The $500 Billion Opportunity: Why Launch an RPM Program Now
Home healthcare is the fastest-growing segment in the healthcare industry, with a projected 25.3% CAGR through 2030. Remote Patient Monitoring sits at the center of this growth. Medicare's 2026 fee schedule increased RPM reimbursement by approximately 25%, new CPT codes (99445, 99470) eliminated the 16-day minimum data requirement, and chronic disease prevalence continues climbing — 6 in 10 American adults now have at least one chronic condition.
Yet launching an RPM program remains daunting for most practices. Device selection alone involves navigating FDA clearances, BLE connectivity standards, patient usability considerations, and vendor reliability. The platform architecture must handle real-time device data, FHIR-based EHR integration, clinical alert management, and billing automation. And the operational workflow — patient enrollment, clinician training, documentation protocols — determines whether the program generates revenue or just headaches.
This guide provides a complete 90-day launch plan, from device selection criteria to go-live metrics, tested against real RPM program deployments.
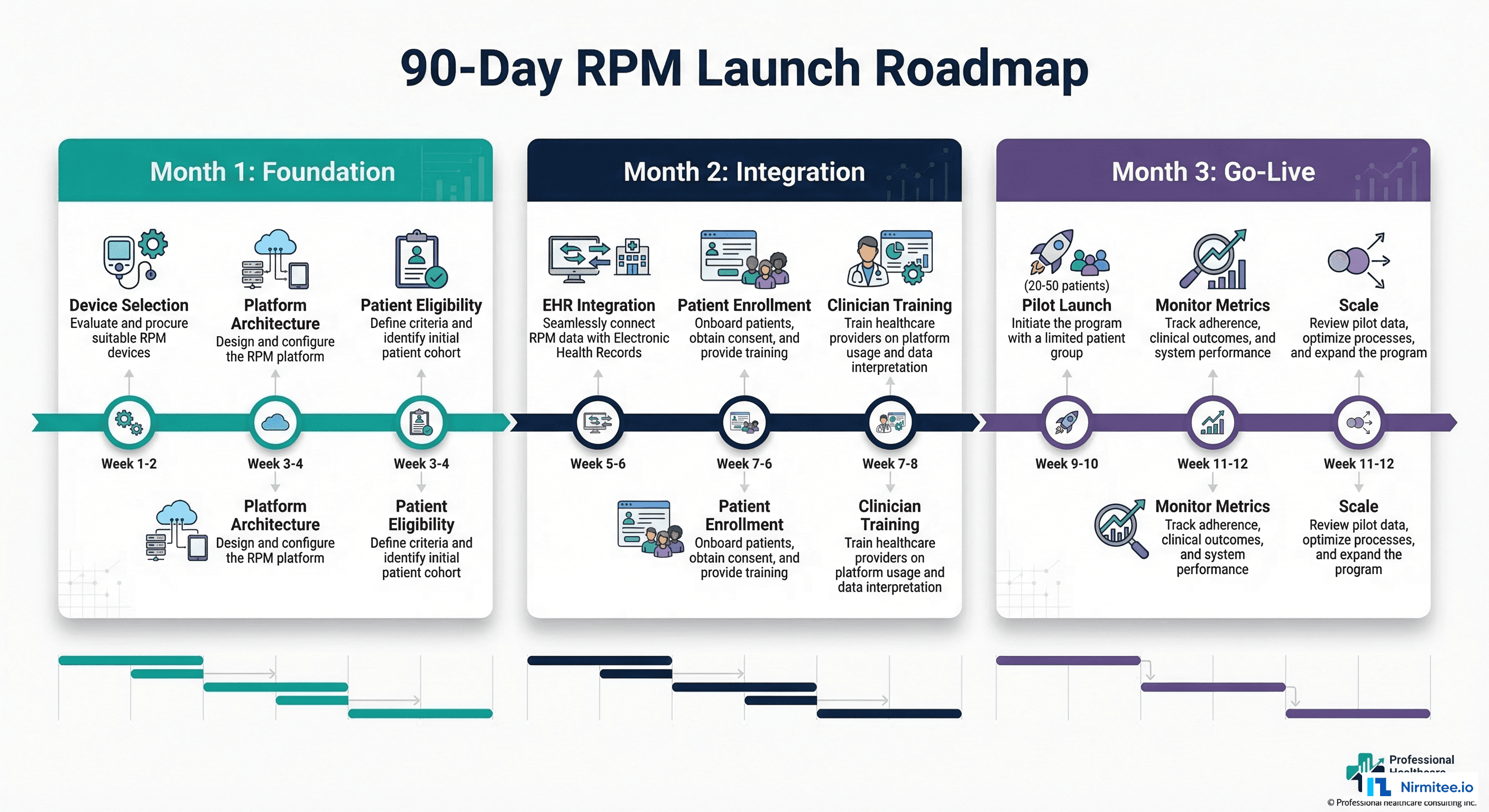
