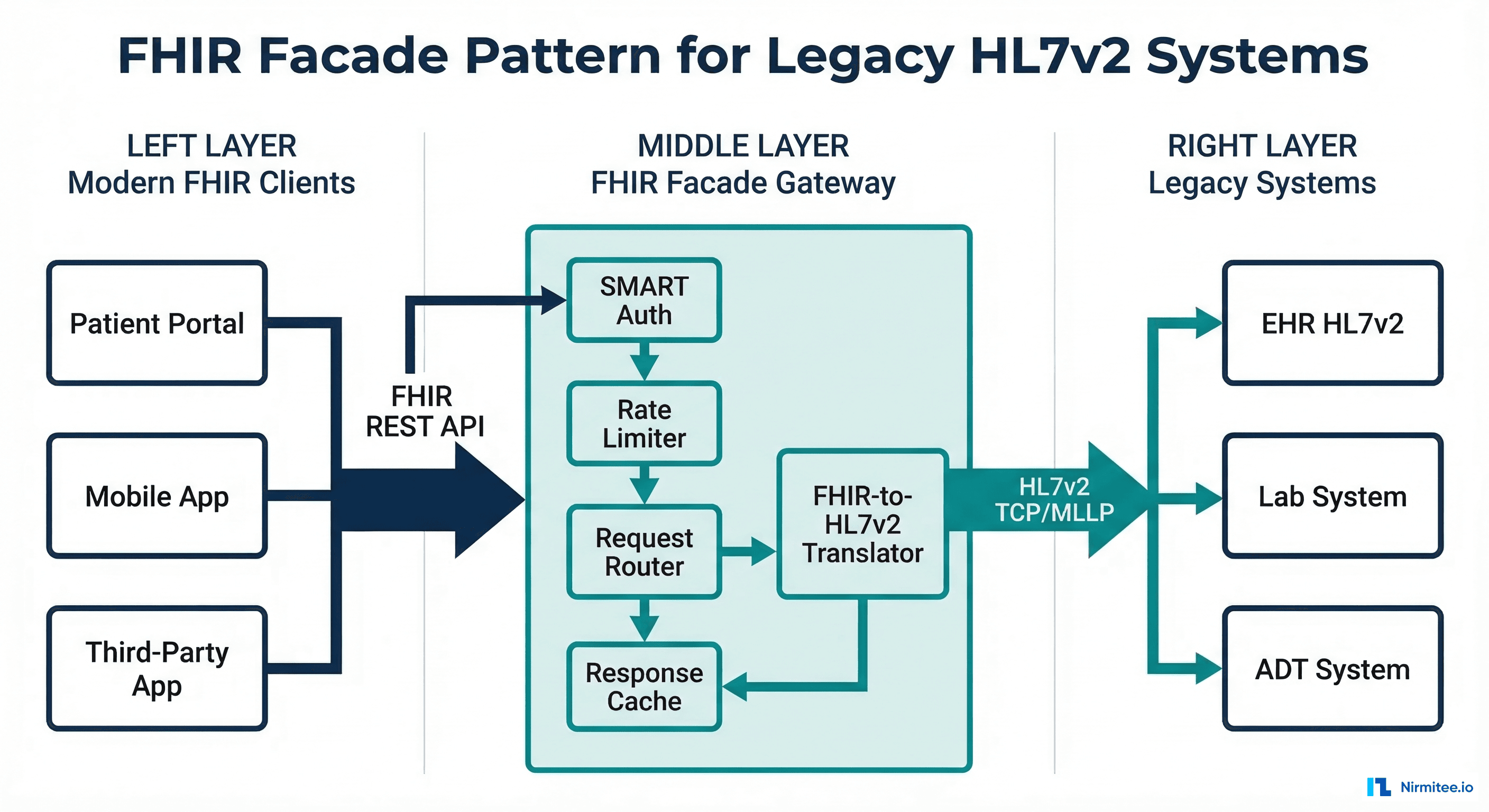
The reality is, despite advances in technology and the widespread use of data-sharing standards like FHIR (Fast Healthcare Interoperability Resources), we're not there yet.
