Your healthtech product works. You've proven it at one hospital, maybe two. The integration was painful — custom HL7 interfaces, weeks of testing, late-night calls with the hospital's interface analyst. But it works. Now, sales has 15 more hospitals in the pipeline, and the CEO wants to know: "How fast can we onboard them?"
The answer depends entirely on whether you built your integration for one hospital or for a hundred. This guide covers the engineering strategy for scaling from MVP to enterprise-grade EHR connectivity.

The MVP Integration Trap
At the MVP stage, your integration probably looks like this: a single connection to a single EHR instance, custom-built for that hospital's specific configuration. Maybe it's an HL7v2 ADT feed, maybe it's a direct FHIR connection to their Epic instance. It works, but it's brittle, manual, and non-transferable.
The trap is assuming that onboarding hospital #2 will take the same effort as hospital #1. It won't — it might take more, because:
- Hospital #2 runs a different EHR (Cerner instead of Epic)
- Same EHR vendor, but different version, different modules enabled, different custom fields
- Different network topology (VPN requirements, firewall rules, IP whitelisting)
- Different IT teams with different processes, timelines, and risk tolerance
- Different data quality — missing fields you assumed would always be present
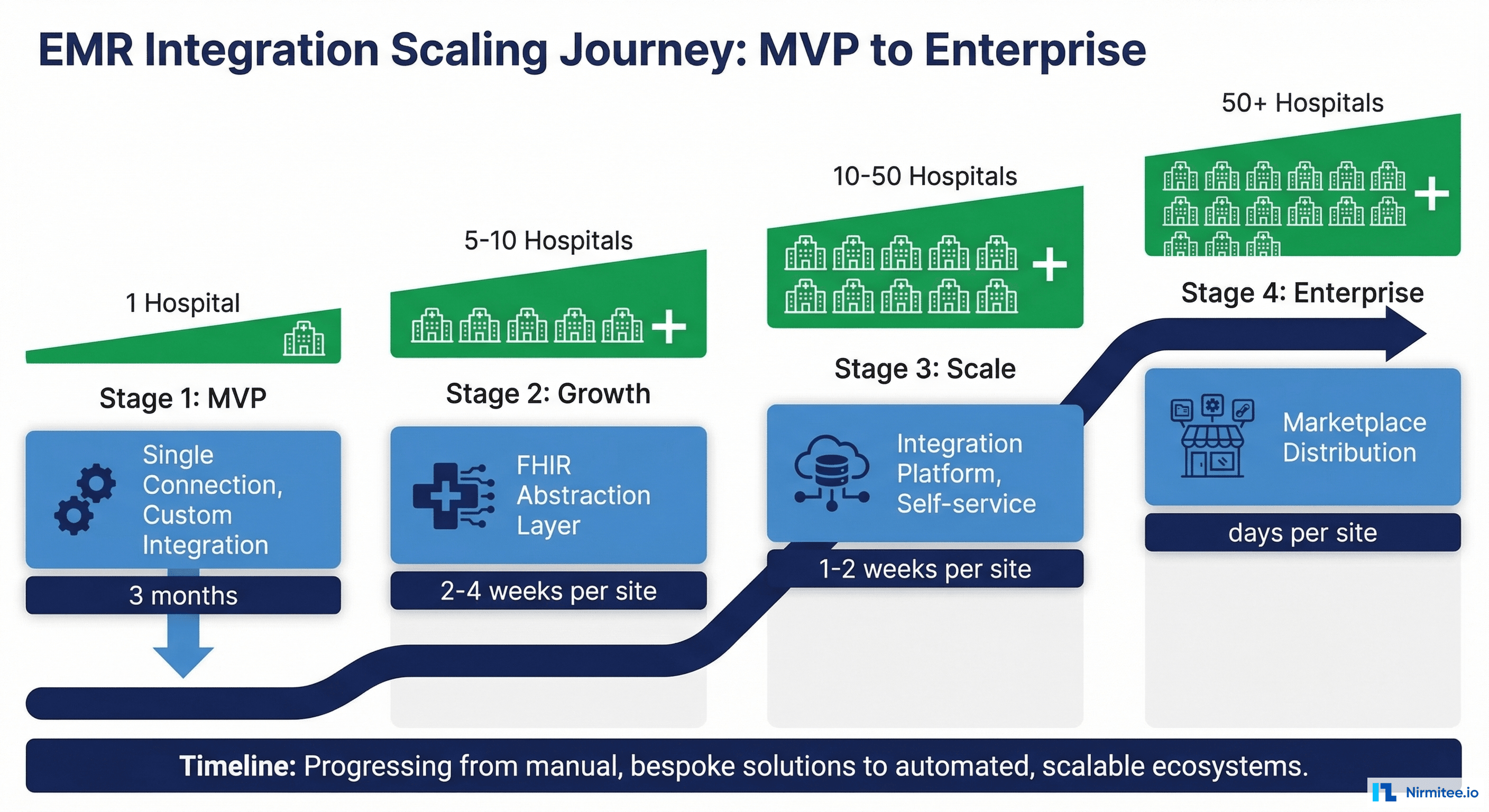
The Four Stages of Integration Maturity
Stage 1: Custom (1-2 hospitals, 2-6 months per site)
Every connection is hand-built. The integration engineer knows each hospital's quirks by heart. Onboarding requires code changes, custom deployment, and manual testing. This is fine for proving product-market fit, but it doesn't scale.
