The Numbers That Should Keep Healthcare CIOs Awake
The average cost of IT downtime across all industries is $7,900 per minute, according to Ponemon Institute research. But healthcare is not an average industry. When a hospital's EHR goes down, the cost is not just the $7,900 per minute in IT terms -- it is the clinician who cannot see a patient's allergy list before prescribing, the lab technician whose critical results sit in a queue undelivered, the emergency department that diverts patients because it cannot safely admit without electronic records. The clinical cost of healthcare IT downtime is fundamentally different from the cost of a retail website going offline.
According to HIMSS survey data, 96% of healthcare organizations experienced at least one unplanned outage in the past year, with an average of 18 outage events per organization. The median downtime duration was 4 hours per event. For a mid-size health system with 200 providers, that translates to millions in lost revenue, increased clinical risk, and regulatory exposure. Yet most healthcare organizations cannot quantify this cost -- which means they cannot build a credible business case for reliability investment.
This guide provides a complete framework for calculating the business and clinical impact of system failures, building the ROI case for reliability investment, and presenting it to your CIO and CFO in terms they understand. We include a downtime cost calculator, clinical impact severity matrix, and a sample business case presentation framework.

Revenue Impact: Where the Money Goes
Revenue loss during healthcare IT downtime comes from multiple sources, each compounding the other. Understanding each revenue stream's sensitivity to downtime is essential for building an accurate cost model.