Yes, we've made significant strides. APIs, EHRs, and Mental health apps are more connected today than they were a decade ago. We're seeing better data exchange across platforms, but when it comes to the seamless flow of information between healthcare systems, there's still a lot of work to be done.
Many healthcare providers are still working with siloed systems. A patient's medical history might be stored in one place, while their recent lab results are stored in another, and their wearable health data exists in yet another system.
While progress has been made, this fragmented approach to data management makes it challenging to achieve the kind of true interoperability we envision.
What Does the Future Look Like for Interoperability?
As the amount of health data continues to grow exponentially, the challenges of achieving interoperability are only going to increase.
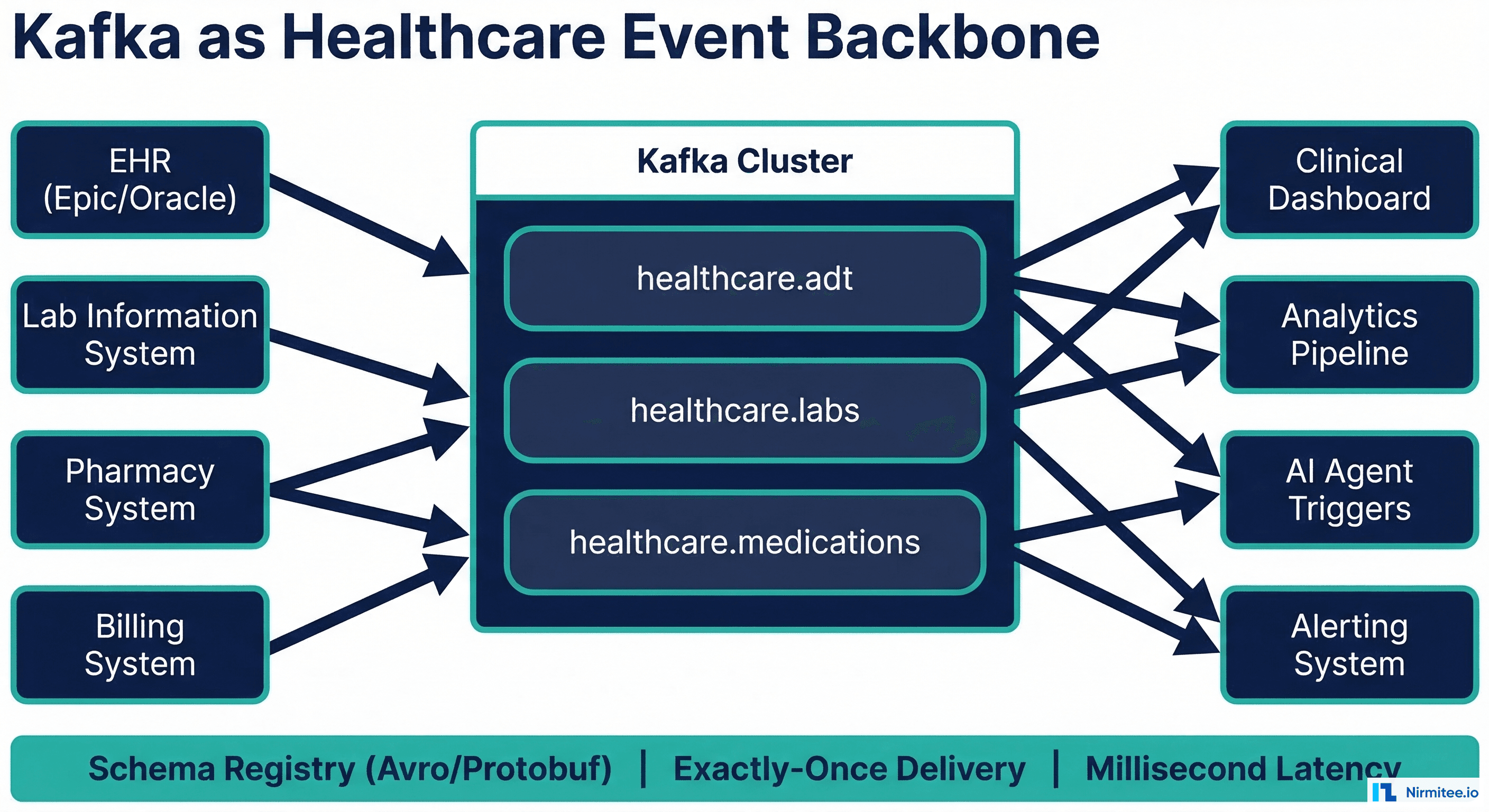
In the future, we'll be dealing with vast amounts of data, not just from traditional healthcare sources like EHRs but from wearables, genomics, AI-driven diagnostics, and remote monitoring devices. All of these data streams need to be integrated, understood, and made actionable across the entire healthcare ecosystem.
True interoperability in the future would mean that healthcare professionals and patients alike can access all relevant data, no matter its source, in a way that's immediately useful.