Month 1: Foundation — Device Selection, Platform Architecture, and Patient Eligibility
Device Selection: What to Look For
The monitoring device is your patient's daily touchpoint with the RPM program. Choose wrong and patient engagement collapses. Choose right and data flows reliably for months. Here are the selection criteria ranked by importance:
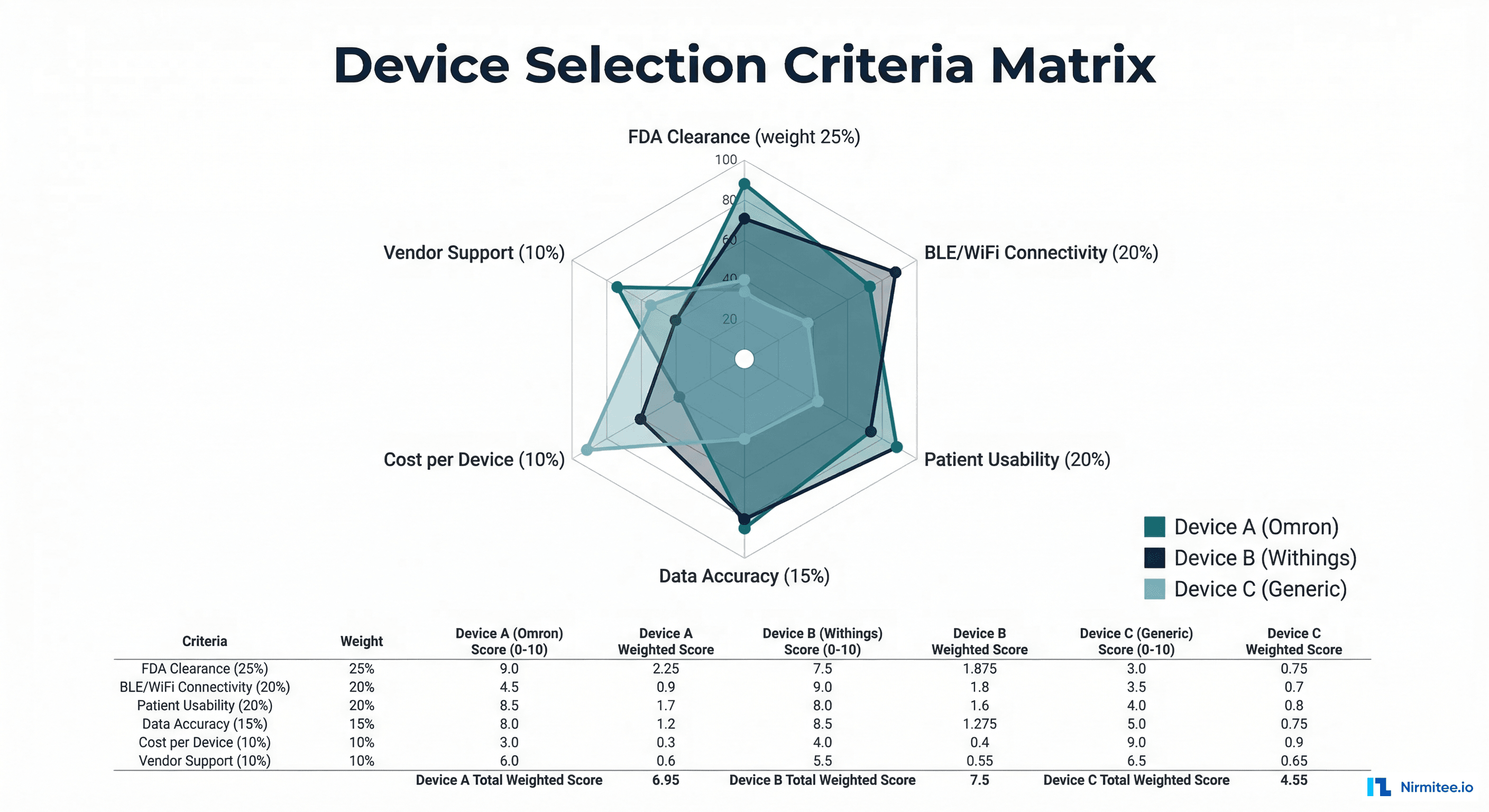
| Criterion | Weight | Why It Matters |
|---|---|---|
| FDA Clearance | 25% | Required for RPM billing — non-cleared devices cannot support CPT 99453-99458 claims |
| BLE/WiFi Connectivity | 20% | Automatic data transmission eliminates patient burden — manual entry kills engagement |
| Patient Usability | 20% | Average RPM patient is 65+ with limited tech literacy — device must be simple |
| Data Accuracy | 15% | Clinical decisions depend on accurate readings — verify against validation standards |
| Cost per Device | 10% | Device cost affects program economics — target under $150/device for BP, $300 for CGM |
| Vendor Support/API | 10% | Integration support, warranty, replacement policies, and API documentation quality |
Recommended Devices by Category
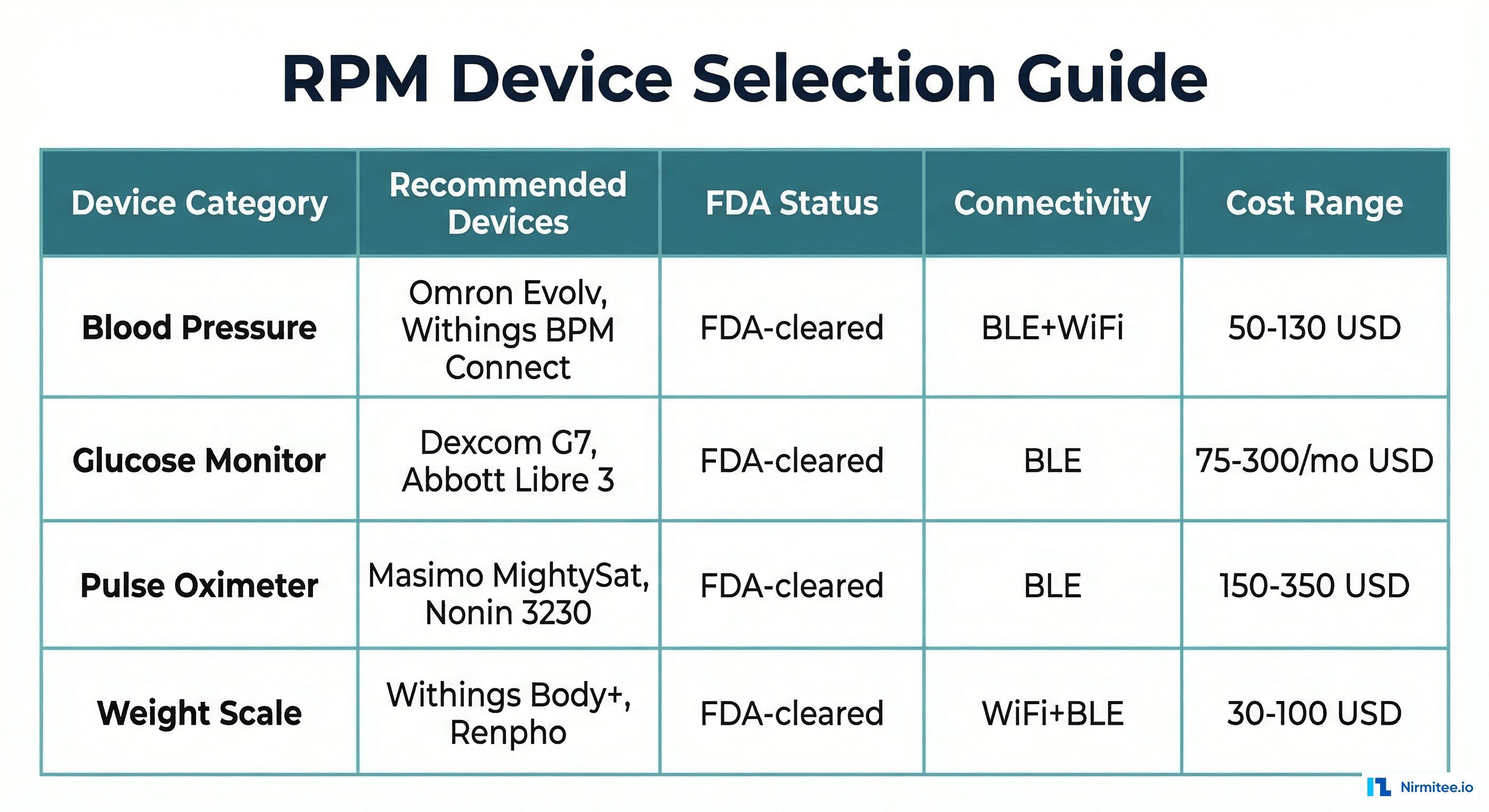