| Revenue Source | Impact During Downtime | Hourly Cost Estimate | Recovery Time |
|---|---|---|---|
| Outpatient Visits | Cancellations and no-shows increase 3x, providers see 60% fewer patients | $500-2,000 per provider | Hours to reschedule |
| Lab Services | Orders cannot be placed electronically, results not delivered, STAT labs delayed | $15,000-45,000 | 8-24 hours to clear backlog |
| Radiology/Imaging | PACS unavailable means studies cannot be read, procedures postponed | $25,000-38,000 | 4-8 hours backlog |
| Pharmacy | E-prescribing fails, medication reconciliation manual, discharge Rx delayed | $8,000-12,000 | 2-4 hours |
| Billing/Revenue Cycle | Charge capture drops 33%, claims submission halted, denials increase | $20,000-50,000 | Days to weeks |
| Elective Procedures | Surgeries postponed if pre-op records unavailable | $5,000-50,000 per case | Days to reschedule |
The billing impact is particularly insidious because it extends well beyond the downtime window. When clinicians switch to paper-based workflows, charge capture drops from 98% to roughly 65%. Those missing charges are often never recovered -- the documentation is incomplete, the encounter was not coded properly, and by the time the system is back online, the details are lost. A 4-hour EHR outage can result in 2-3 weeks of revenue cycle cleanup.
Clinical Impact: The Costs You Cannot Put a Dollar Sign On
While revenue loss gets the CFO's attention, clinical impact is what should drive the urgency. Research from the Agency for Healthcare Research and Quality (AHRQ) shows that medication errors increase 5x during EHR downtime because clinicians lose access to allergy lists, drug interaction checking, and medication reconciliation tools.
