In healthcare, time is often the most critical factor. A delay of even a few seconds can have serious consequences for a patient's health outcome. Whether it's detecting early signs of a heart attack, ensuring a telemedicine session runs smoothly, or processing emergency room vitals, the speed at which health data is captured, transmitted, and analyzed matters deeply.
This blog will explore why latency in health applications is more than just a technical detail. It's a matter of life and death. We'll look at what latency means in a medical context, how real-time architectures are reshaping care delivery, what technologies enable this shift, and why developers and healthcare providers must prioritize real-time design to build safe, scalable, and impactful digital health solutions.
Understanding Latency in Healthcare
Latency, in simple terms, is the delay between when data is generated and when it's available for use. In healthcare applications, this could mean the lag between a wearable device detecting a drop in oxygen levels and that data being displayed on a physician's dashboard.
Why does this matter? Because health data is time-sensitive. A delay in interpreting vital signs could result in missed red flags. For example, if a sepsis detection system operates with high latency, it might fail to detect early warning signs in time for a physician to intervene.
In emergency departments, even real-time display systems such as wait-time dashboards can be misleading if updated data is delayed, leading to poor patient flow and inefficient resource use.
Why Real-Time Architecture Matters in Health Apps
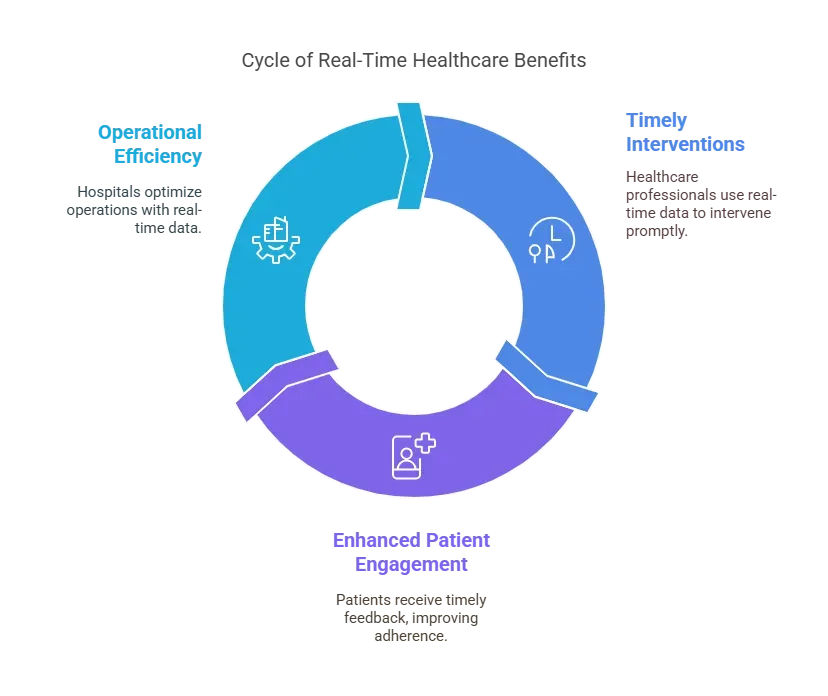
1. Timely Interventions Save Lives
Healthcare professionals need access to accurate, real-time data to intervene at the right moment. Systems like HCA Healthcare's S-P-O-T utilize real-time AI to flag sepsis indicators based on patient vitals. The faster the system reacts, the better the outcomes. In time-sensitive conditions like strokes, cardiac arrests, or sepsis, even seconds can determine the difference between recovery and irreversible damage.
2. Enhancing Patient Engagement
Patients are more likely to adhere to treatment plans when they receive timely feedback. Real-time updates on blood pressure, glucose levels, or medication reminders empower individuals to stay on top of their health. Apps like CareAssure and CareLink provide instant alerts to both patients and caregivers, making care more proactive and less reactive.
3. Operational Efficiency
Hospitals and clinics benefit significantly from real-time data to streamline operations. Whether it's optimizing staff schedules, tracking bed availability, or maintaining a real-time inventory of medical supplies, low-latency data makes these processes more effective. For example, updating ER wait times in real-time helps prevent bottlenecks and overcrowding, improving patient experience and resource utilization.