| Category | Top Picks | FDA Status | Connectivity | Cost | Best For |
|---|---|---|---|---|---|
| Blood Pressure | Omron Evolv | FDA-cleared | BLE | $75-90 | Ease of use, single-piece design |
| Blood Pressure | Withings BPM Connect | FDA-cleared | BLE + WiFi | $100-130 | WiFi auto-sync, HealthKit integration |
| Glucose (CGM) | Dexcom G7 | FDA-cleared | BLE | $75-300/mo | Continuous monitoring, real-time alerts |
| Glucose (BGM) | OneTouch Verio Reflect | FDA-cleared | BLE | $20-40 | Traditional finger-stick, lower cost |
| Pulse Oximeter | Masimo MightySat | FDA-cleared | BLE | $300-350 | Medical-grade accuracy (Masimo SET) |
| Pulse Oximeter | Nonin 3230 | FDA-cleared | BLE | $150-200 | Cost-effective, clinical-grade |
| Weight Scale | Withings Body+ | FDA-cleared | WiFi + BLE | $60-100 | Auto-sync, multi-user, HealthKit |
| Thermometer | Kinsa Smart Thermometer | FDA-cleared | BLE | $20-35 | Connected temp monitoring |
Pro tip: Start with blood pressure cuffs. Hypertension is the most common RPM use case, BP cuffs are the most affordable and reliable devices, and hypertension patients have the highest Medicare enrollment rates. Expand to glucose monitors and pulse oximeters in Phase 2.