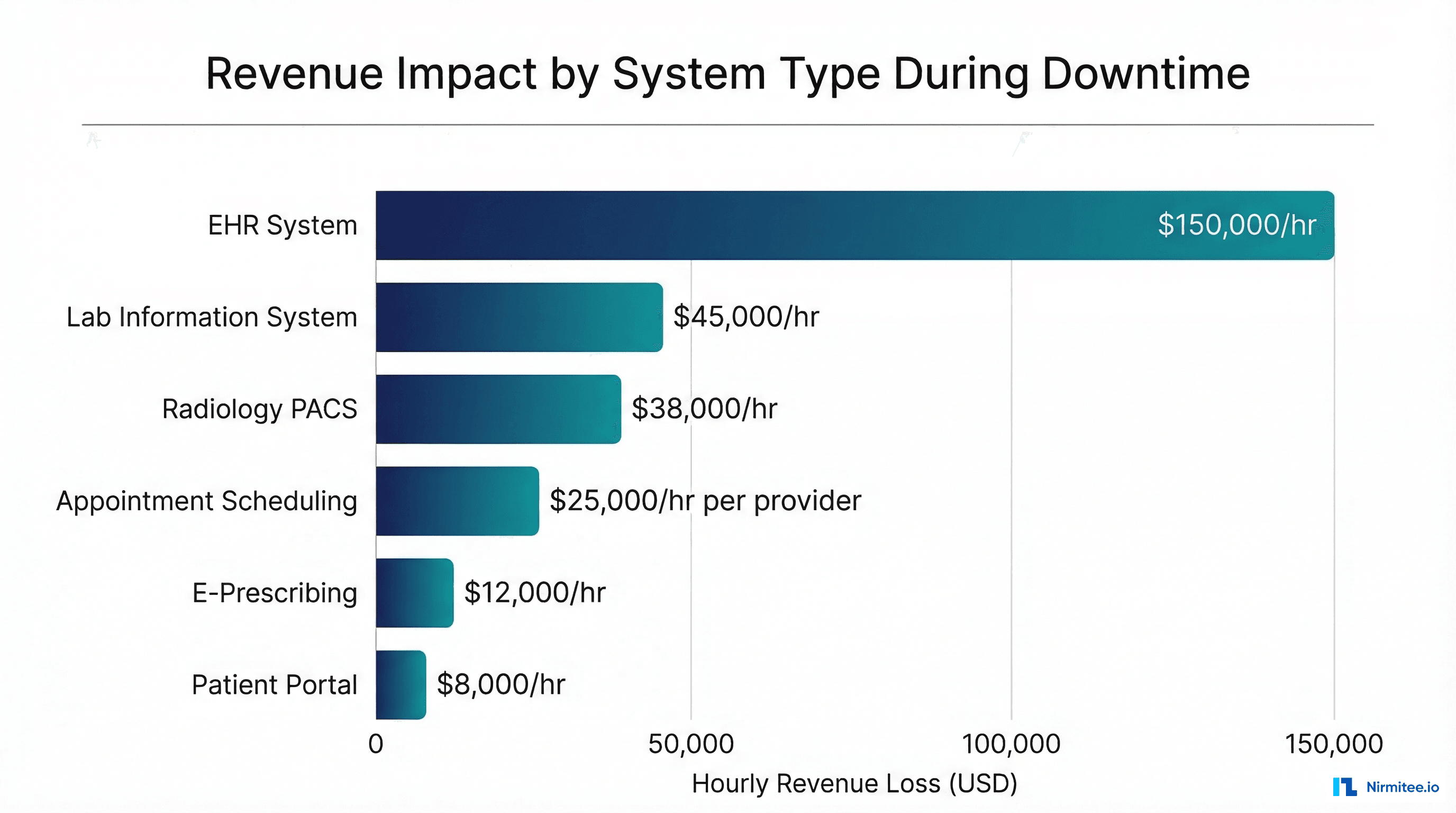
Clinical Impact by System
| System | Clinical Risk During Downtime | Documented Incidents |
|---|---|---|
| EHR (Epic, Cerner) | Medication errors 5x, allergy checks unavailable, vitals not trended, orders verbal only | Multiple sentinel events reported to Joint Commission during major EHR outages |
| Lab Information System | Critical lab values not delivered to clinicians, STAT results delayed 4-8 hours | Delayed critical potassium result leading to cardiac event (case studies) |
| Pharmacy System | Drug-drug interaction checking unavailable, dosing calculators offline | Wrong-dose errors during downtime reported in ISMP newsletters |
| Radiology PACS | Prior studies unavailable for comparison, emergency reads delayed | Missed comparison studies leading to delayed diagnoses |
| Patient Monitoring | Alarm fatigue workarounds, vital signs not trended electronically | Monitoring gaps during system transitions |
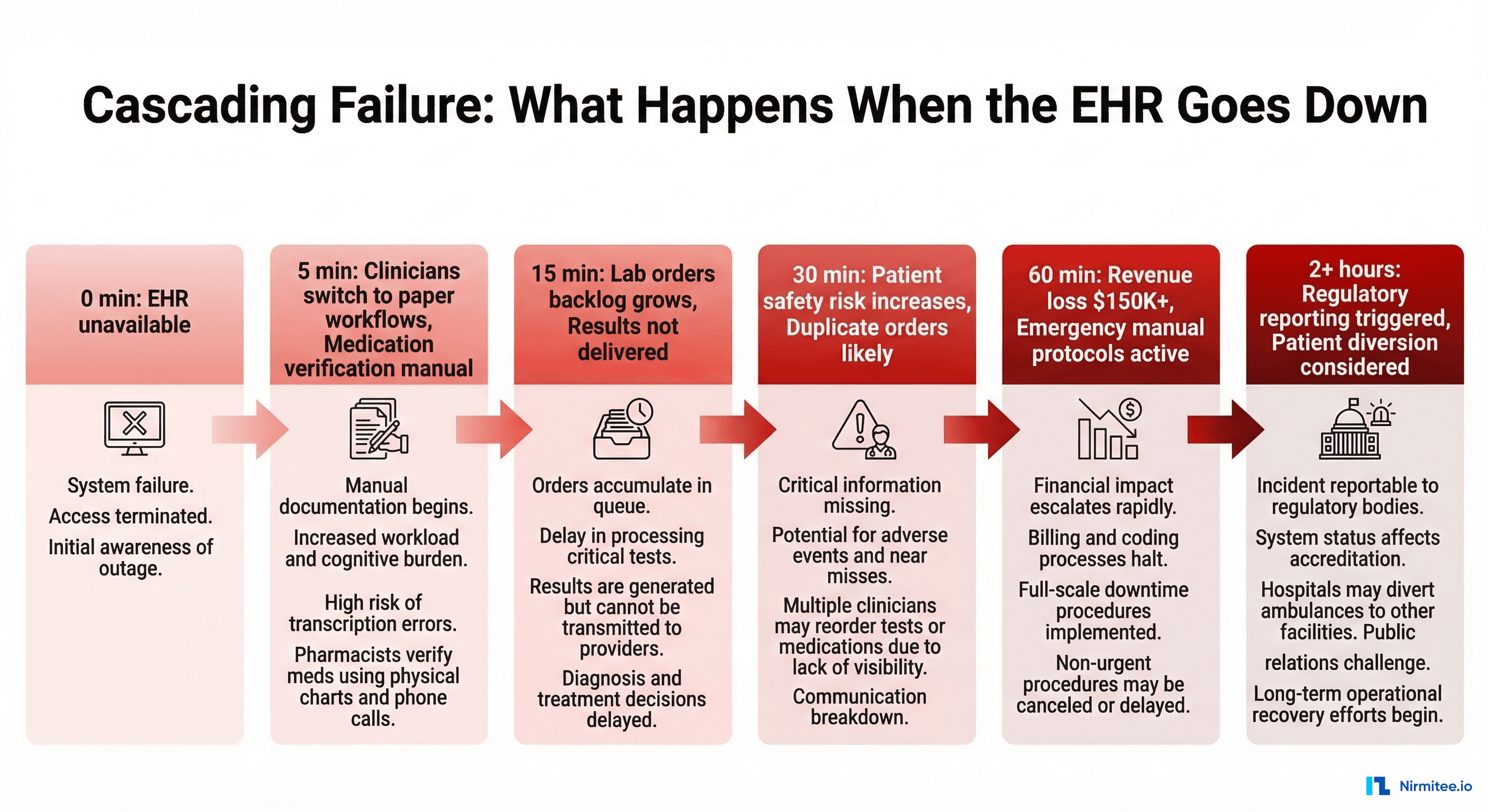
The Cascading Failure Timeline
Healthcare IT failures do not happen in isolation. They cascade across departments, creating a compound effect that multiplies the impact at each stage:
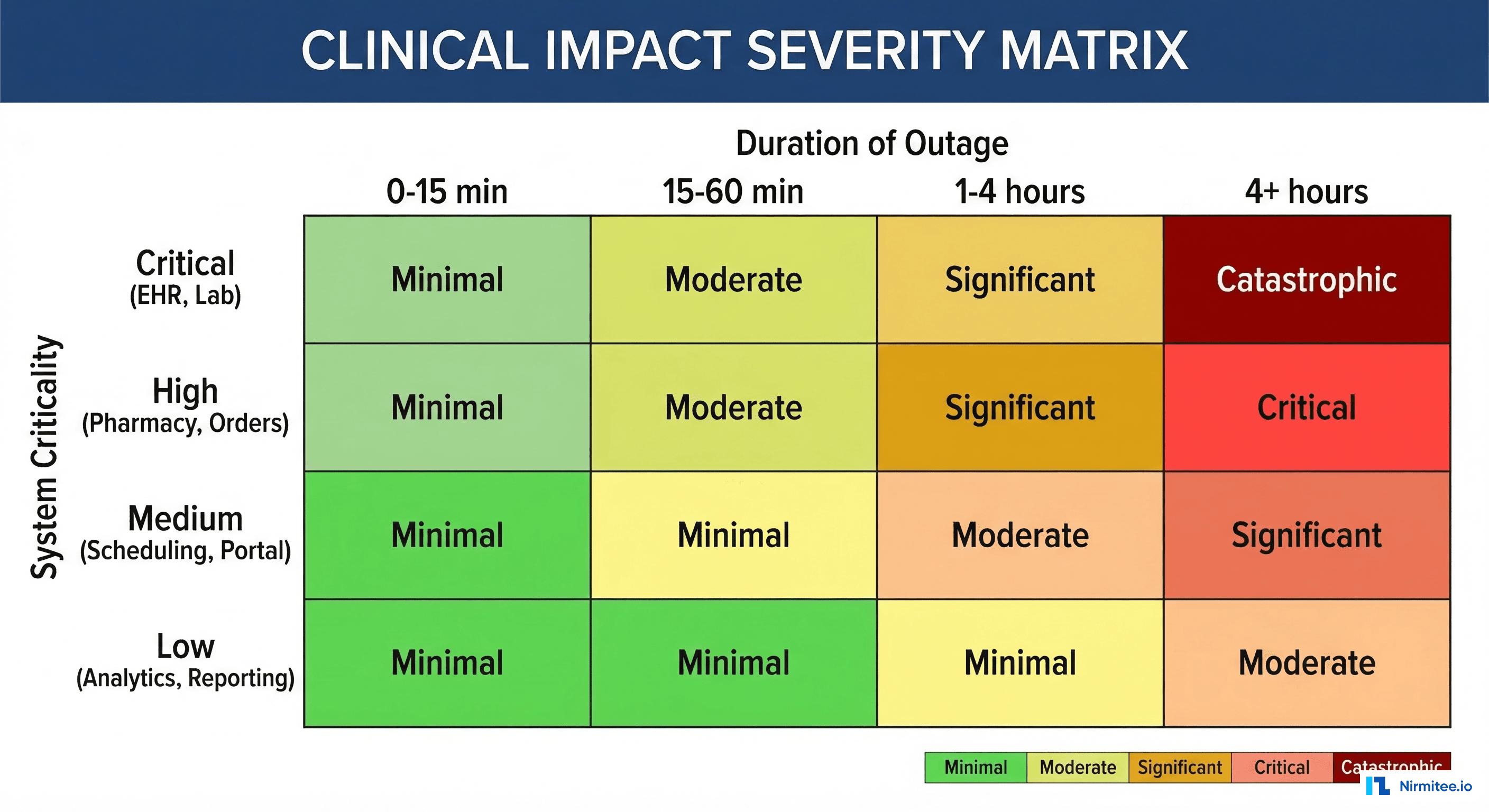
| Time | What Happens | Impact |
|---|---|---|
| 0-5 minutes | System unavailable, IT helpdesk flooded, clinical staff attempt workarounds | Minor disruption, staff frustration |
| 5-15 minutes | Paper-based downtime procedures activated, medication orders go verbal | Workflow efficiency drops 60%, error risk increases |
| 15-30 minutes | Lab orders backlog, results undelivered, scheduled appointments disrupted | Revenue loss begins, clinical delays accumulate |