A patient's wearable device data, lab results, and medical history should all come together in a single, coherent picture that informs their care. For this to happen, we'll need even more sophisticated data-sharing standards and technologies that allow for real-time, meaningful data integration across all systems.
How Do Healthcare Systems Connect?
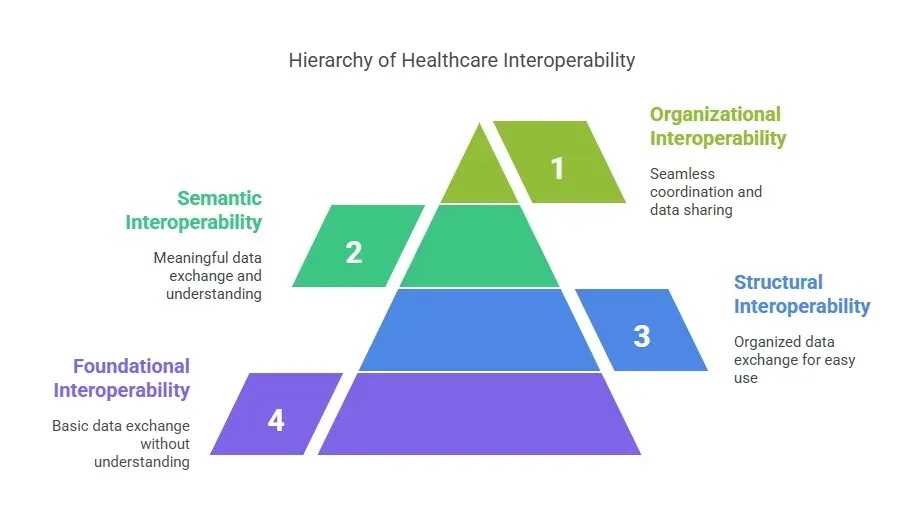
1. Foundational Interoperability
This is the most basic level, where two systems can send and receive data, but they don't necessarily understand or process the information in a useful way. It's like sending an email in a different language; the recipient receives it, but they may not be able to interpret it properly without extra effort.
Example:
A hospital's electronic health record (EHR) system sends a patient's lab test results to a specialist's system. The specialist receives the report, but if their system isn't built to interpret the data automatically, they might need to manually enter or reformat the information before using it in their workflow.
2. Structural Interoperability
At this level, data is exchanged in a structured and organized way, so different systems can understand the format of the information. This ensures that when one system sends data, another system can display it properly without extra manual work.