Platform Architecture
Your RPM platform must handle four core functions: device data ingestion, clinical workflow support, EHR integration, and billing automation. Here is the reference architecture:
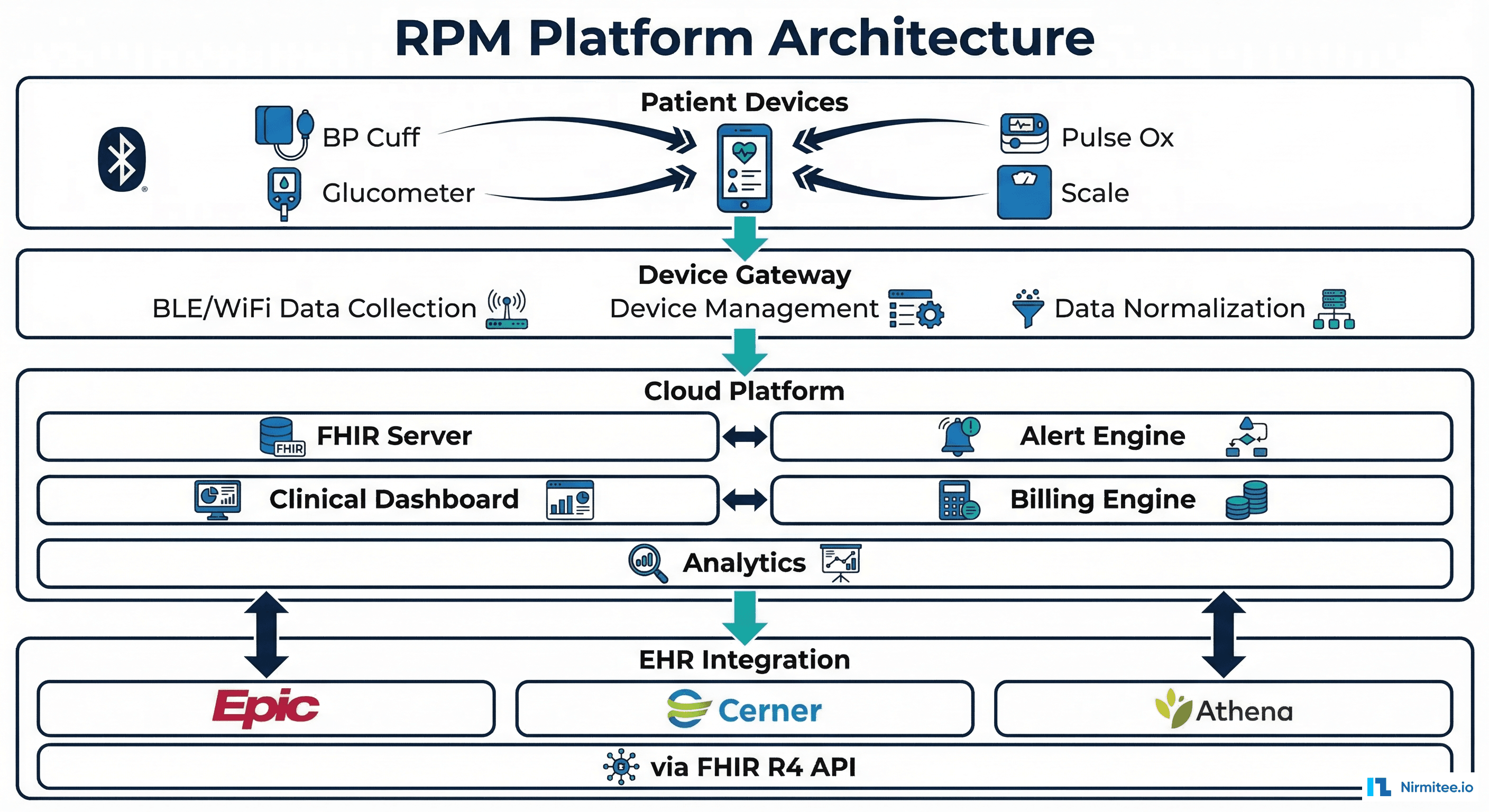
Key architectural decisions:
- Device Gateway: Use a BLE/WiFi gateway service that normalizes data from multiple device manufacturers into a standard format. Consider platforms like Validic, Xealth, or custom-built using manufacturer SDKs
- FHIR Server: Store all patient vitals as FHIR Observation resources with LOINC codes. This enables EHR integration, interoperability, and future-proofing
- Alert Engine: Rule-based alerting with configurable thresholds per patient per vital sign. Alerts must route to the correct clinician with full context (trend data, patient history, care plan). Use AI-driven clinical decision support to reduce alert fatigue
- Clinical Dashboard: Real-time view of patient panel with vital sign trends, alert queue, documentation tools, and time tracking for billing
- Billing Engine: Automated tracking of billable time, data transmission days, and claim generation for CPT codes 99453-99458
Patient Eligibility Criteria
Not every patient is a good RPM candidate. Focus initial enrollment on patients who meet all of these criteria:
- Clinical: 2+ chronic conditions (hypertension, diabetes, CHF, COPD, CKD) requiring ongoing physiologic monitoring
- Insurance: Medicare Part B beneficiary (highest reimbursement) or commercial plan that covers RPM
- Physician order: Documented order for RPM services in the medical record
- Technology readiness: Patient has a smartphone (or caregiver does) and basic willingness to use a connected device
- Engagement potential: Patient is motivated to manage their condition — recent hospitalization or poor control increases motivation
Month 2: Integration — EHR, Enrollment, and Training
EHR Integration
RPM data must flow into the EHR to be clinically useful. The integration approach depends on your EHR system:
| EHR System | Integration Method | Data Destination | Complexity |
|---|---|---|---|
| Epic | FHIR R4 API + MyChart integration | Flowsheets, Observations | Medium-High |
| Cerner/Oracle Health | FHIR R4 API + Millennium integration | Clinical Results, PowerChart | Medium |
| Athenahealth | REST API + Marketplace | Clinical Documents | Medium |
| Custom/Open Source | Direct FHIR R4 API | Observation resources | Low-Medium |
At minimum, push these data points to the EHR flowsheet: blood pressure (systolic/diastolic), heart rate, weight, blood glucose, and SpO2. The EHR integration should be bidirectional — pull patient demographics and care plans from the EHR, push vitals and clinical notes back.