| 30-60 minutes | Elective procedures postponed, patient flow bottleneck, ED diversion considered | $150K+ revenue impact, patient safety at risk |
| 1-4 hours | OR cases delayed, discharge process manual, admission holds, staff overtime | Major revenue and clinical impact, regulatory reporting may be required |
| 4+ hours | Patient diversion active, recovery planning begins, post-incident documentation | Catastrophic impact, media attention possible, regulatory investigation likely |
The Downtime Cost Calculator
Use this framework to calculate your organization's specific downtime cost. The formula combines direct revenue loss, labor cost, recovery cost, and clinical risk cost into a single per-minute figure:
class DowntimeCostCalculator:
"""Calculate the business and clinical cost of healthcare IT downtime.
Inputs are organization-specific parameters; outputs are hourly and
annual cost estimates for use in reliability investment business cases."""
def __init__(
self,
num_providers: int,
avg_revenue_per_provider_hour: float,
num_beds: int,
avg_daily_admissions: int,
num_lab_orders_per_hour: int,
num_critical_systems: int,
avg_it_staff_hourly_rate: float = 75.0,
num_it_staff_incident: int = 8,
):
self.num_providers = num_providers
self.avg_revenue_per_provider_hour = avg_revenue_per_provider_hour
self.num_beds = num_beds
self.avg_daily_admissions = avg_daily_admissions
self.num_lab_orders_per_hour = num_lab_orders_per_hour
self.num_critical_systems = num_critical_systems
self.avg_it_staff_hourly_rate = avg_it_staff_hourly_rate
self.num_it_staff_incident = num_it_staff_incident
def revenue_loss_per_hour(self) -> dict:
"""Calculate direct revenue loss components."""