Building the Backbone: Tech Stack Essentials for Real-Time Health Apps
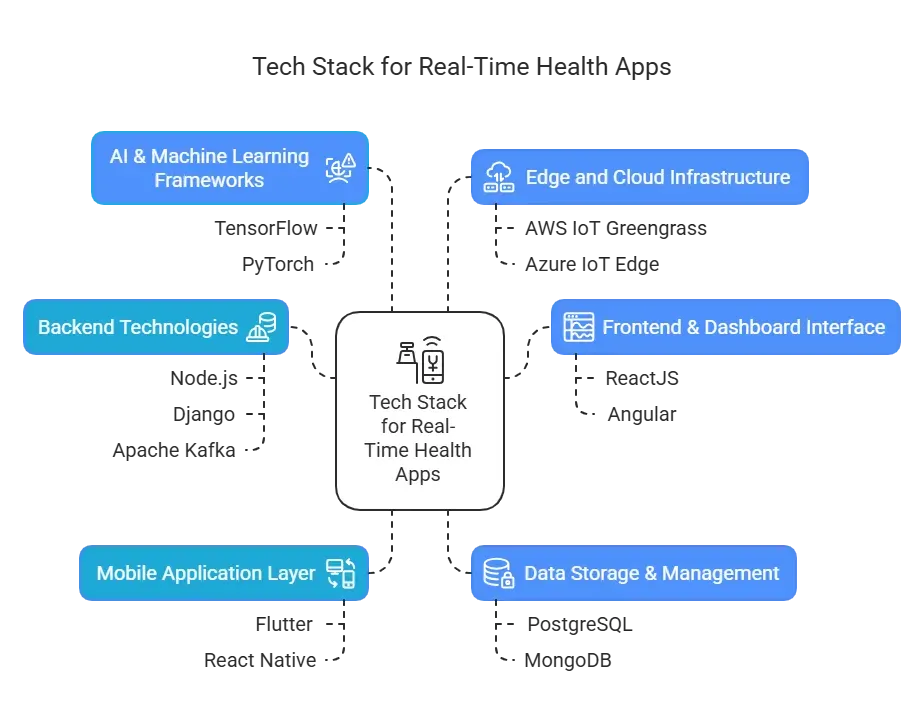
Backend Technologies
Robust backends are the backbone of any real-time health system. Node.js is excellent for building fast, event-driven architectures, especially for applications requiring live updates, like telehealth sessions or real-time symptom tracking. Django, with its built-in security features, offers a strong foundation for HIPAA-compliant apps. For managing real-time data streams from wearables or remote patient monitoring systems, Apache Kafka ensures high-throughput and fault-tolerant message processing.
Frontend & Dashboard Interface
On the frontend, ReactJS or Angular allows developers to build responsive, real-time dashboards - ideal for visualizing patient vitals or appointment updates. These frameworks support dynamic components that refresh instantly as new data comes in, improving clinician workflow and patient experience.
Mobile Application Layer
To ensure broad accessibility and device compatibility, Flutter and React Native are great choices for cross-platform development. They allow you to build one app that works smoothly on both iOS and Android, which is critical for patient engagement apps or mobile-first monitoring tools.
Data Storage & Management
Healthcare apps deal with large volumes of sensitive data. PostgreSQL offers relational integrity and performance, while MongoDB brings flexibility, which is especially useful when handling unstructured data like notes or questionnaire responses. Both are scalable and support encryption, a must for protecting health records.
AI & Machine Learning Frameworks
When it comes to predictive analytics, TensorFlow and PyTorch are industry-standard. They allow healthcare apps to detect anomalies in vitals, predict patient risk levels, or suggest interventions - all in real-time.
Edge and Cloud Infrastructure
For ultra-low latency and on-site processing, AWS IoT Greengrass or Azure IoT Edge enables real-time analysis close to where data is generated - be it a wearable device or a hospital bed. This reduces the delay of sending data to the cloud and back, a key requirement in time-sensitive healthcare environments.