Patient Enrollment Workflow
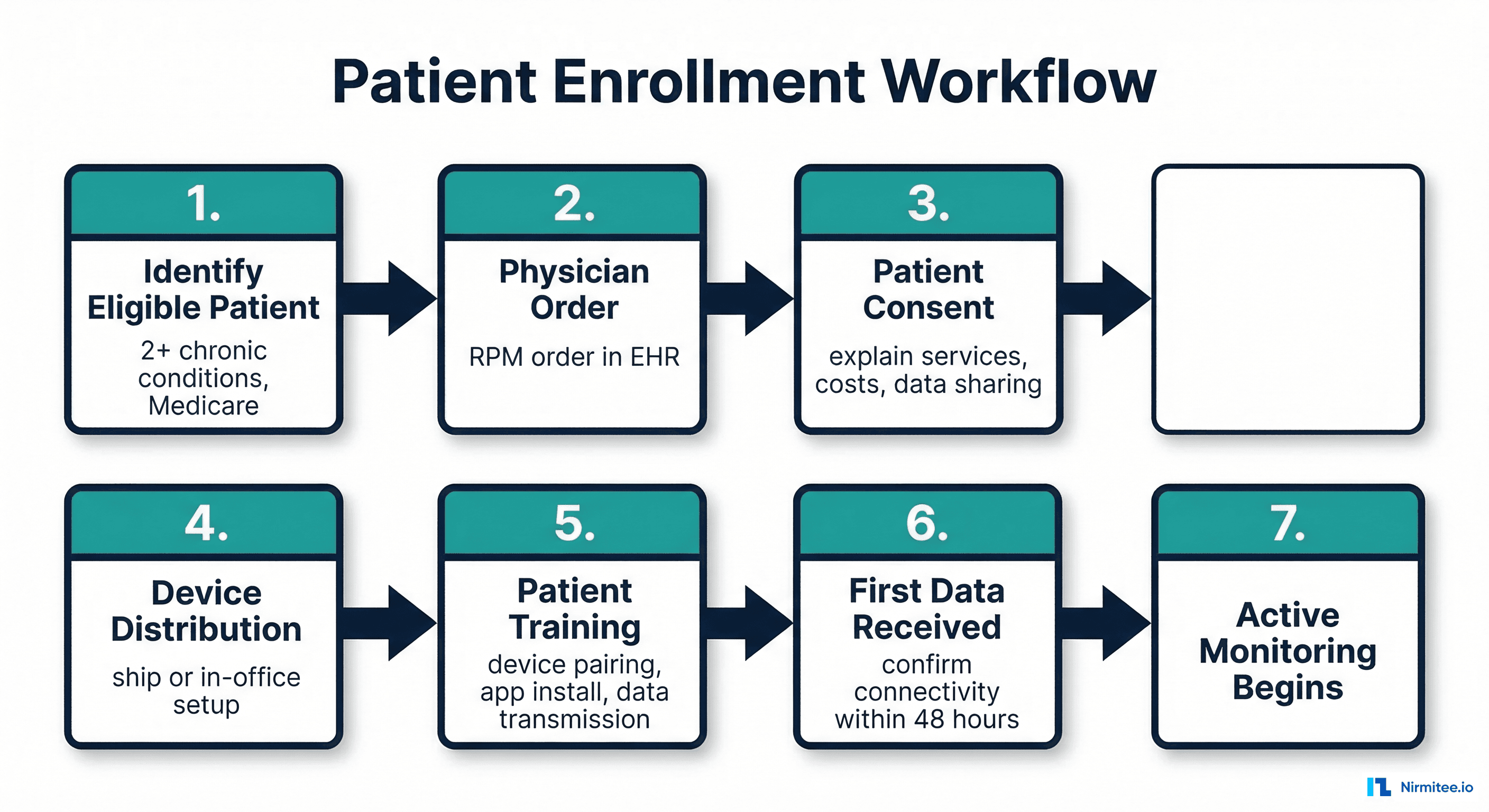
The enrollment process should take no more than 30 minutes per patient. Here is the streamlined workflow:
- Identify eligible patients — Run EHR query for patients with 2+ chronic conditions on active medication regimens. Prioritize recently hospitalized patients and those with poor control metrics (HbA1c > 8%, BP > 150/90)
- Obtain physician order — Physician documents RPM order in EHR with diagnosis codes and monitoring parameters
- Patient consent — Explain services, Medicare cost-sharing (~20% of $55/month = ~$11/month patient responsibility), data sharing practices, and right to cancel anytime
- Device distribution — Ship device to patient home (preferred for scale) or set up during office visit (preferred for complex patients)
- Patient training — 15-minute video call or in-person session: device pairing, app installation, first reading, troubleshooting contacts
- Connectivity confirmation — Verify first data transmission received within 48 hours. Call patient if no data received
- Active monitoring begins — Patient enters 30-day billing cycle. Clinical staff begins monitoring vitals and logging time
Clinician Training Protocol
Clinical staff must be trained on three areas before go-live:
- Platform operation: Dashboard navigation, patient panel management, alert queue workflow, documentation tools
- Alert response protocols: Which alerts are urgent (BP > 180/120, glucose > 400), which are routine (BP 140-160, glucose 180-250), and escalation pathways
- Documentation for billing: Time tracking requirements (minimum 20 minutes/month for 99457), what activities count as billable time, how to document clinical decision-making
Month 3: Go-Live — Pilot Launch, Metrics, and Scaling
Pilot Launch: Start with 20-50 Patients
Do not attempt to enroll your full eligible panel on day one. Start with a controlled pilot of 20-50 patients to identify operational issues before scaling. Select pilot patients who are:
- Highly motivated (recently discussed remote monitoring interest)
- Technologically capable (own smartphone, use apps)
- Clinically stable enough that minor device issues won't create safety risks
- Distributed across common conditions (hypertension, diabetes, CHF)
Key Performance Metrics
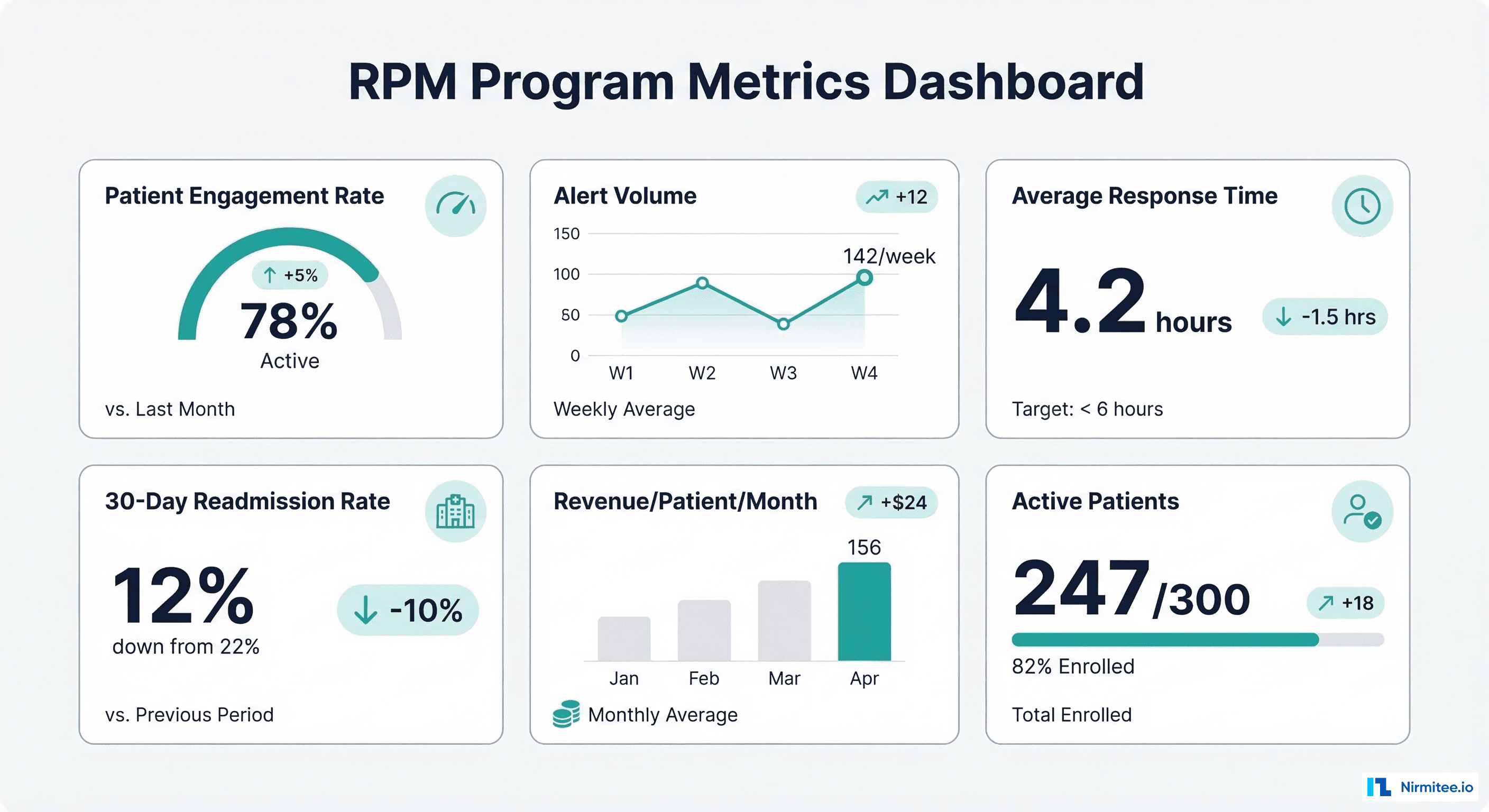
Track these metrics weekly during the pilot and monthly at scale:
| Metric | Target | Why It Matters |
|---|---|---|
| Patient Engagement Rate | >70% | % of enrolled patients transmitting data at least 16 days/month — directly affects 99454 billing |
| Alert Volume per Clinician | <30/day | Too many alerts = alert fatigue and missed critical readings. Tune thresholds |
| Average Alert Response Time | <4 hours | Speed of clinical response to abnormal readings — quality and liability metric |
| Monthly Revenue per Patient | >$150 | RPM reimbursement per enrolled, active, billing-eligible patient |
| 30-Day Readmission Rate | <15% | Clinical outcome metric — RPM should reduce readmissions 20-50% |
| Patient Satisfaction (NPS) | >50 | High satisfaction drives referrals and reduces churn |
| Device Return Rate | <10% | Patients returning or abandoning devices — indicates usability problems |
Billing Setup and Revenue Optimization
Ensure billing infrastructure is ready before go-live:
- Provider credentialing: Verify that billing providers have RPM-specific credentials with Medicare and commercial payers
- Claims configuration: Set up CPT codes 99453, 99454, 99457, 99458 (and new 99445, 99470) in your billing system with correct modifiers
- Time tracking automation: Platform must automatically log time spent reviewing data, responding to alerts, and communicating with patients
- Monthly claim generation: Automated end-of-month claim generation with documentation linkage
Consider stacking RPM with CCM and RTM programs to maximize per-patient revenue — properly stacked, a single patient can generate $360+/month versus $150 for RPM alone.