Stage 2: Standardized (5-10 hospitals, 2-4 weeks per site)
You've built a FHIR abstraction layer that normalizes the differences between EHR implementations. New hospitals are configured, not coded. You have adapters for Epic, Cerner, and maybe MEDITECH. Onboarding is still engineer-led but follows a repeatable playbook.
Stage 3: Platform (10-50 hospitals, 1-2 weeks per site)
Self-service onboarding tools let your customer success team configure new connections without engineering involvement. Automated testing validates data flow before go-live. You have monitoring dashboards, SLA tracking, and incident management.
Stage 4: Marketplace (50+ hospitals, days per site)
Your app is certified on Epic App Market, Oracle Health app gallery, and other EHR marketplaces. Hospitals install your app like an iPhone app — click, authorize, done. Integration is a feature of the EHR ecosystem, not a separate project.
Building the FHIR Abstraction Layer
The key architectural investment for Stage 2 is a FHIR abstraction layer that sits between your application and the EHR ecosystem. Even though FHIR is a standard, every EHR implements it differently:

class FHIRAbstractionLayer:
"""Normalizes FHIR implementation differences across EHR vendors."""
def __init__(self):
self.adapters = {
"epic": EpicAdapter(),
"cerner": CernerAdapter(),
"meditech": MEDITECHAdapter(),
"athena": AthenaAdapter(),
}
def get_patient(self, tenant_config: dict, patient_id: str) -> dict:
"""Get patient data, normalized across EHR differences."""
adapter = self.adapters[tenant_config["ehr_vendor"]]
raw = adapter.fetch_patient(tenant_config, patient_id)
return self.normalize_patient(raw, tenant_config)
def normalize_patient(self, raw_patient: dict, config: dict) -> dict:
"""Handle vendor-specific extensions and field mapping."""
normalized = {
"id": raw_patient["id"],
"mrn": self._extract_mrn(raw_patient, config),
"name": self._extract_name(raw_patient),
"dob": raw_patient.get("birthDate"),
"gender": raw_patient.get("gender"),
}
# Epic stores MRN in a specific identifier system
# Cerner uses a different system URI
# The adapter handles this transparently
return normalized
def _extract_mrn(self, patient: dict, config: dict) -> str:
"""Extract MRN from vendor-specific identifier systems."""
mrn_system = config.get("mrn_system_uri")
for identifier in patient.get("identifier", []):
if identifier.get("system") == mrn_system:
return identifier["value"]
return NoneThe EHR Market Reality
You don't need to integrate with every EHR. Focus on market share:
- Epic: ~38-40% of US acute care hospitals. Non-negotiable — almost every health system RFP requires Epic integration.
- Oracle Health (Cerner): ~25%. Second priority. Covers the VA, DOD, and many mid-size health systems.
- MEDITECH: ~16%. Critical for community hospitals, which are often your easiest sales.
- athenahealth: ~8%. Strong in ambulatory/outpatient settings.
Epic + Oracle Health + MEDITECH = ~80% market coverage. Add Athena, and you're at ~88%. That's your integration roadmap priority.
Self-Service Onboarding Pipeline
At Stage 3, your onboarding should be a structured pipeline, not ad-hoc engineering:
- Configure EHR adapter: Select vendor, enter FHIR endpoint URL, configure auth credentials
- Test connection: Automated health check — can we authenticate? Can we read a Patient resource?
- Map custom fields: Hospital-specific identifier systems, custom extensions, local code mappings
- Validate data: Pull sample data for 10 patients, verify all expected fields are populated
- Load test: Simulate production query volume, verify response times under load
- Go live: Enable production traffic with monitoring and alerting active
Build vs Buy: Integration Platforms
You don't have to build everything yourself. Integration platforms can accelerate your timeline:
- Redox: Most widely used healthtech integration platform. Pre-built connections to 500+ health systems. Best for startups that need to ship fast.
- Health Gorilla: Strong in clinical data aggregation. Good for apps that need comprehensive patient records across providers.
- Particle Health: Claims and clinical data from national networks. Good for population health and analytics use cases.
- Direct FHIR: Build your own connections for maximum control, lowest per-transaction cost, and deepest EHR functionality. Best when you've validated your integration patterns and need to optimize cost at scale.
Our recommendation: Start with a platform (Redox) for your first 10 hospitals to validate your integration patterns and get to market fast. Then build direct FHIR connections for your top 2-3 EHR targets to reduce costs and unlock deeper functionality.
Working with Hospital IT Teams
The technical integration is half the battle. The other half is navigating hospital IT processes:
- Security reviews: Every hospital has its own HIPAA security questionnaire. Build a master response document and keep it up to date. Budget 2-4 weeks for the review process.
- Change management: Hospital IT teams have change windows (often Tuesday and Thursday evenings). Plan your go-lives accordingly.
- Interface analysts: These are your best friends. They know where every HL7 message goes and which FHIR endpoints are configured. Build relationships early.
- Downtime coordination: EHR systems have scheduled maintenance windows. Your integration must handle downtime gracefully — queue messages, retry with backoff, and alert on extended outages.
For a complete framework on the build vs buy decision, see our EHR integration decision guide. For a case study on building a unified FHIR facade across multiple EHRs, read about our multi-EHR FHIR facade.
At Nirmitee, we help healthtech companies scale from MVP integrations to enterprise-grade EHR connectivity. Whether you need a FHIR abstraction layer, multi-tenant architecture, or self-service onboarding tooling, let's talk.
Need expert help with healthcare data integration? Explore our Healthcare Interoperability Solutions to see how we connect systems seamlessly. We also offer specialized Healthcare Software Product Development services. Talk to our team to get started.