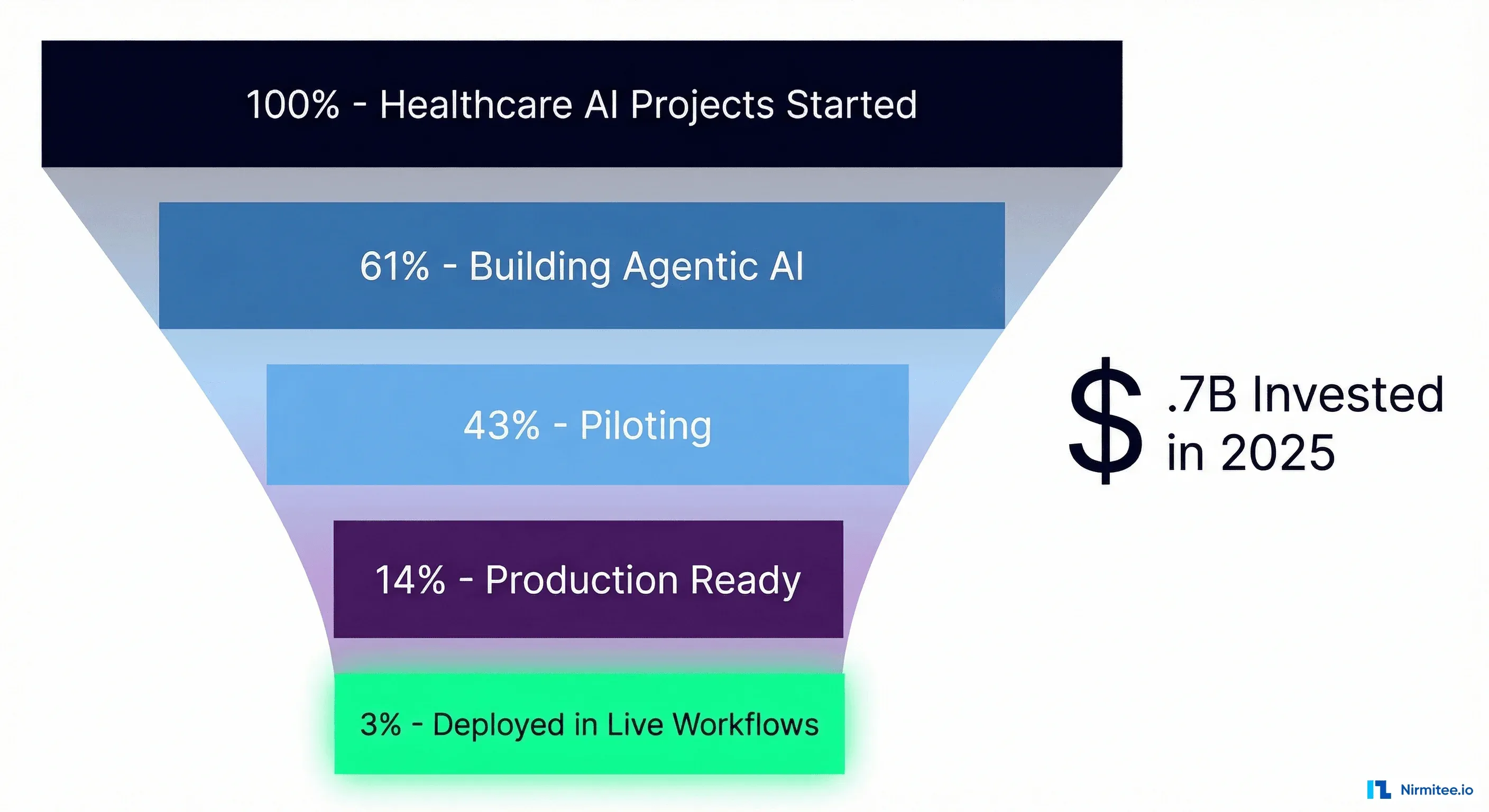
According to the ONC's interoperability data, only 43% of US hospitals routinely engage in all four domains of interoperability (find, send, receive, integrate) as of 2023 — and the gap isn't because the standards are missing. It's because integration code keeps breaking in production. If you've shipped a FHIR integration that worked on day one and was broken three weeks later, you're not alone.
This blog explains the three failure modes that make EHR integrations brittle, and why an intelligent agent layer is the only architecture that survives at scale. For the broader picture, see our pillar on AI Agents in Healthcare.
What "Intelligent EHR Integration" Means
A traditional EHR integration is static code: a FHIR client, a schema mapper, a terminology lookup, and a queue. The integration assumes the source system behaves consistently. That assumption is wrong in production.
An intelligent integration layer adds reasoning. Schema changes get detected and adapted. Semantic mismatches get translated. Edge cases get reasoned over rather than swallowed. The result is integration code that scales to 100 customers without rewriting per customer — see How AI Agents Integrate with EHR Systems for the pattern.
The Three Failure Modes
1. Schema Drift
The hospital upgrades their EHR. A custom field gets renamed. A vendor extension changes from "Observation.component" to "Observation.note". Your integration breaks silently. You find out three weeks later when a dashboard goes flat.