ROI Analysis: Making the Business Case

| Cost Category | Year 1 Investment | Notes |
|---|---|---|
| Platform Development/License | $80,000-$200,000 | Build custom or license existing platform |
| Device Procurement (100 units) | $15,000-$50,000 | $150-500 per device depending on type |
| Staff Training | $10,000-$25,000 | Clinician training, workflow development |
| Clinical Staff (1 FTE RN/MA) | $60,000-$80,000 | Dedicated RPM clinician for 100-200 patients |
| Total Year 1 Investment | $165,000-$355,000 |
| Revenue/Savings Category | Year 1 Return | Calculation |
|---|---|---|
| RPM Reimbursement | $180,000 | 100 patients x $150/month x 12 months |
| Reduced Readmissions | $80,000-$150,000 | 8-15 avoided readmissions x $10,000-15,000 penalty each |
| Improved Quality Scores | $20,000-$50,000 | MIPS/quality measure improvement bonuses |
| Total Year 1 Return | $280,000-$380,000 |
Payback period: 6-9 months for most programs. ROI: 70-115% in Year 1. Revenue scales linearly with patient count — 250 patients generates $450,000+ in direct RPM reimbursement alone.
Market Context: Why 2026 Is the Right Time
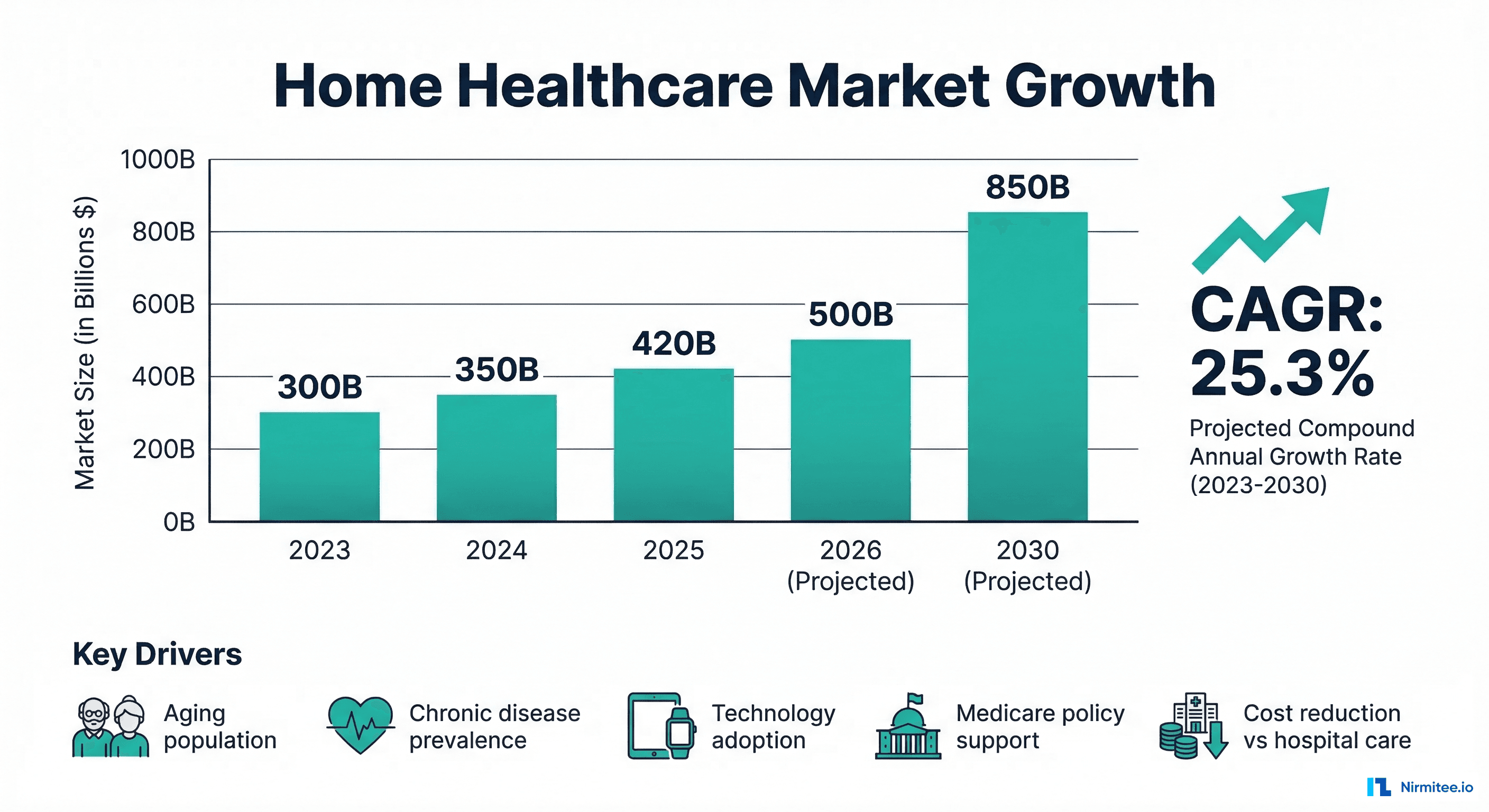
Several converging factors make 2026 the optimal launch window for RPM programs:
- Reimbursement increases: CMS increased RPM payment rates by ~25% overall in the 2026 fee schedule, with the new 99445 code reducing the data transmission barrier
- Technology maturity: BLE-connected medical devices are reliable, affordable, and patient-friendly. Cloud platforms for RPM are proven at scale
- Patient demand: Post-COVID, patients expect digital health options. 76% of patients express interest in remote monitoring according to a 2025 HIMSS survey
- Competitive pressure: Health systems and large practices are building RPM programs rapidly. Practices that wait risk losing patients to competitors offering remote care
- Quality incentives: CMS MIPS and ACO quality measures increasingly reward remote monitoring and care management
Common Pitfalls and How to Avoid Them
- Over-enrolling too fast: Scaling to 200+ patients before workflows are optimized leads to alert fatigue, documentation gaps, and billing denials. Start with 20-50 patients and scale 25% monthly
- Choosing devices patients cannot use: The most accurate device is worthless if the patient cannot operate it. Test every device with actual patients (age 65+) before committing to procurement
- Ignoring engagement: Patients who stop transmitting data within 30 days represent lost revenue and wasted device investment. Build proactive outreach — call patients who miss 3+ consecutive days of transmission
- Manual time tracking: If clinicians manually log RPM time on spreadsheets, documentation will be incomplete and billing will suffer. Automate time tracking in the platform
- No escalation protocol: Without clear alert escalation pathways, critical readings get lost in the queue. Define urgent vs routine thresholds before go-live and assign specific response protocols
- Billing without compliance: Ensure every claim has supporting documentation (time logs, clinical notes, patient consent). Random audits can claw back months of revenue if documentation is incomplete
Frequently Asked Questions
How many patients can one clinician manage in an RPM program?