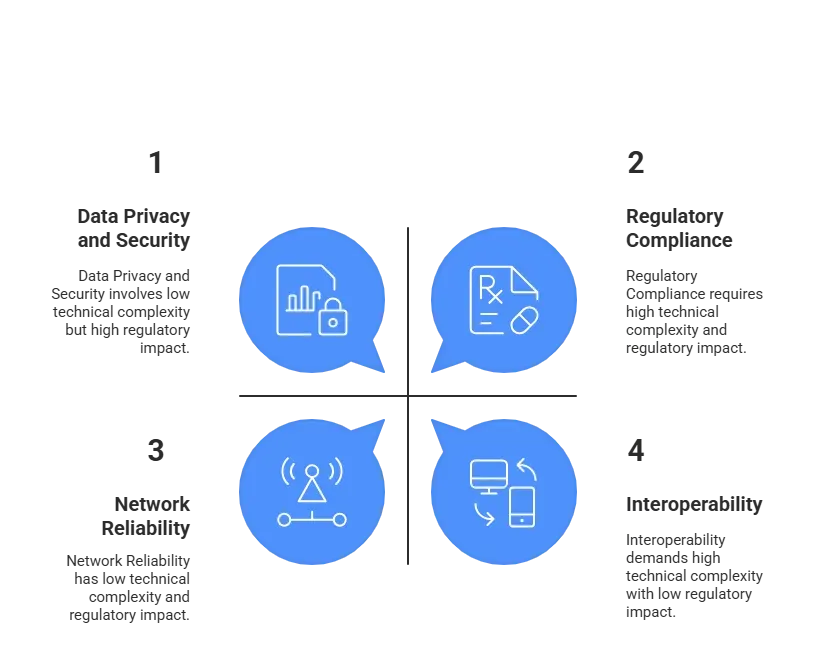
Challenges in Implementing Low-Latency Real-Time Healthcare Apps
Regulatory Compliance
Meeting compliance requirements like HIPAA in the U.S., GDPR in Europe, and HL7 standards worldwide is non-negotiable. These regulations affect everything from data storage to audit trails and demand strong encryption and access controls.
Interoperability
Legacy EHR systems like Epic and Cerner often use different data formats. Integrating with them requires the use of standard APIs like FHIR and HL7. Achieving seamless interoperability while maintaining low latency is a technical and strategic challenge.
Network Reliability
Not all healthcare settings have robust internet infrastructure. Remote clinics and field operations must rely on edge computing and network redundancy to maintain real-time performance even in low-bandwidth conditions.
Data Privacy and Security
Real-time processing involves continuous data flows, which makes securing these pipelines critical. Encryption at rest and in transit, role-based access controls, and strict user authentication protocols are essential to ensure data privacy.
Future Trends and Innovations
As real-time healthcare architecture evolves, the next wave of innovations is bringing even greater speed, precision, and autonomy to digital health solutions. The following emerging technologies are set to redefine what's possible in real-time care:
1. Agentic AI and Autonomous Health Systems
Agentic AI goes a step beyond traditional models by introducing autonomy and proactive behavior. These AI agents aren't just waiting for commands; they monitor patient data continuously, detect anomalies, reason through potential outcomes, and initiate actions independently.
In real-time healthcare, this could mean an AI agent automatically contacting a provider when a patient's vitals cross a critical threshold or modifying medication reminders based on real-time adherence patterns.
This shift toward autonomous health systems could dramatically reduce clinician burden and ensure timely interventions, especially in chronic disease management and home-based care.
2. RAG (Retrieval-Augmented Generation) and CAG (Context-Aware Generation)
RAG and CAG represent the next generation of AI language models, ones that don't just generate responses from fixed training data but actively pull in up-to-date, relevant information in real time.
In healthcare, this means an AI assistant can access a patient's medical history, current medications, or recent lab results before responding to a query or making a suggestion. RAG enables dynamic retrieval, while CAG ensures the model understands the specific context of the user or clinical case.
Together, they bring greater accuracy, personalization, and safety to AI-supported triage, symptom checkers, or even real-time decision support tools for clinicians.
3. Predictive and Prescriptive Analytics in Real Time
While predictive analytics is already improving early detection of conditions like sepsis, the future lies in real-time predictive and prescriptive intelligence. These systems won't just flag potential problems - they'll recommend and even initiate preventive measures.
