EMR Vs. EHR, though these terms are often used interchangeably, they are not the same. Each has a distinct purpose, and understanding the differences is important for patients, healthcare providers, and organizations looking to optimize patient care through technology.
This blog will break down the difference between EMR and EHR in simple language, so you can understand their unique roles, why they are essential, and how they impact the future of healthcare.
What is an EMR?
An Electronic Medical Record (EMR) is a digital version of the paper charts you might see in a doctor's office. It contains all the information about the care a patient receives from a single provider or practice. Think of it as a record of your medical history within one clinic or hospital.
For example, if you go to your primary care physician for an annual check-up, the doctor will record information such as your weight, blood pressure, medications, and any illnesses or treatments in the EMR. This record stays with that doctor and helps them track your health over time.
Key features of EMRs:
- Medical history and patient notes for one specific provider or facility.
- Tracking of patient data over time, such as vaccinations or blood pressure measurements.
- Limited access to other healthcare providers or facilities.
However, while an EMR is useful within a single provider's office, it has limitations. If you go to another clinic or need to see a specialist, your EMR may not easily transfer, meaning you might need to provide your medical history again, or they might not have access to your complete health records.
For organizations seeking to bridge this gap, EMR Integration for RPM enables smoother data sharing and connectivity between remote monitoring and clinical systems.
What is an EHR?
An Electronic Health Record (EHR) is a more comprehensive and connected version of an EMR. It includes everything an EMR does but is designed to share information across different healthcare providers and facilities. In other words, an EHR is intended to follow the patient across multiple locations, allowing different doctors, specialists, and healthcare professionals to access the same up-to-date information.
For example, let's say you visit your primary care physician, and they refer you to a cardiologist. With an EHR system in place, the cardiologist can access your medical history, lab results, and medication lists instantly, without needing to ask you for your medical records again. Similarly, if you visit an emergency room in another state, the ER doctors can view your EHR and provide better care by having your medical history readily available.
Key features of EHRs:
- Comprehensive health records from multiple providers and facilities.
- Data sharing between doctors, specialists, labs, hospitals, and pharmacies.
- Patient engagement, as EHRs often allow patients to access their records through a patient portal.
An EHR is more than just a digital file it's a system that integrates patient data to improve healthcare collaboration and enhance care. Providers can achieve this connectivity using EHR Integration or Healthcare Interoperability Solutions that enable seamless data exchange across systems.
The Main Differences Between EMR and EHR
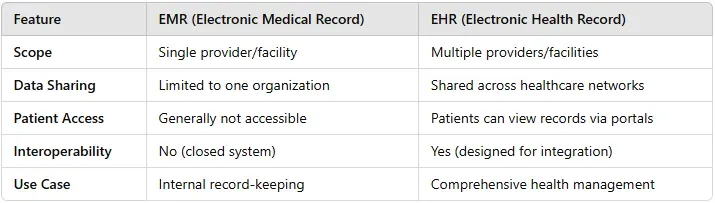
Now that we have an idea of what EMRs and EHRs are, let's dive into the main differences between them:
a) Scope
- EMR: Limited to one healthcare provider or practice. It contains data about the treatment and care provided by that specific provider.
- EHR: Covers a broader range of data that can be shared between multiple healthcare providers and facilities, creating a more comprehensive view of the patient's health.
b) Data Sharing
- EMR: Information is confined to the practice that created it. If you switch doctors or visit a specialist, your EMR may not travel with you unless it is manually transferred.
- EHR: Information can be shared between different healthcare facilities, ensuring that all providers involved in your care have access to the same up-to-date records.
c) Patient Involvement
- EMR: Typically, patients do not have direct access to their EMR. You would need to request copies of your medical record if you wanted to review it.
- EHR: EHR systems often include Automated Patient Communication Software, which enables patients to engage directly with their health data and providers through secure messaging and updates.
d) Efficiency in Care
- EMR: While useful in tracking patient data over time, EMRs are isolated and do not support collaboration between different healthcare providers.