Static integration code is brittle to this. Every schema change is a code change. With dozens of customers, schema drift becomes a full-time job.
2. Semantic Inconsistency
The schema is identical between two hospitals. The meaning is not. Hospital A populates "Encounter.class" with "AMB" for ambulatory. Hospital B uses "ambulatory". Hospital C uses a local code. All three are technically valid FHIR. None are interoperable without translation.
This is by design. FHIR is extensible and intentionally flexible. The flexibility is what makes it adoptable. It's also what makes integrations break.
3. Edge Cases the Spec Doesn't Cover
What happens when a patient has two MRNs from a merger? When a medication quantity is "1 tab" instead of numeric? When a clinical note references an attachment that doesn't exist? When a payer responds with a non-standard error code?
The spec doesn't tell you. Every health system has its own conventions. Static integration code has no choice but to log and ignore — or break.
Why Intelligence Changes the Game
An agent-driven integration layer handles these failure modes structurally:
- Schema drift becomes a detect-and-adapt problem. The agent observes the new schema, maps fields semantically, and continues operating.
- Semantic inconsistency becomes a translation layer. LLM-based reasoning plus a terminology service resolves "AMB" and "ambulatory" to the same concept.
- Edge cases become reasoning problems. The agent looks at the unusual input, decides what it most likely means, and either acts or escalates with context.
None of this is magic. It requires careful design: tools, evaluation suites, fallbacks, audit trails. But the failure modes go away. Building AI agents with FHIR APIs covers the practical mechanics.
The Cost of Static Integration Logic
For most healthtech startups, integration maintenance is the single most expensive non-feature workstream. Common numbers we see:
- 1–2 engineers full-time on integration maintenance once you cross 10 customers
- 30–50% of customer support tickets traceable to integration drift
- Customer churn that nobody traces back to "our integration got slowly worse"
Companies don't lose customers because they lack features. They lose customers because integrations got slowly worse and nobody noticed.
What an Intelligent Integration Layer Looks Like
The reference architecture for FHIR-native healthtech teams has four layers:
- Transport — FHIR R4, HL7v2, X12 EDI. Standard.
- Schema mapper — agent-driven, semantic, learns from new fields.
- Terminology layer — SNOMED, LOINC, RxNorm plus customer-specific code maps maintained by the agent.
- Reasoning + fallback — when the agent can't resolve something, it escalates with context.
This is the difference between integrations that need a maintenance engineer per 10 customers and integrations that scale to 100 customers without adding headcount. The Agent Gateway pattern formalises this architecture.
Real-World Example
A widely-cited industry pattern: the KLAS 2024 Interoperability Report notes that even health systems with mature FHIR deployments report ongoing semantic mismatch issues when sharing data across vendors. Major systems including Mayo Clinic, Cleveland Clinic, and Intermountain have publicly described efforts to add intelligent translation layers on top of standards-compliant FHIR pipes — because the standards alone don't get them to actual interoperability. The technology stack is the same. The intelligence layer is what closes the gap.
Common Pitfalls When Building Intelligent EHR Integration
Three traps cost teams the most when they try to retrofit intelligence onto an existing integration stack:
- Treating the LLM as the integration. The LLM is the reasoning layer. The integration still needs proper FHIR clients, terminology services, error handling, and audit logs. Skipping the boring parts because "the LLM will handle it" produces integrations that look smart in a demo and break in production.
- No evaluation suite for translation accuracy. When the agent maps "AMB" to "ambulatory," is that right? When it resolves an unknown medication code, did it get it right? Without an evaluation suite — preferably one written by a clinician — you have no way to know. The bugs are silent and they compound.
- Letting the agent decide what to write back. Reading from an EHR is one risk profile. Writing back is another. Most production deployments restrict agent writes to a tightly-scoped set of resources with explicit guardrails. Treat write actions as a separate design problem, not as a side effect of read access.
Where to Start If You're Drowning in Integration Maintenance
The pragmatic path: don't try to rewrite the entire integration stack. Identify the single integration touch-point that breaks most often — usually a payer connection or a specific EHR vendor's quirks — and add an intelligent layer there first. Measure: are silent failures detected faster? Does the maintenance burden drop? If yes, expand. If no, the issue isn't the integration; it's something upstream.
Key Takeaways
- FHIR integrations don't fail because the standard is bad. They fail because the standard is interpreted differently in production.
- Three failure modes drive most breakage: schema drift, semantic inconsistency, and edge cases the spec doesn't cover.
- Static integration code grows linearly with customers and consumes engineering time.
- An intelligent layer — agent-driven mapping, terminology, and fallback — scales without per-customer rewrites.
- Your integration maintenance burden is a leading indicator of whether you need an intelligent layer.
Call to Action
This blog is one piece of a larger picture. For the full overview, read the pillar guide: What Are AI Agents in Healthcare and How Are They Transforming Care Delivery.
Want to build or evaluate an AI agent for your healthcare product? Get in touch with Nirmitee — we ship FHIR-native, HIPAA-compliant AI agents for US healthtech teams and global hospitals.