A dedicated RN or MA can typically manage 150-250 RPM patients depending on acuity level and platform automation. High-acuity patients (CHF, uncontrolled diabetes) require more intervention time — expect 80-120 patients per clinician. Lower-acuity patients (stable hypertension) with good alert automation can scale to 200-250 per clinician. Custom RPM platforms with intelligent alerting and automated documentation increase clinician capacity by 30-40%.
What is the minimum patient volume to make RPM financially viable?
At $150/patient/month in reimbursement, you need approximately 50 active patients to cover the cost of one dedicated clinician ($75,000/year). Below 50 patients, RPM is better operated as a part-time responsibility for existing clinical staff rather than a standalone program. The break-even point for a full platform investment (build or license) is typically 75-100 patients.
Should I build or buy an RPM platform?
Buy (license) if you want to launch in 30-60 days with minimal technical investment and are comfortable with per-patient-per-month SaaS pricing ($15-40/patient/month). Build if you want full control over clinical workflows, EHR integration depth, data ownership, and long-term economics. Custom builds typically take 3-6 months and cost $150K-400K but eliminate per-patient SaaS fees. Many organizations choose a hybrid approach — licensed platform with custom integration layer.
Do I need to provide devices to patients or can they use their own?
For RPM billing under CPT 99454, the practice must provide or arrange for the device. Patients using personal devices (e.g., their own Apple Watch) generally cannot be billed under RPM because the device must be prescribed and the practice must manage the device supply. However, patient-owned FDA-cleared devices (e.g., a patient's own Omron BP cuff) may be acceptable if the practice orders and oversees the monitoring. Check payer-specific policies.
What happens if a patient stops transmitting data?
If a patient transmits data fewer than 16 days in a month, you cannot bill CPT 99454. However, the new 2026 code 99445 allows billing for 2-15 days of transmission at a reduced rate (~$30 vs $55). Implement a proactive engagement workflow: automated reminders at day 3 of no data, phone call at day 5, care coordinator outreach at day 7. Most disengagement is due to technical issues (dead battery, lost connection) rather than patient disinterest.
Conclusion: Your 90-Day RPM Launch Checklist
Launching an RPM program is not a technology project — it is a clinical operations transformation with technology as the enabler. The practices that succeed treat RPM as a new care delivery model, not just a billing opportunity. By following this 90-day roadmap — careful device selection, robust platform architecture, systematic patient enrollment, and data-driven metrics — your organization can launch a clinically effective, financially sustainable RPM program that scales to hundreds of patients.
For organizations seeking a technology partner to build or integrate their RPM platform, Nirmitee's remote patient monitoring solutions provide the complete stack — from device connectivity and EHR integration to clinical dashboards and billing automation — purpose-built for healthcare organizations launching or scaling RPM programs.