- EHR: EHRs enhance collaboration and streamline chronic care when integrated with Remote Patient Monitoring Software Services
e) Regulatory Requirements
- EMR: EMRs focus on internal use, primarily for the healthcare provider's office. The provider may not be required to meet certain interoperability standards (the ability of different systems to work together).
- EHR: EHR systems often need to meet specific federal standards that promote interoperability and data sharing across different systems, such as Meaningful Use, a U.S. government program that incentivizes healthcare providers to use EHRs effectively.
Why the difference matters with an example
To illustrate the importance of these differences, let's take an example:
Imagine Jane, a 50-year-old woman, goes to her primary care doctor with chest pain. The doctor takes her vitals, runs some blood tests, and refers her to a cardiologist for further evaluation. With an EMR, Jane's primary care doctor would have all her medical information, but the cardiologist may not have immediate access to that data unless it is faxed or manually transferred. This delay could slow down her diagnosis and treatment.
Now, consider if Jane's doctor uses an EHR. When Jane visits the cardiologist, the cardiologist can instantly access her complete medical history, including the recent test results from the primary care doctor. This allows the cardiologist to make a more informed diagnosis and treatment plan. If Jane later needs surgery, the hospital can access her EHR to ensure continuity of care. In this scenario, the EHR provides a seamless healthcare experience, ensuring all providers are on the same page.
The Benefits of EHR Over EMR
EHRs are quickly becoming the standard in healthcare for several reasons:
-
Better Care Coordination
When multiple healthcare providers can access the same health record, they can work together to provide the best possible care. This is especially important for patients with complex or chronic conditions, who may need to see multiple specialists. For instance, a diabetic patient may need to see an endocrinologist, a primary care doctor, and a podiatrist. EHRs ensure that all these providers have the same information, preventing conflicting treatments or unnecessary tests.
-
Improved Patient Safety
EHRs can reduce errors by ensuring that all healthcare providers have the latest information about the patient's medications, allergies, and health history. For example, if a patient has a known allergy to penicillin, an EHR system can alert healthcare providers if they attempt to prescribe it, avoiding a potentially dangerous situation.
-
Enhanced Patient Engagement
Many EHR systems allow patients to take an active role in their healthcare by giving them access to their medical records. Patients can monitor their progress, see lab results, and communicate with their doctors through secure online portals. This level of engagement can lead to better health outcomes, as patients are more likely to follow treatment plans when they are actively involved.
-
Streamlined Workflows for Healthcare Providers
EHRs help streamline administrative tasks by automating things like appointment scheduling, billing, and insurance verification. This saves time for healthcare providers, allowing them to focus more on patient care.
Challenges of Implementing EHRs
Despite their many benefits, implementing EHRs comes with its own set of challenges:
-
Cost
The initial cost of setting up an EHR system can be high, especially for smaller practices. This includes the cost of the software, hardware, and training staff to use the system effectively. -
Training
Switching from paper records or EMRs to EHRs requires training. Healthcare providers and staff need to learn how to use the system, which can take time and disrupt normal workflows in the beginning. -
Data Privacy and Security
While EHRs make sharing data easier, they also raise concerns about data security. Healthcare providers need to comply with regulations such as HIPAA (Health Insurance Portability and Accountability Act) to protect sensitive patient information.
Conclusion
In summary, EMRs and EHRs are both valuable tools in modern healthcare, but they serve different purposes. EMRs are more limited, focusing on the care provided by one healthcare provider or facility, while EHRs offer a more comprehensive view of the patient's overall health, supporting collaboration across multiple providers and locations.