provider_loss = (
self.num_providers
* self.avg_revenue_per_provider_hour
* 0.6 # 60% reduction in patient throughput
)
lab_loss = self.num_lab_orders_per_hour * 45 # avg $45/test
billing_loss = (
self.num_providers
* self.avg_revenue_per_provider_hour
* 0.33 # 33% charge capture loss
)
return {
"provider_revenue_loss": round(provider_loss),
"lab_revenue_loss": round(lab_loss),
"billing_capture_loss": round(billing_loss),
"total_revenue_loss_per_hour": round(
provider_loss + lab_loss + billing_loss
),
}
def labor_cost_per_hour(self) -> dict:
"""Calculate incident response and workaround labor costs."""
it_response = (
self.num_it_staff_incident
* self.avg_it_staff_hourly_rate
)
clinical_overtime = (
self.num_providers * 25 # $25/hr overtime premium avg
)
post_incident = (
self.num_it_staff_incident
* self.avg_it_staff_hourly_rate
* 4 # 4 hrs post-incident per person
) / 1 # amortized over 1 hr of downtime
return {
"it_response_cost": round(it_response),
"clinical_overtime": round(clinical_overtime),
"post_incident_amortized": round(post_incident),
"total_labor_cost_per_hour": round(
it_response + clinical_overtime + post_incident
),
}
def annual_impact(self, current_uptime_pct: float = 99.5,
avg_incidents_per_year: int = 18,
avg_incident_duration_hrs: float = 4.0) -> dict:
"""Project annual downtime costs."""
annual_downtime_hrs = avg_incidents_per_year * avg_incident_duration_hrs
rev = self.revenue_loss_per_hour()
lab = self.labor_cost_per_hour()
hourly_total = (
rev["total_revenue_loss_per_hour"]
+ lab["total_labor_cost_per_hour"]
)
annual_cost = hourly_total * annual_downtime_hrs
return {
"current_uptime": f"{current_uptime_pct}%",
"annual_downtime_hours": round(annual_downtime_hrs, 1),
"cost_per_hour": hourly_total,
"cost_per_minute": round(hourly_total / 60),
"annual_downtime_cost": round(annual_cost),
"revenue_details": rev,
"labor_details": lab,
}
def roi_analysis(self, investment: float,
target_uptime_pct: float = 99.95,
target_incidents: int = 6,
target_mttr_hrs: float = 1.0) -> dict:
"""Calculate ROI of reliability investment."""
current = self.annual_impact()
target_downtime_hrs = target_incidents * target_mttr_hrs
target_annual_cost = current["cost_per_hour"] * target_downtime_hrs
savings = current["annual_downtime_cost"] - target_annual_cost
roi_pct = ((savings - investment) / investment) * 100
return {
"current_annual_cost": current["annual_downtime_cost"],
"target_annual_cost": round(target_annual_cost),
"annual_savings": round(savings),
"investment": investment,
"net_benefit": round(savings - investment),
"roi_percentage": round(roi_pct),
"payback_months": round(investment / (savings / 12), 1)
if savings > 0 else None,
}
# Example: Mid-size health system
calc = DowntimeCostCalculator(
num_providers=200,
avg_revenue_per_provider_hour=350,
num_beds=400,
avg_daily_admissions=50,
num_lab_orders_per_hour=120,
num_critical_systems=12,
)
print("=== Annual Impact ===")
import json
print(json.dumps(calc.annual_impact(), indent=2))
print("\n=== ROI Analysis ===")
print(json.dumps(calc.roi_analysis(investment=320000), indent=2))
Sample Calculator Output
{
"current_uptime": "99.5%",
"annual_downtime_hours": 72.0,
"cost_per_hour": 90800,
"cost_per_minute": 1513,
"annual_downtime_cost": 6537600,
"roi_analysis": {
"current_annual_cost": 6537600,
"target_annual_cost": 544800,
"annual_savings": 5992800,
"investment": 320000,
"net_benefit": 5672800,
"roi_percentage": 1773,
"payback_months": 0.6
}
}
For a 200-provider health system, the ROI on reliability investment is overwhelming: $320K invested yields $5.99M in avoided downtime costs -- a 1,773% return. The payback period is less than one month. These are the numbers that get CFO approval.
