A ventilator fails during a night shift in the ICU. The biomedical engineering team is called. The manufacturer's service engineer is three hours away. The spare part has to be ordered from Mumbai. For the next 48 hours, the ICU operates with one fewer ventilator than its patient load requires.
This is not a hypothetical scenario. According to a study published in PubMed Central (PMC9968427), hospitals without structured preventive maintenance programs experience equipment failure rates that leave only 57.8% of their medical equipment functioning efficiently. The WHO reports that in developing countries, 50-80% of medical equipment is non-functional at any given time, primarily due to the absence of maintenance programs.
Preventive maintenance is not optional. It is the difference between a hospital that runs and one that gambles with patient safety every day. This guide covers everything a hospital administrator, biomedical engineer, or healthcare IT leader needs to implement a PM program that meets NABH accreditation standards, reduces costs by 30-50%, and extends equipment lifespan by up to 39%.
What Preventive Maintenance Actually Means in a Hospital Context
Preventive maintenance (PM) in hospitals is the systematic inspection, testing, calibration, and servicing of medical equipment on a scheduled basis, before it fails. Unlike reactive maintenance (fix it when it breaks) or corrective maintenance (repair after detecting a problem), PM is proactive. It prevents failures from occurring in the first place.
The distinction matters because the cost difference is not marginal. Industry benchmarks consistently show that reactive maintenance costs 3-5 times more than preventive approaches. A study of over 1,000 hospitals found that institutions relying primarily on reactive maintenance spend an average of Rs 7.5 million more annually on equipment-related costs than those with mature PM programs (Diasurge Medical, 2024).
In the Indian context, where hospitals lose crores annually to poor equipment management, the case for PM is even stronger. The government's Biomedical Equipment Maintenance and Management Program (BMMP) inventoried 756,750 devices across 29,115 public health facilities and found 13-34% of equipment dysfunctional across states before intervention.
The Four Types of Hospital Equipment Maintenance
A mature maintenance program uses all four types in combination, weighted by equipment criticality:
1. Preventive Maintenance (PM)
Scheduled inspections and servicing at fixed intervals. This is the backbone of any equipment management program. ECRI Institute publishes Inspection and Preventive Maintenance (IPM) procedures for over 150 device types, covering electrical safety testing, alarm performance verification, output measurements, and mechanical integrity checks.
Example: An MRI scanner receives quarterly PM including helium level checks, gradient coil inspection, RF calibration, and software updates. Each PM visit takes 4-6 hours of scheduled downtime versus 72+ hours of unplanned downtime if the magnet quenches due to low helium.
2. Predictive Maintenance (PdM)
Uses sensor data, vibration analysis, thermal imaging, and AI-driven analytics to predict when a component will fail. GE HealthCare's OnWatch AI system, for example, has demonstrated a 40% reduction in unplanned downtime and increased MRI uptime by 4.5 additional days per year per scanner (GE HealthCare, 2024).
3. Corrective Maintenance
Repairs performed after a defect is identified but before complete failure. This is triggered by PM inspections that catch early warning signs, such as unusual noise from a compressor, a slight drift in calibration, or a worn bearing that has not yet failed.
4. Reactive/Breakdown Maintenance
Emergency repairs after equipment fails. This should account for no more than 20% of total maintenance activity in a well-run program. If reactive maintenance exceeds 40%, the PM program needs restructuring. The industry target is an 80/20 preventive-to-reactive ratio.
Why Preventive Maintenance Is Non-Negotiable for Indian Hospitals
Patient Safety
Equipment failure during patient care is not just an operational inconvenience. It is a patient safety event. When a defibrillator fails during a cardiac arrest, a pulse oximeter gives false readings in the NICU, or a ventilator alarm malfunctions, the consequences are measured in lives, not rupees.
The WHO Medical Device Technical Series documents that equipment malfunction is a contributing factor in a significant percentage of adverse events in hospitals that lack structured maintenance programs.