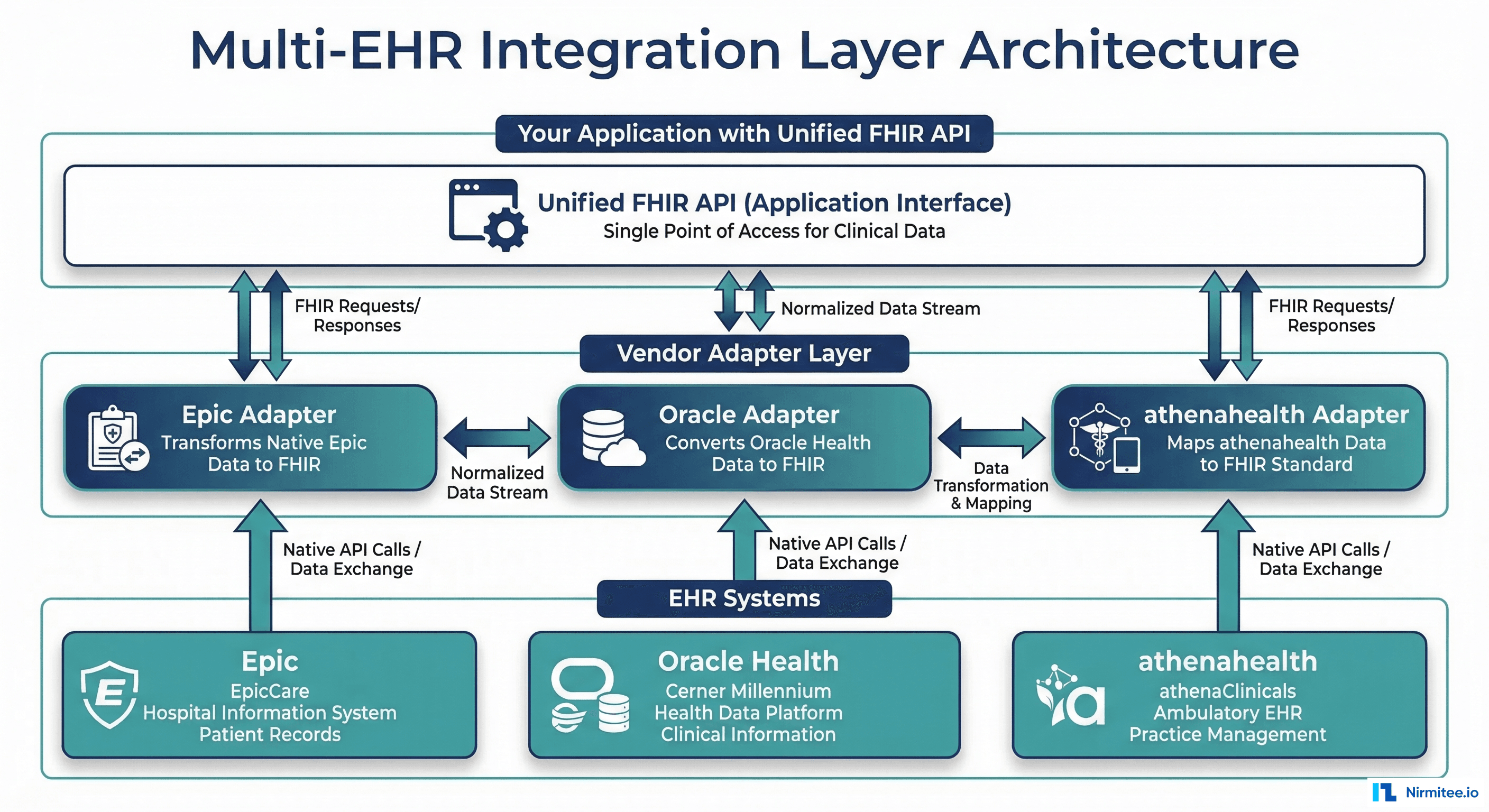
To build a seamless, interoperable environment, healthcare providers must focus on integration-first architecture,connecting systems through smart APIs, HL7/FHIR frameworks, and Healthcare Technology Consulting expertise.