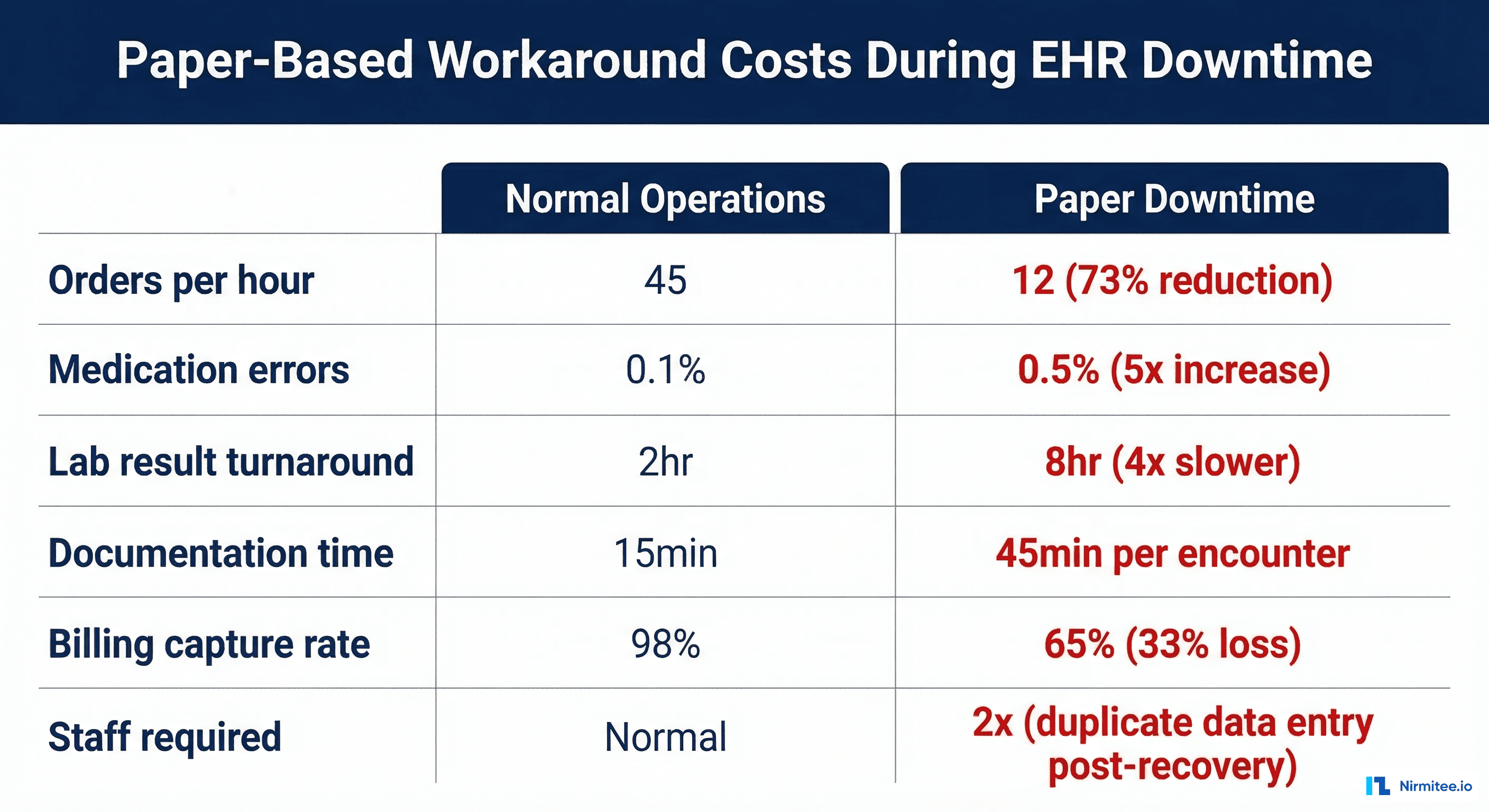
The Paper-Based Workaround Tax
When systems go down, healthcare does not stop. Clinicians switch to paper-based workarounds -- and the cost of these workarounds is often underestimated. It is not just the downtime period that hurts; it is the recovery period where staff must re-enter all paper documentation back into the EHR.