NABH Accreditation Requirements
For Indian hospitals pursuing or maintaining NABH accreditation, preventive maintenance is not a recommendation but a documented requirement. The NABH 6th Edition Standards (January 2025) mandate:
- Equipment Inventory Register: Every medical device must have a unique identifier in a central register
- Preventive Maintenance Schedule: Documented PM calendar with frequencies based on manufacturer recommendations and risk classification
- Equipment History Sheet: Complete log for each device covering purchase date, all PM activities, calibration records, repairs, spare parts replaced, and downtime
- Calibration Records: Traceable calibration for all measuring and diagnostic equipment, with certificates from NABL-accredited laboratories
- Uptime Tracking: The BMMP program sets minimum uptime targets of 95% for District Hospitals, 90% for CHCs, and 80% for PHCs
- Condemnation Process: Documented protocol for equipment that has exceeded its economic repair threshold
Financial Impact
The numbers are unambiguous. According to data compiled from GE Healthcare, MedTech Europe, and HFMA studies:
- Unplanned equipment downtime costs up to $760 per device per day (approximately Rs 63,000)
- Unplanned CT/MRI downtime: $60,000-$120,000 per incident (Rs 50-100 lakhs)
- The U.S. healthcare industry loses approximately $3 billion annually from idle and broken equipment
- Failure to perform PM reduces equipment lifespan by 39% (Diasurge Medical)
- Hospitals implementing robust PM for bed equipment reduced CapEx from $15.3M to $7.6M, saving $7.7M annually
For an Indian hospital with Rs 50 crore worth of medical equipment, the maintenance budget calculation is straightforward: spend Rs 2-3 crore annually on PM, or spend Rs 8-12 crore on emergency repairs, premature replacements, and the hidden costs of downtime.
Risk-Based Equipment Classification for PM Scheduling
Not all equipment needs the same maintenance frequency. The AAMI EQ56:2024 standard and the CMS Alternative Equipment Management (AEM) program both recommend risk-based classification to allocate maintenance resources efficiently.
Critical Equipment (Monthly PM)
Life-support and life-safety devices where failure directly threatens patient survival:
- Ventilators and respiratory support devices
- Defibrillators and cardiac monitors
- Anesthesia machines and vaporizers
- Infusion pumps (especially high-risk IV medications)
- Patient monitors in ICU/CCU/NICU
PM protocol: Monthly functional testing, quarterly comprehensive inspection, annual performance verification per ECRI IPM procedures. Spare critical devices must be available as backup.
High-Priority Equipment (Bi-Monthly PM)
Equipment where failure causes significant operational disruption or patient risk:
- Sterilizers and autoclaves
- Surgical lights and electrosurgical units
- Blood gas analyzers
- Emergency generators and UPS systems
- Medical gas pipeline systems
Standard Equipment (Quarterly PM)
High-value imaging and diagnostic equipment where PM focuses on calibration accuracy and performance optimization:
- MRI scanners (quarterly PM, annual magnet service)
- CT scanners (quarterly calibration, tube monitoring)
- X-ray machines and C-arms
- Ultrasound systems
- Laboratory analyzers
Low-Priority Equipment (Semi-Annual PM)
Non-clinical and low-risk equipment:
- Hospital beds and stretchers
- Wheelchairs and patient transport equipment
- Weighing scales and height measurers
- Examination lights
- Suction machines (non-surgical)
Implementing a PM Program: The 6-Month Roadmap
Based on the NHSRC India guidelines and successful implementations across Indian hospitals, here is a realistic implementation roadmap:
Phase 1: Foundation (Months 1-2)
Complete Asset Inventory
You cannot maintain what you have not inventoried. Every medical device needs:
- Unique asset ID (recommended format: DEPT-FLOOR-TYPE-SERIAL, e.g., RAD-2F-MRI-001)
- Manufacturer, model, serial number
- Purchase date, warranty status, AMC details
- Location (building, floor, room)
- Risk classification (Critical / High / Standard / Low)
- Current condition (Functional / Needs Repair / Non-Functional)
The BMMP program accomplished this across 29,115 facilities. A single hospital should complete this in 2-4 weeks with a dedicated team of 2-3 biomedical engineers. If your hospital already uses an asset management system, export the existing data and validate it against physical verification.