For example, if a wearable detects early signs of atrial fibrillation, the app could suggest dietary changes, alert caregivers, and pre-book a virtual consultation - all autonomously and instantly. This evolution marks the transition from reactive to proactive care models, where data not only informs decisions but drives interventions in real time.
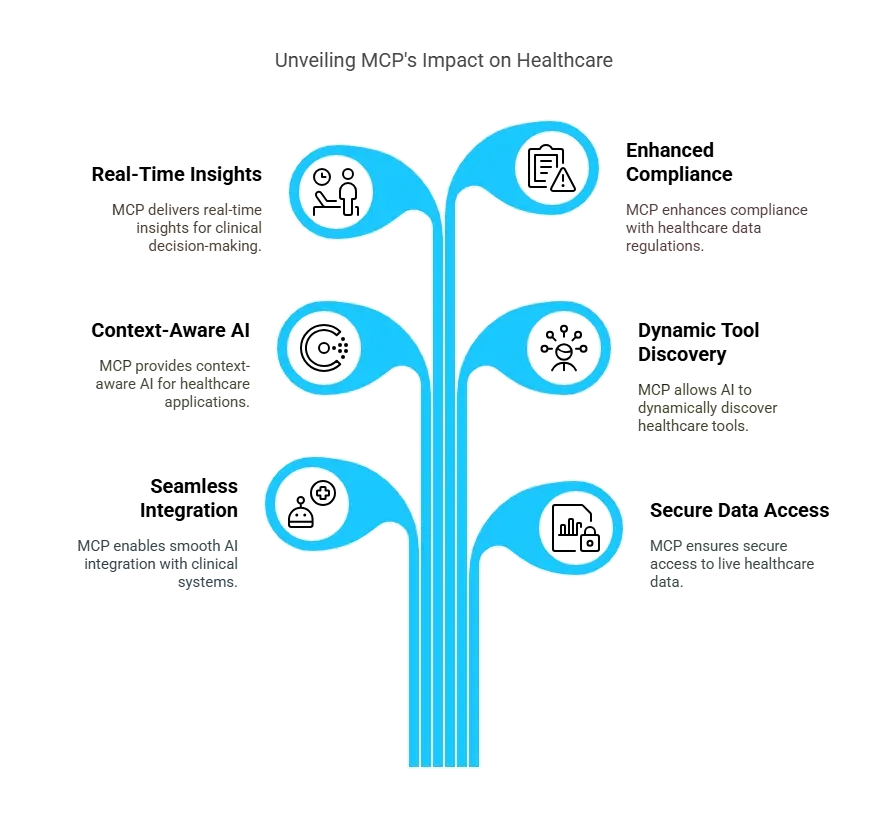
The Role of MCP in Real-Time Healthcare Architecture
The Model Context Protocol (MCP) is rapidly emerging as a foundational technology for real-time healthcare applications, addressing one of the industry's biggest challenges: seamless, secure, and context-aware integration between AI models and diverse clinical systems.
MCP acts as a universal adapter, allowing AI, such as large language models or digital assistants, to securely connect with APIs, EHRs, and operational tools in real time.
This means that instead of relying on rigid, custom integrations or manual prompt engineering, healthcare organizations can expose their internal services as standardized MCP tools, enabling AI to dynamically discover, access, and act on live data across the enterprise.
The result is a new generation of intelligent healthcare apps that can provide clinicians with up-to-date patient information, automate workflows, and deliver actionable insights at the point of care - all while maintaining strict auditability, compliance, and data governance.
By bridging fragmented IT systems and empowering AI to act safely and predictably, MCP is transforming real-time healthcare architecture and enabling truly responsive, life-saving digital solutions.
Conclusion
In the evolving world of digital healthcare, latency isn't just a technical challenge; it's a matter of patient safety and clinical success. Real-time architecture empowers faster diagnoses, timely interventions, and proactive care, ultimately saving lives.
Building such systems requires the right mix of technology, regulatory knowledge, and development expertise. Partnering with healthcare-focused developers who understand these nuances is essential.