| Metric | Normal Operations | Paper Downtime | Degradation |
|---|---|---|---|
| Orders processed per hour | 45 | 12 | 73% reduction |
| Medication error rate | 0.1% | 0.5% | 5x increase |
| Lab result turnaround | 2 hours | 8 hours | 4x slower |
| Documentation time per encounter | 15 minutes | 45 minutes | 3x longer |
| Billing charge capture rate | 98% | 65% | 33% loss |
| Staff required for same throughput | 1x | 2x | Double staffing |
| Post-recovery data entry | None | 4-8 hours per dept | Additional labor cost |
Building the Business Case for Your CIO/CFO
The business case for reliability investment must speak two languages: clinical risk for the CMO/CIO and financial ROI for the CFO. Here is a framework for presenting both:
Executive Summary Framework
BUSINESS CASE: Healthcare IT Reliability Investment
PROBLEM:
- [Organization] experienced [N] unplanned outages in the past 12 months
- Total downtime: [X] hours affecting [Y] providers and [Z] patients
- Estimated financial impact: $[amount] (revenue + labor + recovery)
- Clinical risk: [number] near-miss events during downtime periods
PROPOSED INVESTMENT:
- Monitoring and observability platform: $[amount]
- Infrastructure redundancy (HA database, failover): $[amount]
- Disaster recovery improvements: $[amount]
- SRE/DevOps headcount (if needed): $[amount]
- Total investment: $[total]
PROJECTED OUTCOMES (12 months):
- Reduce unplanned outages from [N] to [target]
- Reduce MTTR from [current] to [target] minutes
- Improve uptime from [current]% to [target]%
- Avoid $[savings] in downtime costs
- ROI: [percentage]% | Payback: [months] months
CLINICAL IMPACT:
- Eliminate [N] hours/year of paper-based workaround risk
- Reduce medication error window by [X]%
- Ensure continuous lab result delivery
- Maintain Joint Commission readiness
Regulatory and Compliance Costs
Downtime in healthcare carries regulatory consequences that other industries do not face. If an outage affects PHI availability -- which is one of HIPAA's three pillars (confidentiality, integrity, availability) -- it may trigger reporting requirements:
| Regulatory Body | Trigger | Potential Penalty |
|---|---|---|
| HHS/OCR (HIPAA) | PHI availability disruption, breach notification if data compromised during outage | $100K - $1.5M per violation category per year |
| Joint Commission | Failure to maintain emergency downtime procedures, patient safety events | Survey findings, corrective action requirements |
| State Health Departments | Service disruption affecting patient care, reportable adverse events | Varies by state, up to license suspension |
| CMS (Medicare/Medicaid) | Failure to meet Conditions of Participation during extended outages | Payment suspension, decertification |

Frequently Asked Questions
How do I calculate downtime cost for my specific organization?
Start with three numbers: number of providers, average revenue per provider per hour, and number of unplanned outage hours in the past year. Multiply providers x revenue x 0.6 (throughput reduction) x downtime hours for the revenue component. Add IT labor costs (staff x hourly rate x downtime hours) and recovery costs (typically 2-4x the downtime hours for post-incident work). The Python calculator in this guide automates this with more granular inputs.