Risk Classification
Classify every device using the AAMI EQ56 risk scoring framework:
Risk Score = Function Score + Physical Risk Score + Maintenance Requirements Score
Function Score:
Life support = 10 | Therapeutic = 8 | Diagnostic = 6 | Analytical = 4 | Other = 2
Physical Risk Score:
Patient contact, energy delivery = 5 | Patient contact, no energy = 3 | No patient contact = 1
Maintenance Requirements Score:
Extensive calibration = 5 | Some calibration = 3 | Visual inspection only = 1
Total 12+ = Critical | 8-11 = High | 5-7 = Standard | Below 5 = LowNABH Gap Analysis
Audit your current documentation against NABH requirements. The most common gaps in Indian hospitals:
- Missing equipment history sheets (70% of hospitals have incomplete records)
- No documented PM schedule tied to manufacturer recommendations
- Calibration certificates expired or missing for diagnostic equipment
- No formal condemnation process for end-of-life equipment
- Uptime/downtime not tracked systematically
Phase 2: Execution (Months 3-4)
Build PM Schedules
Create a master PM calendar that maps every device to its maintenance schedule. For each equipment class, document:
- PM frequency (based on risk class and manufacturer specs)
- Specific inspection checklist (use ECRI IPM procedures as baseline)
- Required tools and test equipment
- Estimated time per PM activity
- Competency requirements for the technician
Sample PM Schedule for a 200-Bed Hospital:
Monthly PMs: ~45 devices x 30-60 min each = 35-45 hours/month
Bi-Monthly PMs: ~80 devices x 45-90 min each = 30-60 hours/bi-monthly
Quarterly PMs: ~120 devices x 60-120 min each = 60-120 hours/quarter
Semi-Annual PMs: ~200 devices x 30-45 min each = 50-75 hours/semi-annual
Biomedical engineer requirement: 3-4 FTEs for a 200-bed hospital
(Industry benchmark: 1 biomed engineer per 500-750 devices)Spare Parts Procurement Strategy
India imports 80% of its medical devices. Spare parts procurement is the single biggest bottleneck in hospital equipment maintenance. Build a critical spares inventory:
- Identify the top 20 failure-prone components across your equipment fleet
- Maintain minimum stock for critical equipment spares (fuses, batteries, sensors, tubing)
- Establish relationships with at least 2 authorized distributors per OEM
- Budget 6-10% of equipment value annually for spare parts (AAMI benchmark)
Phase 3: Optimization (Months 5-6)
KPI Dashboard
Track these metrics monthly:
Equipment Uptime (%) = (Total Available Hours - Downtime Hours) / Total Available Hours x 100
Target: 95%+ for critical equipment, 90%+ overall
PM Compliance Rate (%) = Completed PMs / Scheduled PMs x 100
Target: 95%+ (NABH expects documented compliance)
Mean Time Between Failures (MTBF) = Total Operating Hours / Number of Failures
Track trend: MTBF should increase quarter-over-quarter
Mean Time To Repair (MTTR) = Total Repair Hours / Number of Repairs
Target: Under 4 hours for critical equipment
Preventive-to-Reactive Ratio = PM Work Orders / Reactive Work Orders
Target: 80/20 or better
Cost-of-Service Ratio = Annual Maintenance Cost / Equipment Acquisition Cost
Benchmark: 4.5-15% depending on device type (AAMI data)Predictive Analytics Integration
For hospitals with connected medical devices, predictive maintenance is the next evolution. IoT sensors on critical equipment can monitor vibration patterns, temperature anomalies, power consumption, and operational cycles to predict failures 2-4 weeks before they occur. Industry data shows predictive maintenance achieves a 40-50% downtime reduction within 12 months and reduces maintenance costs by 25-35% compared to time-based PM alone.
PM Procedures for Critical Equipment Categories
Ventilators (Monthly PM)
- Verify tidal volume accuracy within +/- 10% across all modes
- Test all alarm conditions: high pressure, low pressure, apnea, power failure
- Inspect patient circuit for leaks and integrity
- Verify oxygen sensor calibration against known concentration
- Check battery backup: must sustain operation for minimum 30 minutes
- Clean and inspect air intake filters
- Run self-diagnostic tests and document results
Defibrillators (Monthly PM)
- Deliver test shock into 50-ohm load at all energy levels
- Verify energy delivery accuracy within +/- 15% of selected level
- Test ECG monitoring quality and lead selection
- Verify charge time: must reach maximum energy in under 10 seconds
- Check battery capacity: must deliver minimum 20 full-energy shocks
- Inspect pads, cables, and connector integrity
- Verify date on disposable electrodes/pads
MRI Scanners (Quarterly PM)
- Helium level check (must maintain minimum level per manufacturer)
- Image quality assessment using ACR phantom
- Gradient coil performance verification
- RF transmit and receive calibration
- Table positioning accuracy and weight capacity
- Emergency stop and quench button functionality
- Cooling system inspection (chiller performance, water flow)
- Software version verification and security patches
Sterilizers/Autoclaves (Bi-Monthly PM)
- Biological indicator testing (spore test for sterilization validation)
- Bowie-Dick test for steam penetration (daily for prevacuum sterilizers)
- Chamber door gasket inspection and leak testing
- Pressure gauge calibration verification
- Safety valve testing
- Water quality testing (conductivity, pH)
- Print/record verification for cycle documentation
Common PM Program Failures and How to Avoid Them
Failure 1: Paper-Based Tracking
Hospitals that track PM on paper or spreadsheets consistently underperform. PM completion rates drop below 70% when there is no automated scheduling and alert system. Invest in a computerized maintenance management system (CMMS) that generates work orders automatically, sends reminders, and tracks completion with timestamps.