Example:
A telemedicine app retrieves a patient's medication history from a hospital's EHR system. Both systems use the same data format (such as FHIR API), so when the medication list is displayed in the app, it is organized and readable, without requiring a doctor to manually enter the details.
Challenge: While the data format is consistent, different healthcare systems may still interpret the same data differently, which can create inconsistencies.
3. Semantic Interoperability
This is a more advanced level where different healthcare systems not only exchange data but also understand and use it meaningfully. The information remains consistent and useful, no matter where it comes from or where it goes.
Example:
A person with diabetes wears a continuous glucose monitor (CGM) that tracks their blood sugar levels in real time. This data is automatically sent to their doctor's EHR system, which recognizes a pattern of dangerously high sugar levels. The system triggers an alert, recommending a change in medication or diet.
Challenge: Achieving true understanding between different healthcare systems requires all platforms to follow the same medical definitions and coding standards, which is not always the case.
4. Organizational Interoperability
This is the highest level, where interoperability goes beyond technology and includes policies, regulations, and workflows to ensure smooth coordination between different healthcare providers. It's about sharing the right data at the right time, while ensuring privacy and security.
Example:
A patient first visits their primary care doctor, then a specialist, and later gets surgery at a hospital. With organizational interoperability, all three providers have access to the same up-to-date patient records through a connected Health Information Exchange (HIE). This ensures:
- The specialist sees the primary doctor's diagnosis and previous treatments.
- The surgeon knows the patient's allergies and medications before surgery.
- The primary doctor receives post-surgery updates to adjust follow-up care.
Current Challenge: Many healthcare organizations still work in silos, meaning they don't always share patient data across different systems, which leads to gaps in care.
Why These Levels Matter for Patients and Healthcare Providers?
Each level of interoperability plays a role in improving healthcare. However, the higher the level, the more useful and efficient the data exchange becomes:
Basic interoperability
helps in data sharing but often requires extra effort to process and understand the information.
Advanced interoperability
ensures systems automatically recognize and use data correctly, reducing errors and improving patient care.
The goal is to reach true interoperability, where patient data flows seamlessly and meaningfully between different healthcare providers, devices, and applications.
This will lead to better diagnoses, faster treatments, and improved patient outcomes.
What's Stopping Us from Achieving True Interoperability?
So, if the technology exists, what's stopping us from achieving this vision of seamless data flow? Several key barriers still exist:
- Data Silos
Many healthcare systems still store data in isolated silos, making it difficult to share or integrate with other systems. Until these silos are broken down, interoperability will remain elusive.
- Inconsistent Standards
While frameworks like FHIR are a step in the right direction, not all systems follow the same standards. Without universal adoption of data-sharing protocols, we'll continue to see fragmented data that can't easily be integrated.
- Data Privacy & Security Concerns
The more we move data between systems, the greater the risk of breaches or misuse. Strict privacy regulations like HIPAA in the U.S. or GDPR in Europe mean that any approach to interoperability must prioritize data security, something that's often easier said than done.
- Cost & Investment
Transitioning to fully interoperable systems requires significant financial investment and a willingness to overhaul existing technologies. Many healthcare providers are hesitant to invest in the infrastructure needed to achieve true interoperability, particularly if they're already working with legacy systems.
- Technological Complexity
Even with the right standards and the right investment, the technological challenges are immense. Integrating data from a variety of sources, each with its own format, privacy considerations, and context, requires sophisticated solutions that aren't easy to implement.
Dream or Reality?
In the end, the question remains: Is true interoperability a dream or a reality? Right now, it feels like both. We've made remarkable progress, but we are still far from the ideal.
However, the future holds promise. With advancements in data-sharing protocols, AI, and decentralized technologies like blockchain, we're getting closer to a world where true interoperability could be more than just a goal; it could be our reality.
Building interoperable healthcare systems is complex. Our Healthcare Interoperability Solutions team has deep experience shipping production integrations. We also offer specialized Custom Healthcare Software Development services. Talk to our team to get started.