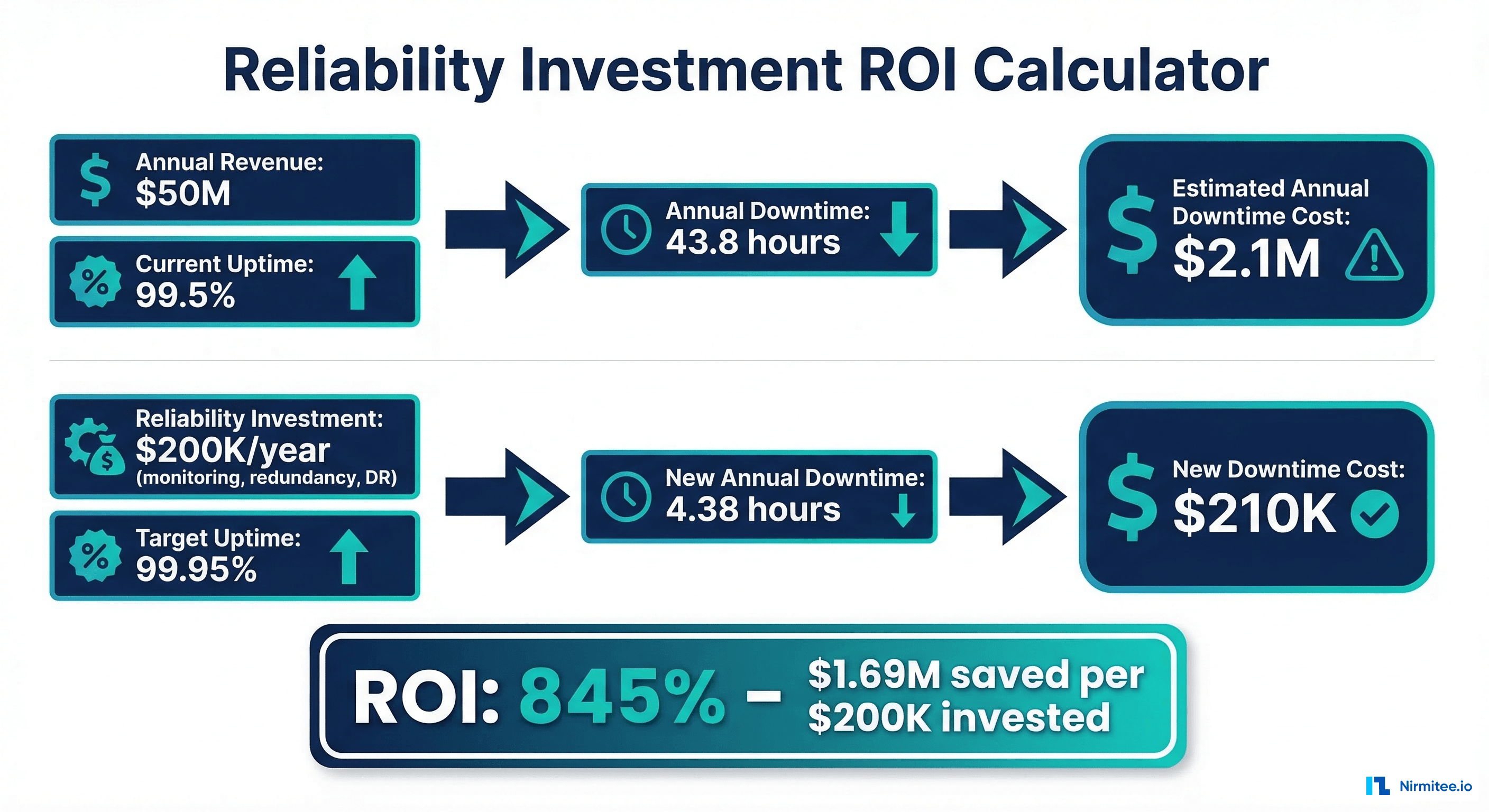
What is a realistic uptime target for healthcare systems?
The industry benchmark for critical healthcare systems (EHR, LIS, pharmacy) is 99.95% uptime, which translates to approximately 4.38 hours of downtime per year. Achieving 99.99% (52.6 minutes/year) is possible but requires significant investment in redundancy and is typically only justified for life-critical systems. Use synthetic monitoring to measure your actual uptime accurately.
How do I convince the CFO that reliability investment is worth it?
Frame it as risk mitigation with quantified ROI. Use the calculator in this guide to show the current annual cost of downtime, then present the investment required to reduce it. Most healthcare organizations find the ROI exceeds 500% -- meaning for every dollar invested, they avoid $5+ in downtime costs. Present the payback period (typically under 3 months) and compare the investment to a single major outage event. Also emphasize that HIPAA does not distinguish between data breaches and availability failures -- both can trigger enforcement actions.
What are the most cost-effective reliability investments?
In order of impact per dollar spent: 1) Centralized logging and monitoring ($30-60K/year, detects issues 80% faster), 2) Automated database failover ($50-80K, eliminates the #1 cause of extended outages), 3) Runbook automation ($20-40K, reduces MTTR by 60%), 4) DR testing ($15-30K/year, validates recovery actually works), 5) SRE staffing ($150-200K, provides dedicated reliability engineering). Building on a solid technology stack with reliability built in from the start is always cheaper than retrofitting.
How does downtime affect patient satisfaction scores?
Research from Press Ganey shows that patients who experience service disruptions during their care are 2.3x more likely to give low satisfaction scores. In the era of public reporting (Hospital Compare, Leapfrog), satisfaction scores directly impact patient volume and, for Medicare patients, reimbursement rates through the Hospital Value-Based Purchasing Program. A single extended outage can measurably depress patient satisfaction scores for the following quarter.
Conclusion
The cost of healthcare IT downtime is not a mystery -- it is a calculable business risk that most organizations simply have not quantified. By applying the framework and calculator in this guide, you can build a precise, defensible business case for reliability investment. The numbers consistently tell the same story: investing in monitoring, redundancy, and recovery capabilities delivers ROI that few other IT investments can match. For healthcare organizations building interoperable systems with increasingly complex integration points, proactive reliability investment is not optional -- it is a clinical and financial imperative.