Failure 2: Skipping PM Under Operational Pressure
When the ICU is full and the MRI schedule is packed, PM gets postponed. This is the most dangerous pattern. A postponed PM on a ventilator does not make the news today, but a ventilator failure in three months does. Build PM windows into the operational schedule at the department level, and track PM compliance as a quality metric with the same weight as clinical outcomes.
Failure 3: OEM-Only Maintenance
Relying exclusively on OEM service contracts is expensive and often slow. Train in-house biomedical engineers to perform routine PM, and reserve OEM service for complex repairs and annual performance verifications. The cost difference is significant: in-house PM costs Rs 500-2,000 per device per visit versus Rs 5,000-25,000 for OEM service visits.
Failure 4: Ignoring Environmental Systems
Medical equipment PM programs often focus exclusively on clinical devices and ignore the infrastructure that supports them: HVAC systems (critical for OR and isolation rooms), medical gas pipelines, UPS and power conditioning, and water purification systems. A failure in any of these support systems can take down an entire department.
Need a custom-built healthcare solution? Our Custom Healthcare Software Development team delivers end-to-end, from requirements to production. Talk to our team to get started.
Frequently Asked QuestionsWhat is the ideal maintenance budget for a hospital?
Industry benchmarks suggest allocating 6-10% of total equipment value annually for maintenance. For a hospital with Rs 50 crore in medical equipment, this means Rs 3-5 crore per year. The AAMI standard recommends a Cost-of-Service Ratio of 4.5-15% of device acquisition price, varying by equipment type and age.
How many biomedical engineers does a hospital need?
The industry benchmark is 1 biomedical engineer per 500-750 devices. A 200-bed hospital typically has 400-600 medical devices, requiring 1-2 senior and 2-3 junior biomedical engineers. Larger hospitals with complex imaging equipment may need additional specialized staff.
Can PM be outsourced entirely?
Partial outsourcing works well. Keep routine PM (monthly functional checks, basic inspections) in-house, and outsource specialized PM (MRI magnet service, CT tube replacement, linear accelerator calibration) to OEMs or authorized service organizations. The BMMP program in India uses a PPP model across 20 states, where private maintenance partners handle equipment across public health facilities.
What is the difference between PM and calibration?
PM ensures the equipment functions correctly (mechanical, electrical, and functional checks). Calibration ensures the equipment measures accurately (comparing device output against a known reference standard). Both are required by NABH, but calibration must be performed by technicians with traceable standards and documented per NABL requirements.
How does NABH audit PM compliance?
NABH assessors review: (1) the master equipment list with risk classification, (2) PM schedules with documented completion dates, (3) equipment history sheets with complete maintenance records, (4) calibration certificates with traceability, (5) uptime/downtime data, and (6) the condemnation process for end-of-life equipment. The most common non-conformities are incomplete history sheets and missing calibration certificates.
What is the ROI timeline for implementing a PM program?
Most hospitals see measurable results within 3-6 months: reduced emergency repair frequency, improved equipment availability, and lower spare parts costs. Full financial ROI, including extended equipment lifespan and reduced CapEx, typically materializes within 12-18 months. The Diasurge Medical study showed hospitals reducing CapEx by up to 50% within the first year of structured PM implementation.
The Bottom Line
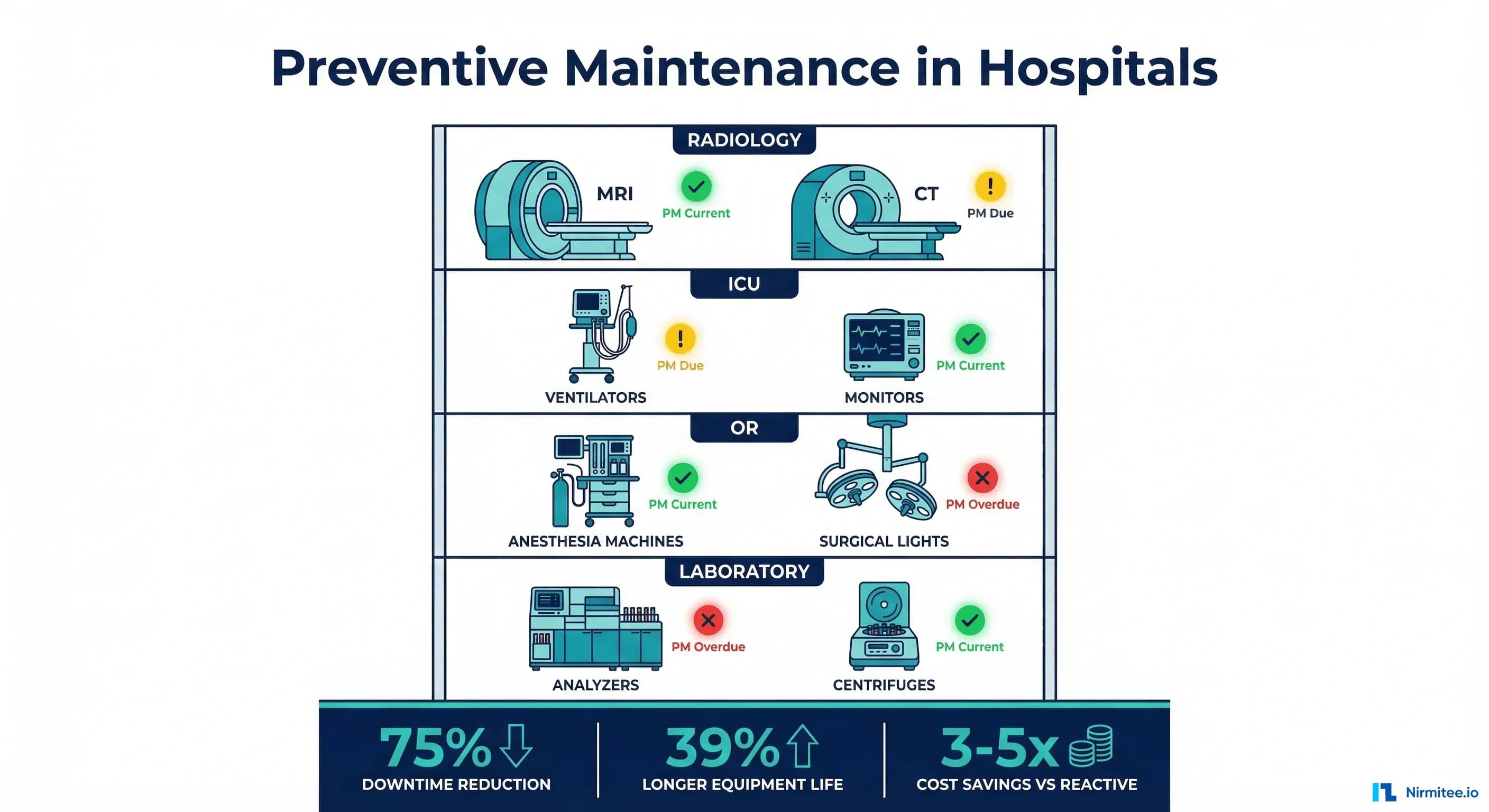
Preventive maintenance in hospitals is not a cost center. It is the single most effective strategy to protect patient safety, reduce operational costs, extend equipment lifespan, and maintain regulatory compliance. The data is unambiguous: hospitals with mature PM programs spend 3-5x less on maintenance, keep equipment running 39% longer, and experience 75% fewer unplanned downtime events.
For Indian hospitals specifically, the convergence of NABH accreditation requirements, the BMMP program's infrastructure, and the growing availability of digital asset management tools makes this the right time to build or upgrade a PM program. The cost of inaction, measured in crores of rupees, patient safety incidents, and accreditation risk, far exceeds the investment required.
Start with an asset inventory. Classify by risk. Build PM schedules. Track compliance. The equipment that keeps your patients alive deserves at least as much systematic attention as the clinical protocols that guide their care.